A three year review of Tuberculosis surveillance data in Montserrado County, Liberia, 2016-2018
Alberta Berlynda Corvah1, Himiede Wilson Sesay2, Delia Akosua Bando1, Patrick Konwloh3, Benedict Calys-Tagoe4, Ernest Kenu1
1Ghana Field Epidemiology Training and Laboratory Training Program, School of Public Health, College of Health Sciences, University of Ghana, Legon, Accra, 2Liberia Field Epidemiology Training Program, Monrovia, Liberia, 3National Leprosy and Tuberculosis Control Program of Liberia, Ministry of Health, Monrovia, Liberia, 4University of Ghana Medical School Korle bu Teaching Hospital, Accra, Ghana
&Corresponding author
Delia Akosua Bandoh, Ghana Field Epidemiology and Laboratory Training Program, School of Public Health. Email: deliabandoh@gmail.com
Introduction:
Tuberculosis (TB) is a public health problem. Liberia's annual mortality rate remains high with estimated incidence 14,000 cases (308 per 100,000). The study's objective was to analyze the distribution of TB cases by person place and time, estimate the prevalence, case detection rate and outcome of all form of TB cases in Montserrado from 2016-2018.
Methods:
We conducted a descriptive analysis where we reviewed and analyzed reports for all forms of TB notified by districts through the DHIS2 in Montserrado County from 2016 to 2018. We also extracted data from the data sources and analyzed the data to obtained measure of disease occurrence and disease frequency using Microsoft Excel, 2013.
Results:
A total of 18141 cases of all forms of TB were notified in Montserrado County from 2016 to 2018; out of which 5271 (29%) cases were sputum smear positive. Of cases notified, 58% (5081/8716) were males and 20%1026 were among 25-34 year age group. TB cases were 36% in 2017 and 29% in 2018. In 2017, the prevalence was 140/100000 population. Prevalence among the male population was 461/100,000 population and female accounted for 306/100,000 population. Up to 60% of TB cases were notified by two districts (Bushrod & Central Monrovia). Cases were detected at the rate of 46% in 2017 and 43% in 2018 with Bushrod district detection rate of 151%. On average, 34% of patients on treatment were cured and 15% defaulted showing treatment success rate at 24%.
Conclusion:
Tuberculosis remains a problem in Liberia and males in productive age group accounted for most cases in Bushrod and Central Monrovia districts. The prevalence of TB is high. Though more cases were detected in Bushrod district, the case detection rate showed a decreasing trend in 2018. Patients were cured of TB but data also showed defaulted record and a treatment success rate far lower than the national target 85%. We recommend that Ministry of health through National TB control should intensify sensitization and TB health education to improve the case detection and treatment success rates.
Introduction

Tuberculosis (TB) is caused by bacteria, Mycobacterium tuberculosis that affects the lungs. Tuberculosis can be cured and prevented but spread among humans through droplets in the air [1, 2]. Tuberculosis (TB) which has been existing for many years is a public health problem worldwide [3]. The TB pandemic has been progressing worldwide due to HIV co-infection, poor health care services and emergence of multidrug resistant tuberculosis [4]. In 2015, global estimates showed 10.4 million incident cases of TB including 1.4 million deaths (including 400,000 deaths among people co-infected with HIV) of which, about 55% had comorbidity involving Human immuno-deficiency Virus (HIV) [5]. The two continents that accounted for the highest number of TB cases and 75% of the deaths attributable to TB globally are South East Asia (29%) and Africa (26%) [6]. India is among the countries with the highest TB burden, accounting for 1.98 million cases [7]. Tuberculosis prevalence results from a 2013 survey conducted in Ghana revealed that there were 165 incident cases per 100,000 people which showed that there were more undetected cases than previously estimated [8].
In 2016, Liberia reported a total of 7180 TB cases. Of these, 7105 (98.9%) were the new and relapse TB cases; of which 63% were bacteriologically confirmed with high incidence among the reproductive age group of 15-49 years [
9]. Treatment and retreatment success rates were below 80 %. In the last quarter of 2015, after GeneXpert testing was introduced in Liberia, a total of 92 patients were diagnosed with TB and enrolled into treatment [
9].
Liberia is among the high TB burden countries. According to WHO GTB report (2017), TB incidence in Liberia increased over the years from 242 in 2002 to 308 per 100,000 populations in 2016. The National Leprosy and Tuberculosis Control program (NLTCP) advocates for resources in favor of people with TB to contribute to reducing the potential risk of poor treatment outcomes that lead to development of drug-resistant TB. Montserrado county which hosts Liberia´s capital consists of clusters with a high population density where TB is easily transmissible. Data shows that in 2014, Montserrado accounted for the highest prevalence of TB cases in Liberia [
9].
Given the multi-sectoral influences on the TB epidemic and the multi-sectoral actions needed to end it, WHO developed a TB-SDG monitoring framework in 2017. There have been some interventions initiated to deal with more TB infections. In order to achieve the targets and milestones of the” End TB”, WHO launched the stop TB strategy. One thematic pillar of this strategy is to intensify research and innovation with the objective of identifying limited factors. This research in particular intended to analyze the distribution of TB cases by person, place and time, estimate the prevalence, case detection rate and treatment outcomes of TB cases detected in Montserrado County. Findings from this research will provide decision makers clues on gaps identified and which strategies that work best for the program.
Methods


Setting
The data analysis was conducted in Montserrado County which is one of the 15 counties in Liberia. It hosts the capital city which is Monrovia and is located Northwest of Liberia. Montserrado is the smallest county in size at 1,909 square kilometers (737 sq mi), but has the largest population estimated at 1,293,349 or approximately 33% of Liberia´s total population. Montserrado County has seven (7) health districts and 351 health facilities including 23 tuberculosis treatment centers.
Study Design and Data source
A descriptive study done to review all Tuberculosis cases that were reported in Montserrado County from January 2016 to December 2018 as well describe the data. The study included all registered and reported TB cases from 2016-2018. The data is generated at the health facility where the hard copies are compiled on a monthly basis and reported to the district. The data manager at the district level uploads the recorded data to the HMIS which is linked to the DHIS2 platform using the monthly reporting form template. The DHIS2 is an open source software platform for reporting, analysis and dissemination of data. This data is accessed at both the County and national level by logging into the platform. Every level of the system has a TB focal person/coordinator and data manager responsible for reporting TB cases.
Case definitions used by the TB surveillance system
Case definitions were adopted form Liberia IDSR used by the NPHIL and the Ministry of Health and social welfare, Liberia [
10,
11].
Suspected
Any person with a cough for 3 weeks or more.
Confirmed
Smear-positive pulmonary TB: a) a suspected patient with at least 2 sputum specimens positive for acid-fastbacilli (AFB), or
b) one sputum specimen positive for AFB by microscopy and radiographic abnormalities consistent with active pulmonary TB as determined by the treating medical officer, or
c) one positive sputum smear by microscopy and one sputum specimen positive on culture for AFB.
Pulmonary tuberculosis (PTB)
Refers to any bacteriologically confirmed or clinically diagnosed case of TB involving the lung parenchyma or the tracheobronchial tree.
Extra-pulmonary tuberculosis (EPTB)
Refers to any bacteriologically confirmed or clinically diagnosed case of TB involving organs other than the lungs, e.g. pleura, lymph nodes, abdomen, genitourinary tract, skin, joints and bones, meninges.
Treatment success rate
The proportion of new smear-positive TB cases registered under Direct Observe Therapy (DOTS) in a given year that successfully completed treatment, whether with bacteriologic evidence of success (“cured”) or without (“treatment completed”)
Cured
Patient initially bacteriologically confirmed (microscopy, culture or molecular test) who completed treatment AND shows no signs of continued active disease AND has at least 2 negative smears or cultures: one at 4-5 months and the other at the end of treatment AND does not meet the definition of failure
Completed
Patient who completed treatment AND has no signs of continued active disease AND does not meet the bacteriological criteria for cure.
Relapsed
TB patient who was declared cured or treatment completed by a physician, but who reports back to the health service and is now found to be sputum smear positive.
Default
When a TB patient interrupts treatment for two (2) months or more.
Data Collection procedure
We explored the HMIS platform where the monthly tuberculosis data is kept. We reviewed and extracted variables of interest and exported them into an excel spread sheet for analysis purpose. The data was also collected from the hard and electronic copies of the quarterly TB reporting forms. We compared the data reported through the TB quarterly reporting form/ledgers, laboratory ledgers, with electronic copies from the Health Management Information System (HMIS) platform to correct discrepancies where necessary.
Data Variable and Extraction
Variables extracted included specific variables needed to achieve the objectives of the study: socio-demographic of TB cases so as to analyze by person, place and time (age, sex, year of reporting, district of residence), treatment outcome (completed, cured, death). Patients are considered cured if they completed treatment and tested negative for TB but are considered “completed” if they completed treatment time without further test for TB. Other variables included: defaults (incomplete treatment) and laboratory outcomes (positive and negative) which was used to calculate the prevalence (the proportion of positive cases per the population). These are variables that were included on the HMIS form for TB. The TB reporting form is built in the DHIS2 platform with the listed variables. Therefore, we accessed the platform and extracted the data filtering these specific variables, downloading the contents/data concerning these variables and exporting the data to an excel spread sheet.
Data management and analysis
The three-year data was cross-checked, cleaned and entered into Microsoft excel, 2013 for processing and analysis. For the measures of disease occurrence, we calculated frequencies, rates and proportions for the some of the variables including sex, districts and age (which was categorized into groups). To calculate the sex proportion, all positive female/male cases were expressed over the total positive cases and multiplied by hundred. We calculated prevalence by 100,000 populations to estimate the burden and time trend of the disease in the population. The total cases that were positive for TB were expressed as a proportion of the total population and multiplied by 100,000 populations. We determined the rate at which cases were detected by dividing the number of cases notified by the number of cases estimated for each year under review and stated it as a percentage. We calculated proportions of the different treatment outcomes for the patients to show the percentage of those patients that were considered cured, those who completed treatment and those who died. We divided the number of cases for each treatment outcome by all the positive TB cases undergoing treatment and multiplied by 100%. The treatment success rate was determined by dividing the proportion of cases that had completed treatment and cases cured by the total number of registered cases. The results are presented in tables and graphs.
Ethical Consideration
Prior to the data collection, we obtained permission from the Liberia Ministry of Health, National Leprosy and Tuberculosis Control program (NLTCP). The Ghana Field Epidemiology and Laboratory Training Program (GFELTP), School of Public health, University of Ghana, wrote an introductory letter to the NLTCP, requesting for the data to be used in this study. The NLTCP Program Manager, endorsed the letter and granted us permission to conduct the study. To ensure confidentiality of the patient data, names were eliminated throughout the data analysis. We developed another database where a unique identifier was assigned to each case in the line-list and linked the newly created database with the original database in case clarity was needed.
Results


A total of 18,141 cases of TB were detected over the three-year period (2016-2018). Out of this number, 5,271 were diagnosed sputum smear positive. TB cases were 29% (1541) in 2016, 36% (1893) in 2017 and 29% (1837) in 2018. Of those who were diagnosed sputum smear positive, 59% (3125) were males and 41%(2146) were females. The 25-34 years age group accounted for the highest number of cases during the three-year period 20% (1026). The highest number of TB cases were reported from Bushrod District 32% (1677) (Table 1). The overall treatment success rate for the three-year period was 24%.
The prevalence of TB positive cases reported by the seven health districts in Montserrado County, was 460/100,000 population among males and 306/100,000 population for females. The yearly trend shows a prevalence of 117 per 100,000 population in 2016, 140 per 100,000 population in 2017 and 133 per 100,000 population in 2018(
Figure 1).
The overall case detection rate for Mondserrado County is 124% (5271). Bushrod which is one of the seven health districts in Montserrado county case detection rate was 151% (1677) while Todee district detection rate was the lowest 12% (14). In 2016, 39% (1541) cases were detected, increasing to 46% (1893) detected cases in 2017, and decreased to 43% (1837) in 2018(
Figure 2).
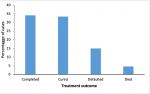
The success of the TB control program depends on the treatment outcomes of patients. The total of 18,141 cases of TB were reported between 2016-2018. Within the three-year period, 6,200 (34%) of the reported patients were diagnosed with TB, enrolled into treatment and completed it, while 6,068 (33%) of them were declared cured of TB. We observed that 4,200 (23%) of reported patients defaulted (
Figure 3).
Discussion


To achieve the objectives, all notified and registered TB cases from 2016- 2019 in Montserrado County were analyzed. The findings from this study showed that throughout the three-year period, males had the highest proportions with TB than females. This could be because men are sometimes more exposed to some predisposed factors such as alcohol and smoking. Study shows that generally, men smoke more than women [12]. The results in this study were similar to findings from a study in Nigeria in which the prevalence rate observed was high among males. The study indicated that men experience more exposure to the world at large as compared with women (particularly in rural areas), including social relations with others and higher risk of being exposed to TB infected individuals, thus getting the possibility of becoming infected with TB [1]. This finding is inconsistent with a study which proved that TB sputum smear positive cases were more among women than men, providing evidence that men may not visit the health facility for care most often in many situations. (Horton, Macpherson, Houben, White, & Corbett, 2016) [13].
In Montserrado, Liberia, the proportion of Tuberculosis seems high among the age group 25-34 followed by 35 to 44 years. Anecdotally, this could probably be due to the engagement of this youthful population in laborer jobs as well as their daily activities including productivity, socio-economic status, job descriptions that may disposed them to TB. A study conducted in Kenya indicated that TB mainly affected young adults in their most productive ages of life and the age-group 15-44 year continues to bear the highest burden (Nyamogoba & Mbuthia, 2018) [
14]. Findings of this study are also similar with the perception that TB is an adults´ disease and the male gender carries the heavier burden. (Horton et al., 2016)[
13].
Tuberculosis prevalence was highest in 2017 as compared to the other years in the study. The reason for this increase in prevalence is not really known but may probably be due to increase in case detection and community sensitization as well as change in microscopic or laboratory diagnostics (introduction to gene xpert) or data quality issues. The decreasing trend noted in 2018 could be due to under-reporting by health facilities. This result should encourage further studies especially with regards to the quality of microscopic centers. According to a 2018 WHO annual report, the high prevalence of TB in Liberia is associated with some socioeconomic factors including insufficient housing (given that Montserrado County hosts the Country´s capital with high population density) and poor-quality health care services, rise in the prevalence of drug resistance TB and TB/HIV comorbidity. The high prevalence recorded in Lima, Peru study was due to the poor living condition and overcrowded communities which of course served as risk for tuberculosis [
15]. Jappar & Low, (2015) in Singapore recognized an increasing trend of tuberculosis over a five (5) year period due to tourism and the high influx of people in the area [
16]. On the contrary, an Ethiopian study conducted amongst prisoners indicated findings of a low prevalence. Though with an unclear reason, but it was realized that multiple factors may have contributed to the low prevalence including campaign to prevent TB that was conducted by the Federal Ministry of Health of Ethiopia which led to reduction of TB prevalence in the general population prior to the study [
17].
This research findings also differ from that of Uganda which study results showed a modest declining trend in TB notification rate reported in Kampala [
18].
Our findings revealed that majority of the cases notified during the three-year period completed treatment and were cured. The National TB and Leprosy control program of Liberia classified patients as cured if they completed treatment and were negative of tuberculosis infections upon retesting. Whereas, those who just completed treatment, are those not retested. However, the data showed that majority of the patients were not retested which could probably be due to poor knowledge or awareness amongst patients on the final testing after the medication has been completed. The treatment success rate among patients in Montserrado County was low (24%) which is less than the national target of 85%. In 2017, higher percentage of patients on treatment defaulted. This could be due to pill burden, stigma or even inadequate treatment support. Another study suggested that TB patients default due to inadequate supervision by health providers within the Direct Observed Treatment (DOT) strategy [
19]. Due to infrastructure and inadequate health services, treatment support services for TB in several developing countries, is accessible to a minute percentage of the population [
20]. A study established that adherence in urban areas, is connected to how well the health care worker provides education on TB specifically to patients as well as the patients´ level of knowledge about the disease [
21]. Similar findings were shown in a study conducted in India that more than one fourth of patients defaulted because of drug toxicity, migration, adverse effects of anti-TB drugs, alcohol, long distance of DOT center from residence and social stigma [
22].
Liberia surveillance system considers TB as a priority disease to be detected and reported at the various levels of the healthcare system. One target outlined in the strategic plan of the National Leprosy & TB Control program is to increase case detection [
11]. It can be observed that from 2016 to 2018, TB case detection rate increased in 2017 dropped slightly in 2018. However, on the overall, the detection rate for the three years is below 50%. This could be due to limited outreach by health providers or poor diagnostic quality. A health facility based study conducted in Ethiopia showed inadequate functioning of health facilities as well as limited reagents contributed to low case detection rate for TB cases [
23]. Another reason could also be staff commitment in sensitizing the public or community on early reporting of TB signs and symptoms. A study conducted in southern Nigeria showed significant increase in the first eight years of case detection rate for TB and stabilization in later years mostly due to the growth and improvement of DOTS services, and the increase was due to the arrangement of enhanced diagnostic and decentralization of the laboratory services, which caused the processing of a huge backlog of cases during the early periods [
24].
Limitation
There were some limitations with the variables on the monthly TB reporting forms at the time including missing treatment outcome variables on cases lost to follow-up, and/or treatment failure. Data showed on the forms are strictly aggregated therefore, some variables like “age” was already categorized and not consistent during the three-year period leaving the researcher with no other choice but to analyze accordingly. The findings from this study are only applicable to the study setting.
Conclusion


The rising trend of Tuberculosis still remains a major problem in Liberia. More males in their productive age group are detected in Bushrod district. The prevalence for sputum smear positive TB was high, 382 per 100,000 population. Almost half of the patients were cured of TB but a few numbers defaulted. The success rate following treatment was very low. We therefore recommend that the National TB control Program should ensure treatment support is provided to patients to enable them adhere to treatment properly in order to improve the treatment success rate and also intensify sensitization on TB education to contribute to the declining trend and improve case detection rate.
What is known about this topic
- The burden and estimated incidence of Tuberculosis
- Tuberculosis is spread rapidly in a cluster or overcrowding population but preventable
What this study adds
- Tuberculosis occurred mostly in a district that is outside of the city center.
- The treatment success rate for Montserrado county is very low
- Not every patient who completes treatment is cured of Tuberculosis
Competing interests


The authors declare no competing interests.
Authors' contributions


The authors declare no competing interests.
Funding
As part of the two (2) years academic work, this research was conducted as a competency output therefore, the principle author was supported by the West Africa Health Organization (WAHO) and the Ghana Field Epidemiology and Laboratory Training Program, University of Ghana.
Acknowledgments


We acknowledged the the following Individuals and Institutions:West Africa Health Organization, Ghana Field Epidemiology & Laboratory Training Program (GFELTP), National Leprosy & Tuberculosis Control Program of Liberia, National Public Health Institute of Liberia, School Of Public Health, University of Ghana.
Tables and figures


Table 1: Demographic Characteristics of reported smear/culture Positive TB cases in Montserrado County, Liberia, 2016-2018
Figure 1: Trend of TB prevalence by year, Montserrado County, Liberia, 2016-2018
Figure 2: TB case detection rate, Montserrado County, Liberia, 2016-2018
Figure 3: Treatment outcomes of TB patients in Montserrado County, 2016-2018
References


- CDC. How TB Spreads: Basic TB Facts[Internet]. CDC; [reviewed 2022 May 3; cited 2022 Dec 29].
- Nugussie DA, Mohammed GA, Tefera AT. Prevalence of Smear-Positive Tuberculosis among Patients Who Visited Saint Paul's Specialized Hospital in Addis Ababa, Ethiopia. Biomed Res Int[Internet]. 2017 Aug 21[cited 2023 Jan 31]; 2017:1-5. https://doi.org/10.1155/2017/6325484 PubMed | Google Scholar
- GBD Tuberculosis Collaborators. The global burden of tuberculosis: results from the Global Burden of Disease Study 2015. Lancet Infect Dis[Internet]. 2018 Mar[cited 2022 Dec 26];18(3):261-284. https://doi.org/10.1016/S1473-3099(17)30703-X PubMed | Google Scholar
- Lawn SD, Wood R, Wilkinson RJ. Changing concepts of "latent tuberculosis infection" in patients living with HIV infection. Clin Dev Immunol[Internet]. 2010 Sep 26[cited 2022 Dec 26];2011:1-9. https://doi.org/10.1155/2011/980594 PubMed | Google Scholar
- WHO. Tuberculosis and HIV[Internet]. WHO; [cited 2023 Jan 31]. PubMed | Google Scholar
- Woimo TT, Yimer WK, Bati T, Gesesew HA. The prevalence and factors associated for anti-tuberculosis treatment non-adherence among pulmonary tuberculosis patients in public health care facilities in South Ethiopia: a cross-sectional study. BMC Public Health[Internet]. 2017 Mar 20[cited 2023 Jan 31];17(1):269. https://doi.org/10.1186/s12889-017-4188-9 PubMed | Google Scholar
- Ragonnet R, Trauer JM, Denholm JT, Marais BJ, McBryde ES. High rates of multidrug-resistant and rifampicin-resistant tuberculosis among re-treatment cases: where do they come from? BMC Infect Dis[Internet]. 2017 Jan 6[cited 2022 Dec 26];17(1):36. https://doi.org/10.1186/s12879-016-2171-1 PubMed | Google Scholar
- GNA. Survey says tuberculosis prevalence in Ghana is high. Ghana Web.[Internet] 2015 Mar 26[ updated 2015 Mar 28, cited 2022 Dec 29]. PubMed | Google Scholar
- World Health Organization, WHO Regional Office for Europe, National Tuberculosis and Lung Diseases Research Institute (Poland)TB Manual National Tuberculosis Programme Guidelines[Internet]. WHO; 2001[cited 2023 Jan 31].
- Ministry of Health and National Public Health Institute of Liberia, World Health Organization and US-Centers for Disease Control and Prevention. National Technical Guidelines for Integrated Disease Surveillance & Response. Third Edition[Internet]. WHO; 2021[cited 2023 Jan 31].
- Ministry of Health and Social Welfare Liberia. National Leprosy and Tuberculosis Strategic Plan 2014 - 2018[Internet]. Ministry of Health and Social Welfare Liberia; 2014[cited 2022 Dec 28].
- Marçôa R, Ribeiro AI, Zão I, Duarte R. Tuberculosis and gender-Factors influencing the risk of tuberculosis among men and women by age group. Pulmonology[Internet]. 2018[cited 2023 Jan 31];24(3):199-202. https://doi.org/10.1016/j.pulmoe.2018.03.004 Google Scholar
- Horton KC, MacPherson P, Houben RM, White RG, Corbett EL. Sex Differences in Tuberculosis Burden and Notifications in Low- and Middle-Income Countries: A Systematic Review and Meta-analysis. PLoS Med[Internet]. 2016 Sep 6[cited 2023 Jan 31];13(9):e1002119. https://doi.org/10.1371/journal.pmed.1002119 PubMed | Google Scholar
- Nyamogoba H, Mbuthia G. Gender-age distribution of tuberculosis among suspected tuberculosis cases in western Kenya. Med. Sci. Int. Med. J[Internet]. 2018[cited 2023 Jan 31];7(2):252-6. https://dx.doi.org/10.5455/medscience.2017.06.8735 Google Scholar
- Otero L, Shah L, Verdonck K, Battaglioli T, Brewer T, Gotuzzo E, Seas C, Van der Stuyft P. A prospective longitudinal study of tuberculosis among household contacts of smear-positive tuberculosis cases in Lima, Peru. BMC Infect Dis[Internet]. 2016 Jun 8[cited 2023 Jan 31];16(1):259. https://doi.org/10.1186/s12879-016-1616-x PubMed | Google Scholar
- Jappar SB, Low SY. Tuberculosis trends over a five-year period at a tertiary care university-affiliated hospital in Singapore. Singapore Med J[Internet]. 2015 Sep[cited 2022 Dec 27];56(9):502-5. https://doi.org/10.11622/smedj.2015134 PubMed | Google Scholar
- Tsegaye Sahle E, Blumenthal J, Jain S, Sun S, Young J, Manyazewal T, Woldeamanuel H, Teferra L, Feleke B, Vandenberg O, Rey Z, Briggs-Hagen M, Haubrich R, Amogne W, McCutchan JA. Bacteriologically-confirmed pulmonary tuberculosis in an Ethiopian prison: Prevalence from screening of entrant and resident prisoners. PLoS One[Internet]. 2019 Dec 12[cited 2023 Jan 31];14(12):e0226160. https://doi.org/10.1371/journal.pone.0226160 PubMed | Google Scholar
- Wobudeya E, Sekadde-Kasirye M, Kimuli D, Mugabe F, Lukoye D. Trend and outcome of notified children with tuberculosis during 2011-2015 in Kampala, Uganda. BMC Public Health[Internet]. 2017 Dec 19[cited 2023 Jan 31];17(1):963. https://doi.org/10.1186/s12889-017-4988-y PubMed | Google Scholar
- Kigozi G, Heunis C, Chikobvu P, Botha S, Van Rensburg D. Factors influencing treatment default among tuberculosis patients in a high burden province of South Africa. International Journal of Infectious Diseases[Internet]. 2017 Jan 1[cited 2023 Jan 31];54:95-102. https://doi.org/10.1016/j.ijid.2016.11.407 Google Scholar
- Danso E, Addo IY, Ampomah IG. Patients´ compliance with tuberculosis medication in Ghana: evidence from a periurban community. Advances in Public Health[Internet]. 2015 Feb 1[cited 2023 Jan 31];2015:1-6. https://doi.org/10.1155/2015/948487 Google Scholar
- Dooley KE, Lahlou O, Ghali I, Knudsen J, Elmessaoudi MD, Cherkaoui I, El Aouad R. Risk factors for tuberculosis treatment failure, default, or relapse and outcomes of retreatment in Morocco. BMC Public Health[Internet]. 2011 Feb 28[cited 2023 Jan 31];11(1):140. https://doi.org/10.1186/1471-2458-11-140 PubMed | Google Scholar
- Burton NT, Forson A, Lurie MN, Kudzawu S, Kwarteng E, Kwara A. Factors associated with mortality and default among patients with tuberculosis attending a teaching hospital clinic in Accra, Ghana. Transactions of the Royal Society of Tropical Medicine and Hygiene[Internet]. 2011 Dec 1[cited 2023 Jan 31];105(12):675-82. https://doi.org/10.1016/j.trstmh.2011.07.017 Google Scholar
- Abayneh M, HaileMariam S, Asres A. Low Tuberculosis (TB) Case Detection: A Health Facility-Based Study of Possible Obstacles in Kaffa Zone, Southwest District of Ethiopia. Can J Infect Dis Med Microbiol[Internet]. 2020 May 15[cited 2023 Jan 31];2020:1-9. https://doi.org/10.1155/2020/7029458 PubMed | Google Scholar
- Ukwaja KN, Alobu I, Ifebunandu NA, Osakwe C, Igwenyi C. Trend in case detection rate for all tuberculosis cases notified in Ebonyi, Southeastern Nigeria during 1999-2009. Pan Afr Med J[Internet]. 2013 Sep 12[cited 2023 Jan 31] ;16(11). https://doi.org/10.11604/pamj.2013.16.11.680 PubMed | Google Scholar