Factors associated with stillbirths in Kibogora District Hospital catchment area, Rwanda, 2015
Esperance Niragire1, &, Lawrence Rugema1, Eric Noёl Kamayirese1, Jared Omolo2, Vincent Mutabazi3, Jean d’Amour Sinayobye3, Joseph Ntaganira1
1Department of Epidemiology and Biostatistics, School of Public Health, University of Rwanda, Kigali, Rwanda, 2Rwanda Biomedical Centre, Kigali, Rwanda, 3African Field Epidemiology Network, Kigali, Rwanda
&Corresponding author
Esperance Niragire, Department of Epidemiology and Biostatistics, School of Public Health, University of Rwanda, Kigali, Rwanda.
Introduction:
Stillbirths pose a significant challenge in Rwanda, particularly in the Kibogora District Hospital catchment area, where the percentage of perinatal deaths attributed to stillbirths has been steadily increasing.In 2015, 70.8% of all perinatal deaths were attributed to stillbirths. This study assessed factors associated with stillbirths in Kibogora District to inform targeted interventions.
Methods:
A hospital-based retrospective unmatched 1:2 case-control study was conducted using 2,605 records of newborns and their mothers that occurred at Kibogora DH in the western province of Rwanda, in 2015. A total of 133 stillborn and 266 controls were enrolled. A stillbirth was defined as the birth of a baby showing no signs of life at birth after 28 weeks of gestation. Data were extracted from various sources (electronic HMIS reports, patients' files, delivery and operating room registers, and stillbirth audit reports) using a structured data collection tool, and analyzed using Stata version 13 software. Multivariate logistic regressions were performed to ascertain the factors associated with stillbirths and adjusted odds ratios (AOR) with a 95% confidence interval (CI) were computed.
Results:
Of the 2.605 total births recorded at Kibogora Hospital, Rwanda in 2015, 5.1% (133/2605) were stillborn, with varying proportions across maternal age groups.
While no statistically significant association was found among known stillbirth risk factors such as maternal age, parity and ANC attendance, maternal HIV-positive status and presence of fetal heart at admission were found to be associated with lower odds of stillbirths (aOR = 0.29, 95% CI=010-0.75 and aOR = 0.02, 95% CI=0.00-0.009 respectively).
Conclusion:
The study underscored the importance of maternal health interventions, particularly in HIV management, and emphasised the need for comprehensive monitoring of fetal well-being throughout pregnancy to mitigate the risk of stillbirths.
Keywords: Risks factors, Stillbirths, occurrence, Kibogora DH.
Introduction

Globally, an estimated 2.6 million stillbirths occur annually; 98% of stillbirths take place in low-income and middle-income countries. Half of all stillbirths (1.3 million) occur during labour and birth, and most of them are due to possible preventable conditions [1]. Absent from the Millennium Development Goals, and still missing in the Sustainable Development Goals (SDGs), stillbirths remain a neglected issue, invisible in policies and programmes, underfinanced and in urgent need of attention [2].
The stillbirth rate in sub-Saharan Africa is about 10 times that of developed countries (29 versus 3 per 1000 births). About 60% occur in rural areas; and more than half in conflict and emergency zones, affecting the families most underserved by healthcare systems [
3]. Every year, 814,000 neonatal deaths and 1.02 million stillbirths result from intrapartum-related causes, such as intra-uterine hypoxia. Almost all of these deaths are in low- and middle-income countries where women frequently lack access to quality antenatal and perinatal care which may delay care-seeking [
4-6]
In resource-limited settings, stillbirths contribute significantly to the broader challenge of prenatal, perinatal, and under-five mortality rates. Developing countries continue to grapple with substantial health concerns for mothers, newborns, and children under the age of five [
6]. Sub-Saharan Africa, in particular, faces the highest rates of maternal, neonatal (including stillbirths), and child mortality. The disparities are stark, with an average of 510 maternal deaths per 100,000 live births compared to 16 in developed countries. Similarly, 109 children out of 1000 live births succumb before the age of five, whereas in developed countries, only seven children out of 1000 live births meet the same fate. Furthermore, 34 newborns out of 1000 live births perish within the first 28 days of life in low- and middle-income countries, contrasting with the significantly lower figure of four newborns out of 1000 live births in developed countries [
7]. These statistics underscore the critical role of stillbirths in the broader context of maternal and child health challenges, particularly in resource-limited settings.
In Rwanda, there has been a consistent downward trend in neonatal mortality over the past decade, accompanied by significant reductions in infant mortality rates. Specifically, infant mortality decreased from 86 deaths per 1000 live births in 2005 to 32 in 2015, while child mortality dropped from 72 deaths to 19 during the same period [
8,
9]. Likewise, according to estimates provided by the UN Inter-Agency Group for Child Mortality Estimation, the neonatal mortality rate in Rwanda decreased to 18.70 per 1000 live births[
9].
This positive trend is attributed to concerted efforts to improve healthcare services at all levels, ensuring both accessibility and quality for the population.
Meanwhile, data from the Rwanda Health Information System (HMIS) documented 323,976 deliveries from January to December 2015, with 317,855 live births and 6,121 stillbirths reported (resulting in a stillbirth rate of 19.2 per 1000 live births). During this same period, there were a total of 3,459 newborn deaths, yielding a neonatal mortality rate of 10.88 per 1000 live births [
7,
8,
10]
During the routine monitoring of health information in the Kibogora DH catchment area, a significant number of perinatal deaths were observed between the fiscal years 2014 and 2017. It is important to note perinatal deaths encompass stillbirths (both fresh and macerated), deaths at birth, and deaths within the first seven days of life. Analysis of the related data revealed that in 2015, 70.8% of all perinatal deaths at Kibogora DH zone were attributed to stillbirths. Subsequently, this percentage increased to 78.4% in 2016-2017. There was a need to assess factors associated with the increase in stillbirths in Kibogora District Hospital (DH). We, therefore, assessed factors that are associated with stillbirth in Nyamasheke district and Kibogora DH area to inform prevention strategies in its catchment area and Nyamasheke district in general.
Methods


Study settings
The research took place within the catchment area of Kibogora DH, situated in Nyamasheke District, in the western province of Rwanda. This rural hospital serves a population of 240,730 (as of 2015) divided into 9 sectors and 28 health facilities comprising one hospital,13 health centers, and 14 health posts. Kibogora District Hospital offers various clinical services, including obstetrics and gynecology services.
Study design
A hospital-based 1:2 unmatched case-control study was conducted using secondary data (records from electronic HMIS reports, registers, patient files and stillbirth audit reports) at Kibogora DH from 1 January 2015 to December 31, 2015.
Study participants
The study participants comprised mothers who gave birth at Kibogora DH between January 1st 2015, and December 31st, 2015, along with their infants, regardless of whether the pregnancy resulted in a stillbirth or live birth. Cases with incomplete or insufficient records, which lacked important research variables such as stillbirth background, signs of fetal distress upon admission, pregnancy history, maternal morbidity during pregnancy, or records that were missing or couldn't be found, were excluded. Also excluded were infants who died before reaching 28 weeks of gestation, or fetuses born deceased weighing less than 500 grams. For controls, the live birth immediately preceding and following each stillborn (at a ratio of 2:1), were enrolled.
Sample size and sampling procedures
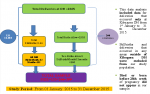
All 133 stillbirths reported in the health management information system (HMIS) database of Kibogora DH during the study period were included. Each one was matched with two live birth controls at a ratio of 1:2 (
Figure 1). A stillbirth was characterized as the delivery of a baby displaying no signs of life at or beyond 28 weeks of gestation, encompassing both fresh and macerated stillbirths categorized as cases, while controls consisted of two surviving neonates: one immediately preceding and another following each stillbirth. Maternal records for all stillborn infants and selected controls were collected and reviewed. The roster of all registration files of mothers who gave birth from January 1, 2015 up December 31, 2015 served as the sampling frame.
Research instrument, data sources and data collection procedures
A structured checklist was used to extract information from the various sources including the patient case notes and delivery register. Four hospital staff members were trained and assisted the primary investigator in data collection.
A pilot study was conducted one month before the main study to pre-test and validate data collection tools. Subsequently, comprehensive data collection activities were carried out during the study period. Data were gathered from both Health Management Information System (HMIS) electronic database and paper-based sources. The medical records of women and their babies, maternity and operating room registers for C-section, surgery and hospitalization registers, patient files, death audit reports, partographs, as well as the HMIS monthly reports for 2015 of Kibogora DH were reviewed, examined, and data triangulated across the various sources and tools.
Study variables
Data were collected on diverse aspects of mothers' profiles, encompassing socio-demographic details such as age, parity and gestational age. Gynecological and obstetrical information included details on pregnancy type, stillbirth background (if the mother has had another stillbirth event in the past) and mode of delivery, while fetal information covered term status, signs of fetal distress upon admission and congenital malformations. The study also delved into pregnancy history and maternal morbidity during pregnancy including urinary and genitourinary infections, HIV, syphilis, hypertension, malaria, and diabetes. Furthermore, data on pregnancy outcomes (stillbirths and live births), the quality of antenatal care services (quantified by the number of standard ANC visits), the quality of care provided by health staff before and during labor (capturing delays in consultation, decision-making, transfer and ambulance availability as it was described in stillbirth audit reports), mothers' information-seeking behaviors (involving the use of traditional medicine and consultation delays), and financial accessibility (indicating health assurance status) were systematically gathered.
Data analysis
A completed Excel sheet of line list was exported into Stata version 13 software for statistical analysis. Bivariate analysis was run to check the association of independent variables with the outcome variable. Variables showing p<0.05 in bivariate analysis were entered into multivariate logistic regression analysis to identify risk factors of stillbirths by controlling for confounding variables. The adjusted Odds ratios (OR) with a 95% confidence interval were reported.
Ethical considerations
Ethical approval was obtained from the University of Rwanda, College of Medicine and Health Science Institutional Review Board with reference number 384/CMHS IRB/2018. Permission to use the data was obtained from the Kibogora DH. Stringent measures were implemented to guarantee the privacy and confidentiality of the gathered information.
Results


A total of 2,605 births were recorded at Kibogora Hospital, Rwanda in 2015, of which 5.1% (133/2605) were stillborn. Among the stillbirths 47% (62/133) were fresh stillbirths while 53% (71/133) were macerated.
Maternal sociodemographic and health-related factors
The mothers' ages ranged from 14 to 45 years old, with a mean age of 29.3 years. Majority of the mothers were aged 30-34 years, accounting for 29.3% (39/133), whereas the lowest proportion was among those aged 14-19 years, constituting only 3.0% (4/133). On the other hand, majority of the control mothers were aged 25-29 years (26.3%, 70/266) and the least proportion were among 14-19 years age group (6.8%, 18/266). However, statistical analysis did not establish any significant association between maternal age and stillbirth occurrence (
Table 1).
We explored medical insurance availability among mothers and found that most mothers in both stillbirth and live birth groups had medical insurance (91.7%, 122/133 and 93.2%, 248/266, respectively). No statistically significant association between medical insurance status and stillbirth was identified (cOR:0.8, 95% CI:0.37-1.81, p = 0.6).
Approximately 30.1% (40/133) of mothers to stillborn infants had associated pathology, compared to 32.0% (85/266) among mothers with live births. However, there was no statistically significant association between presence of an associated pathology and stillbirth (cOR:0.92, 95% CI:0.58-1.43, p = 0.7). We found that poly/oligo hydramnios (characterized by abnormal amniotic fluid levels) occurred minimally in both stillbirth (0.8%, 1/133) and live birth groups (2.3%, 6/266) and did not have any statistically significant association with stillbirth (cOR:0.33, 95% CI:0.02-1.95, p = 0.3).
Only 6.8% (9/133) of mothers with stillbirth were HIV-positive, contrasting with 20.3% (54/266) among mothers with live births. This difference was statistically significant in bivariate analysis (cOR: 0.28, 95% CI:0.13-0.57, p < 0.001). Among mothers with stillbirth, 8.3% (11/133) reported using traditional medicine, compared to 2.6% (7/266) among mothers with live births. This difference was statistically significant (cOR:3.34, 95% CI:1.28-9.26, p = 0.015) in bivariate analysis, suggesting a potential association between traditional medicine use and stillbirth risk (
Table 1).
Reproductive and pregnancy-related factors
The study found that a parity of 5-8 children was associated with a higher stillbirth rate (21.8%, 29/133) compared to 13.2% (29/266) for live births. We observed that stillbirths were nearly two-fold among mothers who were para 5-8 compared to those who had parity of less than 5 children (cOR:1.79, 95% CI: 1.03-3.10, p=0.037). Spontaneous vaginal deliveries (SVD) were more common among the stillbirths group (69.2%, 92/133) compared to livebirths group (41.4%, 110/266). We observed a three-fold rate of stillbirths among SVDs compared to caesarean sections (cOR:3.18, 95% CI: 2.06-4.99, p < 0.001). Multiple pregnancies showed a higher stillbirth rate (12%, 16/133) compared to live births (5.3%, 14/266). Multiple pregnancies were statistically significantly associated with stillbirths compared to monofetal pregnancies (cOR:2.46, 95%CI:1.16-5.28, p=0.019) in bivariate analysis.
Term and post term births were significantly associated with lower odds of stillbirths when compared to pre term births (cOR= 0.48, 95%= 0.30 -0.761, p = 0.002) in bivariate analysis. Having a fetal heart at admission was significantly protective against stillbirths (cOR:0.01, 95% CI:0.00-0.03, p<0.001). In bivariate analysis, attending at least four ANC visits was protective against still births compared to not attending ANC (cOR:0.53, 95% CI:0.29-0.99, p=0.048) (
Table 2).
Predictors of stillbirths in Kibogora District Hospital catchment area
After adjusting for confounding through multivariate logistic regression, two variables were significantly associated with stillbirths: maternal HIV-positive status (aOR: 0.29, 95% CI:0.10-0.75, p = 0.017) and presence of a fetal heart at admission (aOR: 0.02, 95% CI:0.00-0.009, p < 0.001) (
Table 3).
Discussion


This retrospective case-control study conducted at Kibogora DH, aimed to identify the factors linked to stillbirths in Nyamasheke district, Western province of Rwanda, during the period from January 2015 to December 2015. The study explored the association between stillbirths and various socio-demographic, clinical, reproductive, and pregnancy-related factors. It provides valuable insights into potential predictors of stillbirths in the Kibogora District Hospital catchment area. After multivariable logistic regression, two key factors were found to be associated with stillbirths: maternal HIV positive status and presence of a fetal heart at admission.
Previous studies have identified higher prevalence of stillbirth among mothers with HIV [
11,
12] However, in this study, maternal HIV-positive status was associated with lower odds of stillbirths. This could likely be an outcome of the increased interaction between HIV positive mothers and health providers as part of the efforts to prevent mother to child HIV transmission. The integrated support and increased ANC attendance provides additional opportunities for identifying and mitigating obstetric risks which would likely contribute to adverse outcomes like stillbirths.
The presence of a fetal heart during admission was associated with lower odds of stillbirths in this study. Auscultation of a fetal heart especially during labor is often an indicator of fetal vigor and absence of fetal distress, a condition which has been found to be strongly associated with stillbirths [
13] and is a common precursor to peripartum mortality.
Previous studies have identified an association between stillbirths and maternal, reproductive, pregnancy-related factors. Although these were explored in this study, they were not statistically significant. Studies investigating the association between socio-demographic factors and stillbirths have revealed mixed results. In a study conducted in Nepal by Ghimire et al, still births were associated with education, occupation, and ecological zones of residence [
14]. In this study, maternal socio-demographic like age did not show a statistically significant association with stillbirth. This aligns with findings from a study conducted in 2013 in National Health Service (NHS) England that indicated that advanced maternal age may not always be a significant risk factors for stillbirth [
15]. It is also consistent with another study conducted in India by Neogi et al which did not identify any link between socio-demographic factors and stillbirths [
16].
The use of traditional medicine was more common among the stillbirths compared to the live births in this study even though it was not a statistically significant predicator. This highlights the importance of addressing such traditional practices in maternal healthcare interventions, as these practices may have negative implications for pregnancy outcomes [
17].
Among the reproductive and pregnancy-related factors, parity and pregnancy status did not have statistically significant association with stillbirth in this study, contrary to some previous research which have identified multiparity and post-term pregnancy as potential risk factors for stillbirth. Similarly, cesarean delivery has been found to be associated with adverse pregnancy outcomes, including stillbirth [
14,
18] However, in this study, although it was more prevalent among stillbirth cases than livebirths, it was not an independent predictor [
19-21]
While some findings from this study align with previous research on stillbirth risk factors, such as the association with HIV infection, other findings diverge from established literature[
22]. This disparity may be attributed to differences in study populations, healthcare infrastructure, and socio-cultural factors influencing maternal and child health outcomes in rural settings like Kibogora DH catchment area.
Study limitations
As this study was hospital-based, the reported stillbirth rates and determinants exclude stillbirths that may have occurred outside health facilities[
23]. Therefore, the findings do not necessarily reflect the essential predisposing factors that lead to stillbirths in the entire population[
22]. Additional personal and environmental factors may have influenced the stillbirths but could not be assessed due to use of hospital records[
24].
The study may also have been affected by the limitations associated with case-control studies. Although recall bias was minimised by objectively reviewing records, it could not be completely eliminated. The challenge of missing data could not be completely eliminated but was mitigated through use of multiple data sources.
Conclusion


Maternal HIV status and presence of fetal heat rate at admission were associated with lower odds of stillbirths in this study. These results underscore the critical role of maternal health interventions, specifically in HIV management, and emphasizes the necessity for careful monitoring of fetal well-being throughout pregnancy and during labor to mitigate the risk of stillbirths within the Kibogora DH catchment area. There is need to conduct a population-based assessment to further explore the role of known risk factors like maternal; age, parity, ANC attendance and mode of delivery which were not found to be independently associated with stillbirths in this study.
What is known about this topic
- Previous researches highlighted various factors influencing stillbirth risk, including HIV infection, maternal health conditions like hypertension and diabetes, socioeconomic status, and the importance of antenatal care in detecting and managing pregnancy complications
- While some findings align with established literature, others diverge, possibly due to differences in study populations and healthcare settings.
- Previous studies indicate that conditions like hypertension, diabetes, infections, and maternal age significantly influence stillbirth risk by affecting fetal development if not managed effectively.
- Previous Researches consistently link lower socioeconomic influence (status) encompassing poverty, limited education, and restricted healthcare access, to higher stillbirth rates, underscoring the need to address social determinants of health.
- Highlight the importance of Antenatal Care(ANC) as crucial for identifying and managing pregnancy complications associated with stillbirth risk, including placental abnormalities, fetal growth restriction, and preterm birth, highlighting the necessity of improved access to quality antenatal services to reduce stillbirth rates.
What this study adds
- This study adds valuable insights to the global understanding of stillbirth factors by focusing on a specific geographic area and enriching the existing body of research with data from Rwanda.
- By identifying unique risk factors and considering community-specific dynamics within the Kibogora District Hospital catchment area, it contributes to the development of more insights and informs the development of effective strategies for stillbirth prevention worldwide.
Competing interests


The authors declare no competing interests.
Authors´ contributions


EN, LR and JN conceptualized the study, designed the methods, analyzed data and drafted the manuscript. MN, JN, JO and JBS provided substantial contributions to the interpretation of data. JBS and EN contributed to the data analysis, review and proofreading of the manuscript. JN, KEN, JBS,JO,JN provided substantial contributions to the interpretation of data and took part in revising the paper critically for important intellectual contents. All authors agreed to submit to the current journal, are accountable for all aspects of the work, and provided final approval of the version to be published.
Acknowledgements


We acknowledge the University of Rwanda/College of Medicine and Health Sciences/School of Public Health, Rwanda Biomedical Centre, Rwanda African Epidemiology Network (AFENET) and Kibogora District Hospital.
Tables and figure


Table 1: Maternal socio-demographic and health-related factors associated with stillbirth in Kibogora district hospital catchment area
Table 2: Reproductive and Pregnancy-related factors associated with stillbirth in Kibogora district hospital catchment area
Table 3: Predictors of stillbirths in Kibogora District Hospital catchment area
Figure 1: Sampling strategy description
References


- Lawn JE, Cousens S, Zupan J. 4 million neonatal deaths: When? Where? Why? The Lancet [Internet]. 2005 Mar 5[cited 2024 May 8];365(9462):891-900. https://doi.org/10.1016/s0140-6736(05)71048-5 PubMed
- Khurmi MS, Sayinzoga F, Berhe A, Bucyana T, Mwali K, Manzi E, Muthu M.Newborn Survival Case Study in Rwanda - Bottleneck Analysis and Projections in Key Maternal and Child Mortality Rates Using Lives Saved Tool (LiST). Int J MCH AIDS [Internet]. 2017 Oct [cited 2024 May 6];6(2):93-108. https://doi.org/10.21106/ijma.214 PubMed | Google Scholar
- United States Agency for International Development; Ministry of Health (Rwanda). Assessment of Maternal and Perinatal Death Surveillance and Response Implementation in Rwanda [Internet]. Washington (WA): United States Agency for International Development; 2017 Dec [cited 2024 May 6]. 37 p. Grant No.: AID-OAA-A-14-00028. Download PA00SZDW.pdf.
- WHO;UNICEF;WORLD BANK GROUP;UNITED NATIONS, editors. A Neglected Tragedy: The global burden of stillbirths [Internet]. New York (NY): United Nations Children´s Fund; 2020 Nov 30 [cited 2024 May 6]. 86 p. Report of the UN Inter-agency Group for Child Mortality Estimation (IGME). Download UN-IGME-the-global-burden-of-stillbirths-2020.pdf.
- Lawn JE, Lee AC, Kinney M, Sibley L, Carlo WA, Paul VK, Pattinson R, Darmstadt GL. Two million intrapartum-related stillbirths and neonatal deaths: where, why, and what can be done? Int J Gynaecol Obstet [Internet]. 2009 Oct 6[cited 2024 May 6];107(Suppl 1):S5-19. https://doi.org/10.1016/j.ijgo.2009.07.016 Google Scholar
- Countdown to 2030 core collaborators. Maternal and newborn health in low- and middle-income countries: A brief assessment of mortality, coverage and policies [Internet]. Countdown to 2030; 2021 [cited 2024 May 7]. 18 p. Prepared for the AlignMNH Opening Forum, 20-21 April 2021. Download Report-AlignMNH-Final-19Apr2021-1.pdf.
- Ministry of Health and Family Welfare, Child Health Division (India). Operational Guidelines for Establishing Sentinel Stillbirth Surveillance System [Internet]. Delhi (India): Ministry of Health and Family Welfare; 2016 Jun [cited 2024 May 7]. 32 p. Download Operational_Guidelines_for_establishing_Sentinel_Stillbirth_Surveillance_System.pdf.
- Lee AC, Cousens S, Wall SN, Niermeyer S, Darmstadt GL, Carlo WA, Keenan WJ, Bhutta ZA, Gill C, Lawn JE.Neonatal resuscitation and immediate newborn assessment and stimulation for the prevention of neonatal deaths: a systematic review, meta-analysis and Delphi estimation of mortality effect. BMC Public Health [Internet]. 2011 Apr 13 [cited 2024 May 7]; 11 (Suppl 3): S12. https://doi.org/10.1186/1471-2458-11-s3-s12 PubMed | Google Scholar
- Ministry of Health (Rwanda). Rwanda Annual Health Statistics Booklet 2012[Internet]. Kigali (Rwanda): Ministry of Health; 2013[cited 2024 May 7]. 80 p. Download MOH_Booklet_2012_final_September_2013.pdf. Google Scholar
- De Bernis L, Kinney MV, Stones W, Ten Hoope-Bender P, Vivio D, Leisher SH, Bhutta ZA, Gülmezoglu M, Mathai M, Belizán JM, Franco L, McDougall L, Zeitlin J, Malata A, Dickson KE, Lawn JE.Stillbirths: ending preventable deaths by 2030 . The Lancet [Internet]. 2016 Feb 13[cited 2024 May 7];387(10019):703-16. https://doi.org/1016/s0140-6736(15)00954-x Google Scholar
- Gardosi J, Madurasinghe V, Williams M, Malik A, Francis A.Maternal and fetal risk factors for stillbirth: population based study. BMJ [Internet]. 2013 Jan 24 [cited 2024 May 7];346:f108. https://doi.org/10.1136/bmj.f108 PubMed | Google Scholar
- Li H, Liu J, Tan D, Huang G, Zheng J, Xiao J, Wang H, Huang Q, Feng N, Zhang G.Maternal HIV infection and risk of adverse pregnancy outcomes in Hunan province, China: A prospective cohort study. Medicine [Internet]. 2020 Feb 1[cited 2024 May 7];99(8):e19213. https://doi.org/10.1097/md.0000000000019213 PubMed | Google Scholar
- Peltzer K, Phaswana-Mafuya N, Treger L.Use of traditional and complementary health practices in prenatal, delivery and postnatal care in the context of HIV transmission from mother to child (PMTCT) in the Eastern Cape, South Africa . Afr J Trad Compl Alt Med [Internet]. 2009 Mar 7 [cited 2024 May 7];6(2):155-62. https://doi.org/10.4314/ajtcam.v6i2.57087 PubMed | Google Scholar
- Flenady V, Koopmans L, Middleton P, Frøen JF, Smith GC, Gibbons K, Coory M, Gordon A, Ellwood D, McIntyre HD, Fretts R, Ezzati M.Major risk factors for stillbirth in high-income countries: a systematic review and meta-analysis. The Lancet [Internet]. 2011 Apr 16 [cited 2024 May 7];377(9774):1331-40. https://doi.org/10.1016/s0140-6736(10)62233-7 Google Scholar
- Ellis A, Chebsey C, Storey C, Bradley S, Jackson S, Flenady V, Heazell A, Siassakos D.Systematic review to understand and improve care after stillbirth: a review of parents´ and healthcare professionals´ experiences . BMC Pregnancy Childbirth [Internet]. 2016 Jan 25 [cited 2024 May 7];16(1):16. https://doi.org/10.1186/s12884-016-0806-2 PubMed | Google Scholar
- Darmstadt GL, Yakoob MY, Haws RA, Menezes EV, Soomro T, Bhutta ZA.Reducing stillbirths: interventions during labour . BMC Pregnancy Childbirth [Internet]. 2009 May 7[cited 2024 May 7];9(S1):S6. https://doi.org/10.1186/1471-2393-9-s1-s6 PubMed | Google Scholar
- Neogi SB, Negandhi P, Chopra S, Das AM, Zodpey S, Gupta RK, Gupta R.Risk Factors for Stillbirth: Findings from a Population-Based Case-Control Study, Haryana, India. Paediatric Perinat Epid [Internet]. 2015 Oct 7[cited 2024 May 7];30(1):56-66. https://doi.org/10.1111/ppe.12246 Google Scholar
- Ghimire PR, Agho KE, Renzaho A, Christou A, Nisha MK, Dibley M, Raynes-Greenow C.Socio-economic predictors of stillbirths in Nepal (2001-2011) . Dangal G, editor. PLoS ONE [Internet]. 2017 Jul 13 [cited 2024 May 7];12(7):e0181332. https://doi.org/10.1371/journal.pone.0181332 PubMed | Google Scholar
- Lawn J, Shibuya K, Stein C.No cry at birth: global estimates of intrapartum stillbirths and intrapartum-related neonatal deaths. Bull World Health Organ [Internet]. 2005 Jun 17[cited 2024 May 7];83(6):409-17. Download pdf to view full article. Google Scholar
- Cheptum JJ, Muiruri N, Mutua E, Gitonga M, Juma M.Correlates of stillbirths at nyeri provincial general hospital, kenya, 2009-2013: a retrospective study. Int J MCH AIDS [Internet]. 2016 Mar [cited 2024 May 7];5(1):24-31. https://doi.org/10.21106/ijma.89 PubMed | Google Scholar
- Musafili A, Persson L�, Baribwira C, P�fs J, Mulindwa PA, Essén B.Case review of perinatal deaths at hospitals in Kigali, Rwanda: perinatal audit with application of a three-delays analysis . BMC Pregnancy Childbirth [Internet]. 2017 Mar 11[cited 2024 May 7];17(1):85. https://doi.org/10.1186/s12884-017-1269-9 PubMed | Google Scholar
- Akombi BJ, Ghimire PR, Agho KE, Renzaho AM.Stillbirth in the African Great Lakes region: A pooled analysis of Demographic and Health Surveys. Uthman O, editor. PLoS ONE [Internet]. 2018 Aug 29 [cited 2024 May 7];13(8):e0202603. https://doi.org/10.1371/journal.pone.0202603 PubMed | Google Scholar
- National Institute of Statistics of Rwanda, Ministry of Health (Rwanda), ICF International. Rwanda Demographic and Health Survey 2014-2015 [Internet]. Kigali (Rwanda): National Institute of Statistics of Rwanda; 2016 Mar [cited 2024 May 7]. 615 p. Jointly published by ICF International. Download FR316.pdf.
- Wall SN, Lee ACC, Carlo W, Goldenberg R, Niermeyer S, Darmstadt GL, Keenan W, Bhutta ZA, Perlman J, Lawn JE.Reducing intrapartum-related neonatal deaths in low- and middle-income countries-what works? Semin Perinatol [Internet]. 2010 Nov 18 [cited 2024 May 7];34(6):395-407. https://doi.org/10.1053/j.semperi.2010.09.009 Google Scholar