A Process Evaluation of the Isoniazid Preventive Therapy Program in Sanyati District, Mashonaland West Province, Zimbabwe 2019
Chamunorwa Mhembe1, Daniel Chirundu2, Cleophas Chimbetete1,3, Notion Tafara Gombe4, Tsitsi Patience Juru1, Addmore Chadambuka1,&, Gerald Shambira1, Mufuta Tshimanga1
1Department of Primary Health Care Sciences: Family Medicine, Global and Public Health Unit, University of Zimbabwe, 2Kadoma City Health Department, Kadoma, Zimbabwe, 3Newlands Clinic, Harare, Zimbabwe, 4African Field Epidemiology Network, Harare, Zimbabwe
&Corresponding author
Addmore Chadambuka, University of Zimbabwe, Office 3-68 Kaguvi Building, Cnr 4th/Central Avenue,Harare, Zimbabwe
Introduction:
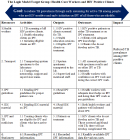
The Isoniazid Preventive Therapy (IPT) is a public health program dedicated to reducing mortality due to TB through early screening for active TB among people who are HIV-positive and early initiation on IPT of all who are eligible. A review of the 2019 Sanyati District IPT program data indicated that not all clients eligible for the IPT were initiated on the IPT program. In January, June, September, and December, 3% of IPT eligible HIV-positive clients were initiated on IPT; in March, May, and October, 2%, in April, July and November, 1%, in February, 5% and in August 2019, 4%. Only 4% of all IPT illegible HIV positive clients were initiated on IPT in 2019 against a target of 100% set by the Global Fund. A 31% dropout rate was recorded from the 94 clients initiated on IPT. Of the 26 health facilities in Sanyati District including five Kadoma City Council Clinics, only 16 health facilities were offering Antiretroviral Therapy (ART) initiation and IPT services. The IPT program in Sanyati District has never been evaluated, therefore a process evaluation of the IPT programme in the district was conducted to recommend strategies to improve on initiation of all eligible IPT clients.
Methods:
A process evaluation among 16 health facilities which were offering IPT and ART services in Sanyati District was conducted using the logic model and the IPT program theory. The evaluator employed a mixed methods approach, using interviewer administered questionnaires, key informant guides to collect data and a review of IPT registers and all the documents used for the IPT program. The Statistical Package for Social Sciences (SPSS) software was used to generate frequencies, means and proportions, narrative, content, and thematic analyses were used for qualitative data analysis. The evaluation was approved by Mashonaland West Provincial Ethics Committee and permission was obtained from Sanyati District Health Executive and the Health Studies Office.
Results:
Data from 81 health workers in health facilities offering IPT services in Sanyati District were analysed. Majority of health workers 39% (31/81) were Primary Care Nurses (PCNs). Only two of 16 health facilities had inadequate health workers. The median years in service for the interviewed key informants was 2(Q1=1; Q3=2.5) years. Only seven IPT guidelines and 11 TB/HIV Co-management guidelines were available, and they were not adequate for the 26 health facilities in the district. Tuberculosis screening tools, Directly Observed Therapy (DOT) registers and the Isoniazid (INH) medicines were all available more than the district requirements. Health worker mentorship, social mobilisation, support and supervision as well as IPT review meetings were not done in 2019. Only 4% (94/2350) of the HIV-positive clients who were illegible for IPT were initiated on IPT. No meetings were held on IPT in the district and only 10% (224/2350) of HIV-positive clients were screened for TB in 2019.
Conclusion:
The IPT program in Sanyati District had inadequate inputs; not all processes were achieved and, most of the program outputs were not met as most clients who were eligible for IPT were not initiated on IPT. There was lack of health worker mentorship as well as quarterly support and supervision visits by the program managers. We recommended training of health workers on IPT, production and distribution of IEC material and procurement of IPT guidelines and motorization of health workers who were involved in IPT follow ups.
Introduction

The overlap of latent tuberculosis infection (LTBI) and Human Immunodeficiency Virus (HIV) infection has resulted in marked increase in tuberculosis (TB) incidence in countries with dual epidemics and TB has become one of the most common opportunistic infections and the leading cause of death in HIV-infected people in Africa, Asia and Latin America [1]. Zimbabwe is among the countries with highest estimated TB incidence per capita (603/100 000 population) in the world. Sixteen percent of adult population in Zimbabwe is HIV infected, and approximately 75% of active TB cases occur among persons with HIV [1]. The World Health Organisation (WHO) demonstrated that ART reduces the risk of TB in HIV-infected patients, but rates of TB remain unacceptably high despite this intervention [1]. The isoniazid preventive therapy (IPT) program is dedicated to reduce mortality due to TB through early screening for active TB among people who are HIV-positive and early initiation on IPT of all those who are eligible [2]. HIV-positive clients who are screened for TB and found without active TB are initiated on IPT, those screened and found to have active TB are commenced on TB treatment. Isoniazid-induced peripheral neuropathy and neurotoxicity are well known adverse effects among IPT clients. Vitamin B6 or Pyridoxine is usually prescribed to clients on IPT for the prevention of Isoniazid-induced side effects. [3]. Studies demonstrated that there is a remarkably consistent effect, with reduction in the relative rate of TB by 80% in patients who received ART compared with those not receiving ARVs, even after adjusting for CD4 cell count [4]. The Mashonaland West Provincial TB and HIV data indicated that the province had a TB/ HIV co-infection rate of 54% as of December 2018. Among the seven districts in Mashonaland West Province, Sanyati District had the highest TB HIV co-infection rate of 67%.
A review of the 2019 Sanyati District IPT program data indicated that not all clients eligible for the IPT were initiated on the IPT program. Of the 2350 clients eligible for IPT in 2019, only 4% were initiated. In January, June, September, and December 2019, 3% of IPT eligible HIV-positive clients were initiated on IPT on each month against a target of 100% which is recommended by the Global Fund. In March, May, and October of 2019 only 2% of IPT eligible HIV-positive clients were initiated on IPT on each month, only one percent of IPT eligible HIV-positive clients were initiated in the months of April, July, and November. In February, 5% were initiated and only 4% were initiated in August 2019. In 2019, the monthly percentages of HIV-positive clients who were initiated on IPT were far below the Global Fund recommended target of 100%. According to the IPT guidelines, all HIV-positive patients who do not have active TB are supposed to be put on IPT medication for six months to prevent the development of latent TB [
5]. In 2019, a 31% dropout rate was recorded from a total of 94 clients which were initiated on IPT. We did not find evidence of previous evaluation of the IPT program in Sanyati District. Despite resources being continuously availed for the IPT program in Sanyati District by the Global Fund in conjunction with the Ministry of Health and Child Care, immediate and intermediate outcomes of the program have not been achieved. A process evaluation of the IPT program in Sanyati District was important to evaluate resources availability, to assess IPT programme processes such as, IPT surveillance meetings held, health workers´ support, supervision and mentorship, to assess knowledge of Health Workers who were involved in the IPT program and to assess the outputs of the IPT program in Sanyati District.
Isoniazid Preventive Therapy Program Design
The IPT program aims to reduce TB prevalence among people living with HIV [
6]. Stakeholder consultations were done at district level as part of the IPT program process evaluation. Information from the consultations was used to come up with the logic model
Figure 1.
Program Theory for the Isoniazid Preventive Therapy
The program theory applied for this process evaluation was based on existing evidence of cause-and-effect relationship between TB and associated morbidity and mortality. An existing program theory for the IPT program is as follows:
- If TB screening services are provided to all HIV-positive clients and those without active TB are initiated on IPT and those with active TB on TB medicines, It is expected that most HIV-positive clients will know their TB status on time and will be put on either TB treatment or on IPT to reduce the chances of developing TB diseases and of dying from TB. If Isoniazid (INH) initiation is done to all eligible HIV-positive clients, it is expected that latent TB in clients will not develop to active TB. If IPT training and mentorship is provided to all health workers involved in the IPT program, it is expected that the quality of IPT services offered within Sanyati District will improve. If health promotion activities which include producing and procuring IPT IEC material targeting all HIV-positive clients are provided, it is expected that health workers will have skills and confidence to screen, categorize, initiate, and properly manage IPT clients. Both health workers and eligible IPT clients are also expected to have adequate information on IPT services like, benefits of IPT and importance of early TB screening.
Evaluation Questions
The IPT program evaluation questions were: 1) what processes are involved in the IPT program in Sanyati District? 2) Are the inputs adequate for effective implementation of the IPT program in Sanyati Districts? 3) What are the challenges in implementing the IPT program in Sanyati District?
Evaluation Objectives
The objectives of the process evaluation were to evaluate resource availability for the IPT program, to assess IPT program processes such as, IPT surveillance meetings held, health worker support, supervision, and mentorship, to assess knowledge of health workers who are involved in the IPT program, to assess the outputs of the IPT program and to assess how social mobilisation was conducted in Sanyati District, Mashonaland West Province, 2019.
Readiness for Evaluation
Following the evaluability assessment, we found it plausible for the program to achieve its expected results. The evaluability assessment established the existence of enough program data that was sufficient to answer the evaluation questions. Information that was not available was collected from interviews with the health care workers and key informants during the evaluation. The cost of gaining new data during the process evaluation was minimum as data were collected from only 16 health facilities which were providing the IPT services in Sanyati District. Resources to conduct the evaluation were easily acquired as there was buy in for this evaluation from most stakeholders. The evaluability assessment established program readiness for evaluation prior to the comprehensive evaluation.
Methods


Study Design
We conducted a retrospective process evaluation of the Isoniazid Preventive Therapy program in Sanyati District in Mashonaland West Province using the logic model and the IPT program theory. A mixed methods approach was used, where both quantitative and qualitative methods were used in the evaluation.
Study Setting
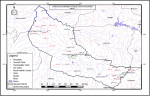
The evaluation was conducted in Sanyati District, one of the seven districts in Mashonaland West Province, Zimbabwe. Data gathered from the Mashonaland West Provincial Health Information office indicated that, Sanyati District was the least performing district in the IPT program among the seven districts in the province. The other six districts which are Makonde, Kariba, Chegutu, Zvimba, Mhondoro-Ngezi and Hurungwe had more than 50% of all IPT illegible HIV-positive clients initiated on IPT. Sanyati District had two referral hospitals, Kadoma General Hospital located in Kadoma City in the southern end of the district and Sanyati Mission Hospital located 80 kilometers from Kadoma City in a northern direction. Amongst the twenty-six health facilities, 16 are rural health centres, five local authority clinics, one military clinic and two mine clinics that refer patients to these two major hospitals
Figure 2. Only 16 facilities were offering IPT services in Sanyati District. Five rural health centres, two Kadoma City council clinics, one military clinic and two mine clinics were not offering IPT services.
Study Population
The study population consisted of all the Nurses in-charge and EHTs at the 16 health facilities which were offering IPT services in Sanyati District. The Nurses in-charge, EHTs, OI/ART focal nurses and the health facilities were recruited into the study. The District Medical Director (DMO), Director Health and Environmental Services for Kadoma City Council, District TB Coordinator (DTC), Pharmacist and Laboratory Scientist from Sanyati District Hospital, were recruited as key informants.
Sample Size Calculation
A sample size of health workers who were involved in the IPT program and who participated in the study was calculated using the Dobson formula {Z2(p(1-p)/d2}, basing on a study by Abossie A, et al. (2017) , where the prevalence (p) of health workers who were not trained on IPT and did not have adequate knowledge on IPT in Ethiopia was 4%[
4]. The sample size was calculated using a study power of 80% at 5% level of significance. The calculated sample size was 59 and after factoring in the 10% non-response rate, the calculated minimum sample size was 65 health workers who were involved in the IPT program. However, in this process evaluation, all the 81 health workers who were involved the IPT program in Sanyati District were interviewed in this process evaluation.
Sampling
All 16 health facilities which were offering IPT services in Sanyati District participated in the study and all health workers involved in the IPT program at those health facilities were interviewed. The District Medical Officer (DMO), Director Health and Environmental Services at Kadoma City Health, District TB Coordinator (DTC), OI/ART focal persons, Laboratory Scientist and the Pharmacist from the district hospital, were purposively recruited into the study as key informants.
Data Collection
Interviewer administered questionnaires were used on health workers in the district to get information about IPT services in Sanyati District and demographics of respondents. On data collection for the IPT program, all hard copies of registers in use during the evaluation and all hard copies of IPT registers at all facilities offering IPT services were reviewed. We checked for availability of electronic copies of the Isoniazid Preventive Therapy and TB/HIV co-infection management guidelines. Hard copies of IPT registers and health centre Directly Observed Treatment (DOT) registers were reviewed. To ensure confidentiality of all physical paper documents used in this evaluation, the documents were kept under lock and key. A five point Likert scale adopted and adapted from a study by Teklay G et al. (2016) was used in assessing health workers knowledge on IPT program in Sanyati District [
7]. Process evaluation focus group discussion guides and key informant guides were used to collect data from the key informants on plans made, budget allocations, trainings and support and supervisions done within the district.
Validity and Reliability
To test for validity and reliability of research instruments, all the data collection tools were pretested at Chegutu District Hospital. Necessary adjustments were made on the questionnaires and checklists. Some of the research instruments used in this evaluation were adopted and adapted from the New England Journal of Medicine on a trial of mass Isoniazid Preventive Therapy for Tuberculosis [
8].
Data Analysis
Data were checked for completeness and accuracy then captured using the Statistical Package for Social Sciences (SPSS) version 20. The statistical software was used to generate frequencies and proportions. Content, narrative, and thematic analyses were used for analysis of qualitative data from the key informants.
Ethical Considerations
The study was reviewed and approved by the Mashonaland West Provincial Ethics Committee. We obtained permission to carry out the study from Sanyati District Health Executive and Kadoma City Council. We maximised the study benefits to Sanyati District health personnel by continuously giving them feedback during and after the study. Confidentiality was assured and maintained throughout the study by interviewing each participant privately and ensuring that no information obtained was disclosed to any persons other than those relevant for the purposes of the study. Confidential documents were kept under lock and key. Names of participants were not written on questionnaires.
Results


Program Description
The Isoniazid Preventive Therapy is one of the public health strategies being used to reduce the incidence of HIV-related TB in developing countries [
5]. In Zimbabwe, the Isoniazid Preventive Therapy program is being funded by the Global Fund. In Sanyati District, health workers were trained when the programme was initiated in 2003, however the Global Fund recommend funded districts to conduct on-job training to their nurses, doctors and EHTs who are involved in the IPT program. Information Education and Communication (IEC) material is produced by the health promotion unit housed in the AIDS and TB unit at Ministry of Health and Child Care (MoHCC) head office, for onwards distribution to HIV/TB high burden districts like Sanyati. Some of the resources for the IPT program are Isoniazid Preventive Therapy registers, TB and HIV co-management guidelines, Directly Observed Treatment Short course registers, sputum mugs used for TB screening purposes, TB screening tools and Isoniazid medicines are distributed to every district upon request by the Global Fund in Partnership with MoHCC
Table 1.
The processes involved in running the IPT program include training and mentorship of health workers on IPT program, conducting IPT review clinics, budgeting, conducting IPT advocacy, TB screening of all HIV-positive patients and IPT initiation in all the patients without active TB
Table 2. Some of the outputs of the IPT program are the number of meetings on IPT held, number of health workers trained, number of HIV-positive screened for TB, number of screened HIV-positive patients who are eligible for IPT and number of HIV-positive clients who completed IPT
Table 3. The outcomes of the IPT program include health workers with improved knowledge and skills on IPT, increased proportion of HIV-positive clients screened for TB and increased proportion of eligible IPT clients who will be on IPT medication. The stakeholders and intended users of the evaluation include Mashonaland West Provincial Health Executive (PHE), Sanyati District Health Executive (DHE), partners, program officers and the implementers.
This process evaluation was done in Sanyati District and involved 81 health care workers who were involved in the IPT program in health facilities in Sanyati District. Sixteen health facilities offering IPT services in Sanyati District participated in the study and all health workers involved in the IPT program at those health facilities were interviewed. The District Medical Officer, Director Health and Environmental Services at Kadoma City Health, District TB Coordinator, OI/ART focal persons, Laboratory Scientist, and the Pharmacist from the district hospital, were recruited into the study as key informants
Table 4. The median years in service for the interviewed key informants was 2(Q1=1; Q3=2.5) years
Figure 3.
Only 19% (15/81) of health workers were trained on IPT in Sanyati District. All the health workers who reported to have received training on IPT, reported that it was in service training. Majority (13/15) of the health workers who received IPT training were nurses. On other inputs injected into the IPT program, no IPT Information Education and Communication (IEC) materials were received for the program in 2019. Only 7 IPT guidelines and 11 TB/HIV Co-management guidelines were available, and they were not adequate for the 26 health facilities in the district. In 2019 the district received 8 000 sputum mugs against a requirement of 12 000 mugs per year. Tuberculosis screening tools, Directly Observed Treatment registers and the INH medicines were all available more than the district requirements. The program was being implemented without some of the necessary inputs like, trained health workers, IEC material and specimen courier services. The district was operating without vehicle dedicated for the TB and HIV collaborative activities
Table 1.
The whole district had seven IPT guidelines against a requirement of 26 and 11 TB/HIV co-management guidelines against a requirement of 26. Logbooks for IPT support and supervision were also reviewed and only two health facilities were visited by some DHE members for IPT support and supervision in February 2019. Though the district received excess (48 against a requirement of 26) IPT registers for the year 2019, three health facilities were improvising IPT registers. They were using counter books as IPT registers. The use of improvised IPT documents was reported to contribute to loss of data as some of the data was even collected on pieces of paper that ended up being lost before being entered in the main registers.
Some of the processes which were involved in the IPT program include: planning for IPT services, training of health workers on IPT, IPT advocacy, INH initiation and holding of IPT review meetings. No plans for the IPT program were in place and health workers in Sanyati District did not receive any IPT training in 2020. Health worker mentorship, support, and supervision as well as IPT review meetings were not done in 2020. Out of the 2 350 HIV positive clients who were illegible for IPT only 4% (94/2350) of those eligible were initiated on IPT
Table 3. No meetings were held on IPT in the district and only 10% (224/2350) of HIV positive clients were screened for TB in 2020 of which 4% of eligible patients (94/2350) were initiated on IPT. One client was lost to follow up and two clients died whilst they were still on IPT treatment
Table 3.
In this evaluation, we assessed knowledge of health workers on IPT. All health workers in the district had heard about the IPT program, however only 93% (75/81) knew the goal of the IPT program. Among the respondents, 84% (68/81) and 73% (59/81) knew the recommended duration of IPT and clients who were eligible for IPT respectively. Most health care workers in Sanyati District had good knowledge of the IPT program
Table 5.
We assessed number of health workers who were involved in the IPT program at each facility in Sanyati District. The median number of health workers involved in IPT at health facilities in Sanyati District was 10(Q1=7; Q3=16). Of the 16 facilities evaluated, only two facilities had inadequate health workers. Only 2.47% (2/81) of the health workers received formal training in IPT while the rest received “on-job´ training. Kadoma and Sanyati Baptist Hospitals had the greatest number of health workers involved in the IPT program. Kadoma Hospital had 22 health workers involved in IPT whilst Sanyati Baptist Hospital had 16 health workers involved in the IPT program. Two health facilities had six health workers at each facility who were participating in the IPT program in Sanyati District. The two facilities had the least number of health workers who were participating in the IPT program in the district.
On IPT social mobilization, eleven facilities out the 16 facilities reported conducting social mobilizations in their respective communities to generate demand for IPT services. Social mobilizations were done monthly, and some facilities did quarterly. Owing to lack of resources, some facilities were not able to conduct social mobilization resulting in frequency of conducting social mobilizations that was as low as twice yearly. The common channel for social mobilization was through utilization of community meetings and gatherings. Environmental Health Technicians were the key health workers in interfacing with the communities. The list frequently recorded method of communication was using village heads and writing letter to potential patients and key stakeholders.
On Sanyati District support in social mobilization, only fourteen health facilities reported getting social mobilisation from the district. For those facilities that got support, it was in the form of IPT medicines and social mobilisation support from the Health Promotion department. Two of the 16 health facilities indicated not having benefited from district social mobilisation activities.
From the key informants, the district health executive confirmed that, IPT activities were being neglected in the district. The DHE members admitted that they did not conduct IPT support and supervision as well as supporting of IPT social mobilization within the district as reflected:
“We neglected the AIDS and TB unit of our district for the year 2019, we never carried out support and supervision visits particularly for the TB program. The IPT services never got support from the district” (Key Informant 1).
The process evaluation focus group discussion noted that IPT resources were available, however, lack of dedication by DHE members to supervise the distribution and usage of IPT resources was cited as the major barrier to successful implementation of the IPT program and to achieve IPT set targets as reflected:
“Sanyati as a district received all the necessary support for the IPT program, however only few items like sputum mugs were sometimes in short supply” (Key Informant 4).
The DHE also cited lack of funds to conduct formal trainings for health workers as a challenge in achieving IPT set targets. The Ministry of Health and Child Care, AIDS and TB unit in conjunction with partners was supposed to provide funding for IPT training, but nothing was provided in 2019. Some key informants recommended strengthening of support and supervision activities targeting the IPT program within Sanyati District as reflected:
“I strongly recommend that the DHE members should conduct support and supervision visits to all health facilities within the district, as this will help the in improving the IPT program within the district” (Key Informant 6).
Discussion


In our process evaluation of the Isoniazid Preventive Therapy in Sanyati District, in Mahonaland West Province, we found out that lack of resources was the major barrier to smooth implementation of the IPT program in in the district. In real life experience, it is common that programs with inadequate resources will usually fail to achieve intended outcomes and impact. This was the case with the IPT program in Sanyati District, inadequate IPT inputs could have led to the failure by the district to initiate all eligible IPT clients on IPT medicines. The most important resource in any program is the human resource component. Adequate and motivated human resources, coupled with adequate financial resources and properly laid down processes and procedures promote achievement of program outcomes and impacts [9]. In Sanyati District, health workers to implement the IPT program were inadequate. Adequate, motivated and trained health workers plays a key role in developing, reinforcing and changing the culture of any health delivery system. Training of health workers promotes ongoing opportunities to learn, develop and enhance skills and knowledge [10]. A few Primary Care Nurses in Sanyati District Rural Health Centres received on-job training of the IPT program in 2013 when the program was piloted in the district citing lack of resources to capacitate the health workers. Consistent to our study findings, Grant et al. (2015) in South Africa noted lack of trained human resources as the major hindrance to the IPT program in that country [11].
Sanyati District also experienced shortage of IPT guidelines as well as TB/HIV co-management guidelines. Clinical guidelines assist health practitioner and patient decisions about appropriate health care for specific clinical circumstances. We found out that, no IEC material was received from the district and provincial Ministry of Health offices during the year. In a study on beneficial and perverse effects of IPT for latent tuberculosis infection in HIV/TB-co-infected populations, it was highlighted that lack of adequate IEC material in TB programs can result in failure to meet intended TB outcomes by the program [
11]. This was the case with the IPT program in Sanyati District which failed to meet the intended outcomes as the IPT program was being implemented without all the necessary inputs.
Lack of trained human resources and materials to use for any program is always linked to failure of many programs [
12]. In Brazil, programs which were implemented with insufficient resources and untrained manpower were failing to yield intended results [
13]. In Sanyati District, we noted similar results as those noted in Brazil as shortages of fuel, IEC materials and a reliable courier system were noted. The deficiencies noted in the IPT program in Sanyati District negatively contributed to the low performance of the program in the district.
In our evaluation we noted that, there we no IPT plans in the district. Planning and budgeting are very necessary in an organisation as they assist in mobilisation of sufficient and necessary resources [
14]. Planning for the IPT program is important in deciding clearly and concretely what needs to be done to have the desirable effects on a community. In Cambodia, similar results to our findings were also reported, whereby, lack of planning was cited as a major factor that contributed to failure in meeting IPT targets in the country [
15].
The study also revealed that quarterly supervision visits, health worker mentorship and support were not conducted. The purpose of health worker mentorship is to help mentees tap into the knowledge of those with more experience and expertise than themselves. Mentorship in Sanyati District was going to assist health workers to learn faster on IPT program best practices and to establish a good platform for knowledge sharing with supervisors than they would on their own. These findings are consistent with Burungi et al. (2018), who found out that lack of health worker mentorship as well as lack of support and supervision visits in the TB program by district managers in Rwanda, contributed to failure in achieving WHO set targets [
16].
The WHO highlighted that supportive supervision encourages open two-way communication and building team approaches that facilitate problem solving. For the IPT program in Sanyati District, the District Health Executive was supposed to conduct quarterly visits to health facilities focusing on monitoring IPT program performance towards IPT goals. The District Health Executive was also supposed to follow-up with health workers to ensure that IPT program tasks were being implemented correctly. This was also highlighted by one of the key informants who pointed out the importance of staff mentorship as well as support and supervision in promoting successful implementation of the IPT program. Support and supervision visits are very necessary as barriers to successful implementation of the program are timeously identified by health managers and corrective measures are also timeously put in place for smooth running of any health program [
17].
In 2019, Sanyati District did not hold any IPT review meetings and key informants cited lack of funds to support these meetings as the major challenge. Review meetings help health workers to understand how to optimise their performance, identify where they are, who needs to be involved in the program implementation, how to make improvements, and how often review meetings need to be held to make those improvements. Yumo et al. (2016) in Cameroon noted that lack of coordination meetings was a major drawback in reducing the burden of TB among HIV positive patients in Cameroon [
1].
Sanyati District was operating without vehicle dedicated for the TB and HIV collaborative activities. A vehicle in the TB and HIV program is used to transport patients, supply drugs to TB/HIV clinics, collect sputum specimen for laboratory testing, support and supervisory visits to clinics as well as in monitoring treatment supporter programs. Contrary to our findings in Sanyati District, Durovin et al. (2010) in Rio de Janeiro Brazil noted successful implementation and meeting of targets in the TB and HIV programs in the Brazil capital as a result of having enough resources particularly dedicated vehicles for the HIV and TB control programme [
18].
A successful TB program should be supported with a reliable courier system. A successful IPT program require TB ambulances, motorcycles for contact tracing, active case finding and for timeous transportation of specimens [
19]. This was not the case with Sanyati District as there were no vehicles dedicated for the program and only one serviceable motorcycle for the TB coordinator was available. Only three malaria control program motorcycles were used by three EHTs who were stationed in Rural Health Centres to conduct TB/HIV activities in their catchment areas. The transport situation in Sanyati District was not ideal for the smooth flow of the IPT program. Specimens from clinics were supposed to be transported in leak proof biohazard bags with sealed lids and absorbent material. Specimens are to be transported to the laboratory in a cooler box with chilled ice packs as soon as possible after collection. In Sanyati District specimens were not being timeously transported to the laboratory as 77% (10/13) of the newly recruited EHTs were not motor and these were the cadres who were tasked with the responsibility of transporting specimens to the laboratory. If all the EHTs were motorized, the district was going to witness a smooth implementation of the IPT program and other TB/HIV collaborative activities, as active case finding, contact tracing, client follow up and timeous specimen transportation to the lab was going to be possible. Golub et al. 2014) in Brazil highlighted that community health workers play multiple roles and important roles in making community programs successful if they are given enough resources [
20]. In Sanyati District we noted that motorcycles and fuel were not sufficient for the few community health workers who were supposed to assist in patient follow ups and transportation of sputum specimens to the laboratory.
We assessed IPT knowledge levels of health workers in Sanyati District. and we noted that most health workers had good knowledge of the IPT program. With adequate resources and motivation, the good knowledge base of health workers can be utilised to improve the performance of the IPT program in Sanyati District. Berhe et al. (2014) in Ethiopia also noted that good knowledge among health workers was associated with successful of the IPT among HIV positive patients in Ethiopia [
21].
Study Limitations
Out of the 26 health facilities in Sanyati District, the evaluation was conducted at 16 health facilities which were offering IPT services in the district hence the evaluation findings cannot be generalised to all the districts in Mashonaland West Province or to the whole country. However, insights into the operations of the IPT program in the province can be obtained.
Conclusion


The performance of the IPT program in Sanyati District was negatively impacted by stock outs of some inputs like sputum mugs, inadequate IPT guidelines, inadequate TB/HIV guidelines and unavailability of courier services. Data quality issues that include incompleteness of IPT registers at health facilities and use of loose papers to record IPT data contributed to poor performance of the IPT program in Sanyati District. Minimal involvement of the district in supporting IPT demand creation activities has contributed to low performance of the IPT program. The IPT program in Sanyati District had inadequate inputs, not all processes were achieved and, most of the program outputs were not met as most clients who were eligible for IPT were not initiated on IPT. Though the knowledge of health workers on IPT was good, there was lack of health care worker mentorship as well as quarterly support and supervision visits by the program managers. Lastly there was ample evidence of a lack of resilient monitoring and evaluation systems and plans at health facilities to enable tracking of IPT program progress. We recommended training of health workers in IPT, the DHE to source enough resources for the program and to correct all deviations noted during the process evaluation.
What is known about this topic
- The Isoniazid Preventive Therapy is one of the public health strategies being used to reduce the incidence of HIV-related TB in developing countries
- The IPT program is dedicated to reducing mortality due to TB through early screening for active TB among people who are HIV positive and early initiation on IPT of all those who are eligible
What this study adds
- This study will add literature on IPT program in Zimbabwe, as there was limited literature on this subject. This study will add on strategies that can be employed in various settings to improve TB/HIV programs
Competing interests


The authors declare no competing interests.
Authors´ contributions


CM: conception, design, acquisition, analysis and interpretation of data and drafting the manuscript. DC: conception, design, acquisition, analysis and interpretation of data and drafting the manuscript. GS, CC, NTG, TJ, SC, AC, MT: conception, design, data collection, analysis, interpretation and reviewing of the draft of the manuscript for important intellectual content.
Acknowledgements


The authors gratefully acknowledge Sanyati District Health Team, Kadoma City Council and the University of Zimbabwe, Department of Primary Health Care Sciences: Family Medicine, Global and Public Health Unit, and Zimbabwe Field Epidemiology Training Programme (ZimFETP) for their support.
Tables and figures


Table 1: Demographic Characteristic of Health workers, Sanyati District, Mashonaland West Province, 2019
Table 2: Inputs injected into the IPT Program, Sanyati District, Mashonaland West Province, 2019
Table 3: Processes for IPT program in Sanyati District, Mashonaland West Province, 2019
Table 4: Outputs for IPT Program in Sanyati District, Mashonaland West Province, 2019
Table 5: Knowledge of health workers on IPT program in Sanyati District, Mashonaland West Province, 2019
Figure 1: Logic Model for Isoniazid Preventive Therapy in Sanyati District, 2019
Figure 2: Spatial Distribution of Health Facilities in Sanyati District, Mashonaland West Province, 2019
Figure 3: Number of years in service for the interviewed key informants at health facilities, Sanyati District, Mashonaland West Province, 2019
References


- Yumo HA, Kuaban C, Neuhann F.WHO recommended collaborative TB/HIV activities: evaluation of implementation and performance in a rural district hospital in Cameroon. PAMJ[Internet]. 2011 Nov 02[cited 2023 Sep 15]; 10:30. https://doi.org/10.11604/pamj.20110.30.581 Google Scholar
- Hart L.Isoniazid Preventive Therapy for the Prevention of Tuberculosis in People Living with HIV/AIDS [Internet]. FIH360; Pretoria, South Africa; 2011 Sep[cited 2023 Sep 22]. 5 p. Available from: Download Isoniazid Preventive Therapy for the Prevention of Tuberculosis in People Living with HIV-AIDS Fact Sheet_0. Google Scholar
- Ministry of Health and Child Care (ZIM), AIDS & TB Programme. Operational and Service Delivery Manual for the Prevention, Care and Treatment of HIV in Zimbabwe 2022. 3rd ed. [Internet]. Harare, Zimbabwe: Ministry of Health and Child Care (ZIM), AIDS & TB Programme; 2022 [cited 2023 Sep 23]. 145 p. Download MSF-Zim-OSDM-Nov2022-WEB2.
- Abossie A, Yohanes T.Assessment of isoniazid preventive therapy in the reduction of tuberculosis among ART patients in Arba Minch Hospital, Ethiopia . Journal of Therapeutics and Clinical Risk Management[Internet]. 2017 Mar 24 [cited 2023 Sep 15]; 2017:13. https://doi.org/10.2147/TCRM.S127765 PubMed | Google Scholar
- World Health Organization. A guide to monitoring and evaluation for collaborative TB/HIV activities - 2015 revision [Internet]. Geneva, Switzerland: World Health Organization; 2015 Apr 13[cited 2023 Sep 15]. 48 p. Google Scholar
- Cohen T, Lipsitch M, Walensky RP, Murray M.Beneficial and perverse effects of isoniazid preventive therapy for latent tuberculosis infection in HIV-tuberculosis coinfected populations . Proc Natl Acad Sci USA [Internet]. 2006 May 2 [cited 2023 Sep 15];103(18):7042-7. https://doi.org/10.1073/pnas.0600349103 PubMed | Google Scholar
- Teklay G, Teklu T, Legesse B, Tedla K, Klinkenberg E.Barriers in the implementation of isoniazid preventive therapy for people living with HIV in Northern Ethiopia: a mixed quantitative and qualitative study . BMC Public Health [Internet]. 2016 Aug 19[cited 2023 Sep 15];16(1):840. https://doi.org//10.1186/s12889-016-3525-8 PubMed | Google Scholar
- Churchyard GJ, Fielding KL, Lewis JJ, Coetzee L, Corbett EL, Godfrey-Faussett P, Hayes RJ, Chaisson RE, Grant AD. A trial of mass isoniazid preventive therapy for tuberculosis control . N Engl J Med [Internet]. 2014 Jan 23 [cited 2023 Sep 15];370(4):301-10. https://doi.org/10.1056/NEJMoa1214289 Google Scholar
- Sandgren A, Vonk Noordegraaf-Schouten M, Van Kessel F, Stuurman A, Oordt-Speets A, Van Der Werf MJ.Initiation and completion rates for latent tuberculosis infection treatment: a systematic review . BMC Infect Dis [Internet]. 2016 May 17[cited 2023 Sep 23];16(1):204. https://doi.org/10.1186/s12879-016-1550-y PubMed | Google Scholar
- Maponga BA, Chirundu D, Shambira G, Gombe NT, Tshimanga M, Bangure D.Evaluation of the notifiable diseases surveillance system in sanyati district, Zimbabwe, 2010-2011 . PAMJ[Internet]. 2014 Nov 14[cited 2023 Sep 22];19:278. https://doi.org/10.11604/pamj.2014.19.278.5202 PubMed | Google Scholar
- Grant AD, Charalambous S, Fielding KL, Day JH, Corbett EL, Chaisson RE, De Cock KM, Hayes RJ, Churchyard GJ.Effect of Routine Isoniazid Preventive Therapy on Tuberculosis Incidence Among HIV-Infected Men in South Africa: A Novel Randomized Incremental Recruitment Study . JAMA [Internet]. 2005 Jun 8 [cited 2023 Sep 15];293(22):2719-2725. https://doi.org//doi:10.1001/jama.293.22.2719 Google Scholar
- Souza CTVD, Hökerberg YHM, Pacheco SJB, Rolla VC, Passos SRL.Effectiveness and safety of isoniazid chemoprophylaxis for HIV-1 infected patients from Rio de Janeiro. Mem Inst Oswaldo Cruz [Internet]. 2009 Jun 09[cited 2023 Sep 15];104(3):462-7. https://doi.org/10.1590/S0074-02762009000300011 Google Scholar
- Dowdy DW, Golub JE, Saraceni V, Moulton LH, Cavalcante SC, Cohn S, Pacheco AG, Chaisson RE, Durovni B.Impact of Isoniazid Preventive Therapy for HIV-Infected Adults in Rio de Janeiro, Brazil An Epidemiological Model . JAIDS Journal of Acquired Immune Deficiency Syndromes [Internet]. 2014 Aug 15 [cited 2023 Sep 15];66(5):552-8. https://doi.org//10.1097/QAI.0000000000000219 PubMed | Google Scholar
- Getahun H, Granich R, Sculier D, Gunneberg C, Blanc L, Nunn P, Raviglione M. Implementation of isoniazid preventive therapy for people living with HIV worldwide: barriers and solutions . AIDS [Internet]. 2010 Nov [cited 2023 Sep 15];24(Suppl 5): S57-65. https://doi.org/10.1097/01.aids.0000391023.03037.1f Google Scholar
- Hart L, Canoutas E, Ferradini L, Tonsing J, Harradhya K. National Scale-Up of Isoniazid Preventive Therapy in Cambodia[Internet]. FHI360; Bangkok, Thailand; 2012 Sep[cited 2023 Sep 25]. 6 p. Download ipt-case-study.pdf.
- Birungi FM, Graham S, Uwimana J, Van Wyk B. Assessment of the Isoniazid Preventive Therapy Uptake and Associated Characteristics: A Cross-Sectional Study . Tuberculosis Research and Treatment [Internet]. 2018 May 06 [cited 2023 Sep 15]; 2018: 8690714. https://doi.org/10.1155/2018/8690714 PubMed | Google Scholar
- WHO. Update and summary guide to the report Advancing the right to health: the vital role of law [Internet]. Geneva: World Health Organization; 2018.Chapter 9, Monitoring, Surveillance and Investigation of Health Threats; [cited 2023 Sep 23]; 58 p. Download 9789241513739-eng. Google Scholar
- Durovni B, Cavalcante SC, Saraceni V, Vellozo V, Israel G, King BS, Cohn S, Efron A, Pacheco AG, Moulton LH, Chaisson RE, Golub JE.The implementation of isoniazid preventive therapy in HIV clinics: the experience from the TB/HIV in Rio (THRio) Study . AIDS [Internet]. 2010 Nov [cited 2023 Sep 15];24(Suppl 5):S49-56. https://doi.org/ 10.1097/01.aids.0000391022.95412.a6 PubMed | Google Scholar
- Phalkey RK, Yamamoto S, Awate P, Marx M.Challenges with the implementation of an Integrated Disease Surveillance and Response (Idsr) system: systematic review of the lessons learned . Health Policy and Planning [Internet]. 2013 Dec 20 [cited 2023 Sep 23];30(1):131-43. https://doi.org/10.1093/heapol/czt097 Google Scholar
- Golub JE, Saraceni V, Cavalcante SC, Pacheco AG, Moulton LH, King BS, Efron A, Moore RD, Chaisson RE, Durovni B.The impact of antiretroviral therapy and isoniazid preventive therapy on tuberculosis incidence in HIV-infected patients in Rio de Janeiro, Brazil . AIDS [Internet]. 2007 Jul 11 [cited 2023 Sep 15];21(11):1441-8. https://doi.org/10.1097/2FQAD.0b013e328216f441 PubMed | Google Scholar
- Berhe M, Demissie M, Tesfaye G.Isoniazid Preventive Therapy Adherence and Associated Factors among HIV Positive Patients in Addis Ababa, Ethiopia . Advances in Epidemiology [Internet]. 2014 Jul 22 [cited 2023 Sep 15];2014: 230587. https://doi.org/10.1155/2014/230587 Google Scholar