Descriptive characterization of the cerebrospinal meningitis outbreak in Zamfara State, 2017-18
Ahmad Njidda1,2,&, Ismail Raji1, Sulaiman Lawal1, Hakeem Yusuff1, Evaristus Aniaku1,3, Rabi Usman1,4, Auwal Usman Abubakar1, Jamilu Nikau1,2, Moreen Kamateeka1, Muhammad Shakir Balogun1, Patrick Nguku1
1Nigeria Field Epidemiology and Laboratory Training Programme, 2Department of Public Health, Federal Ministry of Health, Abuja, Nigeria, 3Nigeria Centre for Disease Control, Abuja, Nigeria, 4Department of Public Health, Zamfara State Ministry of Health, Zamfara, Nigeria
&Corresponding author
Ahmad Njidda, Department of Public Health, Federal Ministry of Health, Abuja, Nigeria. ahmad.njidda1@gmail.com
Introduction:
Cerebro-spinal meningitis (CSM) is an epidemic-prone disease characterized by inflammation of the meninges. From epidemiological week 36, 2017 through epidemiological week 21, 2018, Zamfara State reported an outbreak of CSM that affected all the 14 Local Government Areas (LGAs). Therefore, we conducted a descriptive analysis of the outbreak to determine its epidemiology.
Methods:
We line-listed all suspected cases during the outbreak between September 4th 2017, and May 22nd 2018. We described the outbreak in time, place and person and calculated the attack rates by LGA and the age- and sex-specific case fatality rates (CFR).
Results:
A total of 1125 cases were reported with an overall attack rate and CFR of 25.2 cases/100,000 population and 7.6%, respectively. The age-specific CFR was highest among individuals aged 5-9 years (9.7%), while the sex-specific CFR was almost equal in males and females. The epidemiologic curve showed an increasing number of weekly reported cases with several peaks, the highest in week 12, 2018. A clustering of cases was seen in 2 contiguous LGAs, Bungudu and Gusau; while the highest attack rate was recorded in Shinkafi LGA (51 cases/100,000 population). Only 24% of suspected cases had their cerebrospinal fluid collected, and Neisseria meningitidis C accounted for 77.1% of causative agents.
Conclusion:
Zamfara State has experienced an outbreak of CSM. Training health workers and improving their skills on sample collection and treatment protocol will improve profiling of causative agents and outcomes. The use of Vaccines containing serogroup C will help to prevent future outbreaks.
Introduction

Cerebrospinal Meningitis (CSM) is characterized by inflammation of the lepto-meninges caused by microbial pathogens, including viral and bacterial organisms. Neisseria meningitides is of major public health importance as it is responsible for the occurrence of Epidemic Meningococcal Disease (EMD) in the “African Meningitis belt” [1]. It is associated with high mortality of up to 50% if untreated [2], and can be as high as 70% [3]. In treated cases, the fatality rate is usually between 10-15% [4,5]. The disease is highly transmissible during the dry season, causing epidemics, with attack rates higher in children under 15 years [6-8]. It is estimated that over 1.2 million bacterial meningitis cases occur worldwide each year [9]. Between 1991 and 2010, a total of 1 million suspected cases of meningitis occurred in the countries of the meningitis belt, with 100,000 deaths [10]. Each year, an estimated 30,000 cases occur in the belt [11]. Among the 12 serotypes of Neisseria meningitides, serogroup A (NmA) accounts for most of the epidemics in the African meningitis belt, but recently, the incidence of serogroup C (NmC) tends to be on the increase in northern Nigeria probably due to “MenAfriVac” campaign in 2011, which targeted serogroup A only [12,13].
In cases of CSM, all suspected cases that meet the case definition should have cerebrospinal fluid (CSF) taken before antibiotic therapy [
14]. However, few samples are being collected and analyzed in outbreaks in Nigeria [
6,
15,
16].
Nigeria has witnessed major outbreaks of meningitis between 1970 to date, the largest of which was in 1996, with 109,580 cases and 11,717 deaths (CFR= 10.7%) [
17,
18]. In 2016/2017, a total of 14,518 cases were reported with 1,166 deaths (CFR 8.0%) across 26 states. Zamfara State alone reported 7,140 cases (49%), and NmC accounted for 82.7% of identified organisms [
8]. This was the largest outbreak of meningococcal meningitis caused by the serogroup NmC in Nigeria. The Nigeria Centre for Disease Control (NCDC) activated the Emergency Operation Centre (EOC) to coordinate the multi-agency effort in managing the outbreak [
18].
The 2017/18 outbreak started in Magami Ward, Gusau LGA of Zamfara State and spread to involve all the 14 LGAs in the state. We conducted a descriptive analysis of the outbreak to determine its epidemiology.
Methods


Study design
We conducted a descriptive analysis of the cases of cerebrospinal meningitis line listed during the outbreak between September 4th, 2017 and May 22nd, 2018.
Study area
Zamfara State lies within the North-West geo-political zone of northern Nigeria. It lies within Nigeria's meningitic belt, with annual focal outbreaks of meningitis during the dry season from November to April. The state has been experiencing outbreaks of CSM, the last of which was in 2016/17 [
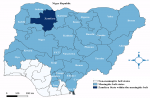
18]. It is bounded by Sokoto, Katsina, Kebbi, Niger and Kaduna States within Nigeria, and shares international boundary with Niger Republic in the north
Figure 1.
The state has a land mass of 35,171 km2 and a population density of 93.2 persons/km2 [
19]. The population of Zamfara State is about 4.9 million people projected from the 2006 census. The state has 14 LGAs. There are 715 health facilities comprising two tertiary hospitals, 23 general hospitals, over 668 PHCs, 150 maternal and child health clinics and 22 private hospitals. These health facilities are manned by 4,746 staff under the health sector, and these are mostly unskilled [
20]. Only 35% of the population have access to medical services, which is higher in urban areas. Leading causes of ill health and deaths include vaccine-preventable and other communicable diseases [
20]. The climatic condition of Zamfara is tropically warm, with temperatures rising to 38�C and above between March and May. The rainy season begins in late May to September, while the cold and dry season starts from December to February, during which the nasopharyngeal mucosa becomes dry and vulnerable to invasion by pathogens[
21].
Case definitions
Suspected case: Any person, from September 4th, 2017 - May 22nd, 2018, with sudden onset of fever and one of the following meningeal signs: neck stiffness, altered consciousness or other meningeal features like Kernig´s sign, Brudzinski´s sign, nuchal rigidity, and raised intracranial pressure including bulging fontanelle in infant.
Probable case: Any suspected case, from September 4th, 2017 to May 22nd, 2018, with cerebrospinal fluid turbid, cloudy or purulent on visual inspection.
Confirmed case: Any suspected or probable case, from September 4th 2017 to May 22nd 2018, that is laboratory-confirmed by culturing or identifying a bacterial pathogen (
Neisseria meningitidis, Streptococcus pneumoniae, Haemophilus influenzae type b) using Pastorex
®, culture or PCR.
Identification of cases
We conducted active case searches in health facilities and communities that reported suspected cases. We line listed cases that met the case definitions. Data on age, sex, residence, date of onset, signs and symptoms and outcome were obtained from cases.
Laboratory diagnosis
Cerebrospinal fluid samples were collected from some suspected cases using spinal needles under aseptic and standard conditions [
14]. Once the suspected cases met the case definition, CSF samples were collected. The aim was to get at least ten samples from each LGA. Due to the inadequate number of skilled manpower to carry out lumbar puncture and also logistic difficulties, only a fraction of suspected cases had CSF collected. About 1 to 2 ml of CSF were collected from each suspected case. The transport media were maintained at cold temperature during transport to the field and warmed to room temperature (25
oC) prior to use. The inoculated media were transported from the health facilities to the state laboratory using vaccine carriers and maintained at room temprature. The samples were handled at Biosafety Level-2 (BSL-2) and tested using Pastorex
®,latex agglutination test kits and confirmed by culture.
Data analysis
We conducted a descriptive analysis of the line-listed cases of cerebrospinal meningitis in Zamfara State between September 4th, 2017 and May 22nd, 2018. We characterized the outbreak in time, place and person using Microsoft Excel 2016. We calculated the median age, and frequencies and proportions of cases by age, sex, and signs and symptoms. For the signs and symptoms, we omitted the cases for whom information on these variables were not captured in the line list from the analysis. The attack rates (AR/100,000) were computed using reported cases and projected population data obtained from the state based on the 2006 population census. The overall CFR, LGA-, age- and sex-specific CFR were calculated using complete clinical information of LGA, age, sex, and outcome. The numerators for LGA-, age-, sex-specific CFR were the number of deaths in the LGA, age group and sex, respectively. While the denominators were the number of cases for the specific variable (LGA, age group and sex) with complete clinical information. All cases on the line list had complete clinical information for these variables.
Ethical consideration
The data on the line list was generated as part of the outbreak response of CSM by the state and national officials as well as the Nigeria Field Epidemiology and Laboratory Training Programme (NFELTP) residents. Due to the exigencies of the outbreak, ethical approval was waived, and permission given to the team to conduct the investigation. All patient records were obtained following informed oral consent, and these were line listed as part of the field data. Patient identifiers were removed to maintain anonymity.
Results


The index case was a 7-year-old from Magami ward, Gusau LGA, whose symptoms began on September 4th, 2017 (Epi week 36), and was seen at Yariman Bakura Specialist Hospital on September 5th. The State Ministry of Health was notified on the 6th of September.
A total of 1,125 cases were reported between September 4th, 2017 and May 22nd, 2018. The median age was 10 years (IQR: 7-15 years), with the age group 5-14 years reporting the highest number of cases, 55.4% (623/1125), followed by the age group 15-24 years, 17.6% (198/1125). The age group
≥45 years had the fewest cases, 1.3% (15/1125)
Table 1.
Majority cases, for whom information on the signs and symptoms were captured, presented with fever 97.8% (846/865), headache 94.3% (816/865), neck stiffness 92.3% (798/865), sensitivity to light 63.4%(548/865) and vomiting 38.7% (335/865)
Table 2.
The overall CFR was 7.6% (85/1125), the age group 5-14 years had the highest CFR of 8.5% (53/623). The CFR in males and females were 7.6% (47/620) and 7.5% (38/505), respectively
Table 3.
Shinkafi LGA had the highest attack rate (AR) of 51.0 per 100,000 population, followed by Bungudu with AR of 44.9 per 100,000 populations, while Maru had the least AR of 2.6 per 100,000 populations. Maradun LGA had the highest CFR of 22.9%
Table 4
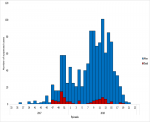
The epidemic curve shows a propagated pattern with several peaks, the first peak was in week 50, 2017 (December 2017) with 43 cases and 15 deaths, and the highest peak was in week 12, 2018 (March 2018) with 93 cases and eight deaths. Thereafter, except for weeks 14 and 15, the cases subsided
Figure 2.
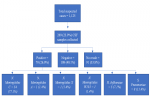
Only about 24% (269/1125) of cases had their samples collected for laboratory analysis, 26% (70/269) were positive.
Neisseria meningitidis C accounted for 77.1% (54/70) of causative organisms
Figure 2.
Discussion


Our descriptive study analyzed an outbreak of cerebrospinal meningitis in Zamfara State. The outbreak started in a ward in Gusau LGA and spread to affect the entire state. The finding that the highest number of cases occurred among those aged 5-14 years is consistent with patterns typically described in meningitis outbreak [6,7,22]. These individuals accounted for the most cases likely because they are of school age, physically active, play more with their peers and share objects among themselves, increasing their risks of exposure and thus coming down with the disease. Also, the carriage rate was found to be highest in adolescents and young adults [23].
Our study showed more males were affected compared to females. This is consistent with similar studies conducted in the past within the same geographical area [
7,
24]. The preponderance of males to females in this study could be explained by the cultural setting. In a typical northern Nigerian setting, males are more likely to play and mix with their peers than females, who are more confined to the home. This increases the male´s opportunity for infection [
25]. The preponderance of males to females is not due to any sex predisposition, and that is why the disease does not overwhelmingly affect males over females. However, a study conducted in the neighbouring Kebbi State on CSM contradicts our findings because 51% of cases were females [
6].
The overall CFR was below the CFR described for well-managed cases in earlier studies [
3-5], and it is almost the same as the CFR of the previous outbreak in the state [
18]. The age group 5-14 years had the highest CFR, perhaps due to the fact that they had the highest number of cases reported.
The disparities in the morbidity and mortality rates among the LGAs could only be explained by the different ways in which the cases may have been managed as well as the prevailing poor housing and other deplorable living conditions.
Only 24% of cases had their CSF collected, and this is typical in most outbreaks of CSM in Nigeria, which reveals low sample collection [
8,
15,
16]. This is due to inadequate or few skilled professionals that can perform a lumbar puncture, especially in areas further from the state capital, Gusau, where fewer samples were collected. These few professionals are often overwhelmed in outbreak settings because they have to cover a wide geographic area to collect samples. This could cause delays in sample collection if at all the samples are collected. A considerable number of these samples had no result returned, probably because they were not processed. Inadequate infrastructure and human resources limit laboratory management of outbreaks [
15].
It is noteworthy that the NmC serotype accounted for the overwhelming majority of all laboratory-confirmed cases. Only one sample was positive for NmA in this outbreak. This has been consistent in recent outbreaks of CSM in Nigeria and other meningitis belt countries. In Nigeria and Niger, especially, NmC appears to be the dominant cause of meningococcal disease in recent years [
26]. The low cases of CSM due to NmA, which have been the predominant causative agent in the past, could be attributed to the impact of vaccination against NmA in Nigeria and other countries in the meningitis belt [
12,
13]. This shift in the epidemiology of the disease could inform a new or improved approach to managing epidemics due to the disease.
Haemophilus influenza and
streptococcus pneumonia accounted for 18.6% of positive samples. This shows an outbreak with possibly mixed pathogenic causes and the low sample collection in this outbreak undermines the accurate profiling of the causative agents responsible for the outbreak.
Many of these results returned as negative, which could be explained by late sample collection and possible initiation of antibiotic treatment before collection.
Conclusion


Outbreaks of CSM due to NmC have replaced NmA in recent years. Training health workers on sample collection and laboratory diagnosis is important for accurate profiling. Vaccination with molecules containing serogroup C will prevent future outbreaks. There is a need to improve and sustain surveillance in the state and also stockpile of supplies to enhance outbreak preparedness.
What is known about this topic
- Meningitis outbreaks in the meningitic belt
- The increasing dominance of NmC as the causative agent of meningococcal disease
What this study adds
- Low sample collections hinder accurate profiling of causative agents
Competing interests


The authors declare no competing interests.
Authors' contributions


Ahmad, Ismail, Suleiman, Hakeem, Evaristus and Rabi participated in the study and data collection, analysis and manuscript writing. Moreen, Muhammad, Patrick, Jamilu and Auwal participated in data analysis and revision of the manuscript. All authors have read and approved the final manuscript.
Acknowledgements


We will like to acknowledge the Zamfara State ministry of health and the Nigeria Centre for Disease Control (NCDC) for allowing us to conduct this investigation. We are grateful to the Nigeria Field Epidemiology and Laboratory Training Programme (NFELTP) for the support provided for this manuscript.
Tables and figures


Table 1: Socio-demographic characteristics of suspected cases of CSM in Zamfara State, 2017-18
Table 2: Sign and Symptoms the cases presented with in Zamafara State, 2017-18
Table 3: Age- and sex-specific CFR of CSM in Zamfara State, 2017-18
Table 4: LGA specific CFR and AR/100,000 population of CSM in Zamfara State, 2017-18
Figure 1: Map of Nigeria showing the meningitic belt states, highlighting Zamfara State within the belt
Figure 2: Reported cases of cerebrospinal meningitis in Zamfara State between epidemiological weeks 36, 2017 and 21, 2018
Figure 3: Flow chart of sample collection, results and causative agents
References


- Obaro SK, Habib AG. Control of meningitis outbreaks in the African meningitis belt. The Lancet Infectious Diseases. 2016 Apr 1; 16(4):400-2. https://doi.org/10.1016/S1473-3099(16)00121-3. Google Scholar
- WHO. Meningococcal meningitis - Key facts. WHO. 2018 Accessed Mar 2018.
- Rosenstein NE, Perkins BA, Stephens DS, Popovic T, Hughes JM. Meningococcal Disease. N Engl J Med. 2001 May 3; 344(18):1378-88.https://doi.org/10.1056/nejm200105033441807 Google Scholar
- Centers for Disease Control and Prevention (CDC). Meningococcal Disease - Epidemiology of Vaccine Preventable Diseases. CDC. 2015. Accessed Mar 2018.
- Robbins JB, Schneerson R, Gotschlich EC, Mohammed I, Nasidi A, Chippaux JP, Bernardino L, Maiga MA. Meningococcal meningitis in sub-Saharan Africa: the case for mass and routine vaccination with available polysaccharide vaccines. Bull World Health Organ. 2003; 81(10):745-50. PubMed | Google Scholar
- Chow J, Uadiale K, Bestman A, Kamau C, Caugant DA, Shehu A, Greig J. Invasive Meningococcal Meningitis Serogroup C Outbreak in Northwest Nigeria, 2015 - Third Consecutive Outbreak of a New Strain. PLoS Curr. 2016 Jul 7; 8.https://doi.org/10.1371/currents.outbreaks.06d10b6b4e690917d8b0a04268906143 PubMed | Google Scholar
- Gana GJ, Badung S, Bunza AU, Gidado S, Nguku P. Outbreak of Cerebrospinal Meningitis in Kebbi state, Nigeria. Ann Ib Postgrad Med. 2017 Jun; 15(1):23-28. PubMed | Google Scholar
- Nnadi C, Oladejo J, Yennan S, Ogunleye A, Agbai C, Bakare L, Abdulaziz M, Mohammed A, Stephens M, Sumaili K, Ronveaux O, Maguire H, Karch D, Dalhat M, Antonio M, Bita A, Okudo I, Nguku P, Novak R, Bolu O, Shuaib F, Ihekweazu C. Large Outbreak of Neisseria meningitidis Serogroup C - Nigeria, December 2016-June 2017. MMWR Morb Mortal Wkly Rep. 2017 Dec 15; 66(49):1352-1356.http://dx.doi.org/10.15585/mmwr.mm6649a3 PubMed | Google Scholar
- Center for Disease Control and Prevention (CDC). Epidemiology of Meningitis Caused by Neisseria meningitidis, Streptococcus pneumoniae, and Haemophilus influenza. CDC. Accessed Mar 2018.
- WHO. Number of suspected meningitis cases and deaths reported. WHO. 2015. Accessed Apr 2018.
- WHO. Meningococcal meningitis. World Health Organization. 2018. Accessed Mar 2018.
- Trotter CL, Lingani C, Fernandez K, Cooper LV, Bita A, Tevi-Benissan C, Ronveaux O, Préziosi MP, Stuart JM. Impact of MenAfriVac in nine countries of the African meningitis belt, 2010-15: an analysis of surveillance data. The Lancet infectious diseases. 2017 Aug 1; 17(8):867-72. https://doi.org/10.1016/S1473-3099(17)30301-8. Google Scholar
- Sambo L, Chan M, Davis S, Lake A, Berkley S, Poonawalla C, Elias CJ. A Vaccine Meets Its Promise: Success in Controlling Epidemic Meningitis in Sub-Saharan Africa. Clin Infect Dis. 2015 Nov 15; 61(Suppl 5):S387-8.https://doi.org/10.1093/cid/civ490 PubMed | Google Scholar
- Nigeria CDC. Preparedness and Response to Cerebrospinal Meningitis Outbreaks. Nigeria CDC. 2017. Accessed Mar 2018.
- Omoleke SA, Alabi O, Usman YB, Ijaya K, Koko AA. Lessons Learnt from Cerebrospinal Meningitis Outbreak Surveillance Data-A Case for Public Health Action. Glob J Health Sci. 2016; 9(2):76.https://doi.org/10.5539/gjhs.v9n2p76 Google Scholar
- Bassey BE, Vaz RG, Gasasira AN, Braka F, Weldegriebriel G, Komakech W, Toritseju MS, Fatiregun AA, Okocha-Ejeko A. Pattern of the meningococcal meningitis outbreak in Northern Nigeria, 2009. Int J Infect Dis. 2016; 43:62-7.https://doi.org/10.1016/j.ijid.2015.12.016 . Google Scholar
- Mohammed I, Nasidi A, Alkali AS, Garbati MA, Ajayi-Obe EK, Audu KA, Usman A, Abdullahi S. A severe epidemic of meningococcal meningitis in Nigeria, 1996. Trans R Soc Trop Med Hyg. 2000; 94(3):265-70.https://doi.org/10.1016/S0035-9203(00)90316-X . Google Scholar
- Hassan A, Mustapha GU, Lawal BB, Na'uzo AM, Ismail R, Womi-Eteng Oboma E, Oyebanji O, Agenyi J, Thomas C, Balogun MS, Dalhat MM, Nguku P, Ihekweazu C. Time delays in the response to the Neisseria meningitidis serogroup C outbreak in Nigeria - 2017. PLoS One. 2018 Jun 19; 13(6):e0199257.https://doi.org/10.1371/journal.pone.0199257 PubMed | Google Scholar
- International Household Survey Network (IHSN). Population and Housing Census 2006, Nigeria: National Population Commission. IHSN 2010. Accessed November 2021.
- SPARC NigeriaHealth Sector Medium Term Sector Strategy 2014 - 2016. SPARC Nigeria. 2013. Accessed November 2021.
- Agier L, Deroubaix A, Martiny N, Yaka P, Djibo A, Broutin H. Seasonality of meningitis in Africa and climate forcing: aerosols stand out. J R Soc Interface. 2012 Dec 5; 10(79):20120814.https://doi.org/10.1098/rsif.2012.0814 PubMed | Google Scholar
- Akhimien MO. An outbreak of Cerebrospinal meningitis in Jigawa state Nigeria 2009. International Journal of Infectious Diseases. 2010 Mar 1; 14:e65.https://doi.org/10.1016/j.ijid.2010.02.1632 . Google Scholar
- Stephens DS. Biology and pathogenesis of the evolutionarily successful, obligate human bacterium Neisseria meningitidis. Vaccine. 2009 Jun 24; 27(Suppl 2):B71-7.https://doi.org/10.1016/j.vaccine.2009.04.070 PubMed | Google Scholar
- Kwambana-Adams BA, Amaza RC, Okoi C, Rabiu M, Worwui A, Foster-Nyarko E, Ebruke B, Sesay AK, Senghore M, Umar AS, Usman R, Atiku A, Abdullahi G, Buhari Y, Sani R, Bako HU, Abdullahi B, Yarima AI, Sikiru B, Moses AO, Popoola MO, Ekeng E, Olayinka A, Mba N, Kankia A, Mamadu IN, Okudo I, Stephen M, Ronveaux O, Busuttil J, Mwenda JM, Abdulaziz M, Gummi SA, Adedeji A, Bita A, Omar L, Djingarey MH, Alemu W, D'Alessandro U, Ihekweazu C, Antonio M. Meningococcus serogroup C clonal complex ST-10217 outbreak in Zamfara State, Northern Nigeria. Sci Rep. 2018 Sep 21; 8(1):14194.https://doi.org/10.1038/s41598-018-32475-2 PubMed | Google Scholar
- Hassabu M. Historical background and epidemiology of cerebrospinal meningitis (CSM). Sudan J Paediatr. 2013; 13(2):115-23. PubMed | Google Scholar
- Mustapha MM, Harrison LH. Vaccine prevention of meningococcal disease in Africa: Major advances, remaining challenges. Hum Vaccin Immunother. 2018 May 4; 14(5):1107-1115.https://doi.org/10.1080/21645515.2017.1412020 PubMed | Google Scholar