Strengthening preparedness and response to epidemics in West Africa: a scoping review of strengths, gaps, and challenges (2016-2019)
Virgil Lokossou1, Emma Edinam Kploanyi2, Delia Akosua Bandoh3,&, Edgard-Marius Ouendo4, Issiaka Sombie5, Kofi Mensah Nyarko6, Ernest Kenu3
1ECOWAS Regional Center for Disease Surveillance and Control, Abuja, Nigeria, 2University of Ghana School of Public Health, Legon Accra, 3Ghana Field Epidemiology and Laboratory Training Programme, University of Ghana School of Public Health, Accra, Ghana, 4Institut Regional de Santé Publique, Ouidah, Benin, 5West African Health Organisation, Bobo Dioulasso, Burkina Faso, 6Sierra Leone Field Epidemiology Training Programme, Freetown, Sierra Leone
&Corresponding author
Delia Akosua Bandoh, Ghana Field Epidemiology and Laboratory Training Programme, University of Ghana School of Public Health, Accra, Ghana. deliabandoh@st.ug.edu.gh
Introduction:
West Africa has seen several epidemics of infectious diseases including the 2014-16 Ebola virus disease epidemic that revealed inadequate national and regional response to epidemics and other health emergencies. We conducted a situational analysis to identify strengths, gaps, and challenges in preparedness and response (P&R) capacities in the West African region.
Methods:
A scoping review was conducted to identify the strengths and gaps in P&R capacities which were validated through interviews with key stakeholders from all fifteen countries in the Economic Community of West African States. Data were collected from April to August 2018 using a structured questionnaire and interview guide administered to country officials. Data from the scoping review and document verification were analysed under eight major themes drawn from the IHR capacities and triangulated with the interviews.
Results:
Response coordination mechanisms existed in all 15 countries as supported by EOCs of which some operated virtually. All countries reported additional criteria to be met for their NPHIs to be fully functional. Only one-third of the countries had plans for generic epidemic preparedness. The study also found over-reliance on donors due to inadequate internal funding for laboratory testing.
Conclusion:
This study revealed some strengths and weaknesses that should be targeted for the improvement of P&R capacities and capabilities. Countries need to establish fully functional National Public Health Institutes for ensuring effective coordination. They should also update legislations in support of P&R to ensure rapid and effective response to public health emergencies.
Introduction

The West African region has seen several epidemics of infectious diseases including the Ebola Virus Diseases (EVD) epidemic that devastated the region between 2014 and 2016 [1-6]. This epidemic resulted in high morbidity and mortality in Liberia, Sierra Leone, and Guinea with its subsequent adverse impact on the health systems of these countries. This has posed multiple health challenges including the limited access to health services for both epidemic and endemic diseases such as human immunodeficiency (HIV/AIDS), tuberculosis (TB), and malaria.[6].
Other health emergencies or disasters, particularly related to meteorological and hydrological hazards and climate extremes, are also increasing across the region. They have been further exacerbated by unplanned and unregulated land use, weak environmental controls, poor enforcement of building standards, urbanization, and other development-linked factors that increase the vulnerability of people and livelihoods. Hydro-meteorological events cause the majority of loss of life and economic losses in West Africa.[
7] Other disasters that have occurred in the region comprise droughts, tropical cyclones, strong winds, storm surges, extreme temperatures, forest fires, sand or dust storms, and landslides.[
8-10]. These emergencies require particular attention and tremendous efforts for ECOWAS Member States for their prevention and control.
These efforts, although commendable, need to be expanded for adequate preparedness and response (P&R) to health emergencies in the region. Countries need to fully develop the IHR core capacities to prevent, detect and respond to public health events[
11]. Hence, there is the need to first identify preparedness capacities that need strengthening to inform response capabilities. Since there may be variations in the capacities that need improvement across Member States,[
12] the West African Health Organisation (WAHO) conducted a situational analysis of strengths, gaps, and challenges in P&R for the period 2016 to 2018 at the regional level. This analysis is towards the development of a regional strategy for advancing P&R in West Africa.
Methods


Study design
Given the lack of synthesized evidence focusing on ECOWAS region, the complexity and interconnected nature of preparedness, a scoping review was considered the most appropriate approach to examine the strengths and gaps in epidemic P&R. A scoping review is a form of “knowledge synthesis, that follows a systematic approach to map evidence on a topic and identify main concepts, theories, sources, and knowledge gaps [
13].” The review adapted the methodology developed by Arskey and O´Malley [
14] and further refined by Levac et al. [
15] and Joanna Briggs Institute [
16]. This study encompassed a comprehensive desk review as well as a consultation phase through series of key informant interviews (KII), a survey for country officials and a regional meeting for discussing the preliminary findings.
Phase 1: Desk review
We conducted a literature review of published (peer reviewed journal articles) and grey literature (technical reports, meeting and conference reports, position papers) to explore strengths, challenges, opportunities and threats in regional P&R. All the fifteen (15) ECOWAS Countries were included in the study. We searched in electronic databases including Google Scholar, PubMed, HINARI, African Journals Online, Web Science, websites of relevant organizations, country MoH websites, and published activities on areas including preparedness and response, epidemics, IHR capacities/JEE evaluation, resilience in West Africa. This review also included national and regional health documents, assessments reports, guidelines and policies available online that described or assessed capacities that could potentially strengthen P&R to either infectious disease threats or natural hazards.
Papers written in English and French were included, which meant that the majority of relevant literature should have been captured, as almost all related academic papers in West Africa are published in these two languages. French papers had to have an abstract written in English. All related literature in Portuguese had versions in either English or French hence they were not excluded. The search covered papers published from the years 2016 to 2019. The eligibility criteria for inclusion in the review are summarized in Box 1. The search yielded to 36 documents that satisfied the inclusion criteria as summarized in
Table 1. Documents reviewed are listed in
Table 2.
Charting the data was done using a structured Microsoft Excel spreadsheet that were clustered under eight (8) themes: coordination, legislation, and policies; surveillance on epidemic-prone diseases; cross border preparedness and response; workforce development; risk communication and community engagement; laboratory systems and networks; information systems and health research; and one health concept. Points for assessment are summarised in
Table 3.
The charted data were split into key strengths, gaps, and challenges in relation with systems, processes and policies established after the Ebola Virus Outbreak in West Africa. Data were grouped into common categories the findings were then analysed in the context of the overall objectives of the study.
Phase 2: Consultation phase
The consultation phase combined a questionnaire-based survey of country officials, some KIIs and a regional meeting for validating the results. Data were collected from April to August 2018. Building on the literature review, a structured questionnaire was developed and administered to leaders of National Public Health Institutions (NPHI) and any relevant official contributing to P&R in ECOWAS countries. The questionnaire was developed based on the International Health Regulation (IHR) capacities and Joint External Evaluation (JEE) checklists.
Interviews were conducted with key informants including representatives from ECOWAS Member States and some international agencies (expatriates) in the fields of P&R, health system strengthening, global health security, epidemic response and management, and the community health sector. Each KII lasted for approximately 1hour. The interviews were recorded and transcribed for further analysis.
To ensure triangulation of the information, the WAHO jointly organized a technical meeting at Abuja in December 2019 to discuss the status of P&R at the regional level in West Africa through a participatory panel discussion referred to as an “organized public exchange of ideas with experts and other participants discussing a particular topic to create an action map and incorporate directions for possible future actions”[
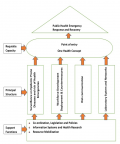
17]. During this meeting, the preliminary findings of this study were discussed based on various themes with representatives from the 15 ECOWAS Countries including NPHI leads, experts from partner organizations, and 14 stakeholders from academia. The discussion offered additional sources of information, and expert perspectives on the preliminary findings, how to effectively support ECOWAS in the implementation of P&R initiatives, and the best practices to strengthen P&R both at regional and national levels. The entire discussion lasted about six hours. The decision on points considered as strengths, gaps, challenges, opportunities and threats were arrived at through a participatory approach by the moderators of the panel discussions. The findings of this scoping study were summarized through the various thematic pillars into 3 core sections: support functions, principal structures and requisite capacity
Figure 1.
Data analysis
Data gathered from KIIs were transcribed and analysed under major eight themes drawn from the WHO IHR core capacities. These themes were selected based on their importance for developing the ECOWAS regional preparedness and response plan. Data generated from the scoping review and document verification were also analysed under these major themes and triangulated with the interviews. Strengths and gaps in regional preparedness and response were identified through a SWOT analysis
Figure 2 and organized under the major thematic areas for capacity strengthening drawn from the scoping review and transcripts.
Ethical considerations
From all participants, consent was obtained but anonymity was not guaranteed. The Ministries of Health (MoH) of all ECOWAS Member States gave their consent through WAHO for this assessment. Interviews were only conducted after participants gave their approval based on the explanation of the purpose of the assessment. Participants and countries had the liberty to withdraw from the assessment at any point and they were assured that it would not affect them in any way as a nation.
Results


Situational Analysis of regional capacities for public health emergency P&R
The situational analysis conducted in all ECOWAS Member States revealed certain strengths and gaps in capacities for public health emergency P&R that were organized under eight (8) themes comprising coordination, legislation, and policies; surveillance on epidemic-prone diseases and risk of health emergencies; cross border preparedness and response; workforce development; risk communication and community engagement; laboratory system and network; information systems and health research; and one health concept.
Coordination, legislation, and policies
The analysis examined four key aspects of the response coordination mechanism including the presence of a functional National Public Health Institute, and EOCs; agencies responsible for major disasters and emergencies; the legal framework supporting coordination and P&R in general; as well as P&R plans. All countries had some form of EOCs with varying functionality including some that operated virtually. However, all member States had reported additional criteria to be met for the National Public Health Institute (NPHI) to be fully functional.
About 70% of the Member States had a legal framework and/or legislation that support and enable the implementation of public health emergency P&R. Nonetheless, there were no legal or ethical guidelines laid out for handling public health emergencies before, during, and after such events. Moreover, most of the relevant legislation from Member States were outmoded and needed revision.
Out of the 15 Member States reviewed, only Nigeria, the Gambia and Liberia had plans for generic epidemic preparedness. Almost all the plans reviewed from the member states did not have timelines linked to indicators to enable periodic tracking/ monitoring of the progress. Also, all the plans were not budgeted and therefore no well-defined budget lines were available for the key activities for epidemic preparedness and response.
Member States had agencies established to be responsible for major disasters or emergencies. All the agencies had plans that outlined the major disaster in the country and how it should be managed. However, they did not clearly state how they will support coordination and how the various stakeholders will collaborate and work together.
Surveillance on epidemic-prone diseases and risk of health emergencies
The implementation of Integrated Disease Surveillance and Response (IDSR) in the region promoted indicator and event-based surveillance systems in all Member States although reporting sites in the countries largely excluded private health facilities. Moreover, not all Member States had been able to successfully roll out event-based surveillance systems countrywide. Liberia had implemented sentinel surveillance for selected diseases and pathogens such as neglected tropical diseases, Lassa fever, rotavirus and HIV. Ghana also had sentinel surveillance for HIV and malaria. All Member States carried out syndromic surveillance for some diseases and conditions such as polio, severe acute respiratory infection, influenza, acute viral haemorrhagic fever and acute diarrhoea with dehydration. The assessment only found evidence of real-time early warning systems in countries with functional EOCs. Besides, none of the 15 countries was found to have evidence of surveillance for unexplained deaths.
IDSR reporting was low in some member countries. Routine surveillance data generated were not regularly analysed at lower levels due to inadequate capacity. A few countries - Sierra Leone, Gambia and Ghana - disseminated reports more frequently through weekly epidemiologic/surveillance bulletins. No member country had a fully functional interoperable and interconnected electronic real-time reporting system at the time of assessment. Member States were at various stages of development and functionality; whereas some of them had no real-time reporting system in place; Sierra Leone, Senegal, Nigeria, and Benin were at the development stage. On top of that, Cote D´Ivoire had a functioning electronic reporting system that enabled real-time reporting of notifiable diseases by making information collection tools available. However, there was no real-time data collection within laboratories and no mechanisms for centralizing data. Also, the Gambia was yet to attain full functionality at the time of assessment.
Cross border preparedness and response
Countries with cross border preparedness and response included Nigeria, Liberia, Cote D´Ivoire, Sierra Leone, Mali, Guinea, Ghana, Benin, Gambia, and Senegal. Most of them had worked together on several outbreaks such as meningitis among the countries within the meningitis belt and also during the EVD outbreak in West Africa. Liberia had ongoing cross border arrangements along the Mano River Union countries. The assessment did not find any regional cross border policy or strategic plan nor any formalized routine cross-border meetings between neighbouring countries to review relevant surveillance data.
Workforce Development
For all Member States assessed, there were inadequate numbers of public health personnel especially field epidemiologists and trained frontline healthcare workers to implement IHR core capacity requirements. Apart from Ghana, none of the assessed countries had a full complement of all three FETPs (basic, intermediate, and advance). Also, there was poor in-country coordination of activities among the available personnel in the containment of epidemics and health emergencies.
Risk Communication and community engagement
Although WAHO recently developed a risk communication plan for the ECOWAS sub-region, no Member State had stand-alone risk communication plans for risk communication during epidemics. Rather, they had risk communication as part of their epidemic preparedness and response plans. Countries employed multiple channels to communicate health risks ranging from mass media to gong beating. However, most countries had limited technical, financial, and human resources for risk communication. The majority of countries lacked anthropologists; Liberia, however, had one and also implemented a strong rumour control mechanism. The region lacked a functional regional platform for inter-sectoral collaboration in risk communication and had limited sustainability of risk communication activities. Budget lines for risk communication at the regional and country levels were weak and even non-existent in some Member States. The JEE evaluation corroborated these findings as it revealed that most member countries had low scores in the areas of risk communication.
Laboratory System and Network
All Member States had laboratories at various levels such as district and regional hospital facilities, as well as national level laboratories that were usually specialized referral national laboratories. However, at the time of assessment, Sierra Leone and Liberia had weak laboratory capacity even though Liberia had a Public Health Reference Laboratory. Liberia could not test for several IDSR Priority Diseases in-country, therefore samples were sent out of the country for testing. The major gaps identified were shortage or stock out of laboratory reagents and consumables, inadequate equipment, and poor equipment maintenance culture. Also, accreditation of laboratories and harmonization of methods needed strengthening. Not all member countries had national-level protocols and policies for specimen referral and transportation of routine clinical specimens within and outside the country (e.g. sample packaging, transportation options, and transmission of results). There was no specimen referral network for priority diseases not under surveillance. Also, not all laboratories were implementing quality assurance systems such as SLIPTA.
Information Systems and Health Research
There were some collaborations including sub-regional research on meningitis, Lassa fever, measles, and other zoonotic-related research. Four countries (Mali, Guinee, Liberia, and Sierra Leone) formed a consortium and were researching drugs and vaccines against Ebola. The objective of this consortium was to enhance human resources capacity in managing epidemics, provide drugs and vaccines against Ebola to better prepare for subsequent outbreaks and other public health emergencies. All member countries had some one form of information system but none of them had 100% coverage. Largely, the private sector did not contribute data to the national pool.
Resource Mobilization
The analysis found that there was inadequate financing for P&R domestically even if countries indicated resources were usually mobilized during outbreaks either from partners or National Governments. Most of activities were funded by donors and partners through bilateral arrangements (German cooperation, Agence Française de development) and regional projects such as Regional Disease Surveillance Enhancement Project (REDISSE). The 11 Member States on (REDISSE) each had budget allocations for public health emergencies.
One Health Concept
Almost all member states had One Health structures in place although there were not many supported by formal structures. Only three (3) countries had formal documents on One Health. The Gambia was the only country with a veterinary epidemiology unit and a veterinary epidemiologist working in the unit.
SWOT Analysis of regional P&R capacities for public health emergencies
A SWOT analysis based on findings from the assessment revealed the strengths and weaknesses in regional capacities (
Figure 2). The major threats posed to regional P&R for public health emergencies ranged from insufficient stockpiles, the lack of a budget for public health emergency preparedness to over-reliance on donor partner support for most activities. The analysis also presented opportunities to maximize for capacity strengthening such as the training offered by FETPs and other public health-related training programs in the region, technical assistance from development partners, as well as strong collaborations with other regional structures and international organizations among others.
Discussion


This situational analysis conducted in ECOWAS region reviewed and documented strengths, gaps, and challenges in P&R in Member States. A level of response coordination mechanisms existed in all 15 countries as supported by EOCs. Some EOCs operated virtually but not all were fully functional. Moreover, all countries reported additional criteria to be met for their NPHIs to be fully functional. This is concerning because the national coordinating body should manage EOCs, multi-sectoral committees, technical working groups among others to achieve crisis management and effective communication at all levels and between various sectors[12]. Such coordination and collaboration in response to public health emergencies greatly contribute to its success [18].
The development of formal policies within an enabling legal framework alongside response plans introduce some stability in response[
19] to public health emergencies. The situational analysis indicated that some countries had a legal framework and legislation that supported the implementation of public health emergency P&R although there were no specific guidelines laid out for addressing these events before, during, and after. Relevant legislation in most countries needed revision as they were outmoded. Recent studies have posited that response has been affected by inadequate guidelines for coordination and collaboration among organizations; this is reflected in communication breakdowns, and weak managerial and institutional coordination across federal, state, local, and tribal governments[
20,
21].
Besides, of the 15 countries reviewed, only Nigeria, The Gambia, Guinea, Sierra Leone and Liberia had plans for generic epidemic preparedness. Although there may be challenges in implementing response plans due to the dynamic nature of response involving numerous communications between organizations and individuals leading to decisions beyond the plan,[
22] an effective plan increases the probability of a successful emergency response effort[
23]. More so, beyond a coordination plan, revisions during response to an event are crucial. Findings from an investigation of the response to the 2015 Middle East Respiratory Syndrome Coronavirus (MERS-Cov) in South Korea revealed that although there was a response coordination plan before this event, the multiple revisions and updates during the response could not achieve a good harmony in efforts. Newly emerging relationships among planned actors and several intermediaries between the local and national actors whose roles and relationships were overlooked [
24]. Member States need to factor such dynamics into their plans and revise/update them during implementation in responding to events like the current COVID-19.
Aside the need for updated legislation to support respond coordination locally, there is also the need to develop a regional cross border strategic plan and subsequently a policy to guide formalized routine cross-border meetings between neighbouring countries to review relevant surveillance data and other relevant updates. Early cross-border coordination is critical to controlling epidemics that arise in border regions from pathogens with moderately short generation times[
25].
Developing and expanding surveillance and laboratory preparedness capacities in Member States before an event will substantially contribute to strengthening assessment capabilities that enable “preparedness systems to recognize and characterize a threat, monitor its impact on the population, and evaluate the efficacy of interventions to contain the threat”[
12]. The full implementation of IDSR in Member States increases the likelihood of attaining the required IHR (2005) capacities early as the ultimate aim of this surveillance strategy is to improve public health surveillance and response nationwide. As at 2017, only five (5) Member States namely Benin, Burkina Faso, Cote d´Ivoire, Gambia, Guinea and Guinea-Bissau had achieved full implementation of IDSR [
26]. The current analysis carried out about a year later corroborates this report as countries were found at different stages of implementing IDSR. Most private health facilities were excluded in the reporting coverage and not all member countries had been able to successfully roll out event-based surveillance systems countrywide. An earlier review of the implementation status of IDSR in the African region also reported that event-based surveillance implementation had been inadequate [
26]. However, event-based surveillance plays a key role in accurately identifying outbreaks and affected population groups, and monitoring disease trends as well as the impact of control strategies[
12]. To scale up event-based surveillance, multiple stakeholders and the community must be involved. Also, media scanning should be employed with the aid of information technology products and software[
26].
Surveillance data analysis and reporting is critical in aiding responders to quickly identify potentially affected populations and facilitate rapid decision-making during an event [
27]. It is therefore imperative that routine surveillance data are frequently analysed at lower levels and the electronic real-time reporting systems in countries are enhanced to expand IDSR reporting in Member States. Such efforts can be sustained through mobilization of domestic resources facilitated by advocacy at national and subnational levels, and improved supervision (including electronic) as highlighted by the third edition of the IDSR guidelines [
26].
Generally, the allocation of limited resources for P&R has been a problem. The JEE reports from member countries indicate over-reliance on donors for the provision of laboratory reagents and equipment for the testing of diseases of public health importance [
28-35]. Not all disease conditions were catered for by external funding and internal funding was inadequate hence the stock out of laboratory reagents and consumables, and inadequate equipment as identified by this analysis. The COVID-19 pandemic and previous outbreaks including the West African Ebola outbreak have revealed the challenge in detecting cases due to inadequate testing capacities and the need to develop better mechanisms for specimen and material transport/referral between laboratories and across countries [
36,
37].
Improved specimen collection and transport systems have a direct link to the number of tests performed[
37] and turn-around time. Centralized and decentralized laboratory specimen transport/referral networks have been proposed to reduce turn-around time and retain flexibility for incorporating different specimen types [
38]. Some Member States including Guinea and Burkina Faso have developed national specimen referral policies and piloted their specimen transport systems [
39,
40]. Other countries could learn from their example to also implement effective specimen referral systems. Regional efforts have also been invested into strengthening testing capacity for COVID-19 across Africa[
41]. Countries need to maximize such opportunities and also allocate internal resources alongside develop plans to furnish surges in testing due to public health emergencies as well as ensure continuity of operations for both the short and long term [
27]. The development of an ECOWAS regional strategic plan for improving public health laboratories capacities based on a comprehensive assessment, the identification of regional reference laboratories will permit to strengthen early detection capacities at national level.
For all Member States assessed, there were inadequate numbers of public health personnel especially field epidemiologists and trained frontline healthcare workers to implement IHR core capacity requirements. The deficit in health workforce to tackle outbreaks in the region is a recurring theme in most assessments conducted during and post health events [
42-44]. Field epidemiologists initiate the rapid response process to outbreaks[
45] and CHWs significantly support community engagement in mitigating the impact of health events as they are trusted community members and usually the most accessible point of care[
46]. This is why countries need to engage and train more CHWs to augment the health workforce [
47]. Countries should take advantage of the innovative IDSR eLearning platform to train health workers in disease surveillance [
26]. It is important to also leverage on the field epidemiology training programs (FETPs) in the region to increase the number of competent field epidemiologists. There is evidence of the significant contribution of FETP trainees in responding to the EVD outbreak in the region [
48-50]. These trainees also serve as disease detectives in African Corps of Disease Detectives (ACoDD) that augment rapid response; they even mentor front-line health workers and CHW to respond effectively[
51].
Risk communication constitutes the first set of activities in response to an emergency[
52]. The difficulty encountered in controlling the EVD outbreak had little to do with a significant change of the virus as compared to inadequate surveillance, poor detection of suspected cases, and the community´s poor general understanding about the disease. The severity of the epidemic reflected not only in many deaths but also in the extent of fear, misinformation, and stigma that it created globally. Continued efforts must be invested into culturally appropriate public education and risk communication [
53-56]. Also, countries in the region need to develop stand-alone risk communication plans for response mobilization during epidemics. At the time of assessment, only Liberia had an anthropologist and also implemented a strong rumour control mechanism. The failure to communicate risks and mitigating measures effectively to the public has been tied to the lack of appropriate social science skills, human resources, and communication expertise [
57]. Thus, this gap in skilled personnel to lead risk communication, if not filled quickly, could result in an inadequate response to public health emergencies in the near future.
Research cuts across all aspects of P&R in addressing public health events. The current assessment found some collaborations including sub-regional research on meningitis, Lassa fever, measles, and other zoonotic-related research. It is commendable that four countries (Mali, Guinee, Liberia, and Sierra Leone) had formed a consortium and were investigating drugs and vaccines against Ebola and also to better prepare for subsequent outbreaks. The recent public health emergencies including Ebola and COVID-19 have stimulated investments in research especially clinical trials. A bibliometric study on the first three months of research (January to March 2020) on COVID-19 was performed and scientific contributions were found from 73 countries globally. However, contributions were skewed towards the United States, the United Kingdom, and Italy. Only a few publications from African countries were seen and no country contributed more than 1 publication within the period[
58]. This could be due to the emphasis most countries place on epidemics in their region countries/regions[
59] and only a few cases were recorded in the region at the time this review was conducted. However, it is worthy to note that scientific research played a vital role in characterizing the COVID-19 outbreak and its mitigation[
58]. This should encourage more efforts into producing scientific evidence that is useful to health workers and decision-makers[
60]. Also, community engagement with various stakeholders is crucial to the sustained relevance of research in responding to health emergencies[
61].
The failures and successes in response to public health emergencies over the years have shown that adopting the One Health (OH) approach - multisectoral, and trans-disciplinary collaboration between animal, human, and environmental sectors - by far increases the likelihood of preventing and mitigating the impact of these events in their early stages[
62]. This is because six (6) out of every ten (10) infectious diseases in humans are spread from animals[
63]. Animal, human, and environmental factors have been implicated in the evolution of MERS-CoV[
62] and this is no different for most highly infectious pathogens. Almost all Member States had structures in place to support OH at the time of the analysis although many were not formal. Only three (3) countries had formal documents on OH. The Gambia was the only country with a veterinary epidemiology unit and a veterinary epidemiologist working in the unit. A regional network for OH in West Africa supported by formal documents is crucial to promoting the much-needed multi-sectoral collaboration among Member States for improved public health and sustainable agricultural systems, especially for livestock.
Study Limitations
Only national level stakeholders were engaged in this study.it, however, did not affect the regional approach that the research aimed to achieve. Also, the study did not assess paper-based vs. electronic IDSR reporting. This could be considered in future related research.
Conclusion


The situational analysis of capacities for preparedness and response to public health emergencies has revealed some strengths and weaknesses that should be targeted for improvement. There is the need to establish fully functional National Public Health Institutes and the ECOWAS Regional Centre for Surveillance and Disease Control in countries for effective coordination. Significant strides have been made in implementing IDSR and developing laboratory capacity but there is much left to be done including improving event-based surveillance and establishing effective specimen referral/transport systems. The deficit in health workforce needs urgent attention in the region to facilitate the training of field epidemiologists and the recruitment of public health workers. Research collaborations in the region are encouraging and should be expanded to fully incorporate the one health approach. Country efforts in strengthening preparedness capacities and response capabilities should be supported by updated legislations to ensure rapid and effective response to public health events. Also, Member States need to provide more local funds through dedicated budgetary allocations to strengthen their health systems.
What is known about this topic
- ECOWAS region has seen several epidemics of infectious diseases
- These health crises have exposed shortcomings in national and regional health systems
What this study adds
- Most countries were at different stages of implementing Integrated Disease Surveillance and Response
- Laboratory testing capacity in the region is inadequate
- The study provides a regional perspective on areas that require strengthening including health workforce, legislations and local funding to strengthen preparedness and response.
Competing interests


Authors declare no competing interest
Authors' contributions


Conceptualisation: VL, DAB, KMN, IS, EK. Data collection: VL, DAB, KMN, IS, EMO, EK. Report writing: VL, DAB, KMN, IS, EMO, EK. Drafting manuscripts: VL, EEK, DAB, KMN, IS, EMO, EK. Finalising manuscript: VL, EEK, DAB, KMN, IS, EMO, EK. All authors read the final version of the manuscript.
Acknowledgments


We would like to acknowledge all institutions who participated and assisted us through the data collection process.
Tables and figures


Table 1: Eligibility criteria of documents
Table 2: Documents included in desk review
Table 3: Points of assessment for strengths, gaps and challenges in preparedness and response to epidemics
Figure 1: Analysis framework for public health emergency P&R capacity assessment
Figure 2: SWOT analysis of public health emergency preparedness and response capacities in the ECOWAS region
References


- World Health Organization (WHO). Lassa Fever - Nigeria. WHO. 2018. Accessed Sept 2020.
- World Health Organization (WHO). Rift Valley fever - Gambia. WHO. 2018. Accessed Sept 2020.
- Africanews. WHO assists Ghana to deal with meningitis outbreak. Africanews. 2018. Accessed Sept 2020.
- Baize S, Pannetier D, Oestereich L, Rieger T, Koivogui L, Magassouba N, Soropogui B, Sow MS, Keïta S, De Clerck H, Tiffany A, Dominguez G, Loua M, Traoré A, Kolié M, Malano ER, Heleze E, Bocquin A, Mély S, Raoul H, Caro V, Cadar D, Gabriel M, Pahlmann M, Tappe D, Schmidt-Chanasit J, Impouma B, Diallo AK, Formenty P, Van Herp M, Günther S. Emergence of Zaire Ebola virus disease in Guinea. N Engl J Med. 2014;371(15):1418-25. https://doi.org/10.1056/nejmoa1404505
- World Health Organization (WHO). Ebola outbreak 2014-2015. WHO. 2018. Accessed Aug 2020.
- Amimo F, Lambert B, Magit A. What does the COVID-19 pandemic mean for HIV, tuberculosis, and malaria control? Trop Med Health. 2020 May 13;48:32.https://doi.org/10.1186/s41182-020-00219-6 PubMed | Google Scholar
- Bigg MM, Kpodo K. Ghana petrol station blast, flooding leave estimated 150 dead. Reuters. 2015. Accessed Dec 2020.
- The Watchers. More than 50 houses swept away into Cross River, Nigeria. The Watchers. 2017. Accessed Dec 2020.
- Arsenault C. Drought, expanding deserts and “food for jihad” drive Mali´s conflict. Reuters. 2015. Accessed Dec 2020.
- Jenner L. Fires Cover Large Portions of West Africa. NASA. 2016 Accessed Dec 2020.
- World Health Organization (WHO). International health regulations (2005). WHO. 2008. Accesssed Sept 2022.
- Stoto MA, Nelson C, Savoia E, Ljungqvist I, Ciotti M. A Public Health Preparedness Logic Model: Assessing Preparedness for Cross-border Threats in the European Region. Heal Secur. 2017 Oct; 15(5):473-82.https://doi.org/10.1089/hs.2016.0126 . Google Scholar
- Tricco AC, Lillie E, Zarin W, O´Brien KK, Colquhoun H, Levac D, Moher D, Peters MDJ, Horsley T, Weeks L, Hempel S, Akl EA, Chang C, McGowan J, Stewart L, Hartling L, Aldcroft A, Wilson MG, Garritty C, Lewin S, Godfrey CM, Macdonald MT, Langlois EV, Soares-Weiser K, Moriarty J, Clifford T, Tunçalp Ö, Straus SE. PRISMA extension for scoping reviews (PRISMA-ScR): Checklist and explanation. Ann Intern Med. 2018 Oct 2; 169(7):467-73.https://doi.org/10.7326/M18-0850 . Google Scholar
- Arksey H, O´Malley L. Scoping studies: Towards a methodological framework. Int J Soc Res Methodol Theory Pract. 2005; 8(1):19-32.https://doi.org/10.1080/1364557032000119616 . Google Scholar
- Levac D, Colquhoun H, O'Brien KK. Scoping studies: advancing the methodology. Implement Sci. 2010 Sep 20; 5:69.https://doi.org/10.1186/1748-5908-5-69 PubMed | Google Scholar
- Peters M, Godfrey C, McInerney P, Munn Z, Tricco A, Khalil H. Chapter 11: Scoping reviews. In: Aromataris E, Munn Z, editors. JBI Manual for Evidence Synthesis. 2020 versi. JBI. 2020. Accessed Jun 2022.
- PREDICT, Preparedness&Response. The role of environment in one health and national health security. One health in action, USAID. 2015 Accessed May 2021.
- Kapucu N, Demiroz F. Interorganizational Networks in Disaster Management. In: Social Network Analysis of Disaster Response, Recovery, and Adaptation. Butterworth-Heinemann. 2017: 25-39.https://doi.org/10.1016/B978-0-12-805196-2.00003-0 . Google Scholar
- Robinson SE, Eller WS, Gall M, Gerber BJ. The Core and Periphery of Emergency Management Networks. Public Manag Rev. 2013; 15(3):344-62.https://doi.org/10.1080/14719037.2013.769849 . Google Scholar
- Gorman L, Stoney C. Missed Opportunities: Public Health Disaster Management in Canada. J Public Manag Soc Policy. 2015; 22(2):6. Google Scholar
- Hodge JG, Gostin LO, Vernick JS. The Pandemic and All-Hazards Preparedness Act: improving public health emergency response. JAMA. 2007 Apr 18; 297(15):1708-11.https://doi.org/10.1001/jama.297.15.1708 Google Scholar
- Brooks JM, Bodeau D, Fedorowicz J. Network Management in Emergency Response: Articulation Practices of State-Level Managers-Interweaving Up, Down, and Sideways. Adm Soc. 2012 Oct; 45(8):911-48.https://doi.org/10.1177/0095399712445874 . Google Scholar
- Steigenberger N. Organizing for the Big One: A Review of Case Studies and a Research Agenda for Multi-Agency Disaster Response. J Contingencies Cris Manag. 2016 Jun 1; 24(2):60-72. https://doi.org/10.1111/1468-5973.12106 . Google Scholar
- Kim Y, Ku M, Oh SS. Public health emergency response coordination: putting the plan into practice. J Risk Res. 2020 Aug 2; 23(7-8):928-44.https://doi.org/10.1080/13669877.2019.1628092 . Google Scholar
- Ferguson NM, Cummings DA, Cauchemez S, Fraser C, Riley S, Meeyai A, Iamsirithaworn S, Burke DS. Strategies for containing an emerging influenza pandemic in Southeast Asia. Nature. 2005 Sep; 437(7056):209-14.https://doi.org/10.1038/nature04017 . Google Scholar
- Fall IS, Rajatonirina S, Yahaya AA, Zabulon Y, Nsubuga P, Nanyunja M, Wamala J, Njuguna C, Lukoya CO, Alemu W, Kasolo FC, Talisuna AO. Integrated Disease Surveillance and Response (IDSR) strategy: current status, challenges and perspectives for the future in Africa. BMJ Glob Health. 2019 Jul 3; 4(4):e001427.https://doi.org/10.1136/bmjgh-2019-001427 PubMed | Google Scholar
- Centers for Disease Control and Prevention (CDC). Public health emergency preparedness and response capabilities. Atlanta, GA: US Department of Health and Human Services. 2018. Accessed June 2022.
- World Health Organization (WHO). Joint external evaluation of IHR core capacities of the Republic of Benin. WHO. 2018. Accessed Sept 2020.
- World Health Organization (WHO). Joint External Evaluation of IHR core capacities of the Republic of Côte d´Ivoire. WHO. 2017. Accessed Sept 2020.
- World Health Organization (WHO). Joint External Evaluation of IHR Core Capacities of the Republic of The Gambia. WHO. 2017. Accessed Sept 2020.
- World Health Organization (WHO). Joint External Evaluation of IHR Core Capacities of the Republic of Ghana. WHO. 2017. Accessed Sept 2020.
- World Health Organization (WHO). Joint External Evaluation of IHR core capacities of the Republic of Liberia. WHO. 2017. Accessed Sept 2020.
- World Health Organization (WHO). Joint External Evaluation of IHR core capacities of the Federal Republic of Nigeria. WHO. 2017. Accessed Sept 2020.
- World Health Organization (WHO). Joint External Evaluation of IHR Core Capacities of the Republic of Sierra Leone. WHO. 2017. Accessed Sept 2020.
- World Health Organization (WHO). Joint External Evaluation of IHR Core Capacities of the Republic of Senegal. WHO. 2017. Accessed Sept 2020.
- Osseni IA. COVID-19 pandemic in sub-Saharan Africa: preparedness, response, and hidden potentials. Trop Med Health. 2020 Jun 17;48:48.https://doi.org/10.1186/s41182-020-00240-9 PubMed | Google Scholar
- Sealy TK, Erickson BR, Taboy CH, Ströher U, Towner JS, Andrews Sharon E, Rose LE, Weirich E, Lowe L, Klena JD, Spiropoulou CF, Rayfield MA, Bird BH. Laboratory response to Ebola - West Africa and United States. MMWR Suppl. 2016; 65(3):44-9.http://dx.doi.org/10.15585/mmwr.su6503a7 Google Scholar
- Fonjungo PN, Alemnji GA, Kebede Y, Opio A, Mwangi C, Spira TJ, Beard RS, Nkengasong JN. Combatting Global Infectious Diseases: A Network Effect of Specimen Referral Systems. Clin Infect Dis [Internet]. 2017 Mar 15; 64(6):796-803.https://doi.org/10.1093/cid/ciw817 . Google Scholar
- Standley CJ, Muhayangabo R, Bah MS, Barry AM, Bile E, Fischer JE, Heegaard W, Koivogui L, Lakiss SK, Sorrell EM, VanSteelandt A, Dahourou AG, Martel LD. Creating a National Specimen Referral System in Guinea: Lessons From Initial Development and Implementation. Front Public Heal. 2019 Apr 16 ;7:83. https://doi.org/10.3389/fpubh.2019.00083. Google Scholar
- Dama E, Nikiema A, Nichols K, Bicaba BW, Porgho S, Greco Koné R, Tarnagda Z, Cissé A, Ngendakumana I, Adjami A, Medah I, Ake F, Mirza SA. Designing and Piloting a Specimen Transport System in Burkina Faso. Health Secur. 2020 Jan;18(S1):S98-S104. https://doi.org/10.1089/hs.2019.0068 PubMed | Google Scholar
- Africa Centers for Disease Control and Prevention (ACDC). AU and Africa CDC launch partnership to accelerate COVID-19 testing: Trace, Test and Track. Africa CDC. 2020. Accessed Dec 2020.
- Shoman H, Karafillakis E, Rawaf S. The link between the West African Ebola outbreak and health systems in Guinea, Liberia and Sierra Leone: a systematic review. Global Health. 2017 Jan 4;13(1):1.https://doi.org/10.1186/s12992-016-0224-2 PubMed | Google Scholar
- Ballard M, Westgate C. COVID19: it ain´t over until there´s PPE all over. Think Global Health. Accessed Dec 2020.
- Human Rights Watch. Africa: COVID-19 exposes healthcare shortfalls. Human Rights Watch. 2020. Accessed Dec 2020.
- Nsubuga P. The Ebola outbreak in West Africa: a story of related public health challenges and a pointer to solutions to mitigate the inevitable next outbreak. Pan Afr Med J. 2014 Sep 22;19:48.https://doi.org/10.11604/pamj.2014.19.48.5336 PubMed | Google Scholar
- Nepomnyashchiy L, Dahn B, Saykpah R, Raghavan M. COVID-19: Africa needs unprecedented attention to strengthen community health systems. Lancet. 2020;396(10245):150-2.http://dx.doi.org/10.1016/S0140-6736(20)31532-4 . Google Scholar
- Ajisegiri WS, Odusanya OO, Joshi R. COVID-19 outbreak situation in Nigeria and the need for effective engagement of community health workers for epidemic response. Glob Biosecurity. 2020;1(4).http://doi.org/10.31646/gbio.69 . Google Scholar
- Shuaib F, Gunnala R, Musa EO, Mahoney FJ, Oguntimehin O, Nguku PM, Nyanti SB, Knight N, Gwarzo NS, Idigbe O, Nasidi A, Vertefeuille JF; Centers for Disease Control and Prevention (CDC). Ebola virus disease outbreak - Nigeria, July-September 2014. MMWR Morb Mortal Wkly Rep. 2014 Oct 3; 63(39):867-72. PubMed | Google Scholar
- Lubogo M, Donewell B, Godbless L, Shabani S, Maeda J, Temba H, Malibiche TC, Berhanu N. Ebola virus disease outbreak; the role of field epidemiology training programme in the fight against the epidemic, Liberia, 2014. Pan Afr Med J. 2015 Oct 10; 22 Suppl 1(Suppl 1):5. https://doi.org/10.11694/pamj.supp.2015.22.1.6053 PubMed | Google Scholar
-
Ohuabunwo C, Ameh C, Oduyebo O, Ahumibe A, Mutiu B, Olayinka A, Gbadamosi W, Garcia E, Nanclares C, Famiyesin W, Mohammed A, Nguku P, Koko RI, Obasanya J, Adebayo D, Gbadegesin Y, Idigbe O, Oguntimehin O, Nyanti S, Nzuki C, Abdus-Salam I, Adeyemi J, Onyekwere N, Musa E, Brett-Major D, Shuaib F, Nasidi A. Clinical profile and containment of the Ebola virus disease outbreak in two large West African cities, Nigeria, July-September 2014. Int J Infect Dis. 2016;53:23-9.https://doi.org/10.1016/j.ijid.2016.08.011 . Google Scholar
- Masiira B, Antara SN, Kazoora HB, Namusisi O, Gombe NT, Magazani AN, Nguku PM, Kazambu D, Gitta SN, Kihembo C, Sawadogo B, Bogale TA, Ohuabunwo C, Nsubuga P, Tshimanga M. Building a new platform to support public health emergency response in Africa: the AFENET Corps of Disease Detectives, 2018-2019. BMJ Glob Health. 2020 Oct; 5(10):e002874.https://doi.org/10.1136/bmjgh-2020-002874 PubMed | Google Scholar
- Bedrosian SR, Young CE, Smith LA, Cox JD, Manning C, Pechta L, Telfer JL, Gaines-McCollom M, Harben K, Holmes W, Lubell KM, McQuiston JH, Nordlund K, O´Connor J, Reynolds BS, Schindelar JA, Shelley G, Daniel KL. Lessons of Risk Communication and Health Promotion – West Africa and United States. MMWR Suppl. 2016 Jul 8; 65(3):68-74.http://dx.doi.org/10.15585/mmwr.su6503a10 Google Scholar
- World Health Organization (WHO). One year into the Ebola epidemic: a deadly, tenacious and unforgiving virus. WHO. 2015. Accessed Dec 2020.
- Marzi A, Feldmann F, Hanley PW, Scott DP, Günther S, Feldmann H. Delayed Disease Progression in Cynomolgus Macaques Infected with Ebola Virus Makona Strain. Emerg Infect Dis. 2015 Oct; 21(10):1777-83.https://doi.org/10.3201/eid2110.150259 PubMed | Google Scholar
- Spengler JR, Ervin ED, Towner JS, Rollin PE, Nichol ST. Perspectives on West Africa Ebola Virus Disease Outbreak, 2013-2016. Emerg Infect Dis. 2016 Jun; 22(6):956-63.https://doi.org/10.3201/eid2206.160021 PubMed | Google Scholar
- Rhoads SJ, Bush E, Haselow D, Vyas KS, Wheeler JG, Faulkner A, Lowery C. Mobilizing a Statewide Network to Provide Ebola Education and Support. Telemed e-Health. 2016 Feb; 22(2):153-8.https://doi.org/10.1089/tmj.2015.0011 . Google Scholar
- Bastide L. Crisis communication during the Ebola outbreak in West Africa: The paradoxes of decontextualized contextualization. In: Bourrier M, Bieder C, editors. Risk Communication for the Future: Towards Smart Risk Governance and Safety Management. Switzerland: Springer International Publishing; 2018. p 95-108. Google Scholar
- Nowakowska J, Sobocińska J, Lewicki M, Lemańska Ż, Rzymski P. When science goes viral: The research response during three months of the COVID-19 outbreak. Biomed Pharmacother. 2020 Sep;129:110451.https://doi.org/10.1016/j.biopha.2020.110451 PubMed | Google Scholar
- Zhang L, Zhao W, Sun B, Huang Y, Glänzel W. How scientific research reacts to international public health emergencies: a global analysis of response patterns. Scientometrics. 2020;124(1):747-773.https://doi.org/10.1007/s11192-020-03531-4 Epub 2020 Jun 9. PMID: 32836522; PMCID: PMC7282204.. PubMed | Google Scholar
- Dagenais C, Somé TD, Boileau-Falardeau M, McSween-Cadieux E, Ridde V. Collaborative development and implementation of a knowledge brokering program to promote research use in Burkina Faso, West Africa. Glob Health Action. 2015 Jan 27; 8:26004.https://doi.org/10.3402/gha.v8.26004 PubMed | Google Scholar
- Folayan MO, Peterson K, Kombe F. Ethics, emergencies and Ebola clinical trials: the role of governments and communities in offshored research. Pan Afr Med J. 2015 Oct 10;22 Suppl 1(Suppl 1):10.https://doi.org/10.11694/pamj.supp.2015.22.1.6216 PubMed | Google Scholar
- Zumla A, Dar O, Kock R, Muturi M, Ntoumi F, Kaleebu P, Eusebio M, Mfinanga S, Bates M, Mwaba P, Ansumana R. Taking forward a ‘One Health’approach for turning the tide against the Middle East respiratory syndrome coronavirus and other zoonotic pathogens with epidemic potential. International Journal of Infectious Diseases. 2016 Jun 1; 47:5-9.https://doi.org/10.1016/j.ijid.2016.06.012 . Google Scholar
- CDC. One Health. CDC. Accessed Dec 2020.