Analysis of national Lassa fever surveillance data, Sierra Leone, 2012 - 2018
Kassim Kamara1,2, Robert Nuoh Domo3, Delia Bandoh1,&, Stephen Atasige4, James Sylvester Squire1,2, Joseph Asamoah Frimpong1, Ernest Kenu1
1Ghana Field Epidemiology and Laboratory Training Program, 2Directorate of Health Security and Emergencies, Sierra Leone, Ministry of Health and Sanitation, 3Ghana Health Service, 4Field Epidemiology Training Program Sierra Leone
&Corresponding author
Delia Bandoh, Ghana Field Epidemiology and Laboratory Training Program. deliabandoh@gmail.com
Introduction:
Globally, about 500,000 Lassa fever (LF) cases occur annually with West Africa recording 300,000 infections and 5,000 deaths. LF is one of Sierra Leone's immediately reportable diseases under the integrated disease surveillance and response strategy. However, limited epidemiological analysis has been conducted. We described the demographic, and geographical distribution of reported LF cases and determined trend, incidence, and case-fatality rates of LF in Sierra Leone.
Methods:
We analyzed secondary data from LF sentinel site database for Sierra Leone from 2012 - 2018. We reviewed, cleaned, edited, the data using Microsoft Excel 2016. We calculated proportions, rates, and ratios using the number of deaths, positive cases, suspected cases, and the population at risk with a constant as a multiplier. We mapped LF incidence and presented data using tables, graphs, and maps.
Results:
Of 2,879 suspected cases reported, 14.2% (408/2879) were confirmed for LF. Median age of confirmed cases was 21 years (0-75 years). Females formed 59% (240/408) of the confirmed LF cases. Kenema district recorded the highest incidence ( 21/100,000 population) in 2012 and (24/100,000 population) in 2013. LF incidence was highest in 2013 with 26/100,000 population. The overall CFR was 38.8% (157/408). The trend of cases dropped from 2012 - 2018.
Conclusion:
Incidence of LF in Sierra Leone decreased with cases occurring all year round. Females and those aged 10-39 years were the most affected. The LF program and the Ministry of Health and Sanitation should conduct community sensitizations on LF to promote early health-seeking behavior in high incidence districts.
Introduction

Lassa fever (LF) is an acute viral hemorrhagic fever disease. It was first reported in Nigeria in 1969 and is caused by the LF virus which is an enveloped ribonucleic acid virus belonging to the Arenaviridae family [1]. The incubation period of LF ranges from 5-21 days, with fever and other non-specific symptoms such as headache, sore throat, myalgia, and gastrointestinal symptoms being the most common manifestations. Bleeding occurs less frequently [2]. This non-specific clinical presentation makes LF extremely difficult to identify on clinical grounds alone, particularly during the early phase of the disease [3]. Globally, an estimated 300,000 - 500,000 cases occur annually [4]. Unlike most viral hemorrhagic fevers, which are recognized only when outbreaks occur, LF is endemic in West Africa, with an estimated 300,000 cases and 5,000 deaths reported yearly [5]. These estimates, however, under-represents the true number of cases since some patients do not report to the health facilities for treatment, as such, they are not captured during routine surveillance.
In Sierra Leone, about 10% - 16% of yearly hospital admissions are due to LF cases [
6]. This reflects the impact of the disease in the country. LF is one of Sierra Leone´s immediately reportable diseases under the integrated disease surveillance and response (IDSR) strategy [
7]. Although Sierra Leone has been implementing case-based disease surveillance for LF, limited epidemiological analysis has been conducted. Regular LF data analysis is a critical part of disease surveillance to monitor the disease and evaluate prevention and control efforts. We described the demographic, and geographical distribution of reported LF cases and determined the trend, incidence, and case-fatality rates of LF in Sierra Leone.
Methods


Study design
We conducted a descriptive study using secondary data from LF surveillance in Sierra Leone for the period 2012 to 2018.
Study site and population
Sierra Leone is a small West African country with a population of 7,874,335 inhabitants and a growth rate of 3.2% [
8]. The country is divided into four regions namely; North, South, East, and West. Administratively, the country is divided into sixteen (16) districts distributed in the four regions in the country (
Figure 1). The eastern region lies along the LF belt and has a population of 1,642,370, representing 23.2% of the country´s population [
8]. The country´s system is tiered with over 1,307 public and private health facilities. The population in this study includes records of all categories of people such as community members, healthcare personnel, children, and adults who had LF from 2012 - 2018.
Description of surveillance system and data collection
Lassa fever surveillance in Sierra Leone is conducted through a sentinel surveillance system, which is both active and passive. Healthcare workers are required to immediately report LF cases to the districts and include those cases in the weekly Integrated Disease Surveillance and Response reports submitted to the districts weekly. The data capture and management system is situated at the Kenema government hospital in Kenema district located in the Eastern region. All laboratory specimens of suspected LF cases in Sierra Leone are sent to the LF laboratory for testing and data is entered into LF program database.
LF confirmed cases from the country are also referred to the LF treatment center in Kenema. Surveillance data on LF is recorded in a paper-based forms which are entered and stored in Excel format.
IDSR Lassa fever case Definitions (suspected, confirmed), and positivity rate
A suspected case was defined as an acute onset of fever of less than 3 weeks duration in a severely ill patient AND any 2 of the following; haemorrhagic or purpuric rash; epistaxis (nose bleed); haematemesis (blood in vomit); haemoptysis (blood in sputum); blood in stool; other haemorrhagic symptoms and no known predisposing factors for haemorrhagic manifestations, and a confirmed cases was defined as a suspected case with laboratory confirmation or epidemiologic link to confirmed cases or outbreak. The positivity rate was defined as the proportion of confirmed cases per total suspected cases multiplied by 100.
Data collection
We obtained data for this study from the LF sentinel surveillance database stored in Microsoft (MS) excel format at the Kenema government hospital. We extracted data on demographics, reporting district, date of onset of symptoms, laboratory results, and outcome of positive cases.
Data analysis
We computed median and range for continuous variables and frequencies and proportions for categorical variables. We calculated the incidence rate per 100,000 population and mapped the incidence by districts. We calculated the case fatality rate as the proportion of death among confirmed cases of LF. Cases with missing variables of interest were excluded from the analysis. The data was analyzed using MS excel 2016 and QGIS software version 3.12.2 and presented using tables, graphs, maps, and charts.
Ethical consideration
Approval for the analysis and use of LF surveillance data was obtained from the Ministry of Health and Sanitation (MoHS), and the Tulane university LF sentinel site in Kenema. We maintained the confidentiality of patient information by ensuring that personal identifiers were excluded from the dataset before the analysis. The result of the analysis was only shared with authorized stakeholders and organizations.
Results


A total of 2,879 suspected LF cases were reported in Sierra Leone for the period under review. Of these, 14.2% (408/2,879) were confirmed positive for LF. The median age of the confirmed cases was 21 years (range 0 - 75 years). Most, 30.9% (242/408) were between the age group 20 - 29 years. More than half, 58.8% (240/408) were females. The majority, 72% (292/408) of the confirmed LF cases were reported from Kenema district, followed by Bo district, 15% (61/408). Port Loko, Kono, Kambia, and Western Area districts reported zero confirmed cases for the period under review Table 1. The lowest proportion of confirmed LF cases was recorded in 2018 with 4.4% (18/408).
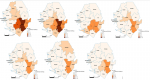
The incidences of LF in 2012 and 2013 were higher than the other years, with each year recording about 27 and 26 cases per 1,000,000 population respectively. The lowest incidence of LF occurred in 2018, with 2 cases per 1,000,000 population. Kenema district reported the highest incidence of LF in 2012 and 2013 at 21 and 25 cases per 100,000 population respectively. This was followed by Bo, 10 and 4 cases per 100,000 population in 2012 and 2013, and Kenema, 2 and 3 cases per 100, 000 population in 2012 and 2013 respectively
Figure 1.
The trend of confirmed LF cases showed high peaks in 2012 - 2013, with the highest peak in July 2012. The LF cases also showed more peaks during the rainy season months in Sierra Leone, that is, from May to October throughout the seven years. There were however no cases reported from June to November in 2015
Figure 2.
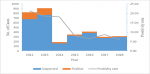
Of the 408 confirmed LF cases, 157 died, giving a case fatality rate (CFR) of 38.8% (157/408). Generally, there was a decrease in the positivity rate of LF, although it increased in 2017. The highest positivity rate was recorded in 2012, and the lowest in 2016
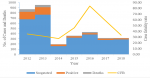
Figure 3. There was an increase in suspected and positive cases in 2012 and 2013, however, the case fatality rate was low in those years, and further declined in 2014. The case fatality, however, started increasing in 2015 and peaked in 2016 , and declined in 2017
Figure 4.
Discussion


From the analysis of LF data in Sierra Leone, this study found the age group 20 - 29 years to be the most affected, followed by those aged 0 - 9 years. This was probably due to the fact that this age group involves people that are active and more exposed to some of the risk factors of the disease including farming, hunting, and domestic activities. Several studies have reported similar findings that LF mostly affects young adults [9-11]. A finding by the current data that the majority of the cases were female could be as a result of females being more exposed to the disease through contact with rats and their excreta during the processing of crops, grains, and other domestic activities. The finding that females are mostly affected by LF is similar to the analysis conducted in Sierra Leone and Liberia were females were reported as the most affected with LF [ 12]. The high proportion of LF cases among those aged 0-9 years could be attributed to the high proportion of cases among females since children of this age are usually close to their mothers and may be exposed to LF infections. However, other studies conducted in Nigeria found that males were the most affected [10, 11]. Our findings are consistent with a study conducted in Sierra Leone with high proportion of cases among children ten years and bellows [13]. However, another study in Nigeria reported that those aged 15 - 34 years were the most affected followed by those aged 35 - 54 years [14]. The variation in the results could be due to the study setting, time, and population.
The distribution of LF confirmed cases were concentrated in the Southern and Eastern Districts of the country which is expected since the incidence of LF in the northern region is very low. Four districts including Kambia, Kono, Western Area, and Port Loko districts did not record a positive case for the period under review. As is the case with other studies, the South and East districts are the most affected. For example, the South-East and South-South in Nigeria are the most affected regions according to a similar analysis conducted in 2017 [
10]. This is because the South-East regions in Sierra Leone and Liberia are endemic with LF
The decreasing trend of LF in general and the overall low case fatality rate in the current study is contrary to other data on LF trends in Nigeria and Liberia where increasing trends of LF were reported for particular study periods [
4,
15]. The overall, gradual decrease in confirmed cases of the disease from 2012 - 2018 could be attributed to underreporting, improved prevention, and control efforts of the disease in the country. For example, the Ebola outbreak interrupted surveillance and response activities the response for LF. The high CFR positivity rate of LF in the present study is consistent with a study in Nigeria who reported a higher CFR when compared to the current study [
4]. The high CFR of LF in the current study suggests that reporting within 24 hours and effective management of LF patients in the treatment facility in Sierra Leone should be improved. With the highest LF case fatality rate recorded in 2016, factors such as delay of LF patients in seeking medical care among other factors could have contributed to this finding [
16]. Also, fear by patients and mistrust of communities on the healthcare system following the Ebola outbreak could have contributed to the high CFR in 2016 [
17].
Although our study observed a decrease in positivity rate of LF over time, a study in Nigeria reported an increase in positivity rate [
4]. The decrease in the positivity rate of LF in Sierra Leone over time could be attributed to the increased community awareness on LF prevention, the provision and use of personal protective equipment, and decrease in incidence of the disease [
4,
18,
19].
The lowest proportion of suspected LF recorded in 2014 - 2015 in the present study could be attributed to the Ebola outbreak which occurred during that period [
20]. The health sector, during that time, was focused mainly on interventions to contain the outbreak, and surveillance for other priority diseases was interrupted. This could have contributed to the low incidence for that period.
The finding that approximately half of the LF cases were reported during the rainy season is inconsistent with other findings which suggests that the incidence of LF is high during the dry season. This is contrary to another study conducted in Nigeria and Liberia who found a higher incidence of LF during the dry season [
12]. The finding from our study suggests that LF could as well be high during the rainy season and can occur all year round.
This study has some limitations. The true estimates of LF in Sierra Leone for the study period has not been determine due some cases that were excluded from the analysis due to missing variables and cases that did not seek care at the health facility. The use of projected population to estimate the incidence could have affected its estimation.
Conclusion


There is decrease in the incidence of LF in Sierra Leone. Cases of LF occurs all year round. Females and the age group -20 - 29, followed by those aged 0 -9 years were the most affected. Kenema district recorded the highest LF incidence throughout the seven years period. The overall positivity rate of LF was low and an overall high CFR.
We are therefore recommending that the LF program and the Directorate of health security and emergencies (DHSE) conduct refresher training for health facility staff and community health workers (CHWS) on early case detection and reporting of LF giving priority to districts with low or zero incidence. The above institutions should also embark on intensive and monthly community sensitization on LF clinical presentation to promote early health-seeking behavior with a focus on high incidence districts. The disease surveillance officers to immediately investigate and timely report all suspected cases of LF and in all districts. Disease surveillance officers should also intensify Community Based Surveillance and active case search to help detect unreported cases.
What is known about this topic
- LF is highly fatal disease and is endemic is West Africa
- Risk factors for LF infection include exposure to urine or faeces of infected Mastomys rats, direct contact with blood, urine, faeces or other bodily secretions of a person infected with LF
What this study adds
- This study adds the estimation of the incidence of LF in Sierra Leone
- It also adds information on the trend of LF in Sierra Leone for seven years.
Competing interests


The authors declare no competing interests.
Authors´ contributions


KK and RND developed the protocol. KK, RND, and SA analyzed and interpreted the data. KK, DB, and JSS reviewed several drafts of the manuscript and made significant contributions throughout the writing process.
Acknowledgements


Our thanks and appreciation to the Ministry of Health and Sanitation, Ghana Field Epidemiology Training Program, Sierra Leone Field Epidemiology Training Program, the Kenema district health management team, and the LF program at Kenema district. Special thanks to the West African Health Organization for providing the opportunity to pursue this course and completion of this competency.
Tables and figures


Table 1: Socio-demographic characteristics of confirmed Lassa fever cases, Sierra Leone, 20122018
Figure 1: Incidence of Lassa fever per 100,000 population by district, Sierra Leone, 2012 - 2018
Figure 2: Distribution of confirmed Lassa fever cases by month, Sierra Leone, 2012 - 2018
Figure 3: Cases and positivity rate of Lassa fever, Sierra Leone, 2012 - 2018
Figure 4: Lassa fever cases, deaths and case fatality rate, Sierra Leone, 2012 - 2018
References


- Lo Iacono G, Cunningham AA, Fichet-Calvet E, Garry RF, Grant DS, Khan SH, Leach M, Moses LM, Schieffelin JS, Shaffer JG, Webb CT, Wood JL. Using modelling to disentangle the relative contributions of zoonotic and anthroponotic transmission: the case of lassa fever. PLoS Negl Trop Dis[Internet]. 2015 Jan 8[cited 2023 Feb 17];9(1):e3398. https://doi.org/10.1371/journal.pntd.0003398 PubMed | Google Scholar
- WHO. Introduction to Lassa Fever: Managing infectious hazards[Internet]. WHO; 2018. p.1-22 [cited 2023 Feb 17].
- Khan SH, Goba A, Chu M, Roth C, Healing T, Marx A, Fair J, Guttieri MC, Ferro P, Imes T, Monagin C, Garry RF, Bausch DG. New opportunities for field research on the pathogenesis and treatment of Lassa fever. Antiviral Research[Internet]. 2008 Apr[cited 2023 Feb 17]; 78(1):103-15. https://doi.org/10.1016/j.antiviral.2007.11.003 Google Scholar
- Olayiwola J, Bakarey A. Epidemiological Trends of Lassa Fever Outbreaks and Insights for Future Control in Nigeria. IJTDH[Internet]. 2017 Jul 28[cited 2023 Feb 17]; 24(4):1-14. http://dx.doi.org/10.9734/IJTDH/2017/32823 Google Scholar
- Usuwa IS, Akpa CO, Umeokonkwo CD, Umoke M, Oguanuo CS, Olorukooba AA, Bamgboye E, Balogun MS. Knowledge and risk perception towards Lassa fever infection among residents of affected communities in Ebonyi State, Nigeria: implications for risk communication. BMC Public Health[Internet]. 2020 Feb 12[cited 2023 Feb 17]; 20(1):217. https://doi.org/10.1186/s12889-020-8299-3 PubMed | Google Scholar
- National Center for Emerging and Zoonotic Infectious Diseases, Division of High-Consequence Pathogens and Pathology (DHCPP). CDC Fact Sheet: Lassa Fever [Internet]. CDC; 2014[cited 2023 Mar 23].
- Ministry of Health and Sanitation Sierra Leone. Technical Guidelines for Integrated Disease Surveillance and Response. Freetown, Sierra Leone: MoH; 2015. p. 310 -315. Google Scholar
- Beresford Weekes S, Silleh Bah. Sierra Leone 2015 Population and Housing Census Thematic Report on Population Structure and Population Distribution[Internet]. Sierra Leone: Sierra Leone Statistics (SSL); 2017 Oct[cited 2023 Mar 23]. p. 1-43. Report No: 1.
- Bausch DG, Demby AH, Coulibaly M, Kanu J, Goba A, Bah A, Condé N, Wurtzel HL, Cavallaro KF, Lloyd E, Baldet FB, Cissé SD, Fofona D, Savané IK, Tolno RT, Mahy B, Wagoner KD, Ksiazek TG, Peters CJ, Rollin PE. Lassa Fever in Guinea: I. Epidemiology of Human Disease and Clinical Observations. Vector-Borne and Zoonotic Diseases[Internet]. 2001 Dec[cited 2023 Feb 17]; 1(4):269-81. https://doi.org/10.1089/15303660160025903 Google Scholar
- Ilori EA, Furuse Y, Ipadeola OB, Dan-Nwafor CC, Abubakar A, Womi-Eteng OE, Ogbaini-Emovon E, Okogbenin S, Unigwe U, Ogah E, Ayodeji O, Abejegah C, Liasu AA, Musa EO, Woldetsadik SF, Lasuba CLP, Alemu W, Ihekweazu C; Nigeria Lassa Fever National Response Team. Epidemiologic and Clinical Features of Lassa Fever Outbreak in Nigeria, January 1-May 6, 2018. Emerg Infect Dis[Internet]. 2019 Jun[cited 2023 Feb 17];25(6):1066-1074. https://doi.org/10.3201/eid2506.181035 PubMed | Google Scholar
- Ekechi HU, Ibeneme C, Ogunniyi B, Awosanya E, Gbadebo B, Usman A, Balogun MS, Ameh C, Okeke L, Dan-Nwafor C, Ihekweazu C. Factors associated with a confirmed Lassa fever outbreak in Eguare community of Esan West, Edo State, Nigeria: January-March, 2019. Journal of Interventional Epidemiology and Public Health[Internet]. 2020 Jan 9[cited 2023 Feb 17];3(1):1. https://doi.org/10.37432/JIEPH.2020.3.1.21 PubMed | Google Scholar
- Olugasa B, Dogba J. Mapping of Lassa fever cases in post-conflict Liberia, 2008-2012: A descriptive and categorical analysis of age, gender and seasonal pattern. Ann Afr Med[Internet]. 2015 Feb 19[cited 2023 Feb 17]; 14(2):120-22. https://doi.org/10.4103/1596-3519.149890
- Samuels RJ, Moon TD, Starnes JR, Alhasan F, Gbakie M, Goba A, Koroma V, Momoh M, Sandi JD, Garry RF, Engel EJ, Shaffer JG, Schieffelin JS, Grant DS. Lassa Fever among Children in Eastern Province, Sierra Leone: A 7-year Retrospective Analysis (2012-2018). Am J Trop Med Hyg[Internet]. 2020 Nov 23[cited 2023 Feb 17]; 104(2):585-592. https://doi.org/10.4269/ajtmh.20-0773 PubMed | Google Scholar
- Buba MI, Dalhat MM, Nguku PM, Waziri N, Mohammad JO, Bomoi IM, Onyiah AP, Onwujei J, Balogun MS, Bashorun AT, Nsubuga P, Nasidi A. Mortality Among Confirmed Lassa Fever cases During the 2015-2016 Outbreak in Nigeria. Am J Public Health[Internet]. 2018 Feb 1[cited 2023 Feb 17]; 108(2):262-4. https://doi.org/10.2105/AJPH.2017.304186 PubMed | Google Scholar
- National Public Health Institute of Liberia. Lassa Fever outbreak in Liberia: Incident management situation report. 2020 Jan 07. 11 p. (Vol: 17). Supported by the World Health Organization.
- Abdulkarim MA, Babale SM, Umeokonkwo CD, Bamgboye EA, Bashorun AT, Usman AA, Balogun MS. Epidemiology of Lassa Fever and Factors Associated with Deaths, Bauchi State, Nigeria, 2015-2018. Emerg Infect Dis[Internet]. 2020 Mar 2[cited 2023 Feb 17]; 26(4):799-801. https://doi.org/10.3201/eid2604.190678 PubMed | Google Scholar
- Yamanis T, Nolan E, Shepler S. Fears and Misperceptions of the Ebola Response System during the 2014-2015 Outbreak in Sierra Leone. Kasper M, editor. PLoS Negl Trop Dis[Internet]. 2016 Oct 18[cited 2023 Feb 17]; 10(10):e0005077. https://doi.org/10.1371/journal.pntd.0005077 PubMed | Google Scholar
- Shaffer J, Schieffelin J, Momoh M, Goba A, Kanneh L, Alhasan F, Gbakie M, Engel E, Bond N, Hartnett J, Nelson D, Bush D, Boisen M, Heinrich M, Rowland M, Branco L, Samuels R, Garry R, Grant D, the Viral Hemorrhagic Fever Consortium. Space-Time Trends in Lassa Fever in Sierra Leone by ELISA Serostatus, 2012-2019. Microorganisms[Internet]. 2021 Mar 12[cited 2023 Feb 17]; 9(3):586. https://doi.org/10.3390/microorganisms9030586 Google Scholar
- Koch MR, Kanneh L, Wise PH, Kurina LM, Alhasan F, Garry RF, Schieffelin JS, Shaffer JG, Grant DS. Health seeking behavior after the 2013-16 Ebola epidemic: Lassa fever as a metric of persistent changes in Kenema District, Sierra Leone. Barker CM, editor. PLoS Negl Trop Dis[Internet]. 2021 Jul 14[cited 2023 Feb 17]; 15(7):e0009576.https://doi.org/10.1371/journal.pntd.0009576 PubMed | Google Scholar
- Marston BJ, Dokubo EK, van Steelandt A, Martel L, Williams D, Hersey S, Jambai A, Keita S, Nyenswah TG, Redd JT. Ebola Response Impact on Public Health Programs, West Africa, 2014-2017. Emerg Infect Dis.[Internet] 2017 Dec[cited 2023 Feb 17]; 23(13):S25-32. https://doi.org/10.3201/eid2313.170727 PubMed | Google Scholar