Implementation of Intensified Tuberculosis Case Finding among People Living with HIV in Kampala, Uganda: A cross sectional study
David Okello1,&, Angela Nakanwagi Kisakye2,3, Justine Namakula2, Esther Buryegyeya4
1Department of Epidemiology and Biostatistics, School of Public Health, College of Health Sciences, Makerere University, Uganda, 2Department of Health Policy and Planning, School of Public Health, College of Health Sciences, Makerere University, Uganda, 3African Field Epidemiology Network, Kampala Uganda, 4Department of Disease Control and Environmental Health, School of Public Health, College of Health Sciences, Makerere University, Uganda
&Auteur correspondant
David Okello, School of Public Health, College of Health Sciences, Makerere University, Uganda. okellojd@yahoo.com
Introduction:
Intensified Case Finding (ICF) is a cost-effective strategy for tuberculosis (TB) control and improving quality of life however, its implementation by health workers is generally reported as low in Uganda. There is limited information on the level of ICF implementation and the barriers or facilitators to its implementation among public health facilities in Kampala Capital City Authority (KCCA). In this study we determined the level of ICF implementation, facilitators and its barriers in KCCA public health facilities.
Méthodes:
We conducted a cross-sectional study between May-July 2015. We purposively selected six KCCA public health facilities and conducted exit interviews with patients attending Anti-Retroviral Therapy (ART) clinics to assess whether they were screened for TB. In-depth and key informant interviews with health workers were conducted to explore their experiences in implementing ICF.
Résultats:
Overall, ICF implementation was sub optimal. Less than 10% (30/321) clients reported being screened for current cough, fever, weight loss or night sweats. Conversely, 90.0% (289/321) clients screened for at least one TB symptom with cough being the most frequently asked symptom 87.5% (281/321). Of 131 clients who were screened and reported having at least one TB symptom, 36.6% (48/131) were sent to the laboratory, 2.3% (3/131) for X-Ray and 61.1% (80/131) to pharmacy. Training, support supervision, proper coordination, and support from implementing partners were facilitators of ICF implementation. Poor staff attitude, irregular supply of ICF related inputs/materials, high workload, transport and stigma were key barriers to ICF policy implementation.
Conclusion:
ICF implementation at ART clinics in KCCA public health facilities was sub optimal. Health workers� attitude, training, support supervision and stigma of TB clients should be addressed for better ICF implementation.
Introduction

Tuberculosis (TB) remains a major global health problem resulting in an estimated 1.3 million deaths among HIV negative people and an additional 300,000 deaths among HIV positive people [1].
HIV is a vital risk factor for the development of TB with the risk of TB development reported to be more than 20 times greater in people Living with HIV (PLHIV) than those without HIV infection [
2]. According to the World Health Organization (WHO) country specific report (2014) Uganda documented, over 45% of all notified TB cases were among HIV positive patients [
3].
Despite the high proportion of reported TB cases annually in Uganda, case detection rate still remains low at 55.2% compared to the WHO target of 70% and the national target set by the National TB and Leprosy Control Program (NTLP) strategic plan of 65% for 2015 [
4].
Routine TB screening offers an opportunity to diagnose and promptly treat TB disease, and to identify those without TB disease who may be eligible for TB preventive therapy[
4]. Therefore, WHO put emphasis on three I´s that is; Isoniazid Preventive Treatment (IPT), Intensified Case Finding (ICF) for active TB and TB Infection Control (IC), as key public health strategies to decrease the impact of TB on PLHIV [
5].
Intensified case finding for TB involves regular screening of all people living with or at high risk of HIV or in congregating settings (i.e., mines, prisons, military barracks) for signs and symptoms of TB, followed promptly with diagnosis and treatment, and screening of the house hold contacts [
5]. In order to optimize the implementation of ICF policy among PLHIV, in 2008, the Ministry of Health Uganda (MOH) adopted the WHO policy on implementation of ICF where through NTLP they developed a screening form to be administered in health care settings to aid tuberculosis detection among high-risk groups. The ministry of health screening form had four questions for screening TB: Cough (for more than 2 weeks), fevers (for more than 3 weeks), excessive night sweats (i.,e for more than 3 weeks) and weight loss (more than 3 kilograms in one month) and any patient found with any of these symptoms is presumed to have TB and would require further investigation thereafter the positive cases are then enrolled for TB treatment [
6].
Studies have shown that ICF implementation increased the number of identified TB suspects by 6% and newly diagnosed TB cases by 30% and improved TB case detection at a low cost [
7]. However, a study done in Uganda reported low use of ICF tools by health workers [
8].
Though efforts were made by NTLP and partners to strengthen ICF implementation, the level of implementation is not known among KCCA health facilities [
9] and little is known about the feasibility, barriers and facilitators of ICF implementation for TB case detection in KCCA public health facilities. This study therefore sought to determine the level of implementation, facilitators and barriers of ICF implementation in KCCA public health facilities and the proportion of PLHIV attending HIV clinic being screened for TB.
Methods


Study site
This study was conducted in Kampala Capital City Authority (KCCA) Public Health facilities due to the fact that KCCA has the highest TB burden compared to all other districts in Uganda. Kampala district health facilities reported between 18-20 percent of TB cases in the country to the National Tuberculosis and Leprosy Program (NTLP), despite having 5% of the national population [
9]. Six ART clinics of KCCA public health facilities; one HCIV and five HCIIIs were purposively selected for carrying out the study.
Study design
This was a cross-sectional study design employing both qualitative and quantitative methods of data collection.
Study population
For the quantitative component of the study, we conducted interviews with clients exiting ART clinics. Clients who attended ART clinic during the same day of the interview were consecutively selected, their consent was sought before they were interviewed in a separate area to ensure confidentiality. For the qualitative study, we conducted key informants (KIs) and in-depth interviews (IDI). We purposively included health workers who were knowledgeable about intensified case finding and had experience in the screening of clients. These included the clinicians, the in-charges of the ART clinics, TB focal persons, and HIV clients visiting ART clinics who consented to participate in the study.
Sample Size
A sample size of 321 study participants was determined using the Leslie Kish formula (1965), for the quantitative study. The number of patients interviewed at each facility was determined using probability proportionate to size method. This was due to the variation of the number of clients attending ART clinic from different facilities. The number of active clients in ART clinics from each facility was obtained at the time of the visit and the overall total was calculated. The number of active clients in each facility was then divided by the sum of active clients from all the facilities, and then multiplied by the sample size to determine the proportion of clients per facility. Regarding the qualitative component of the study, five in-depth and five key informants´ interviews were conducted one in each health facility to triangulate the information generated with that from the quantitative method. Saturation was reached after the tenth interview.
Data Collection
Four research assistants who were familiar with TB were selected and trained. The questionnaire for quantitative data collection was adopted from Tanzania Ministry of Health and Social Welfare and Denegetu, et al 2014 [
10]. The tools were adjusted to fit the context of the study, the questionnaire was translated to Luganda and back translated to English to ensure that the meaning was not lost hence preserving reliability and validity of the tool. The data collection tools, questionnaires, in-depth interview and key informant guides were pre-tested in a facility that was not part of the study. The data was collected from May-July 2015. Face-to-face interviews with patients exiting the ART clinics were conducted using semi-structured questionnaires. The aim was to assess whether the health workers were implementing the ICF or using information contained in it especially by asking the patients whether they had symptoms of TB as documented in intensified case finding screening form. During face-to-face interviews, clients were assigned anonymous codes and data were collected on clients´ socio-demographics, symptoms screened by health worker and action taken among others.
Key informant and in-depth interviews were conducted with health workers (i.e., In-charges of ART Clinics, TB focal person, clinicians, nurses and community supporters) who were purposively selected. The interviews focused on exploring health workers´ perceptions and experiences on barriers and facilitators of ICF implementation in KCCA. The interviews were also audio recorded in addition to note taking. Five key informants and five in-depth interviews that focused on the enablers and challenges of implementing ICF were conducted.
Data management and analysis
Completed questionnaires were kept and codes were used as identifiers for the interviews. Quantitative data was entered using Epi-data version 3.02 computer software and cleaned before exporting it to STATA 12 for analysis. Univariate analysis was run to obtain baseline characteristics of patients and to determine the current level of ICF implementation; which was the proportion of clients asked by the clinician for all the four TB symptoms during the clinic visits (i.e., cough, fever, night sweats and weight loss)[
10]. The level of ICF implementation was considered as the proportion of clients screened for all the four symptoms of TB in all the six facilities. Cross-tabulation was also done to obtain the proportion of clients screened for each symptom of TB per facility. The data were also analyzed to determine the number of patients reporting at least one symptom, two symptoms or three symptoms of TB and actions that were taken. Logistic regression was performed to determine the factors associated with screening. A client who was asked all the four TB symptoms by a clinician was considered to have been screened. Patients´ characteristics including age, gender, and occupation among others were run against the outcome variable (TB screening). An association was considered significant at P<0.05 and 95% confidence intervals (CI). Variables that had a p value <0.2 at bivariate level and known confounders (i.e. age, gender) were included in the multivariable analysis model to determine independent factors associated with TB screening. Qualitative data from in-depth and key informant interviews were recorded, and later transcribed. Transcription was done while consulting the notes for verification of data. Two peer researchers read through the transcripts to ensure consistency of information hence validating the data in the transcripts. The data were analyzed manually using content analysis. Transcripts from audio recordings were the basis for content analysis. Transcripts were read several times to get a clear understanding of emerging issues that were coded. Similar codes were grouped into categories and later themes were generated from categories. In addition, similar questions were used for both key informants and in-depth interviews. This was majorly for triangulation of data. Qualitative data was used to supplement quantitative data hence helping to explain the facility and individual factors that influenced implementation of ICF for TB case detection.
Ethical approval
We obtained ethical approval from Makerere University Higher Degrees Research and Ethics Committee. Permission to conduct the study was obtained from KCCA Directorate of Environment and Public Health and the Office of the health facility In-charge. Written consent was obtained from the study participants who were 18 years and above. The study participants were given identification numbers for anonymity so that they could not be easily identified by anybody who was not involved in the study. All the information gathered was kept confidential.
Results


Characteristics of study participants
A total of 321 clients was interviewed from six health centers in KCCA. Most 210 (65.42%) of the respondents were females. The mean age of the clients was 35.0 with a standard deviation of 10.30. The clients´ median age was 33 with the interquartile range (IQR) of 28-42. Majority of the clients attained secondary education 135 (42.1%). Kiswa HC III in Nakawa division had the highest number of clients 83(25.9%) while Kisugu HC III in Makindye division had the least number of clients 19 (5.9%). The clients who were screened for TB using at least any one symptom constituted the majority 289 (90.0%)
Table 1.
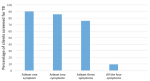
The level of implementation of intensified case finding in KCCA public health facilities
The level of ICF implementation in KCCA public health facilities was 9.4% (30/321). Kawala HC III had 14% (7/50) of the clients screened for all the four symptoms while Komamboga HC III had none of the clients screened for all the four TB symptoms. Kawala HC III also had the highest proportion of clients screened for at least one symptom of TB 96.0% (48/50), while Komamboga HC III had the least number of clients 83.1% (49/59) screened for at least one symptom of TB. All the facilities had ICF implementation below 20% (
Figure 1.
Clients screened for one or more TB symptoms
Over 90% (289/321) of the clients were screened for at least one symptom of TB, 85.7% (275/321) clients were screened for at least two symptoms of TB, and 75.7% (243/321) clients were screened for at least three symptoms of TB, while 9.4% (30/321) clients were screened for all the four symptoms of TB
Figure 2. Cough was the most frequently asked symptom 87.5% (281/321). Kawala HC III in KCCA had the highest level of ICF implementation, with 14% (7/50) clients screened for all the four TB symptoms while Komamboga HC III had the lowest level of ICF implementation with none of the clients screened for all the four TB symptoms
Figure 2.
The symptoms reported by clients and action taken
During the interview, 131 of 321(40.8%) clients reported having at least one symptom of either cough, night sweats, persistent fever or weight loss. Less than a third (36.6%; 48/131) of the clients reported being asked to submit sputum specimen to the laboratory for further investigations, 2.3% (3/131) were referred for chest x-ray while 61.1% (80/131) were sent to the pharmacy for drug refilling hence missed out from further TB investigations
Figure 3.
Factors influencing TB screening among clients
At bivariate analysis, occupation, education level, religion, gender, and age were not statistically significant
Table 2. At multivariable analysis, the clients who were divorced or widowed or separated according to marital status were more likely to be screened for TB compared to clients who were single after adjusting for other factors (AOR=11.4, 95% CI= 2.16-60.30). Also, the clients who were in the age category of 25-34 years were less likely to be screened for TB compared to clients who were in the age category of 18-24 years after adjusting for other factors (AOR=0.11, 95% CI= 0.01-0.92)
Table 2.
The barriers and facilitators to implementation of ICF in HIV clinics in KCCA public health facilities.
Facilitators of intensified case finding implementation
The facilitators were generated based on the emerging issues that were coded and categorized as process and structural factors of the health system as well as individual (i.e., health worker) related factors.
Process facilitators of ICF implementation
Process related facilitators to ICF implementation came from codes generated which included; training, support supervision, support from implementing partners, proper coordination between ART, TB clinic and the laboratory.
Trainings: The majority of the health workers reported that continuous medical education, on job mentorship and continuous quality Improvement trainings organized by the Ministry of Health, KCCA and Implementing partners equipped health workers with knowledge that has enhanced ICF implementation as illustrated in the following quote.>
“�The biggest thing is knowledge, people have the knowledge and we have been able to share with people why we need to diagnose TB and treat TB, how we can control TB so they know why we need to control TB infection, why we need to treat people with TB and follow them up, why we need to screen the people, so really knowledge has helped us because everyone understands the dangers associated with the word TB, so they are able to come up as a team to make sure that the problem is controlled.” (KI_3 HCIV)
Support supervision: The majority of the key informants and in-depth interviews reported that supervision was done by KCCA, implementing partners and the ministry of health was an enabler of ICF implementation.
“�Yes we have got good supervision. We have our medical team coordinator and others that usually come from the ministry she comes at least once in a week to supervise but there are also sometimes a team from the ministry of health comes to mentor us and also to supervise to see whether what they actually recommended is taking root” (KI_1 HCIII)
“�We have supervision by KCCA, we have supervision by ministry of health and then the implementing partners and even in this year we got, I do not know how to call them whether visitors or supervisors from global fund USA, yes and even time and again these implementing partners always come here to see what we are doing and we also have our internal supervision” (KI_4 HCIII)
Support from implementing partners: Implementing partners including; Track TB, Foundation for Innovative New Diagnostics (FIND), and Infectious Disease Institute (IDI)), were reported as enablers to ICF implementation. Many respondents reported that the presence of implementing partners supported health facilities with provision of phones with airtime for calling clients, provision of job aids, provision of ICF screening forms, GeneXpert machine and renovation of some laboratories.
“� I think support from stakeholders has been so key in this. They provided the tent that helped us to keep patients in one place, because initially we didn´t have a tent and controlling the TB patients was not easy because they used to mix with other HIV positive none TB patients. So this has helped us because we can now keep the patients in one place” (KI_1 HCIII).
“�They also provide us with personal protection equipment´s (PPE) like the masks, then also we have a phone that is loaded with the airtime that we use to communicate with the clients, for example if we take off the sputum we send the clients home because we don´t have the GeneXpert, since we don´t have the machine here results usually come back in 24 hours. So we send them home and call them immediately we get the results, so that phone has really helped us” (KI_1 HCIII)
Coordination between ART clinic staff, TB clinic and laboratory
The key informant and in-depth interviewees reported that there was coordination between the units where by in some facilities the presumed clients stay in the tent, while staff take the sputum to the laboratory, other facilities use support staff to guide the clients to the laboratory among others.
“�Everyone is involved it has become a little easier because if we suspect any case of TB we usually give that case to someone to accompany him to the laboratory, they take sputum and that person is taken right away to the isolation tent and they keep there until may be the results come out” (KI_1HCIII).
“�Other units the staffs themselves direct the people here, they escort the clients here and for ICF they put a copy in every unit, yes but in OPD they put there a great number but in units they put few, yes so when any one has the signs of cough they escort the client to TB unit for examination or investigation” (IDI_2 HCIV).
Individual factors related to ICF implementation
Staff Attitude: Staff attitude was reported as being good in some facilities while in other facilities it was still lacking.
“� The attitude used to be bad, but the consequences of the disease have changed people´s attitudes and behaviors towards the management of the disease, so that was history when people didn´t know the management of the disease so when people were taught about the disease, spread, transmission, the management people´s attitude is now changed” (KI_3 HCIV)
“�The attitude is good because they assist us and they know if the patient is not diagnosed he will infect us” (KI_3 HCIV)
Challenges and barriers of intensified case finding implementation
Barriers of ICF implementation included structural or health system related factors such as inadequate staff, irregular supply of ICF related materials and individual related barriers like staff attitude were generated.
Staff attitude: The negative staff attitude was reported as being one of the barriers of ICF implementation in some facilities.
“�Even the health workers´ attitude towards TB is a challenge to ICF implementation, because someone will look at a client and they will not request for TB test because they are thinking this person has TB”. (IDI_4 HCIII)
“� Honestly, I would say the staff (health workers) fear TB, they have a negative attitude towards the TB clinic because ever since that staff caught TB from the clinic she suffered from TB and I don´t know whether she was compensated, so from then they have a negative attitude.´´ (KI_1 HCIII)
Health system related barriers:
The Health system related barriers to ICF implementation such as; irregular supply of ICF related inputs/materials, high workload, transport and sustainability of ICF implementation among others were highlighted.
Irregular supply of ICF implementation related inputs/materials: Many key informants and in-depth interviews reported that inconsistent supply of the ICF screening forms, containers and personal protection equipment like masks was a barrier to ICF implementation.
“�At the moment we don´t have masks you can imagine, frequently we have been running out of containers can you imagine sending the clients away and asking him to come back after two days when we have the containers. These are clients that you won´t send to private settings that you go to such and such a place and do sputum analysis these are the patients that don´t have money.” (KI_1 HCIII)
High workload: Many of the key informant and in-depth interviews reported that they had an overwhelming number of patients. This is still a challenge even after some solutions such as recruitment of additional staff have been provided with support from implementing partners.
“� Yes the workload �, you find that you have many patients” (IDI_3 HCIII).
“�The staff to patient ratio is low and the authorities know about it yet nothing has been put in place” (KI_5 HCIII)
“�We have few staff, or we are understaffed because we don´t have enough people to give time to all these clients”. (KI_1 HCIII)
Transport: Majority of the key informants and in-depth interviewers reported that they encountered challenges in contact tracing because they did not have enough transport to carry out this activity. However, the implementing partners were reported to have been providing assistance in relation to reaching contacts.
“�We have some implementing partners like Track TB and TB REACH they help us reach the families of people who are diagnosed to be having sputum positive TB, they help us contact them but as a facility we can´t access the funds of moving to those families so we ask them to bring the contacts to the facility to be screened.” (KI_3 HCIV)
Sustainability of ICF: Some of the respondents cited fears that the fact that ICF is predominantly reliant on implementing partners whose projects also have a short time frame pauses a serious challenge in relation to sustainability of ICF implementation in KCCA facilities. For instance, the implementing partners such as FIND project, Track TB project among others, employed some staff and provided support for transport and stationary and this support may end with the end of such projects. Respondents expressed doubt that the government would take up such responsibilities.
“�The challenge I find is that when this partner, when this project goes, because almost it is ending in August, who will take on because it´s the person, the staff they recruited who have been doing it and besides the supply of these forms I don´t think KCCA or Ministry of health is willing to print all these forms for each and every patient however, though we have the laminated ones in each and every clinical room but it will not be intense as it has been when this project goes that is my worry” (KI_4 HCIII)
Client related barriers of ICF implementation
Stigma: Many of the key informants and in-depth interviews reported that clients still have stigma. This, according to the respondents, could be the reason why clients keep giving wrong biographical information (wrong address, information, phone numbers and names to the health workers). This in turn makes it challenging for the health workers to do contact tracing and follow up work.
“� But they will even end up giving you wrong information, wrong direction to their homes, thinking you went and told people or when people see you coming out of their place, they will think this person has TB and TB is a death row, so even the clients themselves need more training like TB is treatable” (IDI_4 HCIII)
“� I went to visit this client he told me you come to this place but when I went to that place may be a petrol station to meet with him, when I called the number it was off.” (IDI_2 HCIV)
Discussion


We found that ICF implementation in KCCA was sub optimal with all the selected facilities screening below 20% for all the four symptoms of TB recommended by WHO [3]. The sub optimal level of ICF implementation could be explained by the fact that health workers were putting more emphasis on cough, fever, night sweats symptoms when screening patients and neglecting weight loss symptom which is equally necessary when screening for TB. This undermines the WHO guidelines which recommend screening clients for all the four TB symptoms so that if a patients presents at least any one of the four TB symptom, he/she is presumed to have TB and therefore referred for further investigation [11]. The findings from this study are far different from other studies. For instance a study conducted by Denegetu [10] in Addis Ababa, Ethiopia among people living with HIV at public health facilities found that 92.8% PLHIV were screened for TB during any one of the follow-up visits while Assefa [11] found that between 80% and 95% patients were screened for TB at enrollment and at each three month follow-up visit. The differences of the finding could be explained by the fact that Denegetu´s [10] findings were based on any one of the follow-up visits which was quite different from our study that focused on patients at a particular visit. Assefa [11] also considered screened patients at enrollment and at each three month follow-up visit which was different from the screening that was done at any one of the follow-up visits and at a particular visit as in our study. In addition, this differences could also be due to the fact that health workers do not have adequate time to ask the patient all the four symptoms which is a major challenge experienced in the integration of TB/HIV services [12]. Health workers´ attitude towards TB could also explain why the health workers may not screen patients for all the four TB symptoms. Bulage [13] highlighted that poor health workers attitude and fear of being infected with TB were the key challenges faced by health workers in TB control [13].
Conversely, the proportion of clients screened for at least one symptom of TB in KCCA facilities was high (90%). This however, has implications on ICF implementation because many patients/ clients were missed since they were not screening for all the four TB symptoms. Therefore, the missed clients that had TB, had the potential to spread TB in the facility as well as in the community posing a challenge to the three I´s strategy recommended by WHO to address the TB burden [
5].
The health system related factors that played a critical role in the implementation of intensified case finding, included continuous medical education (CME), on job mentorships and training workshops as well as support supervision. The enablers included support from implementing partners who worked hand in hand with KCCA and ministry of health to build health workers capacity through CMEs, mentorships and trainings. This to some extent partially addressed the attitude of the health workers towards ICF implementation and TB as a disease. A study in Western Uganda revealed that health workers needed more training so as to be able to handle TB and HIV co-infections [
14].
On the other hand, staff attitude, irregular supply of ICF screening forms, workload, and stigma of TB among the clients turned out as key barriers towards the implementation of ICF. Although some of the health workers were reported to have a positive attitude, others were still having a negative attitude towards TB disease and ICF implementation. This could be due to fear of getting TB. These findings also mirror a study that was conducted in Uganda that cited that stock out of drugs/supplies, inadequate space and infrastructure, lack of training, high workload, low staff motivation and poor coordination of health center services were key health system barriers hindering TB evaluation[
15]. In addition, though implementing partners have supported ICF implementation through supplying TB registers, ICF screening forms, and recruiting staff to help in screening, their operations are not sustainable. This calls for KCCA and the ministry of health to have a sustainable strategy towards the ICF program. Furthermore, Clients still have stigma towards TB disease. Most of them considered TB as a death row. Therefore, due to the high levels of stigma, clients gave wrong information about where they stayed, their names, and telephone contacts which also affects follow up. This finding was similar to Osei [
16]who also highlighted that perceived stigma among other factors was associated with delay in diagnosis of TB among TB patients in Hohoe Municipality in Ghana [
16].
Study strength and Limitations
The key informant and in depth interviews with health workers were able to reveal life experiences on the contextual issues experienced by the health workers and produces valuable lessons in ICF implementation. In addition, research assistants were not health workers at the facilities where the study was conducted so as to minimize clients from giving socially desirable answers.
Conclusion


This study identified that implementation of ICF in KCCA public health facilities ART clinics was generally sub optimal. This was mainly due to the fact that health workers did not follow the WHO recommended standards of screening patients for all the four TB symptoms while implementing ICF. In addition, continuous medical education (CME), on job mentorships and training workshops as well as support supervision played a critical role in the implementation of intensified case finding. Conversely, health workers� negative attitude towards TB, and stigma of TB disease among the clients were barriers to ICF implementation. Conducting CME and mentorships helped health workers to acquire knowledge and skills in ICF implementation. Health care workers should put more emphasis on patient counseling and health education to enable patients realize benefits of early TB diagnosis and treatment at individual and community level. This will address clients� negative attitude hence lead to minimized instances of loss to follow up, relapse and continued TB transmission among household contacts and in the community at large.
What is known about this topic
- The study assessed the level of ICF implementation among PLHIV in KCCA public health facilities which was reported to be low among health workers according to the study by Bajwaha [8] which was conducted in Kasese district
What this study adds
- This study explored the various contextual issues on barriers and facilitators of ICF implementation in KCCA public health facilities
Competing interests


The authors declare no competing interests.
Authors' contributions


DO: Conceptualized and designed the study and obtained ethical clearance. He was the principal investigator of the study and led in the writing of the drafts of the manuscript and revised the paper for substantial intellectual content. JNM participated in the review of the draft manuscript and ensured statistical suitability. ANK contributed in scientific editing and critical revision of the manuscript to ensure appropriateness and intellectual content. EB gave professional advice on methodology and analysis of data. She participated in the review of the draft manuscript and updated on current issues in TB research.
Acknowledgements


This study was supported by the German Academic Exchange Service (DAAD) that provided all the financial support. We acknowledge the staff of Makerere University School of Public Health, for their assistance. We also acknowledge Kampala Capital City Authority, Director Environment and Public Health, Manager Clinical services, Health facility in-charges and facility staff. However, the contents of this article are solely the responsibility of the authors and do not represent the views of any organization herein above mentioned.
Tables and figures


Table 1: Characteristics of clients screened for TB symptoms in public health facilities in KCCA, 2015
Table 2: Factors associated with TB screening among PLHIV visiting ART Clinic in KCCA public health facilities, Uganda
Figure 1: Clients screened for at least one symptom and all the four symptoms of TB in KCCA Public Health Facilities, Uganda
Figure 2: Clients screened for TB symptoms in KCCA Public Health Facilities, Uganda
Figure 3: Clients who reported TB symptoms and services provided in KCCA Public Health Facilities, Uganda
References


- WHO. Global Tuberculosis Report 2018. Geneva: World Health Organization. 2018. Accessed Feb 2020. Google Scholar
- World Health Organization. Guidelines for intensified tuberculosis case-finding and isoniazid preventative therapy for people living with HIV in resource-constrained settings. World Health Organization. 2011. Accessed Dec 2021. Google Scholar
- WHO. Global Tuberculosis Report 2013: Country Profiles. WHO. 2014. Accessed Dec 2021.
- Burgess AL, Fitzgerald DW, Severe P, Joseph P, Noel E, Rastogi N, Johnson Jr WD, Pape JW. Integration of tuberculosis screening at an HIV voluntary counselling and testing centre in Haiti. Aids. 2001; 15(14):1875-9.https://doi.org/10.1097/00002030-200109280-00018 Google Scholar
- WHO. Management of tuberculosis and HIV coinfection Clinical Protocol for the WHO European Region (2013 revision). WHO. 2013. Accessed Dec 2021.
- Piatek AS, Van Cleeff M, Alexander H, Coggin WL, Rehr M, Van Kampen S, Shinnick TM, Mukadi Y. GeneXpert for TB diagnosis: planned and purposeful implementation. Global Health: Science and Practice. 2013; 1(1):18-23.https://doi.org/10.9745/GHSP-D-12-00004 . PubMed | Google Scholar
- Hermans SM, Castelnuovo B, Katabira C, Mbidde P, Lange JM, Hoepelman AI, Coutinho A, Manabe YC. Integration of HIV and TB services results in improved TB treatment outcomes and earlier, prioritized ART initiation in a large urban HIV clinic in Uganda. Journal of acquired immune deficiency syndromes (1999). 2012; 60(2):e29.https://doi.org/10.1097/qai.0b013e318251aeb4 . PubMed | Google Scholar
- Bajwaha A. Intensified Case Finding For Tuberculosis Among Patients with Human Immune Deficiency Virus in Kasese District. Uganda: Makerere University; 2013.
- Government of Uganda, MOH. Uganda National Tuberculosis and Leprosy Control Programme Annual Report 2012/2013. Uganda Gov't: Ministry of Health, Programme NTaLC; 2014.
- Denegetu AW, Dolamo BL. Tuberculosis case finding and isoniazid preventive therapy among people living with HIV at public health facilities of Addis Ababa, Ethiopia: a cross-sectional facility based study. BMC public health. 2014; 14(1):52.https://doi.org/10.1186/1471-2458-14-52 . PubMed | Google Scholar
- Assefa D, Melaku Z, Gadissa T, Negash A, Hinderaker S, Harries A. Intensified tuberculosis case finding among people living with the human immunodeficiency virus in a hospital clinic in Ethiopia [Notes from the field]. The International journal of tuberculosis and lung disease. 2011; 15(3):411-3. Google Scholar
- Nansera D, Bajunirwe F, Kabakyenga J, Asiimwe P, Mayanja-Kizza H. Opportunities and barriers for implementation of integrated TB and HIV care in lower level health units: experiences from a rural western Ugandan district. African health sciences. 2010; 10(4). Google Scholar
- Bulage L, Sekandi J, Kigenyi O, Mupere E. The quality of tuberculosis services in health care centres in a rural district in Uganda: the providers´ and clients´ perspective. Tuberculosis research and treatment. 2014; 2014: 685982.https://doi.org/10.1155/2014/685982 . PubMed | Google Scholar
- Wynne A, Richter S, Banura L, Kipp W. Challenges in tuberculosis care in Western Uganda: health care worker and patient perspectives. International Journal of Africa Nursing Sciences. 2014; 1:6-10.https://doi.org/10.1016/j.ijans.2005.001 . Google Scholar
- Cattamanchi A, Miller CR, Tapley A, Haguma P, Ochom E, Ackerman S, Davis JL, Katamba A, Handley MA. Health worker perspectives on barriers to delivery of routine tuberculosis diagnostic evaluation services in Uganda: a qualitative study to guide clinic-based interventions. BMC health services research. 2015; 15(1):10.https://doi.org/10.1186/s12913-014-0668-0 . PubMed | Google Scholar
- Osei E, Akweongo P, Binka F. Factors associated with DELAY in diagnosis among tuberculosis patients in Hohoe Municipality, Ghana. BMC public health. 2015; 15(1):721.https://doi.org/10.1186/s12889-015-1922-z . PubMed | Google Scholar