Descriptive Epidemiology and Mortality Risk Factors of COVID-19 Outbreak in Delta State, Nigeria, March - August 2020
Adaora Rosemary Ejikeme1,2,&, Bola Biliaminu Lawal2, Shalom Ogbonna1, Ehimario Igumbor2,3, Mildred Okowa4, Ivie Airefetalor5, Daniel Otoh6, Angela Okocha-Ejeko2, Onyinyechi Emefiene7, Ann Ojimba4, Henry Uguru-Ekechi1,2, Rhoda Atteh1,2, Nkiruka Obiazor8, Chukwuma David Umeokonkwo9,10, Muhammad Shakir Balogun9, Oladipupo Ipadeola2, Abdulhakeem Abayomi Olorukooba11, Aboyowa Edukugho9, Bolaji Ahmed12, Oladipo Ogunbode2
1Nigeria Field Epidemiology and Laboratory Training Program, Abuja, Nigeria, 2Nigeria Centre for Disease Control (NCDC), Abuja, Nigeria, 3School of Public Health, University of the Western Cape, Cape Town, South Africa, 4Federal Medical Centre, Asaba, Delta State, Nigeria, 5Irrua Specialist Hospital, Edo, Edo State, Nigeria, 6National Primary Health Care Development Agency, Nigeria, 7World Health Organization, Nigeria, 8Ministry of Health, Delta State, Nigeria, 9African Field Epidemiology Network, Abuja, Nigeria, 10Department of Community Medicine, Alex Ekwueme Federal University Teaching Hospital Abakaliki, Ebonyi State Nigeria, 11Department of Community Medicine, Faculty of Clinical Sciences, College of Medical Sciences, Ahmadu Bello University, Zaria, Kaduna State, Nigeria, 12Programmes Department, Damien Foundation, Ibadan, Oyo State, Nigeria
&Corresponding author
Adaora Rosemary Ejikeme, Nigeria Field Epidemiology Program Nigeria Center for Disease Control, Plot 801 Ebitu Ukiwe Street, Jabi, Abuja, Nigeria. rosemaryejikeme@yahoo.com
Introduction:
The highly contagious Coronavirus Disease 2019 (COVID-19) was first confirmed in Nigeria on February 27, 2020. In Delta State, the first COVID-19 case was recorded on April 7, 2020, which spread across the state. We characterized the COVD-19 pandemic in Delta State in terms of person, place, and time, and determined the risk factors for COVID-19 mortality.
Methods:
We conducted a retrospective analysis of COVID-19 pandemic in Delta State between March 23 to August 17, 2020. We obtained line-lists of 5,917 COVID-19 patients, cleaned and analyzed sociodemographic, clinical characteristics and outcome variables using IBM SPSS Statistics 25. We calculated frequencies, proportions, mean and standard deviation (SD). Bivariate and multivariate logistics regression analysis were conducted to determine the risk factors of COVID-19 mortality, adjusted-odds-ratios were reported at 95% confidence interval and p-value set at 5% significance level.
Results:
From March-August 2020, 1,605 confirmed COVID-19 cases and 47 deaths (case-fatality-rate 2.9%) were recorded. Majority were aged 20-39 years 675 (42.1%) while 1,064 (66.3%) were males (mean age 39±15years). Persons aged ≥60years were more likely to die from COVID-19 than younger cases (aOR: 11.0; 95% CI: 4.9-24.4) while Symptomatic positive cases at time of test were more likely to die than those who were not (aOR: 3.2; 95% CI: 1.3-7.5).
Conclusion:
Males in the youthful age-group were mostly affected. Independent predictors of mortality were being elderly or symptomatic at time of testing. Strengthening case management to target symptomatic patients and intensifying sensitization activities targeting youthful males and elderly persons, are important to reduce mortality.
Introduction

Coronavirus Disease 2019 (COVID-19) which was first reported in Wuhan city, China is caused by the novel coronavirus which had not been previously identified in humans [1]. The COVID-19 disease spread fast across countries and was declared a global pandemic by the World Health Organization (WHO) on March 11, 2020 [2,3]. Africa was projected to bear the final burden of the pandemic if countries do not implement effective measures [4]. As of December 28, 2020, over 79 million cases and 1.7million deaths were recorded globally [3]. while in Africa, over 1.9 million cases and 43 thousand deaths were recorded [3]. In Nigeria, over 84,000cases and 1,200 deaths were distributed across the 36 states and Federal Capital Territory (FCT) while Delta State (16th state to report a case) recorded over 1,800 cases and 49 deaths for same period [5].
To halt or significantly reduce the impact of COVID-19, the option of lockdown was mostly adopted globally. Sequel to this, the Nigerian government also imposed a lockdown in three states of the Federation namely: Lagos, Ogun, and Abuja, on March 30, 2020 [
6]. The lockdown was aimed to reduce COVID-19 transmission, reduce the number of confirmed cases and also ensure quick recovery of infected persons. This lockdown was later extended to all states including Delta State [
6]. The concept included compulsory stay at home for everyone (except essential workers e.g. health workers and security operatives). Additionally, there was prohibition of social gathering of more than 20 people and closure of all public places such as schools, hotels and religious houses [
6]. However, despite the imposed lockdown in Nigeria, increase in number of COVID-19 cases was still recorded nationwide including Delta State (7).
The epidemiology of COVID-19 found elderly persons at a higher severity of infection [
8], while 10 -15% of persons under 50 years have moderate to severe infections [
9]. Infection rates are higher among males [
10,
11]. Metropolitan areas with typically abundant economic activities and numerous social interactions are more vulnerable to higher transmission of SARS-COV2 [
12,
13]. As found in Tianjin, China, the pattern of local transmission of COVID-19 was a mixture of the propagated epidemic and the common-source outbreak in Tianjin [
14]. Four-fifth of confirmed cases are asymptomatic but capable of spreading the disease [
15]. Mortality has been recorded among cases with co-morbidities such as diabetes, chronic liver disease, high blood pressure or congestive cardiac failure [
9,
15].
The Index Case
The Delta State index case was a 50-year old Nigerian male who returned from a Canadian trip on March 6, 2020. Upon completion of the compulsory 14-day self-isolation, he had no symptoms suggestive of COVID-19, hence, visited a few places within and outside the State including FCT. On March 30, 2020, he presented at a private health facility in Delta State after his return from FCT, with respiratory symptoms (fever, cough and sore throat). The physician suspected COVID-19 and notified the Local Government Area (LGA) Disease Surveillance and Notification officer (DSNO), who in turn alerted the State´s COVID-19 rapid response team. Sample was collected and sent to Irrua Specialist Teaching Hospital (ISTH) laboratory in Edo State, a laboratory within the Nigeria Center for Disease Control (NCDC) laboratory network, where real-time polymerase chain reaction (RT-PCR) test for SARS-CoV-2 was conducted Test result returned positive for COVID-19 on April 7, 2020, and he was subsequently transferred to the State´s identified treatment center for proper case management.
The onset of COVID-19 pandemic in Delta State and possibility of concomitant community spread despite the nationwide lockdown in Nigeria, necessitated this study to gain comprehensive knowledge on the individuals affected, pattern of transmission (in place and time), co-morbidities and risk factors of the disease, to inform appropriate state-specific public health control measures. We, therefore, undertook a secondary data analysis during March to August 2020, to describe the epidemiology of COVID-19 pandemic in Delta State, Nigeria and to determine the risk factors for mortality among COVID-19 confirmed cases.
Methods


Outbreak setting
Delta State is an agricultural and oil producing state in Nigeria located in the South-South geo-political zone (an area known as Niger Delta) and lies approximately between 5°00' and 6°45' E and 5°00' and 6°30' N [
16]. The state has a total land area of 16,842 km2 with an estimated 2020 population of 6,369,849, from the last census in 2006 [
17]. The states sharing common boundaries with Delta State are Edo to the north, Ondo to the northwest, Anambra to the east and Bayelsa and Rivers to the south-east. On its southern flank is 160 km of the coastline of the Bight of Benin [
16]. The state has two airports located in Asaba and Warri which caters for national flights; four seaports in Warri, Koko, Burutu and Sapele; and major road arterial network making it an important gateway to both the South-South and South-Eastern regions of the country. To manage the COVID-19 pandemic, the State Ministry of Health designated four treatment centers: Federal Medical Center Asaba, Asaba Specialist Hospital Asaba; Delta State University Teaching Hospital Oghara and Central Hospital Warri. Before the deployment of a mobile COVID-19 molecular laboratory for conducting real-time polymerase chain reaction (RT-PCR) tests for SARS-CoV-2 virus in April 2020, oronasopharyngeal samples of suspected cases were transported to the reference laboratory at ISTH, Edo State which is a total driving distance of about 152 Km from Delta State.
Study design
We conducted a cross sectional study using a retrospective analysis of Delta State surveillance data between March 23 and August 17, 2020to characterize the outbreak in terms of time, place, and person and determine risk factors of mortality.
Study population and data collection
Case and contact definitions for COVID-19
We adopted the NCDC COVID-19 case definitions Version 4 [
5]. We defined a suspected case as any person presenting with fever, cough, or difficulty in breathing and who within 14 days before the onset of illness had any of the following exposures: a) history of travel to any high-risk country (consistently reporting increased number of COVID-19 cases) with widespread community transmission of SARS-CoV-2 OR b) close contact (within about 2meters/6 feet/for about 15 minutes or more) with a confirmed case of COVID-19 OR c) exposure to a health care facility where COVID-19 case(s) have been reported. A probable case was any suspect case a) For whom testing for COVID-19 presents an indeterminate test result(s) OR b) For whom testing was positive on a pan-coronavirus assay OR c) Where samples were not collected before the demise of a suspect case. A confirmed case was any person with laboratory confirmation of SARS-CoV-2 infection with or without signs and symptoms.
COVID-19 data source and flow - Surveillance Outbreak Response Management and Analysis System (SORMAS)
SORMAS is an open-source real-time mobile eHealth system concerned with digitization of the Integrated Disease Surveillance and Response (IDSR). SORMAS is hosted by NCDC and data on SORMAS is stored in a central server at the NCDC headquarters in Abuja, Nigeria. SORMAS ensures rapid collection, reporting, analysis and transmission of data in real-time [
18]. However, Data incompleteness is a major data quality issue [
19] as some of the variables in the system had no data entry at all or had some missing data.
At the subnational level, there are community informants (e.g. patent medicine vendors, residents etc.) and health facilities focal persons (clinicians, nurses) who report suspected COVID-19 cases to the LGA DSNO. The LGA DSNO in turn reports to the State DSNO. Upon investigation, the case is entered directly into NCDC SORMAS by the LGA DSNO and verified by the State DSNO/Epidemiologist and the NCDC State SORMAS Surveillance Officer (SSO). The national level (NCDC and partners) is also immediately notified of the case. Validation is also conducted by the NCDC SORMAS point. Upon receipt of the COVID-19 laboratory tests results, from the laboratory, the State DSNO/Epidemiologist communicates same to the concerned LGA DSNO, health facilities and patient involved. Data on SORMAS can only be extracted by authorized persons at the national and state levels.
All cases (suspected, confirmed and probable) of COVID-19 were eligible to be entered into the software and there were no exclusions. Hence, we included all persons investigated for SARS-CoV-2 infection and captured on SORMAS during our study period
Figure 1.
Data management and analysis
We obtained line-lists of confirmed COVID-19 cases from SORMAS and extracted sociodemographic, clinical characteristics and clinical outcome (dead or alive) information. Data was cleaned based on extracted variables on age, sex, education, occupation, place of residence, travel history, date of sample collection, presenting symptoms, and outcome, using MS Excel 2019 and analysed using IBM SPSS Statistics 25 [
21] and Quantum Geographic Information System (QGIS) 2.18.5 [
22]. For univariate analysis, we calculated frequencies and proportions for categorical variables, mean and standard deviation (SD) for numeric variables, calculated the infection rate per 100,000 population (by dividing the number of new cases by the 6,369,849 using 2020 projected population for Delta State). We generated a choropleth map; and an epi-curve showing number of confirmed cases, number of deaths, number of tests conducted per week and weekly positivity rate (by dividing the number of positive COVID-19 cases by the total number of tests conducted (negative and positive). In generating the epicurve, we used date of reporting at health facility instead of date of symptom onset because majority of the cases did not have this information recorded. We conducted bivariate and multivariate logistics regression analysis to determine the risk factors of COVID-19 mortality. The dependent variables were age group, sex, occupation, senatorial district and symptom condition (symptomatic or asymptomatic) while the outcome variable was clinical outcome (dead and alive). Significant variables were added into the multivariate logistic regression model (forward model). Odds ratio (OR) and adjusted odds ratio (aOR) were determined using p-value set at 5% significant level. Variables with p-value less than or equal to 0.05 were considered significant.
Ethical considerations
This study was performed as part of the COVID-19 public health response in Nigeria in 2020. Ethical clearance was obtained from the Health Ethics committee of the Federal Medical Center Asaba, Delta State with approval number FMC/ASB/A81 VOL XII/160.
Results


A total of 5,917 cases were abstracted during March-August 2020of which 1,605 (27.1%) were confirmed COVID-19 cases with 47 deaths representing a case fatality rate (CFR) of 2.9%. Using the 2020 projected population of 6,369,849 for Delta State, the infection rate was 25.2 per 100,000 populations. Majority 1,064 (66%) of the cases were male and persons within aged 20-39years 675 (42.1%) with a mean age ±SD 39±15years. The majority of cases were reported among persons with tertiary education 760 (47.4%). On occupational status, 258 (16%) of cases were health workers. while 1,539 (95.9%)were local transmission. A total of 563 (35.1%) were symptomatic at point of testing and each reported at least one symptom Table 1. The commonest clinical symptoms reported were fever, cough and difficulty breathing Figure 2. Nineteen (1.2%) had co-morbidity and 8 (0.5%) had cardiovascular disease (including hypertension).
At the initial period in the epidemic curve, the number of confirmed cases remained very low but rose gradually in week 18 (11 cases). However, the number of confirmed cases dipped slightly by week 19 (0 case) and thereafter, it rose slightly between weeks 20 and 21. It rose steeply from week 22 (53 cases) and peaked at the 26th epidemiological week (450 cases). Thereafter, the number of cases declined steeply whereby there were 271 cases in the 27th week and 83 cases in the 28th epidemiological week. Between the 30th and the 33rd epidemiological weeks, the number of confirmed cases plateaued and there was a little spike in the number of cases at the 32nd week
Figure 3. The number of deaths increased gradually from 17th week (1 death) until 22nd week when it dipped slightly (0 death). However, it rose in 23rd week (deaths) and peaked in 26th week (8 deaths). There was a slight dip in 27th week (2 deaths) followed by a slight increase in 28th week (4deaths). The number of deaths continued to decline steadily afterwards
Figure 3.
Over the 5-month period, the positivity rate increased with number of confirmed cases. the number of persons tested increased steadily from the 15th epidemiological week but dipped at 19th; 21st; and 23rd epidemiological weeks respectively. It peaked at the 29th week and dipped progressively thereafter until the 31st week and it increased slightly on the 32nd week and after which, it continued to decline steeply
Figure 3.
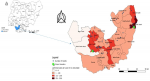
Twenty-three of 25 Local-Government-Areas (LGAs) reported at least one suspected and confirmed case
Figure 2. The cases were clustered around Oshimili North, Oshimili South, Warri South-West; Sapele; Ethiope West; Okpe and Uvwie LGAs. The cases were sparsely clustered around Aniocha North; Aniocha South; Isoko North; Isoko South; Ughelli South; and Bomadi South LGAs
Figure 4.
Table 2 shows the predictors of mortality among the cases of COVID-19 in Delta State between March and August 2020. Cases aged 60years and above were 11 times as likely to die as the cases aged less than 60 years (aOR:11.0, 95% CI: 4.9-24.4). Also, cases who were symptomatic for COVID-19 as at the time of testing were 3.2 times as likely to die as those who were asymptomatic as at the time of testing for the disease (aOR:3.2, 95% CI: 1.3-7.5). Factors such as sex did not appear to play a significant role as predictors of COVID-19 mortality. The model significance was <0.001 and our model explains 25% of the variations in the outcome (clinical outcome of COVID-19 cases).
Discussion


Our study described the epidemiology of COVID-19 pandemic. This study presents an analysis of the sociodemographic, clinical characteristics, transmission and risk factors of COVID-19 mortality among 1,605 confirmed cases in Delta State from March to August 2020. The findings hope to inform effective state-specific response especially with the imminent relaxation [23] of many non-pharmaceutical interventions (NPIs) such as full/partial lockdown and restriction of movement (workplaces, schools, religious houses, public gatherings), social distancing, use of facemasks, hand hygiene, previously imposed to control COVID-19 in Delta State.
Our study shows a preselection for SARS-CoV-2 infection in males as opposed to females. This agrees with previous studies on COVID-19 internationally and nationally [
10,
24,
25]. Additionally, more cases occurred among persons below sixty years while higher mortality was significant among those above sixty years. According to WHO, “95% of deaths occurred in those older than 60 years” [
8]. Explanation for these may include potential higher levels of exposure of males necessitated by their socio-cultural and economic roles to be more mobile. In Delta State, majority of households reported males as breadwinners in the Nigeria Demographic and Health Survey, 2018 [
26]. This may also explain the higher number of cases among persons aged 20-60years, who account for the economically-active age group in the state. However, high mortality among elderly persons may be attributed to their weak immune system [
27].
More cases among persons with tertiary-level education is interesting. Higher number of cases among people with formal education have been found [
25]. This may reflect the occupational and economic exposures that accrue to persons with more formal education.
A higher chance of death was found among persons who were symptomatic at the time of testing in this study. However, majority of COVID-19 cases in Delta State were asymptomatic at testing. In-line with previous studies [
25,
28], this reflects well on the state´s enhanced surveillance activities. Increase in asymptomatic cases implies in management, as such cases, including persons with mild illnesses, would ideally be managed at home. It is likely that home-based management would be central in the response in Delta State. Therefore, the need to strengthen this approach by ensuring well-trained and supported home-care givers, alongside monitoring of other household members, especially the elderly and persons with chronic diseases. Furthermore, developing mechanisms to ensure that relevant clinical information about cases managed at home is captured within the routine health information would be important to provide primary information needed to track COVID-19 in the state.
Majority of the cases presented with fever, cough and difficulty breathing. From previous study, COVID-19 patients most commonly present with fever, cough, and dyspnea, which can progress to more complications, multiple organ failure and death. Co-morbidities -including hypertension, Cardiovascular disease, Chronic liver disease, Diabetes, Chronic Kidney disease, Chronic pulmonary disease. The relationship between several biological age-clocks and genetic tests can identify both the mechanisms of the disease and individuals most at risk. [
27]. Co-morbidities indicate the increased biological age-clock and the affiliated molecular differences between those with co-morbidities and those without may explain why COVID-19 illness is mild in some persons but life-threatening in others.
Sixteen percent healthcare workers´ infection in this study is at par with the national rate and reflects the success of the infection prevention and control (IPC) programme. It is expected that with increasing index of suspicion, the rate of infections among health workers will decrease.
Within five months from the first case, the outbreak spread to almost all LGAs in the state and more than 95% were from community transmission with no travel history. This highlights the withered role of out-of-state travel in determining COVID-19 transmission, emphasizing the limits of lockdown and the need for more general practice of social distancing and other non-pharmaceutical preventive measures (such as use of facemasks, hand hygiene – hand washing and use of hand sanitizers, respiratory etiquette, appropriate ventilation of indoor spaces, regular cleansing of frequently touched surfaces) within the state. The epi-curve of the COVID-19 pandemic showed a propagated pattern which also suggests community transmission. Delta State outbreak seemed to have passed its peak as the incidence appeared to be tailing off.
The positivity rate remained low, the number of deaths declined, and intensity of transmission remained on the wane for several weeks which suggests that the outbreak was long past its peak. The positivity rate shows the percentage of all COVID-19 tests performed that are actually positive. It helps public health officials to determine whether enough tests are being conducted and the current level of transmission of the disease in the community. High positivity rate shows that the number of total tests is too low, therefore suggests there are likelihoods of higher transmission and more people with COVID-19 in the community are not tested [
29]. However, the limitation of basing positivity rates on tests rather than people is that some individuals are tested more than once, and duplicate results may give false low positivity rates. It therefore important for the state government to start developing a "blueprint for effective lockdown" which may be important for the next possible outbreak.
Study limitations
A remarkable proportion of the sociodemographic data, notably on age, education and occupation were missing. In generating the epicurve, we used date of reporting at health facility instead of date of symptom onset because majority of the cases did not have this information recorded. However, all findings have been reported to the Delta State Ministry of Health for improvement of data quality. Due to the small sample size, we could not include the variable - co-morbidity in the regression analysis. This analysis would have further supported previous findings on co-morbidity as a covid-19 risk factor. However, further studies have been recommended to the state. Despite these limitations, data cleaning was properly done to ensure accurate presentation of data.
Conclusion


Our study has provided the epidemiological and mortality risk analysis of COVID-19 in Delta State, Nigeria, which can in turn be used for effective state-specific response. We found that the independent predictors of mortality are being elderly or symptomatic. More cases were males in the economically active age group. To reduce mortality, we recommend intensification of risk communication and sensitization activities by the State Ministry of Health targeting the youths and elderly across the state. Improvement of specific messaging on the preventive measures, especially the non-pharmaceutical interventions (practice of social distancing, use of facemasks, hand hygiene – hand washing and use of hand sanitizers, respiratory etiquette, appropriate ventilation of indoor spaces, regular cleansing of frequently touched surfaces) is needed. Additionally, case management strategies should be improved to include home-based management of COVID-19 cases. Therefore, there is need to strengthen this approach by ensuring well-trained and supported home-care givers, alongside monitoring of other household members, especially the elderly and symptomatic persons and persons with chronic diseases. Also, mechanisms to ensure that relevant clinical information about cases managed at home is captured within the routine health information (SORMAS) should be developed because this would be important to provide primary information needed to track COVID-19 in the state.
What is known about this topic
- COVID-19 spreads in clusters around urban areas
- It affects more males than females
- Case Fatality is higher among the elderly
What this study adds
- This study has been able to describe the epidemiology and risk factors of COVID-19 mortality in Delta State, which will serve as a guide for policy in prevention and control.
Competing interests


The authors declare no competing interests.
Authors' contributions


ARE, BBL, SO, EI, MO, IA, DO, AO, OE, AO, and NO contributed to the study the conceptualization, design, data acquisition, analysis, and interpretation of data, drafting, and revising of the manuscript. HU, RA, MSB, OI, AAO, CDU, AE, BA, and OlO contributed to interpretation of data, initial drafting, and revising of the manuscript. All authors read and approved the final version for submission.
Acknowledgements


We wish to thank all the health workers in Delta State contributing to the COVID-19 response in the state and especially those directly involved in collecting the data upon which this study is based. Our gratitude also goes to the Honourable Commissioner for Health Delta State, Dr Mordi Ononye the State Epidemiologist, Dr. Richard Ikwuogu, the State Disease Surveillance and Notification Officer, Mrs. Nwakaego, Dr. Ojudume Okuguni, members of the COVID-19 Emergency Operations Center, and all State and Local government officers.
Tables and figures


Table 1: Socio-demographic characteristics of confirmed COVID-19 cases in Delta State, March to August 2020 (N=1,605)
Table 2: Predictors of mortality among COVID-19 cases in Delta State, March to August 2020
Figure 1: Surveillance Outbreak Response Management and Analysis System Workflow adapted from Vitagroup-SORMAS
Figure 2: Commonest clinical symptoms reported by confirmed COVID-19 Patients in Delta State, March to August 2020
Figure 3: Trend of COVID-19 pandemic showing weekly confirmed cases, deaths, number tested and positivity rate, in Delta State, March to August 2020
Figure 4: Spot map showing the distribution of COVID-19 cases by Local Government Areas in Delta State, March to August 2020
References


- Mayo Clinic. Coronavirus disease 2019 (COVID-19) - Symptoms and causes. Mayo Clinic. 2020. Accessed May 2020.
- World Health Organization. WHO Director-General´s opening remarks at the media briefing on COVID-19 - 11 March 2020 . WHO. 2020. Accessed May 2020.
- World Health Organization. Rolling Updates on Coronavirus Disease (COVID-19): Events as they Happen. WHO. 2021. Accessed September 2021.
- Amzat J, Aminu K, Kolo VI, Akinyele AA, Ogundairo JA, Danjibo MC. Coronavirus outbreak in Nigeria: Burden and socio-medical response during the first 100 days. Int J Infect Dis. 2020 Sep 1; 98:218-22.https://doi.org/10.1016/j.ijid.2020.06.067 . PubMed | Google Scholar
- Nigeria Centre for Disease Control (NCDC). NCDC Coronavirus COVID-19 Microsite. NCDC. 2020. Accessed October 2020.
- Ibrahim RL, Ajide KB, Julius OO. Easing of lockdown measures in Nigeria: Implications for the healthcare system. Heal Policy Technol. 2020 Dec 1; 9(4):399.https://doi.org/10.1016/j.hlpt.2020.09.004 . PubMed | Google Scholar
- Ajide KB, Ibrahim RL, Alimi OY. Estimating the impacts of lockdown on Covid-19 cases in Nigeria. Transp Res Interdiscip Perspect. 2020 Sep 1; 7:10021. https://doi.org/10.1016/j.trip.2020.100217 . PubMed | Google Scholar
- Ningthoujam R, Khomdram D. WHO statement - “Older people are at highest risk from COVID-19”: Should the hypothesis be corroborated or rejected? Med Hypotheses. 2020; 144:109896.https://doi.org/10.1016/j.mehy.2020.109896 . Google Scholar
- Liu K, Chen Y, Lin R, Han K. Clinical features of COVID-19 in elderly patients: A comparison with young and middle-aged patients. J Infect. 2020 Jun; 80(6):e14-e18.https://doi.org/10.1016/j.jinf.2020.03.005 . PubMed | Google Scholar
- Bukola A, Ayinde O, Akinyode A, Gbolahan A, Bello B. Epidemiology of coronavirus disease 2019 (COVD-19) outbreak cases in Oyo State South West Nigeria, March-April 2020. Pan Afr Med J. 2020; 35(Suppl 2): 88.https://doi.org/11604/pamj.supp.2020.35.2.23832 . PubMed | Google Scholar
- Gebhard C, Regitz-Zagrosek V, Neuhauser HK, Morgan R, Klein SL. Impact of sex and gender on COVID-19 outcomes in Europe. Biology of Sex Differences. 2020; 11:29.https://doi.org/10.1186/s13293-020-00304-9 . Google Scholar
- Hamidi S, Sabouri S, Ewing R. Does Density Aggravate the COVID-19 Pandemic? J Am Plan Assoc. 2020 Jun 18; 86(4):1-15.https://doi.org/10.1080/01944363.2020.1777891 . Google Scholar
- Acuto M. COVID-19: Lessons for an Urban(izing) World. One Earth. 2020 Apr; 2(4):317-9.https://doi.org/10.1016/j.oneear.2020.04.004 . PubMed | Google Scholar
- Chen T, Guo S, Zhong P. Epidemic characteristics of the COVID-19 outbreak in Tianjin, a well-developed city in China. Am J Infect Control. 2020 Sep; 48(9):1068-1073.https://doi.org/10.1016/j.ajic.2020.06.006 . PubMed | Google Scholar
- Day M. Covid-19: four fifths of cases are asymptomatic, China figures indicate. BMJ. 2020; 369:m1375. https://doi.org/10.1136/bmj.m1375. PubMed | Google Scholar
- Ebewore SO. Rural Folks Perception of Suicide Drivers in rural communities of Delta State, Nigeria: Implications for Societal and Agricultural Security. Open Agric. 2020 Jan 1; 5(1):50-62.https://doi.org/10.1515/opag-2020-0005 . PubMed | Google Scholar
- Nigeria Government. About Delta - Delta State Government. Nigeria Government. 2020. Accessed June 2020.
- SORMAS. AFENET. SORMAS. Accessed September 2021.
- African Field Epidemiology Network (AFENET). Nigeria COVID-19 Response: AFENET and other partners develop and implement data quality improvement plan (DQIP) for Improved Quality Data Collection. AFENET. 2020. Accessed September 2021.
- Vitagroup-SORMAS. SORMAS: Epidemien verhindern und bek�mpfen. vitagroup AG. Accessed September 2021.
- IBM SPSS. SPSS Statistics 25.0 Fix Pack 2. IBM SPSS. Accessed May 2021.
- QGIS. Download QGIS . QGIS. Accessed September 2021.
- Nigeria Centre for Disease Control (NCDC). NCDC Coronavirus COVID-19 Microsite. NCDC. 2020. Accessed October 2020.
- Bwire GM. Coronavirus: Why Men are More Vulnerable to Covid-19 Than Women? SN Compr Clin Med. 2020; 2:874-876.https://doi.org/10.1007/s42399-020-00341-w . Google Scholar
- Elimian KO, Ochu CL, Ilori E, Oladejo J, Igumbor E, Steinhardt L, Wagai J, Arinze C, Ukponu W, Obiekea C, Aderinola O, Crawford E, Olayinka A, Dan-Nwafor C, Okwor T, Disu Y, Yinka-Ogunleye A, Kanu NE, Olawepo OA, Aruna O, Michael CA, Dunkwu L, Ipadeola O, Naidoo D, Umeokonkwo CD, Matthias A, Okunromade O, Badaru S, Jinadu A, Ogunbode O, Egwuenu A, Jafiya A, Dalhat M, Saleh F, Ebhodaghe GB, Ahumibe A, Yashe RU, Atteh R, Nwachukwu WE, Ezeokafor C, Olaleye D, Habib Z, Abdus-Salam I, Pembi E, John D, Okhuarobo UJ, Assad H, Gandi Y, Muhammad B, Nwagwogu C, Nwadiuto I, Sulaiman K, Iwuji I, Okeji A, Thliza S, Fagbemi S, Usman R, Mohammed AA, Adeola-Musa O, Ishaka M, Aketemo U, Kamaldeen K, Obagha CE, Akinyode AO, Nguku P, Mba N, Ihekweazu C. Descriptive epidemiology of coronavirus disease 2019 in Nigeria, 27 February-6 June, 2020. Epidemiol Infect. 2020; 148:e208. https://doi.org/10.1017/S095026882000206X. PubMed | Google Scholar
- National Population Commission of Nigeria. Nigeria Demographic and Health Survey 2018 [Internet]. National Population Commission. 2019. Accessed October 2020.
- Mueller AL, Mcnamara MS, Sinclair DA. Why does COVID-19 disproportionately affect older people? Aging. Impact Journals. 2020 May 31; 12(10): 9959-9981.https://doi.org/10.18632/aging.103344 . PubMed | Google Scholar
- Oran DP, Topol EJ. Prevalence of Asymptomatic SARS-CoV-2 Infection?: A Narrative Review. Annals of internal medicine. 2020; 173:362-7.https://doi.org/10.7326/M20-3012 . Google Scholar
- Health JHBS of P. COVID-19 Testing: Understanding the “Percent Positive.” Johns Hopkins Bloomberg School of Public Health. 2020. Accessed September 2021.