Exposure to known COVID-19 infection risk factors among healthcare workers responding to COVID-19 outbreak in Lagos State, Nigeria-2020
Olugbenga Odukanmi1,2,&, Muhammed Balogun2,3, Olayinka Ilesanmi 1,2, Bisola Adebayo 2,4, Adetunji Adenekan 5, Oluwatosin Onasanya 2,6, Oyeladun Okunromade 2,7, Ugochukwu Madubueze 8, Chukwuma Umeokonkwo 2,3,8, Patrick Nguku 3
1University of Ibadan, Nigeria, 2Nigeria Field Epidemiology and Laboratory Training Program (NFELTP), 3African Field Epidemiology Network (AFENET), 4Lagos State University College of Medicine, Nigeria, 5College of Medicine, University of Lagos, 6Lagos State Primary Health Care Board, 7Nigeria Centre for Disease Control (NCDC), 8Alex-Ekwueme Federal University Teaching Hospital, Ebonyi State
&Corresponding author
Olugbenga Adeola Odukanmi, Department of Physiology, College of Medicine, University of Ibadan. odukanmi2@gmail.com
Introduction:
Globally, over 790,000 deaths of COVID-19 cases were reported by August 20, 2020, these numbers included healthcare workers (HCW). The high infection rate among HCW to COVID-19 is worrisome requiring countries to protect them. We examined the risk of exposure among HCW.
Methods:
We conducted a cross-sectional study among 151 healthcare workers responding to the COVID-19 outbreak in Lagos State using an electronic-based self-administered questionnaire. Categorical variables were summarized as proportions, and bivariate analysis of the independent and dependent variables was subjected to the Chi-square test. A P-value of < 0.05 was considered statistically significant.
Results:
Sixty-nine (45.9%) of responders have had over 10-year experience in the health sector. Ninety-eight (64.9%) of the responders had previous experience in responding to outbreaks. Ninety-nine (65.6%) of responders had been involved in the COVID-19 response beyond two months. Sixty-three (41.7%) participants were exposed to aerosol-generating procedures (AGP), with the majority (85%) occurring during the collection of sputum for COVID-19 testing. Forty-three percent were involved directly with facilities where confirmed cases were treated. Among responders, 101 (66.9%) admitted to the regular use of work-appropriate personal protective equipment (PPE) during their activities. One hundred and thirty-seven HCW (90.7%) had no exposure to biological or respiratory fluids. On bivariate analysis, no variable was associated with the risk of contracting the infection by healthcare workers.
Conclusion:
The exposure to known COVID-19 risk factors among healthcare responders in Lagos is high. This exposure is not associated with years of experience of service in the health sector, age or gender of responders, direct contact with confirmed cases, or direct care of confirmed COVID-19 cases.
Introduction

World Health Organization (WHO) declared the Coronavirus disease (COVID-19) a pandemic [1]. Globally, over twenty million confirmed cases have been recorded and about 790,000 deaths as of August 12, 2020 [2]. By the third week in August 2020, confirmed COVID-19 cases in Africa were about 905,000 with over 19,225 reported deaths [3]. In addition, WHO also reported a total of 38,768 COVID-19 cases among healthcare providers with a large number of possible unreported cases in Africa [3].
The mode of transmission of COVID-19 is largely through respiratory droplets as well as aerosolizing activities, thus posing a great risk to healthcare workers (HCW) [
4]. So far, about 10% of all confirmed cases worldwide are HCW, with the proportion varying in countries. Though there is inadequate information about the occurrence of infection among HCW involved in the COVID-19 response in Africa, initial findings of 5% of cases in 14 countries in sub-Saharan Africa alone are discouraging [
3]. In Nigeria, of the 319,851 samples tested, 46,867 were confirmed COVID-19 cases with 950 deaths as of August 10, 2020. Of this total, 16,074 (34.3%) of Nigeria´s confirmed cases and 195 (20.5%) deaths occurred in Lagos State. In addition, more than 800 HCWs in Nigeria had been confirmed COVID-19 positive as of June 2020 [
5]. The data demonstrates the significant risks faced by HCWs as they actively participate in the response to the COVID-19 pandemic.
Globally, HCWs are at risk of contracting COVID-19 because of the exposure risk at their health facilities contrary to the expected stay-at-home orders for other workers and individuals [
6]. When infected, HCWs could be vectors of onward transmission of COVID-19 either to family members or previously healthy persons [
7]. To assure the safety of HCWs amid the COVID-19 pandemic, the World Health Organization has stressed that appropriate and correct use of personal protective equipment (PPE) of all forms could reduce these risks [
8]. Inadequate supply and inappropriate utilization of personal protective equipment (PPE) and poor infection, prevention, and control (IPC) by HCWs have cumulative risks in the ongoing pandemic [
9].
Owing to the high infection rate among HCWs. This study, therefore, aimed to assess exposure to known COVID-19 risk factors among HCWs responding to the COVID-19 outbreak in Lagos State, Nigeria.
Methods


Outbreak setting
Lagos State, the epicenter of the COVID-19 outbreak in Nigeria, is in the South Western Region of the country. It had a projected population of 21 million in 2016, which makes it the most populous city in Africa. The COVID-19 outbreak in Lagos started in late February 2020 and has rapidly increased from the initial imported cases to community transmission involving all the local government areas in the State. This has led to the rapid training and deployment of a large number of healthcare responders in the State to help contain and mitigate the effect of the outbreak. There are six isolation and treatment centers in the State. The study was conducted at state isolation centres, quarantine facilities, NCDC Central Public Health Laboratory, and walk-in sites at the six zonal Local Government Area sites for sample collection.
Study design, population, and sampling technique
We conducted a cross-sectional study among healthcare responders to the COVID-19 outbreak in Lagos between March and June 2020. One hundred and fifty-one healthcare responders in Lagos filled and submitted a completed questionnaire from the total 176 healthcare responders at the time of the study, that is 85.8% of the total available healthcare responders who participated in the study. The healthcare responders were recruited by sending out consent forms and questionnaires through different pillars of COVID-19 response units. Twenty-five (14.2%) HCWs who were either confirmed cases and/or those with an active infection in isolation centres at the time were excluded from the study.
Data collection
We used an electronic-based self-administered questionnaire (Google form) to collect data for the study. This was adapted from a WHO tool in the Interim Guidance on Risk Assessment and Management of Health worker in the Context of COVID-19 [
10].
Data Management and Statistical Analysis
We collated and cleaned the data using the Epi Info 3.5.1 version [
11]. The dependent variable was the healthcare workers' exposure risk category (high or low). The HCWs were categorized using the WHO risk assessment tool for healthcare workers in the context of COVID-19 [
10]. The risk was assessed using three questions; healthcare responders' use of PPE, healthcare workers' adherence to using PPE during AGP, and healthcare workers' or responders´ accidental exposure to biological materials. Responders who always used PPEs as recommended, wore appropriate PPEs during AGP, and have not been accidentally exposed to biological materials were classified as low risk, else they are classified as high risk. The independent variables include age, sex, marital status, religion, work experience, and professions. The proportions of those who were high or low risk were estimated and presented in charts. The relationship between the dependent and independent variables was examined using the Chi-square test at a 5% level of significance.
Availability of data and materials
Data are available from the authors upon rational request.
Ethical Considerations
We sought and obtained ethical approval for the study from the Lagos University Teaching Hospital-Health Research Ethical Committee, with approval number: LUTHHREC/EREV/0520/39. Assurance of absolute confidentiality was provided to the respondents. The questionnaire was administered to respondents after voluntary informed consent was obtained. Participants were assured of the right to decline further participation in the study without loss of benefits after valid informed consent was obtained.
Results


Sociodemography
Among the respondents, 51% (77/151) were males, 49% (74/151) females. One hundred and eight responders (71.5%) were married and 42 (27.8%) were single. One hundred and fifteen (76.2%) of the responders were Christians and the rest practice Islam. Sixty-nine (45.9%) of the responders had worked beyond 10 years in the field while 52 (34.5%) have worked for less than 5 years (Table 1).
Level of Exposure Risk Based on Experience and Activities Performed by COVID-19 Responders
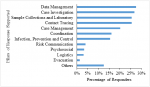
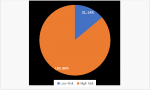
Ninety-eight (64.9%) of the 151 responders have had previous experience in responding to outbreaks compared to those without experience. Ninety-nine (65.6%) of responders had been in the field beyond two months (Figure 1). We captured multiple responses for healthcare workers who served in more than one pillar of response and this also depicts exposure by activities. The case investigation had 40 (26.8%) of the HCWs, contact tracing 38 (25.5%), laboratorians 38 (25.5%), case management 30 (20.1%) and data management 41(27.5%), (Figure 2). The level of risk described in figure 3 shows that 130 (86.1%) of responders had a high-risk level of exposure out of the 151 responders. Overall, 130 (86%) of respondents were exposed to a high level of risk compared to 21 (14%) that had a low-level exposure risk, (Figure 3).
Assessment of Healthcare Responders Exposure Risk to Procedure and Environment of COVID-19 Outbreak Response
We described the level of exposure risk of responders to COVID-19 due to procedures and the work environment. Ninety-nine (65.6%) of the responders had been in the COVID-19 response beyond 60 days, whereas only 8 (5.3%) responders were in the field for less than 30 days. Fifty-seven (37.8%) of the HCW cared directly for confirmed cases, while 94 (62.3%) HCW interacted from a distance (Table 2). Sixty-three (41.7%) responders were exposed to AGP, and 53 (81.4%) of this was during the collection of sputum for COVID-19 screening. The responders that were involved directly with facilities where confirmed COVID-19 cases received treatment were 65 (43.1%)of the total responders. In addition, a total 48 (31.8%) responders visited other health facilities (either public or private), ambulances, or home care settings to manage patients while responding to the pandemic (Table 3).
Adherence to IPC measures and PPE usage among Covid-19 Health Responders
The adherence to IPC and appropriate usage of PPE among COVID-19 healthcare responders in Lagos are described in Tables 4 and 5. Accidental exposure to body fluid from suspected and confirmed cases was alluded to by 14 (9.3%) of the responders against 137 (90.7%) without such exposure. Among responders, 101 (66.9%) reported the regular use of PPE during their activities. Appropriate PPE use, hand-washing after accidental contact with body fluid (72.7%), and wearing of the medical mask (71.8%) ranked the highest. The least form of PPE adhered to was disposable gown (33.1%) and use of face shield (27.5%), (Tables 6 and 7).
Discussion


Corona Virus Disease (COVID-19) transmission to HCW has been a concern since the beginning of the outbreak and they constitute about 10% of the confirmed cases worldwide [12, 13]. Considering the risk of a weak health system, WHO considered Nigeria as one of the 13-high-risk and vulnerable nations for COVID-19 disease [14, 15]. Lagos State, the outbreak setting for this study is bedeviled with factors that promote vulnerability for COVID-19 transmission such as high population density and type of settlements (predominantly slums), commerce, overwhelmed health sector, the reliance on the informal economy among many other dynamics [16].
From this study, we identified that the cadre of people infected in Lagos COVID-19 response indicates that the virus is no respecter of cadre or specialty. This is because the infection is as common among those with no history of direct contact with confirmed cases. Moreover, those with close contact tend to prepare better with the use of adequate PPE compared to those who are not working directly with confirmed cases [
17,
18]. The outcome of our study differs from a study conducted among anesthesiologists in a Wuhan hospital in China where they reported zero infection after intubating 202 confirmed cases. They adduced the success to years of experience [
18]. The reference literature buttresses the effectiveness of experience in tackling the COVID-19 outbreak in Nigeria. Lessons learned from the Ebola outbreak in 2014 appeared not to have been used in the present COVID-19 context although this pandemic has a different mechanism of transmission. This makes many HCWs exposed to the risk of contracting COVID-19 during their duties. Although many HCW had participated in one or more outbreak responses before the present pandemic, the observed level of experience did not reduce the exposure to known risk factors of COVID-19. This reveals that years of experience in IPC training might be insufficient in reducing COVID-19 infection rates among HCWs. Fatigue and inadequate training before the onset of the outbreak could have contributed to the reported large number of infections among healthcare responders.
SARS-CoV-2, the virus responsible for COVID-19 is transmitted mainly by droplet and direct contact [
19,
20]. Droplet transmission may occur from fomites in the immediate environment of the infected person [
21]. From this study, we identified that the most important form of exposure by healthcare responders to droplets is through AGP, mostly from sputum collection. The exposure to AGP among responders in this study suggests a significant risk to healthcare responders who may serve as vectors in the onward transmission of COVID-19 to the community. Although there were indications that AGP increases the chances of contracting COVID-19, however, no known evidence supports the fact that they do [
22].
Infection, prevention, and control professionals are crucial in emergency preparedness and responses to containing the spread of the virus, especially the transmission of infection from clients to outbreak responders [
23]. In this study, we identified that the high risk due to AGP, accidental exposure to biological fluids, inappropriate use of PPE depicts poor IPC. This could result from fatigue or non-adherence to IPC protocols among HCW. Inadequate PPE supply was a global issue at some point as countries sourced for substitutes and this did not help the healthcare responders who went all out to ensure the containment of the spread of COVID-19 disease. The high proportion of those with direct contact with confirmed cases without adequate PPEs could have also contributed to the high number recorded.
It was observed from this study that the age of responders, genders, years of work experience, duration of stay for response participation, direct care for confirmed COVID-19 cases, or direct contact with confirmed COVID-19 cases were not sufficient as individual factors to classify HCW to either high or low-risk class.
Limitations and Strengths
One important limitation of this study was difficulty in assessing the level of risk per individual HCW because some of them worked in multiple pillars of outbreak response, making it a bit cumbersome to score the level of risk. The strength of the study is the location and percentage of healthcare responders (85.8%) recruited- we recruited HCW from Lagos State, Nigeria COVID-19 epicenter where we had the largest HCW who responded to the COVID-19 pandemic in Nigeria at the time.
Conclusion


This study identified a high level of risk to known COVID-19 risk factors among healthcare responders. We realized that for COVID-19 level of risk among healthcare responders, experience and long years in the health sector, age of responders, gender, direct contact, or direct care of confirmed COVID-19 cases were not sufficient as individual factors to increase the risk of exposure of healthcare responders in Lagos to known COVID-19 risk factors. Therefore, inappropriate use of PPE, inadequate IPC training, and poor adherence to IPC protocols during accidental contact with body fluids lingered as the link to the high level of risk among HCWs who are involved in the COVID-19 response in Lagos State. This is a call to our health institutions to step up IPC training and ensure prioritization of the provision of PPE necessary to contain future outbreaks. Governments at all levels should step up training of healthcare workers in infection prevention and control practices. As well as ensure local production of PPE that is useful and needed in the management of future public health emergencies.
What is known about this topic
- We already know that the infection rate among HCW to COVID-19 is high with Exposure to AGP, poor PPE usage, and accidental exposure to body fluid
What this study adds
- It adds that the experience and long years in infectious disease response, age of responders, gender, direct contact, or direct care of confirmed COVID-19 cases were not sufficient as an individual factor to increase the risk of exposure to COVID-19 disease among healthcare responders in Lagos.
Competing interests


The authors declare no competing interests.
Authors' contributions


OOA, BMS, IOS, ABI, AAO, OO, OOF, MUC, NP conceived the study and participated in its design and implementation. OOA, BMS, IOS, UCD, OO, OOF wrote the manuscript. OOA analyzed the data. All authors read and approved the final manuscript.
Acknowledgements


The authors appreciate the Lagos State Government, Nigeria Centre for Disease Control (NCDC), and African Field Epidemiology Network (AFENET) for enabling us to carry out this study at the heat of outbreak response and for providing logistics for the response. We humbly appreciate our colleagues (Dr. Okediran James, Dr. Fetuga Doyin, Ms. Amaza Rahab) who assisted in correcting and distributing our questionnaire.
Tables and figures


Table 1: Socio-Demographic Characteristics of Health Care Responders to COVID-19 in Lagos
Table 2: Level of Health Responder Interactions with COVID-19 Patients in Lagos
Table 3: Health Responders´ Exposure Risk to Procedure and Environment of COVID-19 Response
Table 4: Infection Prevention and Control (IPC) among COVID-19 Healthcare Responders
Table 5: Personal Protective Equipment Practice among Healthcare Responders
Table 6: Increasing exposure risk factors associated with the management of covid-19 patients
Table 7: Analysis of factors associated with the increasing exposure risk with the management of covid-19 patients
Figure 1: Past outbreak responses participated in by healthcare responders in Lagos
Figure 2: Pillars of response to COVID-19 among healthcare responders in Lagos
Figure 3: Level of Risk of healthcare responders to COVID-19 pandemic in Lagos
References


- WHO. WHO, Director-General's opening remarks at the media briefing on COVID-19. WHO. 2020. Accessed March 2020.
- WHO. Coronavirus disease (COVID-19) Situation Report; Reports - 205. WHO. 2020. Accessed August 2020.
- WHO Africa. Situation reports on COVID-19 outbreak - Sitrep 25. WHO Africa. 2020. Accessed 19 August 2020.
- WHO. Risk assessment and management of exposure of health care workers in the context of COVID-19 Interim guidance. WHO. 2020 Accessed March 2020.
- WHO Africa, Adam A. Nigeria: 113 Healthcare workers infected with COVID-19: Latest on Coronavirus Outbreak. AA.com. 2020. Accessed May 2020.
- The Lancet. COVID-19: protecting health-care workers. Lancet. 2020 Mar 21; 395(10228):922.https://doi.org/10.1016/S0140-6736(20)30644-9 PubMed | Google Scholar
- CDC. (Corona Disease 2019): Interim Operational Considerations for Public Health Management of Healthcare Workers Exposed to or with Suspected or Confirmed COVID-19: non-US healthcare setting; 1-9, 2020. CDC. 2020. Accessed May 2020.
- WHO. Over 22,000 healthcare workers across 52 countries infected by COVID-19. Xinhua news agency report. Accessed April 2020.
- Wang J, Zhou M, Liu F. Reasons for healthcare workers infected with novel Coronavirus disease 2019 (COVID-19) in China. J Hosp Infect. 2020 May; 105(1):100-101.https://doi.org/10.1016/j.jhin.2020.03.002 PubMed | Google Scholar
- WHO. Interim guidance, Risk assessment and management of exposure of health care workers in the context of COVID-19. WHO. 2020. Accessed March 2020.
- Shehu NY, Onyedibe KI, Igbanugo JS, Okolo MO, Gomerep SS, Isa SE, Egah DZ. Hand hygiene knowledge, training, and practice: A cross-sectional study in a tertiary health institution, North-central Nigeria. Niger J Clin Pract. 2019; 22(7):1008-13. Google Scholar
- Cook T, Kursumovic E, Lennane S. Exclusive: Deaths of NHS staff from COVID-19 analyzed. Health Service Journal. 2020. Aaccessed April 2020.
- Amzat J, Aminu K, Kolo VI, Akinyele AA, Ogundairo JA, Danjibob MC. Coronavirus outbreak in Nigeria: Burden and socio-medical response during the first 100 days. Int J Infect Dis. 2020 Sep; 98:218-224.https://doi.org/10.1016/j.ijid.2020.06.067 PubMed | Google Scholar
- Ogundiya IS, Olutayo AO, Amzat J, editors. Assessment of Democratic Trends in Nigeria. New Delhi: Gyan Books; 2011. p313-22. Google Scholar
- Marbot O. Coronavirus Africa Map: Which countries are most at risk?. The Africa report. 2020. Accessed April 2020.
- Assessment Capacities Project (ACAPS). COVID-19 in Nigeria - Vulnerabilities to COVID-19 and containment measures - Thematic report. ACAPS. 2020. Accessed May 2020.
- Meng L, Qiu H, Wan L, Ai Y, Xue Z, Guo Q, Deshpande R, Zhang L, Meng J, Tong C, Liu H, Xiong L. Intubation and ventilation amid the COVID-19 outbreak: Wuhan´s experience. Anesthesiology. 2020 June; 132:1317-1332.https://doi.org/10.1097/ALN.0000000000003296 . PubMed | Google Scholar
-
Yao W, Wang T, Jiang B, Gao F, Wang L, Zheng H, Xiao W, Yao S, Mei W, Chen X, Luo A, Sun L, Cook T, Behringer E, Huitink JM, Wong DT, Lane-Fall M, McNarry AF, McGuire B, Higgs A, Shah A, Patel A, Zuo M, Ma W, Xue Z, Zhang L-M, Li W, Wang Y, Hagberg C, O'Sullivan EP, Fleisher LA, Wei H, Peng Z, Liang H, Nishikawa K. Emergency tracheal Intubation in 202 patients with COVID-19 in Wuhan, China: lessons learned and expert recommendations. Bri J of Anaesth 2020.https://doi.org/10.1016/j.bja.2020.03.026 . Google Scholar
- Lake MA. What we know so far: COVID-19 current clinical knowledge and research. Clin Med. 2020 Mar; 20(2):124-127.https://doi.org/10.7861/clinmed.2019-coron . PubMed | Google Scholar
- Wang J, Du G. COVID-19 may transmit through aerosol. Irish J Med Sci 20 24:1e2.https://doi.org/10.1007/s11845-020-02218-2 . Google Scholar
- Ong SWX, Tan YK, Chia PY, Lee TH, Ng OT, Wong MS, Marimuthu K. Air, surface environmental, and personal protective equipment contamination by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) from asymptomatic patient. JAMA. 2020; 323(16):1610-1612.https://doi.org/10.1001/jama.2020.3227 Google Scholar
- Harding H, Broom A, Broom J. Aerosol-generating procedures and infective risk to healthcare workers from SARS-CoV-2: the limits of the evidence. J Hosp Infect. 2020 Aug; 105(4):717-725.https://doi.org/10.1016/j.jhin.2020.05.037 PubMed | Google Scholar
- Wang J, Liu F, Zhou M, Lee YF. Will the status of infection prevention and control (IPC) professionals be improved in the context of COVID-19? Am J Infect Control. 2020; 48(6):729-730.https://doi.org/10.1016/j.ajic.2020.04.003 Google Scholar