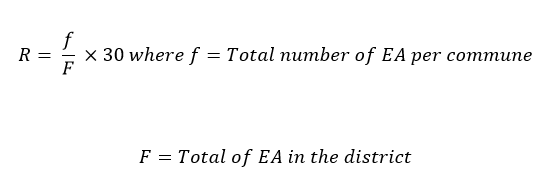Prevalence and factors associated with the use of modern contraceptive methods in the health district of Djibo, Sahel region in Burkina Faso
Smaïla Ouédraogo1,2,3,&, Adama Ouattara1,4, Maurice Sarigda5, Laurent Ouédraogo1, Charlemagne Ouédraogo1,4
1Université Joseph Ki-ZERBO, Ouagadougou, Burkina Faso, 2Unité de Recherche sur le Paludisme et le VIH/SIDA, Ecole Doctorale Sciences de la Santé, Laboratoire de Santé Publique, Université Joseph Ki-ZERBO, Ouagadougou, Burkina Faso, 3Centre Hospitalier Universitaire Yalgado Ouédraogo, Ouagadougou, Burkina Faso, 4Centre Hospitalier Universitaire de Bogodogo, Ouagadougou, Burkina Faso, 5Programme d´appui au développement sanitaire (PADS), Ministère de la santé, Ouagadougou, Burkina Faso
&Corresponding author
Dr Smaïla Ouédraogo, Université Joseph Ki-ZERBO, Ouagadougou, Burkina Faso 13 BP 40 Ouagadougou 13
Email: smaila11@yahoo.fr
Background
Improving contraceptive prevalence in resource-limited countries is one of the cost-effective strategies to reduce the high and unacceptable global maternal mortality rate. This study was conducted to determine the prevalence and factors associated with the use of contraceptive methods in Burkina Faso.
Methods:
We performed a cross-sectional study in 2015 which involved women of childbearing age who were engaged in sexual intercourse activities. Multivariable logistic regressions were performed to identify the factors associated with the use of modern contraceptive methods.
Results:
A total of 761 women were included in the survey. Overall, modern contraceptive prevalence in the district was 18.1% ([95 % confidence interval (CI): 15.1%-21.1%]). After adjustment, women aged 21-30 years used modern contraceptive methods in the 12 months prior to the survey more than the others (Adjusted odds ratio (AOR) = 2.5; 95% CI: [1.3-4.8]). Traders (AOR = 0.1; CI: [0.04-0.5]), housewives (AOR = 0.2; CI: [0.07-0.6]), and farmers (AOR = 0.05; [0.01-0.2]) reported using a contraceptive method less than students. Similarly, indigenous women used modern contraception less than those who had lived in the study area for less than two years (AOR = 0.3; CI: [0.1-0.7]).
Conclusion:
The prevalence of modern contraceptive use in the Djibo health district is low. Some professional activities and indigenous status are factors favoring the non-use of moderne contraceptive methods. Programs targeting indigenous women, housewives and traders could help to fill the gap in modern contraceptive methods utilization.
Background

Global maternal mortality remains unacceptably high, with an estimated 303,000 women dying each year as a result of pregnancy and childbirth-related complications[1]. Despite the decline of maternal deaths worldwide by 44% between 1990 and 2015, this achievement fell far short of the 75% reduction targeted by Millennium Development Goal 5a[1,2]. To strengthen efforts to reduce maternal mortality ratio, the global community set 17 new goals in 2016 as part of the Sustainable Development Goals (SDGs). One of the targets of SDG 3 is to be below 70 deaths per 100,000 live births by 2030[3,4]. The reasons for lack of progress are complex and multifactorial[5-10].
To address the lack of steady progress across all countries and reassert the importance of the unfinished agenda of reducing maternal mortality in the SDG era, the World Health Organization (WHO) released a direction setting report entitled “Strategies toward ending preventable maternal mortality (EPMM)” (EPMM Strategies) in February 2015[
4]. EPMM Strategies has 25 indicators that are well harmonized with the Indicator and Monitoring Framework for the Global Strategy, SDGs 3 and 5. Of the 25 indicators, two focus on gender equality and empowerment of all women and girls, and sexual and reproductive health : the presence of laws and regulations that guarantee women aged 15-49 access to sexual and reproductive health care, information, education, and the proportion of women aged 15-49 who make their own informed decisions regarding sexual relations, modern contraceptive methods (MCM) use, and reproductive health care[
3]. A good family planning system that provides the necessary services to the population is a sure way to accelerate the achievement of these goals.
The WHO defines family planning as “The ability of individuals and couples to anticipate and attain their desired number of children and the spacing and timing of their births. It is achieved through use of MCM and the treatment of involuntary infertility”[
11]. Improving MCM utilization prevalence in resource-limited countries is one of the strategies to achieve this goal[
2,
12]. Indeed, it has been shown that increasing the choice of MCM and the commitment of different countries to family planning increases the continuous use of contraceptives[
13].
There is little data on the use of MCM among adolescents in sub-Saharan African countries, particularly among secondary school students. The analysis of data collected on women from 20 African countries showed that the overall prevalence of MCM was 26%. Women were more likely to use a MCM if they had at least a primary education and were of middle-income status or rich[
14]. In a study from Ghana, 95% of the respondents exhibited some knowledge about contraceptives, but the use of MCM remained low as the prevalence rate was 18%[
15]. The analysis of the Uganda Demographic and Health Survey 2016 data revealed that the prevalence of MCM utilization among female adolescents was 9.4%. The frequency of contraceptives utilisation was higher among married adolescents compared to unmarried adolescents[
16]. In Zambia, a surveys focusing on adolescent girls showed that contraceptives use remains low and ranged from 7.6% in 1996 to 10.9% in 2014, reflecting a change of 3.3 percentage points over 18 years. Over the 18 years, contraceptive use was significantly associated with age, level of education, and marital status[
17].
As many sub Saharan Africa countries, Burkina Faso has high fertility rate with poor knowledge and utilization of family planning methods among women of childbearing age[
18,
19]. A survey conducted in Burkina Faso between 2017 and 2018 showed that MCM utilization prevalence among women of childbearing age was 26%[
20]. Another survey that analyzed data from the 2003 and 2010 Demographic and Health Surveys found that MCM use prevalence among adolescents aged 15-19 is low in Burkina Faso, estimated at 11.2%[
19]. According to data from the Burkina Faso Ministry of Health routine report, MCM utilization prevalence in the Djibo Health District (DHD) (one of 55 health districts in the country), is particularly low, at 23.5% compared to a national average of 32% in 2013[
21]. The district's family planning statistics are based on data collected regularly by the national health system, which are incomplete and appear to be overestimated. To address this shortcoming, this study was conducted to determine MCM prevalence and identify factors associated with its use in the DHD in the Sahel region of Burkina Faso.
Methods


Study design
We analysed data of cross-sectional study performed between January 28 and February 7, 2015.
Study site
The study took place in the DHD in the Soum province, Sahel region of Burkina Faso. The Soum province has 9 communes, 9 departments and 198 administrative villages. The DHD is part of the Sahel regional health directorate, one of the 13 regional health directorates in the country. Djibo, the capital of the DHD, is located 200 km from Dori, the capital of the region, and Ouagadougou, the capital of Burkina Faso. The population of the DHD was estimated at 442,973 inhabitants in 2014 and the proportion of women of reproductive age (15 - 49 years) is 22.3%. According to the Ministry of Health's 2013 statistical yearbook, MCM utilization prevalence in the district was 23.5%[
21].
Study population
Sample size and sampling
In this study, MCM included the intrauterine device, the oral contraceptive pills, the contraceptive patch, the contraceptive implant, the vaginal ring, the cervical diaphragm and the female condom. We assumed the MCM utilization prevalence is 18% instead of 23.5% as reported by the Ministry of health[
21]. With a precision of 5% and a confidence level of 95%, 441 women of reproductive age who were engaged in sexual relations were needed to show a MCM utilization prevalence of 18% in the district. Assuming a 15% non-response, the sample size was increased to 507. To take into account a potential cluster effect which has been established at 1.5, the final sample size was 761 women of reproductive age.
The enumeration areas (EA) in DHD were selected using Excel 10 software, based on the EA file used by the National Institute of Statistics and Demography for the 2010 general population census. We selected 30 EA following the WHO vaccination coverage cluster surveys reference manual[
22]. Afterwards, the number of EA per commune (R) was proportionally determined until we had a total of 30 EA using the following formula:
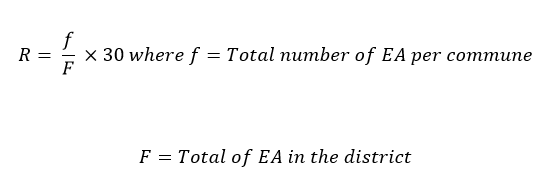
Within each commune, we randomly selected the required number of EA. The number of women to include in the survey by EA (n) was made in proportion to the weight of each EA according to the formula below:

To select the participant, we opted for the pen-and-paper technique. From a public square or the center of the EA, the interviewer throws a pen upwards. As the pen falls back down, the cap of the pen points in a direction to find the first yard. In each courtyard, the survey began with the first household located at the entrance and to the right. After the first household, the survey continued in close succession until they obtained the required number of persons per EA. In each household, the interviewer recruited all women of childbearing age who were engaged in sexual relations (15-49) until we reached the required number of persons for the EA.
Inclusion and exclusion criteria
To be included in the study, a woman had to be between the ages of 15 and 49 years, engaged in a sexual relation, agree to the survey procedures, and give her consent to participate. All women who did not reside in the selected EA and those whose spouses refused the participation were excluded from the survey.
Variables
The outcome variable was the use of a MCM and was measured through a questionnaire during the survey in the households. MCM were defined as intrauterine devices (IUD), implants, injectables, the pill, condoms, and sterilization. The outcome variable was coded as a binary variable: ‘yes’ for women who reported using a MCM in the last 12 months, and ‘no’ for those not using any MCM. Sociodemographic variables (age, place of residence, occupation, level of education, religion, ethnicity and marital status) and knowledge of contraceptive methods. Women's knowledge of MCM was measured by assessing their knowledge of the goals and types of contraceptive methods. Thus, a woman had knowledge of MCM if she was able to name at least one benefit of contraception and at least one type of MCM. She had no knowledge otherwise.
Data collection technique, tools and procedures
A semi-structured interview following a questionnaire was used for data collection in this study. Interviewers and supervisors were recruited and trained for two days. The questionnaire was tested to ensure their consistency and to make adjustments where necessary. During the survey, supervisions were conducted to ensure the quality of data collection.
Data management and analysis
The questionnaires were manually counted to check for completeness and consistency of completion. The data were entered into CSPro and analyzed with Stata 12.0 software. The general characteristics of the study population were described by determining means for continuous variables and proportions for categorical variables.
We first described the study population. The MCM use prevalence was estimated by dividing the number of women of the study sample using MCM by the total of women included in the study x 100. Afterwards, we conducted a univariate and a multivariable stepwise logistic regression to identify factors associated with modern contraceptive methods use. All variables that were associated with contraceptive use with a p-value < 20% in the univariate analysis were considered in the multivariate analysis. At the end of the multivariate analysis, only variables with a p-value of less than 5% were kept in the final model.
Ethical statement
The protocol had the ethical clearance of the Comité d´Ethique pour la Recherche en Santé in Burkina Faso (Reference ID 2014-01-186). All study participants provided written informed consent. In addition, the confidentiality of the interviews and responses to questions was preserved.
Results


A total of 802 women were approached for participation in the study; of them, 41 (5.1%) were non-respondents. Finally, 761 women were included in the survey. Table 1 presents the women´s general characteristics. In the study, 42.2% of the women were between 21 and 30 years of age, and women with no education represented 67.8%. Also 19.3% of the women had attended primary school and 12.9% of them had reached secondary school. The results showed that 69% of the women are housewives and 20% of them are engaged in trade or agricultural activities. Of the participants, 7.2% were students. The study indicated that, 49.2% of the women were indigenous to their village, i.e., they had lived there since birth.
Figure 1 shows the prevalence of MCM use by commune in the DHD. Overall, MCM use prevalence in the DHD is 18.1% (138/761) (95 % confidence interval (CI): [15.1%-21.1%]). The communes of Kelbo and Diguel constitute the two extremes with the highest (42.1%) and lowest (0.0%) MCM utilization prevalence, respectively.
Table 2 presents the factors associated with MCM use in the DHD. In the univariate analysis, we found that the use of MCM was associated to women´s age, material status, ethnicity, religion, education, occupation, knowledge of contraceptive methods, duration of residence and discussion on the family planning. However, after adjustment using logistic regression multivariate analysis, only age, occupation, and duration of residence in the area are the factors significantly associated with the use of a MCM. Women aged 21-30 years reported using an MCM more than others in the 12 months before the survey (Adjusted odds ratio (AOR) = 2.5; 95% CI: [1.3-4.8]). Traders (AOR = 0.1; [0.04-0.5]), housewives (AOR = 0.2; [0.07-0.6]), and farmers (AOR = 0.05; [0.01-0.2]) reported using a MCM less than students. Similarly, women native to the DHD reported infrequent MCM use compared to those who had been in the area for less than 2 years (AOR = 0.3; [0.1-0.7]).
Discussion


This study showed a low level of MCM utilization and a disparity of its use between communes in the DHD. The communes of Diguel and Kelbo present the extreme values in terms of MCM use prevalence in the district. Similarly, we have shown that age, occupation, and duration of residence in the district are factors that influence the use of MCM.
As with many behavioral studies, this study relied on the opinions and statements of respondents, which were sometimes difficult to verify. The subject of family planning remains taboo, especially in rural areas like the DHD. As a result, some respondents said little about the subject during the survey. Some adolescents interviewed in a family setting may not have expressed themselves freely because of fear of their parents, despite the confidentiality measures taken by the interviewers. This may have led to an underestimation of the MCM use prevalence.
The global contraceptive prevalence observed in the DHD is below the national average of 32.4%, according to Ministry of Health 2013 statistical yearbook[
21]. The prevalence reported by the Ministry of Health derives from routine data reporting that often have shortcomings in terms of completeness and accuracy; this could explain the difference observed in prevalences. In contrast, the prevalence we observed in this study is similar to those reported by the WHO and the last Demographic and Health Survey (DHS) survey, which are 16.2% and 16% respectively[
18,
23]. Elsewhere in Africa, similar prevalences have been reported. A cross-sectional study of 500 women of childbearing age conducted in Nigeria reported a contraceptive prevalence of 18.8% in that area[
24]. An analysis of contraceptive use from DHS data of 17 sub-Saharan African countries (Angola, Benin, Burkina Faso, Burundi, Cameroon, Congo, Gambia, Ghana, Guinea, Côte d'Ivoire, Liberia, Mali, Niger, Nigeria, Senegal, Togo and Uganda) revealed that the overall prevalence of current contraceptive use among women of reproductive age was 17%, with Gambia and Uganda presenting the lowest (7%) and the highest (29%) prevalences, respectively[
25]. In addition, the results of this survey highlight important differences in MCM use.
According to the place of residence, MCM use is more frequent in the communes of Kelbo and Djibo, which are less rural than the other communes of the district. This finding corroborates the results of the last DHS, which showed that MCM use is more frequent in urban areas than in rural areas[
18]. Analysis of data from the 2005, 2010, and 2015 Rwanda DHS surveys which included 19,028 women aged 15-49 years showed that MCM use was less frequent among women residing in rural areas as compared to those residing in urban areas[
26].
Another important differential factor appears to be women's level of education. MCM use prevalence is very strongly associated with education level. According to the Burkina Faso 2010 DHS, almost 45% of women with a secondary level of education or higher use a MCM, compared to about 25% of those with a primary level of education and less than 12% of those with no education in Burkina Faso[
18]. In our survey, a similar pattern emerged but remained insignificant in multivariate analysis, probably due to a lack of power. Analysis of data from 17 African countries confirms that women were more likely to use a CMC if they had a secondary or higher level of education than if they had no education[
25].
In addition, the prevalence of MCM use varies by age group of the woman. The greatest users are between women aged between 20 and 30 years. This age range corresponds to the women´s physiological age of maximum fertility. Among women under 20 and those 31 and older, the prevalences of MCM use are relatively lower. The last DHS in Burkina Faso showed high MCM use among women aged 20 to 30[
18]. Results of a study conducted in Cameroon on a sample of 613 women aged 15-49 years to investigate the determinants of MCM use in Yaoundé showed that modern contraceptive use is less frequent among women over 30 years of age compared to those under 30 years of age[
27].
The situation in the commune of Diguel calls for an investigation of the factors influencing contraceptive use in this particular area of the DHD. None of the women were using a MCM in this commune, even though more than 64% of them were between the ages of 20 and 30 (period of maximum fertility) and all of the women in the locality were living in couples. This situation could be explained by several factors, including the rural nature of the area, the very low level of education of the girls[
13], and the low mobility of the women; at the time of the survey, the majority of women were born and have lived in the commune since birth. In addition to these factors, we should note that the women in this locality had a very low level of knowledge of family planning, probably related to the limited access to family planning services and the very low level of education in the area. In fact, the commune of Diguel is covered by only one health facility center, which does not have a midwife, and more than 70% of the women had not received any education. The health facility center has three agents to cover a large commune like Diguel, and this could influence the proper implementation of advanced family planning strategies.
Conclusion


The prevalence of modern contraceptive use in the DHD is low. Within the district, there is a significant disparity between communes. The commune of Djibo has the highest modern contraceptive use prevalence, probably due to the lesser influence of prejudices about family planning methods and greater access to information about them. Conversely, the commune of Diguel, a more rural area, has the lowest contraceptive prevalence in the district. Actions to improve contraceptive coverage in the DHD will require the implementation of district-wide strategies, but also targeted strategies to help close the gap in areas such as Diguel, Nassoumbou and Pobé-Mengao.
What is known about this topic
- Maternal mortality is a challenging public health problem especially in sub-Saharan Africa
- Modern contraceptive use is a cost-effective intervention to reduce maternal mortality but the contraceptive prevalence is still low in sub-Saharan Africa
- Data on contraceptive prevalence and the factors that influence it in Burkina Faso, especially in the Sahel region, are insufficient
What this study adds
- This study provides essential data to inform health policymakers to improve family planning services
- This study produced evidence that facilitated the implementation of a project called “Projet d'accès aux soins de santé sexuelle et reproductive dans le district sanitaire de Djibo ” by Médecins du Monde France
Competing interests


The authors declare that they have no competing interests.
Authors´ contributions


SO, AO and CO conceived and designed the study; SO, MS analysed the data; SO drafted the manuscript; SO, AO, CO and LO revised the manuscript. The final manuscript was read
and approved by all authors.
Acknowledgements


We are extremely grateful to all women who took part to the study, the regional director of health of Sahel region, the Djibo health district's chief medical officer, the midwives, nurses, and field workers, and the whole study team, including interviewers, supervisors, statisticians, students. We thank “Agence Française pour le Dévéloppement” who financed the study via “Médecin du Monde France”. The funders do not play a role in study design, collection, management, analysis and interpretation. They do not influence the writing of the report and the decision to submit.
Tables and figures


Table 1: General characteristics of women of childbearing age in Djibo Health District, Sahel Region, Burkina Faso, (N = 761)
Table 2: Factors associated with modern contraceptive methods use in the Djibo health district, Sahel region, Burkina Faso (Logistic regressions)
Figure 1: Contraceptive prevalence in the Djibo health district in 2015, Sahel region in Burkina Faso (N = 761)
References


- World Health Organization, World Bank, United Nations Population Fund, United Nations Children´s Fund (UNICEF). Trends in Maternal Mortality: 1990 to 2015 Estimates by WHO, UNICEF, UNFPA, World Bank Group and the United Nations Population Division [Internet]. Geneva: World Health Organization; 2015 [cited 2023 Apr 24]. 98 p. PubMed | Google Scholar
- Alkema L, Chou D, Hogan D, Zhang S, Moller AB, Gemmill A, Fat DM, Boerma T, Temmerman M, Mathers C, Say L. Global, regional, and national levels and trends in maternal mortality between 1990 and 2015, with scenario-based projections to 2030: a systematic analysis by the UN Maternal Mortality Estimation Inter-Agency Group. Lancet [Internet]. 2016 Jan [cited 2023 Apr 24];387(10017):462-74. https://doi.org/10.1016/S0140-6736(15)00838-7 PubMed | Google Scholar
- Jolivet RR, Moran AC, O´Connor M, Chou D, Bhardwaj N, Newby H, Requejo J, Schaaf M, Say L, Langer A. Ending preventable maternal mortality: phase II of a multi-step process to develop a monitoring framework, 2016-2030. BMC Pregnancy and Childbirth [Internet]. 2018 Jun 25 [cited 2023 Apr 24];18(1):258. https://doi.org/10.1186/s12884-018-1763-8 PubMed | Google Scholar
- World Health Organization. Strategies towards ending preventable maternal mortality (EPMM) [Internet]. Geneva: World Health Organization; 2015 [cited 2023 Apr 24]. 44 p. PubMed | Google Scholar
- Campbell OMR, Calvert C, Testa A, Strehlow M, Benova L, Keyes E, Donnay F, Macleod D, Gabrysch S, Rong L, Ronsmans C, Sadruddin S, Koblinsky M, Bailey P. The scale, scope, coverage, and capability of childbirth care. Lancet [Internet]. 2016 Oct [cited 2023 Apr 24];388(10056):2193-208. https://doi.org/10.1016/S0140-6736(16)31528-8 PubMed | Google Scholar
- Ceschia A, Horton R. Maternal health: time for a radical reappraisal. Lancet [Internet]. 2016 Oct [cited 2023 Apr 24];388(10056):2064-6. https://doi.org/10.1016/S0140-6736(16)31534-3 PubMed | Google Scholar
- Freedman LP. Implementation and aspiration gaps: whose view counts? Lancet [Internet]. 2016 Oct [cited 2023 Apr 24];388(10056):2068-9. Available from: https://doi.org/10.1016/S0140-6736(16)31530-6 PubMed | Google Scholar
- Graham W, Woodd S, Byass P, Filippi V, Gon G, Virgo S, Chou D, Hounton S, Lozano R, Pattinson R, Singh S.Diversity and divergence: the dynamic burden of poor maternal health . Lancet [Internet]. 2016 Oct [cited 2023 Apr 24];388(10056):2164-75. https://doi.org/10.1016/S0140-6736(16)31533-1 PubMed | Google Scholar
- Koblinsky M, Moyer CA, Calvert C, Campbell J, Campbell OMR, Feigl AB, Graham WJ, Hatt L, Hodgins S, Matthews Z, McDougall L, Moran AC, Nandakumar AK, Langer A. Quality maternity care for every woman, everywhere: a call to action. Lancet [Internet]. 2016 Nov [cited 2023 Apr 24];388(10057):2307-20. https://doi.org/10.1016/S0140-6736(16)31333-2 PubMed | Google Scholar
- Kruk ME, Kujawski S, Moyer CA, Adanu RM, Afsana K, Cohen J, Glassman A, Labrique A, Reddy KS, Yamey G. Next generation maternal health: external shocks and health-system innovations. Lancet [Internet]. 2016 Nov [cited 2023 Apr 24];388(10057):2296-306. Available from: https://doi.org/1016/S0140-6736(16)31395-2 PubMed | Google Scholar
- Bongaarts J, Cleland JC, Townsend J, Bertrand JT, Das Gupta M. Family Planning Programs for the 21st century: Rationale and Design [Internet]. Population Council; 2012 [cited 2023 Apr 27]. https://doi.org/10.31899/rh1016 Download the PDF at the link provided. PubMed | Google Scholar
- Darroch JE, Singh S, Weissman E. ADDING IT UP: The Costs and Benefits of Investing in Sexual and Reproductive Health 2014—Estimation Methodology [Internet]. New York: Guttmacher Institute; 2016. Appendix B, Estimating Sexual and Reproductive Health Program and Systems Costs; [cited 2023 Apr 24]. p.1-50. PubMed | Google Scholar
- Evina A, Ngoy K. L´utilisation des méthodes contraceptives en Afrique : de l´espacement à la limitation des naissances ? [Contraceptive use in Africa: from spacing to birth control?]. In: Gendreau F, editor. La transition démographique des pays du Sud [Internet]Éditions Estem; 2001 [cited 2023 Apr 28] p.253-68. French. PubMed | Google Scholar
- Apanga PA, Kumbeni MT, Ayamga EA, Ulanja MB, Akparibo R. Prevalence and factors associated with modern contraceptive use among women of reproductive age in 20 African countries: a large population-based study. BMJ Open [Internet]. 2020 Sep 1 [cited 2023 Apr 24];10(9):e041103. https://doi.org/10.1136/bmjopen-2020-041103 PubMed | Google Scholar
- Agyemang J, Newton S, Nkrumah I, Tsoka-Gwegweni JM, Cumber SN. Contraceptive use and associated factors among sexually active female adolescents in Atwima Kwanwoma District, Ashanti region-Ghana. Pan Afr Med J [Internet]. 2019 [cited 2023 Apr 24];32(182). https://doi.org/10.11604/pamj.2019.32.182.15344 PubMed | Google Scholar
- Sserwanja Q, Musaba MW, Mukunya D. Prevalence and factors associated with modern contraceptives utilization among female adolescents in Uganda. BMC women´s Health [Internet]. 2021 Dec [cited 2023 Apr 24];21(1):61. https://doi.org/10.1186/s12905-021-01206-7 PubMed | Google Scholar
- Chola M, Hlongwana K, Ginindza TG. Patterns, trends, and factors associated with contraceptive use among adolescent girls in Zambia (1996 to 2014): a multilevel analysis. BMC women´s Health [Internet]. 2020 Dec [cited 2023 Apr 24];20(1):185. https://doi.org/10.1186/s12905-020-01050-1 PubMed | Google Scholar
- Institut National de la Statistique et de la Démographie - INSD/Burkina Faso and ICF International. Burkina Faso Enquête Démographique et de Santé et à Indicateurs Multiples (EDSBF-MICS IV) 2010 [Burkina Faso Multiple Indicator Demographic and Health Survey (EDSBF-MICS IV) 2010] [Internet]. 2012 Apr [cited 2023 Apr 28]; Calverton, Maryland, USA: Institut National de la Statistique et de la Démographie - INSD/Burkina Faso and ICF International. French. PubMed | Google Scholar
- Hounton S, Barros AJD, Amouzou A, Shiferaw S, Maïga A, Akinyemi A, Friedman H, Koroma D. Patterns and trends of contraceptive use among sexually active adolescents in Burkina Faso, Ethiopia, and Nigeria: evidence from cross-sectional studies. Glob Health Action [Internet]. 2015 Dec [cited 2023 Apr 24];8(1):29737. https://doi.org/10.3402/gha.v8.29737 PubMed | Google Scholar
- Greenleaf AR, Gadiaga A, Guiella G, Turke S, Battle N, Ahmed S, Moreau C. Comparability of modern contraceptive use estimates between a face-to-face survey and a cellphone survey among women in Burkina Faso. PLoS ONE [Internet]. 2020 May 13 [cited 2023 Apr 24];15(5):e0231819. Available from: https://doi.org/10.1371/journal.pone.0231819 PubMed | Google Scholar
- Ministry of Health (Burkina Faso). Annuaire Statistique 2013 [Statistical Yearbook 2013] [Internet]. Ouagadougou, Burkina Faso: Ministry of Health (Burkina Faso), 2014 [cited 2023 Apr 28]. French. PubMed | Google Scholar
- WHO. World Health Organization vaccination coverage cluster surveys: reference manual [Internet]. Geneva: World Health Organization; 2018[cited 2023 Apr 24]. Report No.: WHO/IVB/18.09 PubMed | Google Scholar
- WHO. World Health Statistics 2013: A Wealth of Information On Global Public Health [Internet]. Geneva, Switzerland: World Health Organization; 2013 [cited 2023 Apr 24]. Document No.: WHO/HIS/HIS/13.1 PubMed | Google Scholar
- Orji EO, Onwudiegwu U. Prevalence and determinants of contraceptive practice in a defined Nigerian population. Journal of Obstetrics and Gynaecology [Internet]. 2002 Jan [cited 2023 Apr 24];22(5):540-3. https://doi.org/10.1080/0144361021000003126 PubMed | Google Scholar
- Ba DM, Ssentongo P, Agbese E, Kjerulff KH. Prevalence and predictors of contraceptive use among women of reproductive age in 17 sub-Saharan African countries: A large population-based study. Sexual & Reproductive Healthcare [Internet]. 2019 Oct [cited 2023 Apr 24] ;21:26-32. https://doi.org/10.1016/j.srhc.2019.06.002 PubMed | Google Scholar
- Muhoza, Ruhara. Closing the Poor-Rich Gap in Contraceptive use in Rwanda: Understanding the Underlying Mechanisms. International Perspectives on Sexual and Reproductive Health [Internet]. 2019 [cited 2023 Apr 24] ;45:13-23. https://doi.org/10.1363/45e7519 PubMed | Google Scholar
- Njotang PN, Yakum MN, Ajong AB, Essi MJ, Akoh EW, Mesumbe NE, Ako S, Mbu ER. Determinants of modern contraceptive practice in Yaoundé-Cameroon: a community based cross sectional study. BMC Res Notes [Internet]. 2017 Dec [cited 2023 Apr 24];10(1):219. https://doi.org/10.1186/s13104-017-2543-7 PubMed | Google Scholar