Evaluation of the International Health Regulations core capacities at designated points of entry in Liberia, December 2019
Siatta Leemu Alberta Gray1, Tolbert Geewleh Nyenswah1, Julius Saye Miator Gilayeneh Sr1, Maame Amo-Addae2, Himiede Wede Sesay2, Obafemi Joseph Babalola2, Philip Kerkula Bemah1, Chukwuma David Umeokonkwo2
1National Public Health Institute of Liberia, Monrovia, Liberia, 2Liberia Field Epidemiology Training Program, Monrovia, Liberia
&Corresponding author
Siatta L. A. Gray, National Public Health Institute of Liberia, Monrovia, Liberia.
Introduction:
In 2014, Ebola Virus Disease (EVD) outbreak struck West Africa, leaving Liberia as the most affected nation. Two years later, a Joint External Evaluation (JEE) conducted in Liberia revealed gaps within the disease surveillance system. These gaps existed due to limited implementation of the International Health Regulation (IHR) 2005 which was adopted by Liberia in 2007. The IHR 2005 is a legally binding document which guides nations to ensure global public health security, with the establishment of minimum core capacities at ports of entry (PoEs) as a requirement to reduce the risk of disease spread. We evaluated the core capacities at eight designated ports of entry in Liberia to assess the implementation of the IHR 2005, measure progress, and set benchmarks for future interventions.
Methods:
A descriptive cross-sectional study was employed to evaluate the designated PoEs using the WHO PoE assessment checklist. The capacities assessed included vector control, cross-border coordination, quarantine, handwashing, communication, mobility, electricity, portable nearby water sources, and a trained workforce. Key informant interviews, document reviews, and direct observations at PoEs were also conducted. The result of the assessment was summarized in proportions and charts. Thematic analysis of the key informant interviews was also carried out.
Results:
All the eight PoEs assessed had electricity and workforce trained on IHR. Cross-border meetings and information sharing were held with neighbouring countries in two-thirds of the PoEs assessed. The majority (7/8) of the PoEs had a portable water source, however handwashing facilities were only available in three. Similarly, only one had communication equipment, two had vector control mechanisms in place, and two had quarantine space for suspected ill travelers. None of the PoEs had functional transportation services to move sick passengers to the designated treatment facilities.
Conclusion:
Core capacities at the study PoEs are partially established and there is a need to strengthen infrastructural, human resource, surveillance and response, communication, and vector control capacities.
Introduction

The International Health Regulation (IHR 2005) is a legally binding document on 196 countries, which aims to provide the framework for enhancing global health security in which member states take responsibility to identify, detect and respond to health threats and prevent them from spreading other states without interference with international traffic and trade [1]. This expands beyond a specific disease list to include any event that would constitute a public health emergency of international concern (PHEIC), including, new and re-emerging diseases, food safety and animal diseases, and chemical and radiological agents. Along with other states, Liberia adopted the IHR 2005 on 15 June 2007 and began its implementation but requested an extension in 2012 due to competing priorities and political challenges [2].
In 2014, the West Africa Ebola Virus Disease outbreak struck Guinea, Sierra Leone, and Liberia, with Liberia being the most affected nation with 4,808 deaths [
3]. To strengthen disease surveillance infrastructure after the outbreak, Liberia conducted a Joint External Evaluation (JEE) in 2016 [
4], which was a multi-sectoral process and was performed as a peer-to-peer collaboration between national and international experts, using a standard tool to review national capacities across 19 technical areas related to global health security. The JEE is one of the core components of the IHR (2005) monitoring and evaluation framework designed to assess required core capacities [
1].
The outcome of JEE revealed that inadequately trained human resources, insufficient logistics, inadequate coordination between different partners, and sustainability of efforts instituted were major challenges in the implementation of the IHR (2005) at the PoEs [
4]. In response to the findings, the Government of Liberia established the National Public Health Institute of Liberia (NPHIL) to improve disease surveillance, laboratory and outbreak response capacity and efficiency for detection and response to public health threats, while avoiding interruption of routine services in Liberia. This would be done through detection, prevention, and response to public health threats or events [
5]. Upon its establishment, the NPHIL developed a five-year Strategic Plan with targets set to achieve the Global Health for Security Agenda (GHSA), the Sustainable Development Goals (SDGs), and the IHR (2005), focusing especially on the ports of entry (PoE) core capacities, among others. Article 20 of the IHR (2005) requires State Parties to designate the airports and ports and develop the capacities provided in Annex 1b which states that parties are to ensure that these core capacities are present and functioning throughout their territories as set out in Article 5 and 13 of the IHR (2005) [
1]. The core capacities include access to medical services with adequate staff, mobility and communication equipment, a safe environment for travelers using the PoE facilities like water supply, electricity, toilets, etc., and a vector control practicable program at the PoEs. Additionally, in case of any emergency, there should be quarantine space for suspected travelers or animals, preferably in facilities away from PoE.
We conducted an evaluation of the core capacities in December 2019, at eight designated ports of entry in Liberia to assess the implementation of the IHR (2005), measure progress since NPHIL´s establishment, and set benchmarks for future interventions.
Methods


Study setting
Liberia is located on the west coast of Africa, bordered by Sierra Leone, Ivory Coast, and Guinea, and has 15 counties with an estimated population of 4.9 million people [
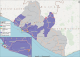
6]. Liberia has 131 points of entry, out of which, 47 were official and 8 were designated in line with the emergency preparedness and response provisions of the IHR (2005). These eight points of entry: Roberts International Airport, James Spring Field Airport, Ganta ground crossing, Loguatuo ground crossing, Yekepa ground crossing, Bo-Waterside ground crossing, Buchanan Seaport, and the Sea Port of Monrovia, were tasked with specific duties during events that may have severe implications for international public health
Figure 1.
The designation of eight of these ports was based on the high volume of people crossing, and the ease of accessibility of these PoEs by travelers [
7]. These ground, sea, and airports handle over 3000 travelers weekly, with Robert´s International Airport and Bo-Waterside land crossing accounting for the highest number of travelers
Table 1.
Study design
We conducted a descriptive cross-sectional study using a mixed approach of qualitative and quantitative methods. The WHO PoE assessment checklist was used to assess the core capacity requirements at designated PoEs. The checklist assesses the current status of existing core capacities to identify gaps and other system requirements to accommodate the implementation of the IHR [
8].
Sample size and sampling technique
Of the 131 PoEs in Liberia, eight were purposefully selected because they are the designated PoEs in Liberia. In each of the selected ports of entry, stakeholders who were involved in the port services operation were selected purposively for the assessment. The participants included members of the staff from Port Health, National Immigration Services, National Security Agency (NSA), Ministry of Agriculture, Liberia Revenue Authority, and Liberia National Police, who were assigned to those ports of entry. In total, 20 participants were selected for the qualitative arm of the study. All eight selected POEs were included in the quantitative arm of the study.
Point of entry core capacities and definition of variables
We assessed eight point-of-entry core capacities within the WHO assessment tool [
9,
10]. These core capacities included: vector control mechanism, cross border coordination, quarantine for travelers, hand washing procedure, communication equipment (VHF radio, telephone, and HF radio), mobility equipment (motorcycle, vehicle), electricity supply, portable nearby water source, and trained workforce in IHR 2005. The authors used the following working definitions for each of the POE core capacities.
Vector Control: program established for the reduction of vector populations in and around the port of entry to a minimum distance of 400 metres with an extension of the minimum distance if vectors with a greater range are present. A PoE is considered to have a vector control program if vectors and reservoirs are detected, identified, tested for pathogens and controlled. Results of the latest audit of services and facilities should be available and accessible [
1].
Cross Border Coordination: Communication with competent authorities at other points of entry, internationally, to provide relevant information regarding evidence found and control measures still needed on arrival of affected conveyance. A PoE is considered to have cross-border coordination if cooperation is being fostered with other ports of entry across borders through meetings and other forms of communication. The researchers asked for copies of the minutes of the previous meetings to confirm the meetings held [
1].
Quarantine: is an independent space through which suspected travelers can be kept until transported to medical care facilities, if needed, in order to avoid infecting other persons. A PoE is considered as having a quarantine space if there is an independent exit passage through which suspect travelers can be transported to medical care facilities, if needed, to avoid infecting other persons [
1].
Handwashing: the presence of hand washing materials and practice. A PoE is considered to practice handwashing if there is a handwashing station with running water, either from a basin or bucket [
1].
Communication equipment: enabled device provided by authorities that allows information sharing. A PoE is considered to have communication equipment if they report all available essential information on events occurring and point of entry by competent authority to health authority at the local, intermediate, or national level for public health assessment, care and response through a port-assigned communication device (computers, cellphones, vhf radio, etc.) [
1].
Mobility equipment: equipment for the transportation of ill travelers to the appropriate medical facility. A PoE is considered to have transportation equipment if arrangements are in place for transporting ill travelers to the appropriate medical facility by safe, hygienic means of transport [
1].
Electricity: having access to the electricity supply through a generator, hydroelectricity, or solar panel. A PoE is considered to have electricity if it maintains at least 12 hours of power daily [
1].
Water Safety: potable nearby water sources. A PoE is considered to have water safety if there are potable water sources, under surveillance and supervision, in secure places, far away from sources of pollution, approved by the relevant health authority and if quality is considered satisfactory under national standards [
1].
Trained Workforce: personnel trained in IHR (2005)/IDSR. A PoE is considered as having a trained workforce if personnel have undergone a training program in IHR (2005)/IDSR, to recognize disease symptoms and are familiar with procedures regarding prompt assessment, care, and reporting of ill travelers [
1].
Data collection
We conducted face-to-face key informant interviews to gather data on the implementation status of the IHR (2005) core capacities at the PoEs and also conducted a document review and direct observation guide to validate findings revealed from the key informant interviews (KIIs). These methods constituted qualitative data collection while the WHO PoE assessment checklist was used to collect quantitative data.
Data analysis
Data gathered from the respondents were cleaned and uploaded into Microsoft Excel for analysis. Thematic analysis was conducted on qualitative data capturing the themes and emerging concepts based on the research objectives and results were presented as frequencies, narratives and verbatims. Quantitative data underwent descriptive analysis and results were presented as frequencies and percentages.
Results


Distribution of respondents
We visited the eight designated PoEs to assess their IHR (2005) core capacities. We interviewed 20 port staff members: four (4) at Roberts International Airport, four (4) at James Spring Field Airport, four at Ganta ground crossing, two (2) Loguatuo ground crossing, two (2) at Yekepa ground crossing, four at Bo-Waterside ground crossing, two (2) at Buchanan Seaport, and the four (4) at Sea Port of Monrovia.
Core capacities
All the POEs assessed reported having trained workforce and none had mobility equipment at the time of the study (
Figure 2). About 75% of the POEs conduct cross-border coordination meetings and information sharing, all the POEs had electricity supply up to 12 hours in a day and communication equipment was only present in 12.5% of the POEs assessed
Figure 2.
Vector Control Mechanism
Through document review, it was revealed that there was no vector control program developed at 75% (6/8) of the PoEs. Also, no vector control measures were implemented at all the PoEs, like disinfecting travelers´ baggage with insecticides and pesticides. However, PoE officers cleaned the environment regularly and ensured that there were no breeding sites for vectors in the surrounding area of the PoE up to a minimum of 400 metres. The lack of insecticide and pesticide was described by one of the PoEs:
‘…fumigation supplies like insecticides and pesticides are not provided or even mosquito spray at least. Previously, these supplies were provided by partners in the country, but ever since this project ended, we have not received any supplies for vector control measures.’ Land PoE, Logatuo
Trained Workforce in IHR
Respondents at all the PoEs were trained in IHR (2005) guidelines and IDSR guidelines and were knowledgeable about these guidelines. This was corroborated by one of the key informants interviewed,
‘… have been trained in the IHR and the IDSR guidelines. They are regulations that prevent and control the spread of diseases from one country to another and boost global security.’ Land PoE, Ganta.
Quarantine
Most of the quarantine units built by the partners during the Ebola virus disease outbreak were no longer functional due to lack of maintenance and nature of the temporary materials they were made of. Travelers could only be quarantined at 25% (2/8) of the PoEs and in the remaining POEs without quarantine facilities, travelers suspected of infection with high-risk conditions were referred to the nearby health facility for treatment. The difficulty in handling infectious diseases at POE was captured in the response of one of the key informants, who reported that,
‘whenever we suspect a sick person or traveler by physical examination or the thermometer, we take them to the nearest health facility on our side of the border or send them back to where they came from because there is nowhere to keep them…’
Portable Water Source
Of the eight PoEs assessed, 87.5% (7/8) have a portable and clean water source nearby, but Bo Waterside did not have one. A participant from Land PoE, Bo Waterside reported that
“there is no hand-pump water near us, we either have to walk miles to fetch water or drink from the creek around here; this is dangerous for our health.” The response was confirmed by the observational findings at the port of entry.
Mobility Equipment
None of the PoEs had a means of transportation for sick travelers in case of emergency. The assigned PoE´s motor bikes were seen but none was functional due to the lack of funding and maintenance. Also, all the PoEs had non-functional or no ambulances. To aid transportation of sick travelers, port staff carry travelers on their personal motorbikes, if available, or a commercial bike. A respondent from Land PoE, Loguatuo informed researchers that,
“…we don´t have any means to take sick travelers to the health facility. We use our personal bikes to carry sick travelers to the nearby health facility, which is more than 30 minutes away.” Also, PoE staff from Land PoE, Bo Waterside said,
‘Since this bike was sent, there has been no money to service it. As a result, it has broken down and we have nothing to use for referral’.
Hand Washing (IPC)
Five out of eight (62.5%) PoEs assessed had no handwashing post. Respondents reported that handwashing procedures were not being carried out routinely as it used to be because partners had stopped facilitating the structures and supplies. Respondent from Land PoE, Ganta, reported that
“during Ebola, partners brought supplies, such as buckets, soap, and they built a tarpaulin structure as post for washing hands, but everything has gotten spoiled and we have not received new supplies…”
Electricity
At all the PoEs, respondents reported that there was some means of electricity, either through public supply or generator. Respondent from Land PoE, Loguatuo stated:
‘…We are being supplied with power by the Ivorian side…’ Researchers observed that there was electricity provided at those PoEs, confirming respondents´ report.
Cross Border Coordination
Study respondents reported that cross border meetings were held with counterparts in Sierra Leone, Guinea, and Ivory Coast. This was observed in 75% (6/8) of the POEs assessed. One of the key informants from a land border POE reported that
‘...we have meetings every other month and the meetings are rotational…’
Communication Tool
7/8 of the PoEs assessed (87.5%) of respondents informed the researchers that communicating health risks was a challenge because there was no means provided at the PoEs; there were no computers, printers, VHF radio, UHF radio, or telephone. They had their personal cell phones only.
A Respondent from Land PoE, Bo-Waterside said,
‘…there is no telephone, computer, not even VHF radio to communicate. We use our personal phones…and the thing is, at this border, there is no gsm coverage and we must use the coverage of Sierra Leone in order to communicate on our cell phones. It is important that they provide us at least VHF radio to pass information from the port’.
Another Respondent said:
‘I use Sierra Leone coverage and the nearby health facility is far from here and the health workers use Liberia coverage. We cannot communicate with each other. I have to carry the suspected person on my bike, and when we get there, we sometimes wait to be attended to because preparation wasn´t made prior to our arrival.’
Discussion


There have been significant challenges regarding the implementation of international health regulation at points of entry in low- and middle-income countries including Liberia [11]. We reviewed the level of operation of the core capacities in the designated PoEs in Liberia. We found that the minimum core capacities needed at the PoEs according to IHR (2005) regulations, were partially implemented. This poses a risk of the spread of infectious diseases across the border from one country to another. There is a need to quickly strengthen these core capacities to improve the ability of these borders to quickly detect and appropriately respond to the possible spread of infectious disease at international PoE.
Annex 5 of the IHR (2005) requires State Parties to establish programs that would control vectors capable of transporting infectious agents constituting a public health risk. Such a program must ensure that vectors are controlled to a minimum distance of 400 meters from the point-of-entry facilities [
1]. However, our findings showed that vector control is still a challenge at the various ports of entry assessed. There is no specially designed program to apply recommended measures to disinfect, derat, disinfect, decontaminate, or otherwise treat baggage, cargo, containers, conveyances, goods or postal parcels and there are no locations designated and equipped for this purpose. No audits were done, and no results of the audit of services and facilities were available and accessible. Although few ports seem to do better than the rest, it is important that every port of entry has a vector control mechanism in place. Vector control mechanisms has been found to be effective in curtailing spillover of infectious diseases into the country. China implemented an effective border vector control mechanism in its malaria elimination efforts [
12].
Annex 1B of the IHR (2005) requires State Parties to provide trained personnel for the inspection of conveyances and other services, including the conduct of IDSR/IHR (2005) training and simulation exercises at PoEs [
1]. Significant efforts have been made in training the port staff in IDSR/IHR (2005) at the PoEs in Liberia. This is particularly important and may have been associated to the lessons learnt from the 2014 EVD outbreak. However, we noted that while the port health staff at the PoEs have been trained, the other staff from other arms of government supporting the port services (National Immigration Services, National Security Agency, Ministry of Agriculture, Liberia Revenue Authority, and Liberia National Police) have not been trained in IDSR/IHR. There is a need to further enhance the collaborative works of all the staff that work at PoEs by ensuring that they were all trained in required areas. Training port staff from other agencies is as important as training health workers at these PoEs, as one health approach is required in responding to PHEIC. It has been reported that the training needs of the different staff that work at the PoE might be different so is the approach of training [
13]. This should be considered while planning the scaleup of training to the other PoE staffs. Our finding contrasts with that reported by Wamala JF, Okot C, Makumbi I, et al in their study [
14], in which they noted that port health staff in Uganda were not trained on IHR. Additionally, it is also required to conduct simulation exercises on workforce capacities at designated PoEs, but contrary to these requirements, no such exercises had been conducted up to the time of our study which was also found in an assessment conducted in Sri Lanka[
15].
Having screening and temporary holding areas for humans or animals is one of the requirements at PoEs [
1]. The majority of the PoEs assessed did not screen passengers and had no facilities for the isolation/care of affected travelers. Sick travelers were referred to the nearby clinic for treatment immediately upon detection. The lack of screening and isolation facilities exposes staff and other passengers to a higher risk of infectious diseases at the PoE and if poorly managed could lead to a major outbreak of the disease in the country. Having an isolation area and a safe means of transporting sick traveler from the PoE to the designated facility for proportion treatment could save the country and the entire West African region from another major disease outbreak. An example was the Ebola virus disease outbreak in Lagos Nigeria[
16]
We found that safe portable water sources were available in the majority of the PoEs similar to Sri Lanka´s assessment [
16] which revealed that activities were carried out to ensure a safe environment for travelers including potable water supplies, this is commendable, and effort should be put in place to ensure that all the PoEs have access to potable water.
However, despite the availability of potable water in most of the POEs, only a few reported having facilities for hand washing. Not having such a facility could increase the risk of transmission of communicable diseases especially those transmitted by contact such as COVID-19, influenza, and other respiratory pathogens. There should be functional hand hygiene stations and other infection prevention measures together with appropriate personal protective equipment maintained at all POEs to minimize the spread of disease from person to person.
Functional communications equipment to send and receive prompt and accurate information about disease threats from and to appropriate sister agencies to help contain the risk of infectious disease at the PoEs is a key requirement. Our study found these were lacking in most of the PoEs assessed. This made communication difficult and, in some cases, impossible. This could put the PoE staff and the entire country at risk of infectious disease as there could be delays in alerting them of ill passengers before arrival to make the appropriate preparations to mitigate the situation and contain possible spread.
Limitation
The study results are subject to some limitations. Due to limited financial resources, we could not cover all of the PoEs in Liberia. However, the findings are representative of the country´s border preparedness, surveillance, and response capacities as the PoEs assessed were designated by the WHO. Moreover, this study revealed important findings that set the baseline for future interventions and guide policy decisions.
Conclusion


The evaluation highlighted critical gaps to guide the IHR (2005) implementation at the ports of entry. The core capacities at the designated PoEs evaluated are partially implemented. Infrastructural and human resource capacities at POEs, surveillance and response capacities, quarantine, coordination among staff, and mechanisms for vectors and reservoir control should be enhanced. A vector control program should be developed with measures applied to disinfect, derat, disinfect, decontaminate, or otherwise treat baggage, cargo, containers, conveyances, goods or postal parcels including, when appropriate, at locations specially designated and equipped for this purpose. There should be the provision of appropriate space, separate from other travelers to interview suspected or affected persons. All port staff should be trained in surveillance and response programs, including vector and conveyance, IDSR, and IHR (2005), and not just staff in health services. Additionally, IPC procedures should be followed to the letter, especially handwashing, which is a minimum core capacity. We also recommend that basic communication be provided to port health staff to ease communication within them and with other agencies at the PoE and externally. Additionally, WAHO should engage with countries in the region to prioritize PoE strengthening as a health security priority and support regional PoE planning meetings, joint cross-border simulation exercises and facilitate regular sharing of health risk information across international borders in the region. Lastly, a follow-up assessment should be done using the 2020 WHO PoE assessment tool, since this study was done prior to its release.
What is known about this topic
- The International Health Regulation (IHR 2005) is significant in preventing, controlling, and responding to public health emergencies of international concern.
- Liberia is required to establish and maintain minimum core capacities at ports of entry.
What this study adds
- There are major gaps in the core capacities at the designated ports of entry in Liberia that need immediate and decisive action to curtail the spread of disease through these ports
Competing interest


The authors declare no competing interests.
Authors´ contribution


SLAG and PKB developed the protocol, collected, analyzed and interpreted the data. SLAG wrote the initial draft, and TN, JG, JB, MAA, CDU, and HWS reviewed several drafts and provided critical comments. All authors read and approved the final manuscript.
Acknowledgment


The authors are grateful to the National Public Health Institute of Liberia for the financial support given to conduct this research, and the Liberia Field Epidemiology Training Program for the technical support in developing this manuscript.
Tables and figures


Table 1: Weekly volume of passenger traffic at the designated ports of entry in Liberia, 2019
Figure 1: Distribution of the designated ports of entry in Liberia, 2019
Figure 2: Distribution of core capacities in the POEs following the assessment, 2019
References


- WHO. International Health Regulations (2005) [Internet]. 3rd ed. Geneva (Switzerland): World Health Organization; 2016 [cited 2024 Feb 9]. 74p. Google Scholar
- Ijaz K, Kasowski E, Arthur RR, Angulo FJ, Dowell SF. International Health Regulations– What Gets Measured Gets Done. Emerg Infect Dis [Internet]. 2012 Jul [cited 2024 Feb 9];18(7):1054-7. https://doi.org/10.3201/eid1807.120487 PubMed | Google Scholar
- Nyenswah TG, Kateh F, Bawo L, Massaquoi M, Gbanyan M, Fallah M, Nagbe TK, Karsor KK, Wesseh CS, Sieh S, Gasasira A, Graaff P, Hensley L, Rosling H, Lo T, Pillai SK, Gupta N, Montgomery JM, Ransom RL, Williams D, Laney AS, Lindblade KA, Slutsker L, Telfer JL, Christie A, Mahoney F, De Cock KM.Ebola and Its Control in Liberia, 2014-2015 . Emerg Infect Dis [Internet]. 2016 Feb [cited 2024 Feb 9];22(2):169-77. https://doi.org/10.3201/eid2202.151456 PubMed | Google Scholar
- WHO. Joint External Evaluation of IHR Core Capacities of the Republic of Liberia - Mission report: September 2016 [Internet]. Geneva (Switzerland): World Health Organization; 2017 May 8[cited 2024 Feb 9]. 57p. Download WHO-WHE-CPI-2017.23-eng.pdf.
- Africa CDC. Providing a Legal Framework for a National Public Health Institute (NPHI) [Internet]. Addis Ababa (ET): Africa Centres for Disease Control and Prevention; 2019 Sep 9 [cited 2024 Feb 21]. 79p. Download Providing-Legal-framework-NPHIs.pdf. PubMed | Google Scholar
- UN. United Nations population estimates and projections [Internet]. New York (US): United Nations; [cited 2024 Feb 19].
- UN Office for the Coordination of Humanitarian Affairs. Liberia: Border Crossing Points [Internet]. United Nations Office for Coordination of Humanitarian Affairs; 2015 Aug 4[cited 2024 Feb 9]. 1p. Download liberia_a3_150804_border_points.pdf.
- WHO. International Health Regulations (2005) Assessment tool for core capacity requirements at designated airports, ports, and ground crossings [Internet]. Geneva (Switzerland): World Health Organization; 2020 Oct 12[cited 2024 Feb 9]. 39 p. Download WHO_HSE_IHR_LYO_2009.9_eng.
- WHO. Protocol for Assessing National Surveillance and Response Capacities for the International Health Regulations (2005) in Accordance with Annex 1 of the IHR - A Guide for Assessment Teams. Geneva (Switzerland), World Health Organization; 200 Dec [cited 2024 Feb 9] 145p. WHO/HSE/IHR/2010.7.
- WHO. Protocol for the assessment of national communicable disease surveillance and response systems: guidelines for assessment teams [Internet]. 145p. World Health Organization; 2001[cited 2024 Feb 9] 121 p. Download WHO/CDS/CSR/ISR/2001.2.
- Lokossou VK, Usman A, Sombie I, Paraiso MN, Balogun MS, Umeokonkwo CD, Gatua J, Wagai J, Ouendo EM, Nguku P.COVID-19 pandemic in Economic Community of West African States (ECOWAS) region: implication for capacity strengthening at Point of Entry . PAMJ [Internet]. 2021 May 25[cited 2024 Feb 9]; 39:67. https://doi.org/10.11604/PAMJ.2021.39.67.29089 PubMed | Google Scholar
- Xu JW, Lin ZR, Zhou YW, Lee R, Shen HM, Sun XD, Chen QY, Duan KX, Tian P, Ding CL, Xu SY, Liu H, Zhou HN.Intensive surveillance, rapid response and border collaboration for malaria elimination: China Yunnan´s “3 + 1”strategy . Malar J [Internet]. 2021 Oct 9[cited 2024 Feb 9];20(1):396. https://doi.org/10.1186/s12936-021-03931-8 PubMed | Google Scholar
- De Rooij D, Belfroid E, Hadjichristodoulou C, Mouchtouri VA, Raab J, Timen A.Assessing training needs in infectious disease management at major ports, airports and ground-crossings in Europe . BMC Public Health [Internet]. 2021 May 29 [cited 2024 Feb 9];21(1):10. https://doi.org/10.1186/s12889-021-11008-z PubMed | Google Scholar
- Wamala JF, Okot C, Makumbi I, Natseri N, Kisakye A, Nanyunja M, Bakamutumaho B, Lutwama JJ, Sreedharan R, Xing J, Gaturuku P, Aisu T, Da Silveira F, Chungong S. Disease surveillance, capacity building and implementation of the International Health Regulations [IHR(2005)] . BMC Public Health [Internet]. 2010 Dec 3[cited 2024 Feb 9];10 (Suppl 1): S9. https://doi.org/10.1186/1471-2458-10-S1-S9 PubMed | Google Scholar
- MOH, Directorate of Quarantine (Sri Lanka). Assessment of core capacities at points of entry, Sri Lanka to implement International Health Regulations (2005)[Internet]. Ministry of Health, Directorate of Quarantine Ministry of Health (Sri Lanka); 2013[cited 2024 Feb 9]. 38p. Supported by the International Organization for Migration (IOM).
- Otu A, Ameh S, Osifo-Dawodu E, Alad e E, Ekuri S, Idris J.An account of the Ebola virus disease outbreak in Nigeria: implications and lessons learnt . BMC Public Health [Internet]. 2017 Jul 10 [cited 2024 Feb 9];18(1):3. https://doi.org/10.1186/s12889-017-4535-x Google Scholar