Epidemiological Characteristics of Novel Coronavirus Disease (COVID-19) in Mombasa County, Kenya 2020
Josphat Kimani Maina1,2,3,&, Moses Melita1,2, Stephen Mutiso1,2, Fredrick Ouma1,2, Sora Jattani1,2, Stella Mmochi1,2, Fredrick Odhiambo1, Ahmed Abade1, Waqo Boru1, Maria Nunga1, Josephine Githaiga1, Elvis Oyugi1, Maurice Owiny1,4
1Kenya Field Epidemiology Training Program, Nairobi Kenya, 2School of Public Health, Moi University, Kenya, 3Zoonotic Diseases Unit, Nairobi, Kenya, 4African Field Epidemiology Network, Nairobi, Kenya
&Corresponding author
Josphat Kimani Maina, Kenya Field Epidemiology and Laboratory Training Programme, Ministry of Health, Kenyatta National Hospital Grounds, Nairobi, Kenya. jkimaina@gmail.com
Introduction:
Mombasa County had, as of April 1, 2020, reported four confirmed COVID-19 cases. There were possibilities of local transmission since most of the cases were reported in densely populated urban areas. We described the epidemiological characteristics of COVID-19 cases in Mombasa County.
Methods:
Standard case definitions were used to review health records of cases that were reported from March 13, 2020, through April 30, 2020, in Mombasa County. We performed descriptive analyses on demographics, case fatality rates, geo-temporal viral spread, epidemic curve, and key subgroups.
Results:
A total of 2,835 suspected cases and 126 confirmed cases (Positivity Rate=4.4%) observed over 1402 person-days were identified. The first case was identified in Nyali sub-county in late March 2020, and by April 20, 2020, all six sub-counties had reported cases. Among confirmed cases, 109 (87%) were aged 20–69 years, 58 (45.8%) were from Mvita Sub-county, and 108 (86.5%) were asymptomatic. Health workers and port workers accounted for 14 (11.1%) and 15 (11.9%) of the confirmed cases respectively. There were ten deaths (Case Fatality Rate=7.9%) observed over 1402 person-days with 0.071 mortalities per 10 person-days. Case Fatality Rate among Persons aged >70 years was 75%. The epidemic curve indicated a propagated mode of transmission.
Conclusion:
The Spread of infections took about 20 days from Nyali Sub-county to the other six sub-counties. Although a below 5% positivity rate had been achieved, the epidemic appeared to be on the rise in the lead up to April 30, 2020. Development/strengthening of community event-based surveillance and a rapid mortality surveillance system was recommended.
Introduction

Early case detection and isolation of patients infected with highly infectious diseases is crucial for timely initiation of case management and control of further transmission of the disease within the population at risk [1]. Active case finding is a systematic search for cases of an infectious disease using a standardized case definition and has been used in infectious diseases such as poliomyelitis and was effectively employed in containing the Ebola Virus Disease (EBV) outbreak in Nigeria [2]. This approach is effective in capturing all the cases as many may not have access to a healthcare facility or may seek alternative care elsewhere [3]. Persistence of undetected cases in the community sustains infectious disease transmission chains and hence delayed outbreak control [4].
The first human cases of coronavirus disease of 2019 (COVID-19) were reported in Wuhan City, China, in December 2019 caused by a novel coronavirus named severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2). Two months later (end of January 2020), more than two hundred countries worldwide reported laboratory-confirmed cases of COVID-19. As of July 27, 2020, a total of 16,264,048 cases and 648,966 deaths (Case Fatality Rate 3.9%) had been reported globally [
5]. The emergence and detection of the novel respiratory pathogen was shrouded in uncertainty over its virulence, transmissibility, virological, clinical, and other epidemiological characteristics in the human population.
The loss of lives, disruption of societies, and devastation of economies associated with the 1918 influenza pandemic and other influenza pandemics during the 20th and early 21st century led the international scientific community to start predicting and preparing for future pandemics with a particular focus on improving the public health means of that time. Despite advances in scientific understanding of viruses of pandemic potential, it was still unknown where and when the next pandemic would strike, and which virus would be responsible. As some experts had predicted, the current pandemic originated from Asia, was not caused by influenza but by a novel ?-coronavirus. The International Committee on Taxonomy of Viruses adopted “severe acute respiratory syndrome coronavirus 2 (SARS-CoV2)” as its official name on February 11, 2020 [
6]. Contact and droplets were identified as the main routes of transmission. The majority of infections, up to 80%, are asymptomatic or mild. The disease has a wide range of clinical presentations with the majority of cases presenting as a febrile respiratory illness of sudden onset. While most people develop an only mild illness, approximately 14% develop severe disease. COVID-19 patients that progress to necessitate hospital care and oxygen supplementation are classified as severe. About 5% of severe cases deteriorate to require intensive care [
7]. The incubation period extends to fourteen days, the average being 4-5 days. It is estimated that 97.5% of symptomatic cases develop symptoms within 11.5 days of exposure [
8].
COVID-19 infection rates are equal between men and women. However, the proportion that progress to require hospital care, oxygen supplementation, intensive care, and even death is twofold greater for men than women [
9]. The COVID-19 infection has been reported across all age groups. People with underlying chronic medical conditions (all ages) and the elderly are at a higher risk of progressing to severe disease [
10]. While the estimated overall case fatality rates vary across countries, fatality is consistently highest among those with underlying comorbidities and the elderly aged >80 years. While several trials were still ongoing, there were no drugs or vaccines licensed for the treatment or prevention of COVID-19 at the time of this investigation [
11].
Egypt reported the first COVID -19 case in Africa on February 14, 2020, a 33-year-old male of foreign national. Algeria confirmed the second case on February 25, 2020, an Italian adult. About a month later (March 2020), most countries across the continent had confirmed COVID-19 cases within their territories. The transmission pattern in Africa mirrored that reported globally, with the first confirmed cases being imported/travel-related followed by widespread community transmission[
12]. Two months after confirming the first case, African countries were reporting up to thousands of cases and hundreds of deaths. Many additional infections were thought to have been unidentified due to poor health seeking behavior, lack of capacity and under-reporting [
13]. While documented new cases and reported deaths remained low in Africa compared with other hard-hit continents, numbers were rising steadily, and fears of a major humanitarian crisis was looming large due to the continent´s limited public health means [
13].
On March 12, 2020, Kenya reported the first positive case less than a month after the first case was reported in the African continent [
14]. Like the rest of the world, this was a travel related case who had traveled to Kenya from the United States of America via the United Kingdom, both of which were among the high disease burden countries at that time [
14]. Despite the entry screening measures applied at the airports and other ports of entry, this first case slipped through only to be detected seven days post-arrival [
15]. As of July 27, 2020, a total of 17,535 cases had been confirmed with 280 deaths i.e., case fatality rate of 1.6% percent [
16]. The majority, 16,989 (97%), were local community transmission cases and 546 (3%) were imported cases. Forty-four counties (93.6%) had reported cases with Nairobi reporting 10,249 (60.3%) and Mombasa reporting 1952 (11.5%) cases. Nairobi and Mombasa Counties had attack rates of 233.1 and 161.5 per 100,000 population respectively [
16].
As of April 1, 2020, Mombasa County reported four confirmed cases, three of them being local transmission cases [
17]. Fears were mounting of a major humanitarian crisis if transmission accelerated in a densely populated county (density of 5495 per km2). At the time of this investigation there were many unknowns which included, the extent of the spread, severity, viral dynamics among others. We sought to attain an early understanding of key County specific epidemiological characteristics of COVID-19 in Mombasa County to guide in the formulation and deployment of targeted public health containment measures to minimize morbidity, loss of life and disruption of society.
Methods


Investigation site
Mombasa County is in the South-Eastern of the Kenyan Coast region. It is the second-largest city in Kenya after Nairobi, despite being the smallest county among Kenya´s 47 counties in landmass. The Population Census report of 2019 indicated that Mombasa had an estimated population of 1,208,333 persons and was the second-most densely populated county in Kenya after Nairobi with a density of 5,495 persons per km2 [
18]. It borders two counties, i.e., Kilifi County on the North, Kwale County located to the South-East, and to the East is the Indian Ocean. It is home to the largest seaport in East Africa and an international airport. Cultural diversity and coastal location make Mombasa a major attraction for local, regional, and global tourists. The county is mainly urban and peri-urban with both settings constituting 98% of its entire population. Mombasa is a cosmopolitan city attracting many people from far and wide looking for investment, employment, and education opportunities [
18]. There are six administrative sub-counties, i.e., Changamwe, Jomvu, Kisauni, Nyali, Likoni, and Mvita.
Investigation design
We employed both passive and active case detection strategies from epi-week 12 of 2020 up to epi-week 18 of 2020 through screening of patients presenting at healthcare facilities and follow-up (contact tracing) of persons known to have had contact with a confirmed case and by inviting key informants to report all possible alert cases for follow up. Active case search targeted high-risk groups, special groups, vulnerable groups, and geographic hotspots. Standardized working/contact definitions and case investigation forms were adopted from the Ministry of Health:
Suspect case: Any person presenting with sudden onset of fever and/or respiratory-related symptoms (e.g., cough/ shortness of breath) whether or not that person had traveled to a foreign country during the fourteen days prior to onset of symptoms or having a history of contact with a probable or a COVID-19 laboratory-confirmed case during the past 14 days before the onset of symptoms, OR any person with sudden onset of respiratory illness that requires hospitalization without an alternative explanation of the presentation.
Probable case: A case that met the suspect case definition but whose COVID-19 test had not been done OR whose COVID-19 test results were not conclusive.
Confirmed case: Any person with a positive COVID-19 test result, regardless of the clinical presentation.
Nasopharyngeal and oropharyngeal swab samples were collected from persons meeting the suspect case definition for PCR testing. Contacts of confirmed cases were identified and followed up in quarantine facilities for 14 days. “A contact was defined as any person who experienced any COVID-19 exposure during the 2 days before and the 14 days after the onset of symptoms of a confirmed case. Such a contact could be a person working together closely or sharing the same environment with a COVID-19 confirmed case or having had face-to-face contact within 1 meter and for more than 15 minutes with a confirmed case.”
Data Source
We used a standardized MOH Case Investigation Form (CIF) to collect data and specimen from all persons who met the case definitions. Data captured included patient information, clinical information, exposure information, travel information, and laboratory information. Investigations targeted health facilities, high-risk groups, special groups, vulnerable groups, and geographic hotspots. The data was immediately uploaded to a national EMR system and specimens transported to approved laboratories. Laboratory diagnostics for COVID-19 was based on nucleic acid amplification tests (NAAT) that detect RNA. All test results, whether positive or negative, were reported within 24 hours to the head of National Public Health Laboratories using the Daily COVID-19 Laboratory Results Submission Template as per the laboratory testing algorithm for verification. The NPHL consolidated and cleaned all results from designated testing laboratories to remove duplicates using national identification numbers as the unique identifiers, Head of NPHL then submitted the consolidated report to the Public Health Emergency Operations Center (PHEOC), where the EMR system was updated with the test result to make a complete line list. Any necessary additional information was obtained through telephone calls, hospital records reviews or physical interviews with the cases and updated accordingly. We then extracted a single dataset of all COVID-19 records from the EMR System as of April 30, 2020 with all personal identifying information expunged.
Variables collected
Case information was collected at the time of sample collection and entered into the EMR System.
Patients who had any kind of active employment in a health facility categorized as health workers.
Persons with a history of foreign travel 14 days prior to either onset of symptoms or the date of positive PCR test for asymptomatic cases were categorized as imported cases. The patients´ underlying comorbid conditions were determined by their self-reported medical history. Symptom severity was classified as either asymptomatic, mild, or severe. Asymptomatic included confirmed cases with no presenting symptoms. Mild cases included those presenting with cough and/or fever but without dyspnea. Severe cases were characterized by dyspnea.
The date of onset used in development of epidemiological curves was defined as the patient´s self-reported start date of either fever or cough during the investigation. Cases that met the case definitions were classified as suspected or confirmed and as asymptomatic or symptomatic. Confirmation of cases was based on positive PCR test results on nasopharyngeal and/or oral pharyngeal swab samples. Diagnosis of suspected cases was based on clinical symptoms and exposure history. Asymptomatic cases were defined as confirmed cases but not presenting with any of the known COVID-19 symptoms.
The date of PCR confirmation was used as the onset date for asymptomatic cases.
Data Analysis
Descriptive statistics were used to summarize demographic and clinical information. Graphs on age distribution were constructed using patient´s declared age at the time of sample collection for confirmed cases. Sex ratio (male: female) and case fatality rates (total deaths divided by total cases, expressed as a percent) were calculated. An estimate of the actual time at risk (person days - PD) was used to summarize the observed time. Mortality (number of deaths divided by observed time) was calculated and expressed per 10 PD. Geo-temporal distribution of cases by sub county was mapped as of March 31, 2020; April 10, 2020; April 20, 2020; and April 30, 2020. QGIS Desktop software (version 2.18.19) was used for mapping. A stacked epidemiological curve for confirmed, asymptomatic, mild, and severe cases was plotted (y-axis - number of cases, x-axis - date of symptom onset) to present cases over time. Separate epidemiological curves were used to analyze all confirmed health workers and seaport workers.
Ethical considerations
This investigation was conducted as response to a public health emergency. Authorization was granted by the Ministry of Health and the County department of public health in Mombasa County. Verbal consent was sought to collect data and swab samples from suspected cases. Collected data was de-identified to guard patient privacy and confidentiality.
Results


Description of people tested for COVID-19
As of April 30, 2020, a total of 2,835 COVID -19 tests had been conducted in Mombasa County
Table 1. Laboratory test results for 126 cases were positive giving a positivity rate of 4.4%. Males accounted for 1,655 (58.4%) while 1,177(41.5%) were female with a variant sex proportion among all sub counties. Suspected cases were across all aged groups. Persons above 35 years old accounted for 79% (35-44 years old = 31.1% (882), 45-54 years old = 24% (679), 55-64 years old = 15.6 % (441), ?65 years old = 8.4% (238). The proportion of suspected cases aged <35 years was 13.3% (25-34 years = 7.9% (225), 15-24 years = 3.6% (102), 5-14 years = 1.8% (51).
All the six sub-counties in Mombasa reported suspected cases; Mvita Sub-county had 45.8% (1,299/2,835), Kisauni had 411(14.5%), Nyali 386(13.6%) while each of the other three sub-counties accounted for less than 10%. Asymptomatic cases were 2,575 (90.9%), 83 (2.2%) were symptomatic and 177 (6.9%) records had missing data. History of travel had the highest proportion of missing data at 61% (1730), other missing variables included age at 6.7% (191), symptom status at 6.2% (177), laboratory test results at 4.5% (127), sub county at 3.6% (101) and sex at 0.1% (3). Pending laboratory test results accounted for 19.7% (558).
Description of all COVID-19 polymerase chain reaction (PCR) positive cases
A total of 126 COVID-19 cases had been confirmed as of April 30, 2020 by four approved laboratories i.e. 106 (84%) were confirmed at the Medical Research Institute in Kilifi, 12 (10%) at the National Influenza Centre in Nairobi, 6 (5%) at an accredited private laboratory, and 2 (2%) at the Medical Research Institute in Nairobi. The detailed description of all COVID-19 PCR positive cases (n=126) is outlined in Table 2. Majority of the confirmed cases (26.2%) were aged between 35 and 44 years, females were 52%, staff working at the port were 11%, and those diagnosed in Mvita Sub-county were 52%. Some patients reported travel-related exposures (13%) and most cases (68%) were classified as asymptomatic, 18.3% as mild, and 13.5% as severe
Table 2.
Description of all Deaths, overall Case Fatality Rates, and Mortality per 10 person-days
A total of 10 deaths among the 126 confirmed cases were reported. The deaths accounted for a case fatality rate (CFR) = 7.9% as shown in
Table 2. The 10 deaths were reported over1402 person-days (PD) of total time observed. Overall mortality rate was 0.071 deaths per 10 PD. Persons aged ?70 years reported the highest case fatality rate at 75%. Males and women had a case fatality rate of 10% and 6.1% respectively. Mvita sub-county reported the highest a case fatality rate of 12.3%, Nyali sub-county had 6.3% and Kisauni sub-county had 4.8%. Cases with no history of any underlying medical conditions registered a case fatality rate of 2.6%, while patients with diabetes, HIV, and hypertension had mortality rates of 2.857 per 10 PD, 2.222 Per 10 PD, and 2.857 per 10 PD, respectively in
Table 3.
Age Distribution and Sex Ratio for Mvita Sub County compared to Mombasa County
Mvita Sub-County had most cases in terms of the overall age distribution of cases in Mombasa County
Figure 1. Persons aged between 20 and 69 years in the entire county accounted for a proportion of
87%. The same age group accounted for 84% of the cases in Mvita Sub-County. Extremes of age, i.e., 0-
9 years and >80 years accounted for 3% and 1 % in Mombasa County and 3%and 2% in Mvita Sub-County respectively. The female to male ratio for Mombasa County and Mvita Sub County was 1.1:1 and 1.17:1 respectively.
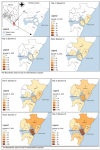
Spatial-Temporal Distribution of Cases
The first COVID-19 case in Mombasa County was confirmed on March 20, 2020, in Nyali Sub-County.
As of March 31, 2020, four Sub-Counties had confirmed 14 PCR positive cases i.e., Nyali (6), Mvita (4), Kisauni (2), and Changamwe (2). Between April 1, 2020, and April 10, 2020, Likoni and Jomvu sub counties reported their first COVID-19 cases. Thus, 32 COVID-19 cases had been reported from all six sub-counties by April 10, 2020, with Mvita and Nyali Sub counties accounting for 71.9% of the cases
Figure 2. As of April 20, 2020, all six Sub Counties had reported 73 PCR positive cases with Mvita reporting 33 (45.2%), Kisauni 15(20.6%), and Nyali 12 (16.4%). A total of 126 cases had been reported as of April 30, 2020, distributed as follows: Mvita 65(52%), Kisauni 21(17%), Nyali 16(13%), Likoni 11(9%), Changamwe 10(8%) and Jomvu 3 (2%). The geo-temporal spread by Epi week is presented in
Figure 2.
Epidemiological Curve
The first case with mild symptoms was reported on March 20, 2020, while the first case presenting with severe symptoms was reported on March 21, 2020. Confirmation of more COVID -19 cases continued throughout the investigation period, with most cases being asymptomatic. The epidemic curve indicated a propagated pattern with several peaks. Three successive waves were demonstrated with the first one peaking on March 31, 2020, the second one peaking on April 20, 2020. The number of cases of the third wave was still on the rise as of April 30, 2020. The highest number of cases that developed symptoms on a single day was 11 on April 20, 2020. The international flights ban was effected on March 25, 2020, restriction on movement in and out of Mombasa County on April 8, 2020, and COVID-19 targeted mass testing initiated on April 16, 2020
Figure 3.
Subgroup Findings
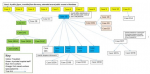
Among the 126 confirmed cases, 15 (11.9%) were port staff and 14 (11.1%) were healthcare workers. The first case at the port was reported on March 21, 2020, while the first health worker was reported on March 26, 2020
Figure 4. The epidemic curve showed multiple peaks indicative of a propagated pattern with a demonstrable rise in reported cases in each successive peak
Figure 5. The highest number of cases reported among port staff on a single day was five and four among healthcare workers. Introduction of targeted mass testing resulted in a rise of COVID - 19 positives cases among these two subgroups (port staff and healthcare workers) across the county. Port workers and health workers were among the groups targeted during mass testing. Asymptomatic cases among port staff were 80%, mild cases were 7%, severe cases were 13% with a 7% case fatality rate. Asymptomatic cases among healthcare workers were 57% while 43% were mild with no severe cases and no fatalities.
Discussion


We gained an early comprehension of the magnitude, trends of spread and other essential characteristics (clinical and epidemiological) of the outbreak in Mombasa County that guided development and deployment of effective public health containment measures. One of the early findings of this 40 days (March 20, 2020 - April 30, 2020) investigation was that both importation and community transmission were driving the spread of the highly contagious disease. This rapid spread saw confirmed cases increase from the initial one sub-county to include all six sub-counties within 20 days. At the time of conducting the activities, the effect of the containment measures instituted by the government could not be documented since their implementation was ongoing. Some of the containment measures included public education on standard precaution (e.g., promotion of hand hygiene, mask-wearing, and physical distancing), ban of international flights, cessation of movement into and out of Mombasa County, Nationwide dusk to dawn curfew, ban of congressional meetings, closure of all schools and higher learning institutions. These measures could contribute to slowing down a rapidly spreading pandemic and achievement of the WHO recommended below 5% positivity rate in a medium-income country and densely populated, predominantly urban, and peri-urban county[19].
Among all the deaths, a majority were in the advanced age group (≥70 years old) who had been battling various underlying chronic conditions including diabetes, hypertension, heart failure, HIV, renal failure, and chronic lung disease. The case fatality rate was also determined by the presentation and severity of infection. Severe cases had the highest fatality rate, with asymptomatic and mild cases reporting no death. Thus, a higher proportion of persons with comorbidities had the worst prognosis with rapid progression of severe clinical signs and symptoms requiring hospitalization and ventilatory support. This finding was corroborated by a global study that demonstrated worse COVID-19 outcomes among cases with underlying medical conditions compared with those without comorbidities [
20].
This investigation described the COVID-19 epidemic curves in Mombasa County and interpreted the overall curve as having a propagated source pattern. This finding is in contrast with early studies in china that showed a mixed outbreak pattern i.e., an initial continuous common source pattern of spread followed by a propagated source pattern[
21]. Our findings like the study in China were consistent with the hypothesis that indeed the outbreak originated from an animal source at Huanan Seafood Wholesale Market in Wuhan, China, where a possible spillover resulted in transmission of the COVID-19 virus from a yet to be identified animal species into humans and later the spread was sustained by variants that allowed efficient human to human transmission due to the resultant mutation and recombination [
22]. This could explain the observed gradual increase in confirmed cases at the community level after the importation of the diseases into the county and the subsequent clustering of cases among people of some specific high-risk occupations (Port and health workers).
The two main clusters of cases that emerged were among health workers and port workers. Analysis of the epidemiological curves of the confirmed cases among port workers and health workers depicted a propagated outbreak pattern. Health workers may have been infected via nosocomial transmission and were among the over 10,000 cases of health workers reported across[
23]. These findings were consistent with observations in the UK and the USA that indicated an increased risk of reporting a positive COVID-19 test result among front-line healthcare workers [
24]. People working in health facilities could be exposed to infectious diseases in health facility settings while interacting with asymptomatic cases whose infectious state may not be apparent as they wait for definitive diagnoses. When dealing with a novel disease like COVID-19, it would be advisable for health care workers and people handling cargo from various origin to take extra precautions and work within the provided guidelines to limit exposure and transmission of infectious pathogens.
The main strength of this investigation was the early initiation which provided an in-depth understanding of the outbreak and the unique dynamics which informed the development of County specific public health containment measures. Nevertheless, this investigation had two limitations. Firstly, there was incompletely entered data, some records had missing data to varying degrees. Data that was missing included variables of interest such as travel history, underlying chronic conditions, and progression of the disease which limited our ability to make conclusions about the outbreak. Secondly, poor turnout by Mombasa residents for the targeted mass testing could have underestimated the true magnitude of the pandemic, as evidenced by results of a seroprevalence study that reported a prevalence of 9.3% in Mombasa and estimated that 5% of Kenyans had been exposed to COVID-19 during the study period [
25].
Conclusion


In conclusion, this early descriptive, exploratory analysis of regional COVID- 19 cases offer additional epidemiological knowledge to the local, national, regional, and international community on the pandemic. This information could be used in the development and deployment of region-specific public health containment measures, to minimize the transmission rates and ultimately reduce impact of disease. Sustained response and targeted containment measures with particular emphasis on the identified high-risk groups were recommended. With the setting in of community transmission of the SARS-CoV-2 responsible for the COVID-19 pandemic, this study recommended the development/strengthening of community event-based surveillance to enhance community COVID-19 surveillance and establishment of a rapid mortality surveillance system to generate timely, quality mortality data to determine excess mortality during COVID-19 pandemic.
What is known about this topic
- Initial cases of COVID-19 were imported from other countries or regions, then followed by local community person to person transmission.
What this study adds
- Clusters related to work areas could amplify the fast transmission of COVID-19 in the community where the workers reside.
Competing interests


The authors declare no competing interests.
Authors' contributions


Conceptualization and design: JKM, MSM, SM, SJ, SMM, FO, RA, MM, PA, AM, WB, MN, JG, E.O,
MO. Data Collection: JKM, MSM, SM, SJ, SMM, EO, MO. Data Analysis: JKM, MSM, SM, SJ, SMM, FO, AM, WB, EO, MO. Development and review of manuscript: JKM, MSM, SM, SJ, SMM, FO, RA, MM, PA, AM, WB, MN, JG, E.O, MO.
Acknowledgments


The authors wish to appreciate the assistance from the county government of Mombasa during the field activities in accessing data and incorporating the investigation team into the county response teams.
Tables and figures


Table 1: Number of suspected SARS-COV 2 cases by Age, Sub-county, sex, occupation, history of travel, symptom status and laboratory results, in Mombasa County as of April 30, 2020 (n=2835 suspected SARS-COV 2 cases)
Table 2: Frequency of confirmed cases, deaths, and case-fatality rates, observed time (PD) and mortality per 10 PD for n=126 confirmed cases in Mombasa County as of April 30, 2020
Table 3: Frequency of clinical characteristics of confirmed cases, deaths, and case-fatality rates, observed time (PD) and mortality per 10 PD for n=126 confirmed cases in Mombasa County as of April 30, 2020
Figure 1: Age distribution and sex ratio of all confirmed COVID-19 cases in Mombasa County and Mvita sub-county as of April 30, 2020
Figure 2: Geo-temporal spread of COVID-19 in Mombasa County as of April 30, 2020
Figure 3: Epidemiological curves of COVID-19 in Mombasa County as of April 30, 2020.
Figure 4: Transmission tree of first 11 confirmed COVID-19 Cases, Mombasa County as of April 15, 2020
Figure 5: Subgroup epidemiological curves of COVID-19 in Mombasa County as of April 20, 2020
References


- Namukose E, Bowah C, Cole I, Dahn G, Nyanzee P, Saye R, Duworko M, Nsubuga P, Mawanda M, Mahmoud N, Clement P, Ngabirano TD, Nyenswah T, Gasasira A. Active Case Finding for Improved Ebola Virus Disease Case Detection in Nimba County, Liberia, 2014/2015: Lessons Learned. Advances in Public Health. 2018 Oct 31; 2018:e6753519. https://doi.org/10.1155/2018/6753519 . Google Scholar
- Fasina FO, Shittu A, Lazarus D, Tomori O, Simonsen L, Viboud C, Chowell G. Transmission dynamics and control of Ebola virus disease outbreak in Nigeria, July to September 2014. Eurosurveillance. 2014 Oct 9; 19(40):20920. https://doi.org/10.2807/1560-7917.ES2014.19.40.20920 . Google Scholar
- Petherick A. Ebola in west Africa: learning the lessons. The Lancet[Internet]. 2015 Feb 14[cited 2022 Dec 15]; 385(9968):591-2.https://doi.org/10.1016/S0140-6736(15)60075-7 . Google Scholar
- Yamin D, Gertler S, Ndeffo-Mbah ML, Skrip LA, Fallah M, Nyenswah TG, Altice FL, Galvani AP. Effect of Ebola progression on transmission and control in Liberia. Ann Intern Med. 2015 Jan 6; 162(1):11-7. https://doi.org/10.7326/M14-2255 PubMed | Google Scholar
- Johns Hopkins Coronavirus Resource Center. COVID-19 Map[Internet ]. Johns Hopkins University and Medicine;[cited 2022 December 15].
- Al-Qahtani AA. Severe Acute Respiratory Syndrome Coronavirus 2 (SARS-CoV-2): Emergence, history, basic and clinical aspects. Saudi J Biol Sci[Internet]. 2020 Oct[cited 2022 Dec 15];27(10):2531-2538. https://doi.org/10.1016/j.sjbs.2020.04.033 PubMed | Google Scholar
- World Health Organization. Clinical management of severe acute respiratory infection (SARI) when COVID-19 disease is suspected: interim guidance, 13 March 2020 [Internet]. World Health Organization; 2020[cited 2022 December 15]. Google Scholar
- Lauer SA, Grantz KH, Bi Q, Jones FK, Zheng Q, Meredith HR, Azman AS, Reich NG, Lessler J. The Incubation Period of Coronavirus Disease 2019 (COVID-19) From Publicly Reported Confirmed Cases: Estimation and Application. Ann Intern Med. 2020 May 5;172(9):577-82. https://doi.org/10.7326/M20-0504 . Google Scholar
- Gebhard C, Regitz-Zagrosek V, Neuhauser HK, Morgan R, Klein SL. Impact of sex and gender on COVID-19 outcomes in Europe. Biol Sex Differ[Internet]. 2020 May 25[cited 2022 December 15];11(1):2. https://doi.org/10.1186/s13293-020-00304-9 . PubMed | Google Scholar
- World Health Organization. Coronavirus disease 2019 (COVID-19): situation report, 51[Internet]. WHO; 2020[cited 2022 December 16]. 9 p. Google Scholar
- Wu C, Chen X, Cai Y, Xia J, Zhou X, Xu S, Huang H, Zhang L, Zhou X, Du C, Zhang Y, Song J, Wang S, Chao Y, Yang Z, Xu J, Zhou X, Chen D, Xiong W, Xu L, Zhou F, Jiang J, Bai C, Zheng J, Song Y. Risk Factors Associated With Acute Respiratory Distress Syndrome and Death in Patients With Coronavirus Disease 2019 Pneumonia in Wuhan, China. JAMA Intern Med[Internet]. 2020 Jul 1[cited 2022 December 15]; 180(7):934-943. https://doi.org/10.1001/jamainternmed.2020.0994 PubMed | Google Scholar
- Sun H, Dickens BL, Cook AR, Clapham HE. Importations of COVID-19 into African countries and risk of onward spread. BMC Infect Dis[Internet]. 2020 Aug 13[cited 2022 December 15]; 20(1):598. https://doi.org/10.1186/s12879-020-05323-w PubMed | Google Scholar
- Rosenthal PJ, Breman JG, Djimde AA, John CC, Kamya MR, Leke RGF, Moeti MR, Nkengasong J, Bausch DG. COVID-19: Shining the Light on Africa. Am J Trop Med Hyg[Internet]. 2020 Jun[cited 2022 December 15]; 102(6):1145-1148. https://doi.org/10.4269/ajtmh.20-0380 . PubMed | Google Scholar
- Ministry of Health Kenya. First case of coronavirus disease confirmed in Kenya[Internet]. Kenya: Ministry of Health; 2020[cited 2022 December 15].
- Aluga MA. Coronavirus Disease 2019 (COVID-19) in Kenya: Preparedness, response and transmissibility. J Microbiol Immunol Infect. 2020 Oct;53(5):671-673. https://doi.org/10.1016/j.jmii.2020.04.011. PubMed | Google Scholar
- Ministry of Health Kenya. COVID-19 outbreak in Kenya daily situation report - 131[Internet]. Kenya: Ministry of Health; 2020 July 27[cited 2022 December 15].
- Kenya FELTP. FELTP - News 1[Internet]. Kenya FELTP;[cited 2022 June].
- Kenya National Bureau of Statistics. 2019 Kenya Population and Housing Census Volume I: Population by County and Sub-County[Internet]. Kenya National Bureau of Statistics;2019 November 4[cited 2022 December 15].
- World Health Organization. Public health criteria to adjust public health and social measures in the context of COVID-19: annex to considerations in adjusting public health and social measures in the context of COVID-19, 12 May 2020[Internet]. World Health Organization; 2020[cited 2022 December 15].
- Sanyaolu A, Okorie C, Marinkovic A, Patidar R, Younis K, Desai P, Hosein Z, Padda I, Mangat J, Altaf M. Comorbidity and its Impact on Patients with COVID-19. SN Compr Clin Med. 2020; 2(8):1069-1076. https://doi.org/10.1007/s42399-020-00363-4 PubMed | Google Scholar
- The Novel Coronavirus Pneumonia Emergency Response Epidemiology Team. The Epidemiological Characteristics of an Outbreak of 2019 Novel Coronavirus Diseases (COVID-19) - China, 2020. China CDC Wkly[Internet]. 2020 Feb 21[cited 2022 December 15]; 2(8):113-122. http://dx.doi.org/10.46234/ccdcw2020.032 PubMed | Google Scholar
- Paules CI, Marston HD, Fauci AS. Coronavirus Infections-More Than Just the Common Cold. JAMA [Internet]. 2020 Feb 25[cited 2022 December 15]; 323(8):707-8. https://doi.org/10.1001/jama.2020.0757 Google Scholar
- Erdem H, Lucey DR. Healthcare worker infections and deaths due to COVID-19: A survey from 37 nations and a call for WHO to post national data on their website. Int J Infect Dis[Internet]. 2021 Jan[2022 December 15]; 102:239-241. https://doi.org/10.1016/j.ijid.2020.10.064 PubMed | Google Scholar
- Nguyen LH, Drew DA, Graham MS, Joshi AD, Guo CG, Ma W, Mehta RS, Warner ET, Sikavi DR, Lo CH, Kwon S, Song M, Mucci LA, Stampfer MJ, Willett WC, Eliassen AH, Hart JE, Chavarro JE, Rich-Edwards JW, Davies R, Capdevila J, Lee KA, Lochlainn MN, Varsavsky T, Sudre CH, Cardoso MJ, Wolf J, Spector TD, Ourselin S, Steves CJ, Chan AT; COronavirus Pandemic Epidemiology Consortium. Risk of COVID-19 among front-line health-care workers and the general community: a prospective cohort study. Lancet Public Health[Internet]. 2020 Sep[cited 2022 Dec 15]; 5(9):e475-e483. https://doi.org/10.1016/s2468-2667(20)30164-x PubMed | Google Scholar
- Uyoga S, Adetifa IMO, Karanja HK, Nyagwange J, Tuju J, Wanjiku P, Aman R, Mwangangi M, Amoth P, Kasera K, Ng'ang'a W, Rombo C, Yegon C, Kithi K, Odhiambo E, Rotich T, Orgut I, Kihara S, Otiende M, Bottomley C, Mupe ZN, Kagucia EW, Gallagher KE, Etyang A, Voller S, Gitonga JN, Mugo D, Agoti CN, Otieno E, Ndwiga L, Lambe T, Wright D, Barasa E, Tsofa B, Bejon P, Ochola-Oyier LI, Agweyu A, Scott JAG, Warimwe GM. Seroprevalence of anti-SARS-CoV-2 IgG antibodies in Kenyan blood donors. Science [Internet]. 2021 Jan 1[cited 2022 December 15]; 371(6524):79-82. https://doi.org/10.1126/science.abe1916 PubMed | Google Scholar