Addressing Human Resources for Health Needs to Support HIV Epidemic Control: Prioritizing Site-Level Interventions in Democratic Republic of the Congo, 2018-2020
Paul Thurman1,&, Susan Michaels-Strasser2, Luc Ferdinand Kamanga Lukusa3, John Ngulefac4, Beatrice Lukeni5, Serge Matumaini6, Lauren Parmley2, Sungani Zidana-Ndovi7, Faustin Malele6
1Columbia University, Mailman School of Public Health, 722 West 168th St., 4th Floor, New York, NY 10032, USA, 2ICAP at Columbia University, 722 West 168th St., 13th Floor, New York, NY 10032, USA, 3Programme National de Lutte Contre le VIH/SIDA (PNLS), Kinshasa, Democratic Republic of the Congo, 4United States Health Resources and Services Administration, 5600 Fishers Lane, Rockville, MD 20852, USA, 5ICAP at Columbia University, Lubumbashi, Democratic Republic of the Congo, 6ICAP at Columbia University, Kinshasa, Democratic Republic of the Congo, 7ICAP at Columbia University, Lilongwe, Malawi
&Corresponding author
Paul W. Thurman, Columbia University, Mailman School of Public Health, 722 West 168th St., 4th Floor, New York, NY 10032, USA. Paul.Thurman@Columbia.edu
Introduction:
The United States President's Emergency Plan for AIDS Relief (PEPFAR) in Democratic Republic of the Congo (DRC) continues to fund programs aimed at achieving epidemic control in three provinces where 30 percent of people living with HIV/AIDS in the country reside. Challenges around human resources for health impede the delivery of quality HIV/AIDS services in DRC.
Methods:
In partnership with the United States Health Resources and Services Administration (HRSA), PEPFAR, and DRC Ministry of Health (MoH), Columbia University's International Center for AIDS Prevention (ICAP at Columbia University) worked with 16 PEPFAR-identified high-priority health facilities and developed specific interventions to address challenges in achieving PEPFAR 95-95-95 targets. Once interventions were selected and prioritized using a collaborative, criteria-driven approach, implementation of these human resources for health improvements began alongside care and treatment efforts already underway. This study began in October 2018, and high-priority interventions were launched in July 2019. Monthly reporting of key PEPFAR metrics continues for evaluation purposes.
Results:
All 16 high-priority health facilities participated fully. Of several hypothesized interventions, 12 were selected as highest priority, and budgets and task plans were developed for each. The interventions were launched for implementation and evaluation within six months of Ministry of Health approval.
Conclusion:
This assessment delineated necessary interventions to address site-specific human resources for health challenges/deficiencies. Downstream reporting of key PEPFAR 95-95-95 metrics, including Monitoring, Evaluation, and Reporting indicators, will allow intervention teams to conduct program evaluations and their impacts on targets.
Introduction

Democratic Republic of the Congo (DRC) Context and Challenges
Democratic Republic of the Congo (DRC) gained independence in 1960, established its current name in 1997, and has received United States President´s Emergency Plan for AIDS Relief (PEPFAR) funding since 2003 [
1]. DRC is a country of over 2 million square kilometers that borders seven sub-Saharan African countries. Decades of violent conflict and instability have taken a toll on the country´s economy, and, coupled with a largely rural population, present challenges to providing healthcare [
2].
DRC has a generalized HIV epidemic with an estimated prevalence of 1.2 percent among adults aged 15 to 49 years. HIV infection is more prevalent in urban (1.6 percent) than rural settings (0.9 percent). An estimated 404,894 people are living with HIV/AIDS, and around 10,535 people die from AIDS-related conditions each year [
3]. The HIV/AIDS epidemic has drastically impacted two of DRC´s most populous provinces, with population prevalence estimates of 1.6 percent in Kinshasa and 2.6 percent in Haut Katanga [
4].
Columbia University´s International Center for AIDS Prevention (ICAP at Columbia University) initiated comprehensive support of HIV/AIDS care and treatment (C&T) services in DRC in 2010. Since then, ICAP has worked with the Programme National de Lutte contre le SIDA (PNLS) to expand the availability, quality, and uptake of adult and pediatric HIV/AIDS C&T in DRC. Emphasis has been on expanding prevention of mother-to-child transmission (PMTCT) activities, development of a laboratory network for disease monitoring, integration of HIV/AIDS and tuberculosis (TB) services, improvement of infrastructure, prevention among key populations (KP) in Kinshasa and Haut Katanga, and epidemic control. In partnership with DRC Ministry of Health (MoH) and donors, ICAP has rapidly expanded its support for PNLS activities from 10 sites in 2010 to 240 public and private hospitals, health centers, and TB clinics in Kinshasa and Haut Katanga as of September 2014. ICAP currently supports over 200 sites in DRC comprising both PEPFAR and non-PEPFAR funded clinics and health facilities. This paper focuses on efforts to improve support for HRH at 16 PEPFAR-identified “high-priority” health facilities (HFs) in Haute Katanga.
Human Resources for Health (HRH): Priorities and Challenges
Strengthening HRH has been a priority focus of many global public health and epidemic control efforts, especially in African nations [
5]. In DRC, numerous training and policy measures have aimed to address gaps in managing a disparate and diverse healthcare workforce, including nurses, community health workers (CHWs), and midwives, across a geographically and culturally diverse country [
6]. Since healthcare is often centralized at major health facilities in large cities, decentralized efforts to reach DRC´s largely rural population (often with higher infection rates) are constrained by lack of trained health care workers able to provide full HIV/AIDS services [
7]. Further, the abilities of these community staff and HFs to influence local healthcare policies and procedures are constrained by distance, staff burnout, and a sense that rural health services may not “matter” as much [
8]. These challenges can lead to staff feeling underappreciated, burned out, or unclear of job responsibilities and expectations [
9].
For example, in response to the urgent need to increase access to antiretroviral therapy (ART), in close collaboration with the Ministry of Health (MoH) and Nursing Council and Associations, ICAP successfully implemented a PEPFAR-funded program administered by the United States Department of Health Resources and Services Administration (HRSA), the Global Nursing Capacity Building Project (GNCBP), across 10 countries including DRC between 2011 and 2018. HRSA and ICAP partnered with in-country nursing leaders and MOHs and education (MoE) to strengthen the nursing and midwifery workforce.
Epidemic Control and PEPFAR
In support of the Joint United Nations Programme on HIV/AIDS (UNAIDS) 95-95-95 goals, PEPFAR-supported programs place emphasis on activities proximal to reaching these targets and rapid treatment initiation and clinic and community efforts which focus on retention in care and viral suppression. Therefore, central to our investigations were the staffing levels and activities at 16 PEPFAR-identified “high-priority” HFs in Haut Katanga towards achievement of 95-95-95 goals. PEPFAR identified these sites as “high-priority” ones based on the volume of patients on ART, regional HIV/AIDS prevalence, and the likelihood of good collaborations between local ICAP resources and HRSA/PEPFAR-funded facilities. The HIV/AIDS prevalence in Haut Katanga is 2.5 percent compared to 1.2 percent in Kinshasa and is challenged by a largely rural population and large land mass borders with Zambia (HIV/AIDS prevalence of 11.4 percent among adults aged 15-49) and Malawi (10.0 percent among adults aged 15-49 years) [
5,
10].
Resilient and Responsive Health Systems (RRHS) Projects
With PEPFAR funding through HRSA, in 2017, ICAP was awarded the RRHS project to continue strengthening HRH in DRC. Using the World Health Organization (WHO) conceptual framework for HRH development, the first two years of the RRHS project built on extensive HRH capacity building and infrastructure improvements for student nurses and midwives through HRSA funding the Nursing Education Partnership Initiative (NEPI) as a follow-on to the previously funded GNCBP [
11]. During 2018-2020, HRSA and ICAP have leveraged these pre-service strengthening efforts to shift focus to in-service capacity building and addressing wider HRH limitations affecting epidemic control. Improving clinic personnel collaboration, implementing healthcare worker and management training in HIV/AIDS, upgrading infrastructure for HRH, and improving morale and job stability via rural rotations of nurse graduates are all examples of RRHS activities that focus on HRH in DRC.
The value-added of such HRH interventions extends beyond C&T programs and thus may support faster achievement of PEPFAR 95-95-95 goals. These faster outcomes are well-known from prior research as are the pitfalls if such HRH needs are not addressed [
12,
13]. Thus, this paper outlines ICAP´s methods to develop targeted, prioritized, and sequenced interventions–at the HF, MoH, and ICAP levels–to improve HRH effectiveness. With improved HRH effectiveness, ICAP and HRSA hope to demonstrate faster and more efficient achievement of 95-95-95 goals than would have been possible with only C&T interventions, alone [
14].
Methods


A needs-driven process was used to determine site-level HRH needs across the PEPFAR-identified 16 high-priority HRs and to develop efficient action plans to address these needs within 12-18 months. This protocol was submitted to the Columbia University Medical Center Institutional Review Board (IRB) and received a “non-research” determination. A series of 13 steps were completed between October 2018 and June 2019 with HRH interventions launched in July 2019:
- The PEPFAR Rapid Site-Level Health Workforce Assessment (hereafter, “HRH assessment”) was modified and translated into French [
15]. The assessment collected no personal information and focused on challenges that HRH faced, not information regarding daily staffing, etc.
- Ten high-priority sites were selected for survey piloting. Local ICAP staff were trained on the survey and then scheduled initial interviews with HF leaders and staff. All participants were advised that no personal information would be logged and that all responses would be anonymous. Any participant could opt-out of the interview at any time
- Once the ten pilot site interviews were completed, the ICAP team reviewed findings and suggestions for how to improve the survey
- All 16 sites were then interviewed–including re-interviews of the ten pilot sites–with the HRH assessment and presentation of current Monitoring, Evaluation, and Reporting (MER) statistics for each site [
16]
- The team reviewed all data and prepared summaries of key needs from HF interviews.
- The team then assessed patient volumes to determine where excessive patient loads were across the HFs
Figure 1
- From this work the team developed several hypotheses for interventions that could address key HRH needs. These were discussed with the local C&T teams to determine if any findings were duplicated with C&T efforts
- Interventions were then prioritized using a framework with criteria including desirability, feasibility, and time-to-impact [
17]. Priorities were shared with key HF and HRSA leaders for review and comment
- Interventions were then determined to be of short-term focus (within the first six months), medium-term (in months 7-12), or long-term (in months 13-18, or to be completed by December 2020)
- Once agreed, HRH interventions were assigned to be the responsibility of specific sites, all sites, the MoH, or ICAP
- Short-term HRH interventions–including establishing a July 2019 baseline of 95-95-95 MER statistics–were launched
- Concomitant with short-term intervention launch, a tracking tool was developed comprising both C&T and HRH intervention efforts, that aligned efforts with all 95-95-95 targets
- Since mid-2019, monthly reporting of MER data–and of key C&T and HRH intervention progress–has been provided to all in-country leadership and HRSA. Bi-weekly discussions with in-country leaders, ICAP staff, and HRSA leadership are held to assess progress and corrective actions
The collaborative process used focused on building trust with sites and empowering HF leaders to express needs for HRH improvement in ways the team could report back to funders and MoH. Trust-building is especially important when providing financial incentives for performance is impossible and quickly adding qualified staff is unlikely [
18,
19].
The tools developed–and early indicators of HRH effectiveness–would not have been possible without direct, site-level data collection and interviews from HF leaders. By assuring respondents confidentiality of collected inputs, the team was able to obtain honest feedback about key HRH needs. Piloting the process first, and then revising the data collection tool also proved valuable since the team could incorporate learnings from early site interviews to make data collection more effective.
Availability of Data and Materials
The amended rapid assessment survey used and site-level data collected for this study are available from the corresponding author upon reasonable request.
Ethical considerations
The Columbia University Irving Medical Center's IRB reviewed this proposed research study and gave it a “non-research” determination (IRB-AAAS2598) on February 22, 2019. This determination was shared with DRC MoH, and the MoH also deemed this study to be of a “non-research” nature. Only site-level information was retained from interviews, and no specific individuals' names or identifying data were captured as part of any interview or discussion. Although none did, any potential interviewee could opt-out of the site-level interview and/or refrain from completing the amended PEPFAR assessment tool in part or in full.
Results


All 16 high-priority HFs responded in detail to the HRH assessment and participated fully in on-site interviews. Results from the team´s initial data collections indicated that, contrary to initial conjecture, gross staffing level challenges were generally not an issue at the HFs. For the most part, HFs in aggregate were well-staffed for HIV/AIDS care.
An evaluation of HIV/AIDS caseload was performed to determine if appropriate levels of HIV/AIDS-trained staff were in place at each HF, see
Figure 1. While midwives are needed across the board, only four sites (shown in red in the figure) required more HIV/AIDS-qualified health staffing (nurses), and only one site (shown in green) required more doctors and nurses. All others (in blue) were adequately trained and staffed.
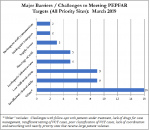
From these analyses, the team concluded that having enough staff was not a key HRH issue and, instead, other needs likely deserved more attention. The team compiled qualitative results from the HF interviews and derived insights into HRH challenges in the HFs
Figure 2
— While few barriers seem to be compensation-related, more HIV/AIDS clinical staff and training may be needed. Low morale seems tied to lack of job descriptions, evaluations, and career pathing
— Staff and managers noted that improvements in morale may lead to better recruiting and employment at HFs [
20]
— Community outreach activities are not well-organized, peer educator staffing is not adequate, and no standard documentation for community health workers exists
— Work environments require improvement–spaces to collaborate, rest, etc.–and workers constantly request more protective clothing and to join/connect to communities of interest to share and learn best practices
— Clinic leaders noted that improved ART distribution would help as would access to more advanced therapies. Budgeting support could also help some HFs according to financial managers [
21]
Discussion


After careful analysis of HF interview data, the team determined that the barriers, above, could be addressed with hypothesized interventions across the following six domains [22]:
Staffing: Increasing clinical hiring and peer educators, and optimizing time allocated to HIV/AIDS patients by these clinical resources
Training: Training CHWs in HIV/AIDS-specific care protocols, improving job descriptions and expectations to enhance morale, and enhancing collaboration and management skills
Workplace Environment: Providing opportunities for, renovating sites, implementing worker protections, and rewarding community involvement and site leadership
Community Outreach: Working to bring more patients into the clinic, increasing screenings, and creating communities of interest to share best practices
Medical Supplies and Equipment: Providing access to advanced drugs and equipment, improving supply chains for ART, and helping sites better budget and report 95-95-95 progress
Monitoring and Evaluation: Standardizing monthly reviews of 95-95-95 progress and collecting ongoing feedback on barriers to HRH effectiveness [
23]
Determining responsible stakeholders for these interventions is critical. Four key stakeholders were then assigned responsibilities for interventions across the six domains, above. Interventions would be implemented by all sites, selected sites, the MoH, and/or by ICAP.
However, not any/every intervention is of the same urgency nor could all hypothesized ones be launched simultaneously. Thus, the team constructed a set of prioritization criteria in order to stage and sequence these interventions in a more manageable way [
24]:
Desirability: Do HFs, MoH, ICAP really
want to pursue this intervention (based on past experience, etc.)?
Feasibility: If the intervention is desirable, do HFs, MoH, ICAP, etc. have the
resources, skills, and
tools ready to kick-off the intervention?
Viability: If stakeholders have the skills and time, do they have the
funding, or can they quickly get it to fund the intervention?
Sustainability: Once implemented, will the HRH interventions
stand the test of time or be lost as one-time changes?
Time to Impact: Finally, if stakeholders implement an intervention, have skills to do it, and can be funded, will they see a return on their efforts based on
meaningful and timely impacts?
After working with HFs, HRSA leadership, ICAP, and MoH, the team prioritized the interventions. Efforts were prioritized in terms of what needed to be implemented in the short-term (within the first six months), over the medium-term (within the following six months), and over the long-term (within the final six months of the total intervention time frame of 18 months). Two short-term interventions had already been initiated by C&T teams
Figure 3.
Based on successes of similar HRH interventions in other sub-Saharan contexts, the team expects to see several improvements [
23]. These are aligned with the major HRH domains mentioned previously:
Staffing: Increase numbers of patients tested for HIV/AIDS and those treated if positive as more qualified health workers, midwives, and peer educators are put into the HRH workforce
Training: Install more staff able to help HIV/AIDS patients, improve satisfaction, and enhance clinic leadership. These should create more awareness for clinics for new and existing cases
Workplace Environment: Improve workplace environments that lead to more team-based care, best practice implementations, and improved morale for staff
Community Outreach: Create wider networks in the community and build trust with clinics. This will increase treated cases, follow-ups, lower viral loads, etc.
Medical Supplies and Equipment: Deploy therapies to patients more quickly and give workers more security via enhanced protective equipment
Monitoring and Evaluation: Place emphasis on achievement of 95-95-95 goals with standard reporting across clinics to implement best practices
To track these expected improvements, a comprehensive reporting system that incorporates both monthly MER data, to track C&T improvements, and the HF interventions noted earlier, was developed. In this way, all stakeholders were able to view monthly progress updates, note where efforts are not meeting desired goals, and see corrective actions being taken to address shortcomings
Figure 4.
The team hopes to use these data to perform future program evaluations to determine intervention- and program-level effectiveness and to show how these efforts have led to better outcomes, as measured by MER reporting, than C&T interventions, alone.
Sustained contact with stakeholders throughout the processes of setting MER baselines and HRH staffing, hypothesizing possible interventions, prioritizing interventions, and launching and tracking implementations allowed the team to keep them aligned and focused on important endpoints. Stakeholders agreed to the major domains of HRH needs, prioritization criteria, and the staged implementation plans. Since launch, stakeholders have appreciated the value of monthly MER reporting aligned with updates that show successes and challenges.
Keeping focus on various stakeholder needs has proven to be valuable as MoH priorities may not always align with HF needs. This, in turn, has built trust across several constituents, all of whom have a vested interest in HIV/AIDS epidemic control through improved HRH staffing, training, and collaboration. But without tracking–of both intervention progress and the direct results of interventions through MER results–any program will likely produce suboptimal or unmeasurable results.
Limitations
Some limitations to this approach are noteworthy. First, only PEPFAR high-priority HFs were interviewed for these targeted HRH interventions. Although the team believes these interventions are relevant to other HFs, the HRH assessment did not compare priority to non-priority sites and has not identified possible divergent HRH needs.
Secondly, given different country contexts in which these interventions may apply, results may vary based on MoH adoption, in-country and external funding, and in-country HRH staffing and skills. The team hopes to pilot this study elsewhere to see if other HFs identify similar HRH needs and can realize similar gains from such interventions.
Conclusion


While the correlation between number of health workers and care outcomes is well documented [25], less evidence exists regarding HRH interventions that go beyond the staffing numbers. Here, the team determined that some HRH needs and challenges, for 16 high-priority PEPFAR HFs in DRC, were not related to staffing levels but to other factors including training, workplace environment, morale, and a need to be connected to other HFs and best practices.
Staffing levels did not appear to be a significant HRH challenge–except for certain needs in certain sites. Getting staff properly trained, connected to each other, and aligned with formal job descriptions could yield significant benefits as measured by MER target achievement and staff morale. Keeping staff trained, on task, and connected appear to be significant drivers of positive culture and therefore help staff work better, together, to improve testing, treatment, and follow-up for those with HIV/AIDS. The team hopes to pilot similar efforts at non-PEPFAR sites, both within DRC and in other countries, and report successes that could not have been achieved with C&T initiatives, alone [
26]. Success of these HRH interventions, then, should be linked to national and regional health policies, and HRH effectiveness can be more of an enabler than a constraint of epidemic control [
27].
What is known about this topic
- PEPFAR funds programs that are aimed at controlling the HIV/AIDS epidemic in areas of Democratic Republic of the Congo where infection numbers are high. However, the delivery of services and human resources for health appear to be impeding HIV/AIDS epidemic control in this country. A review of the extant research literature shows focused efforts on care-and-treatment (C&T) interventions that often support epidemic control efforts; however, few if any studies speak to specific human resources for health (HRH) and site-level interventions that could be implemented in conjunction with these C&T efforts to create more significant improvements and epidemic control that are directly linked to PEPFAR metrics.
What this study adds
- Epidemic control improvements that are C&T-focused coupled with site-level HRH interventions appear to be more effective at effective at HIV/AIDS epidemic control than C&T efforts alone. Further, these HRH site-level interventions can be translated to other domains and geographies with relative ease using both the prioritization and tracking frameworks developed as part of this research. Applying PEPFAR HRH tools at high-priority sites, prioritizing site-level interventions using the framework and evaluative criteria developed by the ICAP team, and implementing a novel tracking system that combines both C&T efforts with prioritized site-level interventions create better and faster epidemic control outcomes as measured by PEPFAR 95-95-95 monitoring and evaluation reporting (MER) statistics.
Competing interests


The authors declare no competing interests.
Funding
Funding for this effort was provided to ICAP at Columbia University through HRSA grant UH6HA30739. John Ngulefac, one of the study's co-authors, is Public Health Analyst, HRSA, and has supervised this funding.
Consent for Publication
The views expressed in this article are those of the authors and should not be construed to represent the positions of HRSA or of the organizations with which the authors are affiliated.
Authors' contributions


PT developed the overall research methodology including interview guides, prioritization frameworks, and intervention plans. SM-S provided background on the PEPFAR, DRC, and HRH contexts and developed a reporting framework for site-level interventions. JN and LFKL contributed to the in-country implementation funding and prioritization. BL and SM provided in-country technical guidance and RRHS leadership (including site-level collaborations). LP provided all strategic information reporting and tracking including MER indicators and site-level intervention evaluation. SZ provided project coordination and communication across New York, Kinshasa, and Lubumbashi teams, and FM provided overall country leadership including ICAP-MoH collaborations and approvals. All authors read and approved the manuscript.
Acknowledgments


The authors wish to thank all study respondents, MoH, PNLS, HRSA, and ICAP leadership and staff for their time and ongoing commitment to HIV/AIDS epidemic control in DRC. The authors also thank Stella M. Lodewick, Glen Ridge High School, Glen Ridge, New Jersey, USA, for her assistance with background research on intervention policy and implementation and for her help organizing our bibliography and citations.
Figures


Figure 1: HIV/AIDS Case Load for High-Priority HFs (as of March 2019)
Figure 2: Major Challenges to Meeting PEPFAR Targets (Across All High-Priority HFs): March 2019
Figure 3: Short-Term Interventions (All Domains) for High-Priority HFs, MoH, and ICAP, May 2019
Figure 4: Site-Level Intervention Tracking Tool (Through November 2019) - MER Indicators and Progress, Only
References


- Wembonyama S, Mpaka S, Tshilolo L. Medicine and health in the Democratic Republic of Congo: from Independence to the Third Republic. Med Trop (Mars). 2007 Oct; 67(5):447-57. Google Scholar
- Messina JP, Emch M, Muwonga J, Mwandagalirwa K, Edidi SB, Mama N, Okenge A, Meshnick SR. Spatial and socio-behavioral patterns of HIV prevalence in the Democratic Republic of Congo. Soc Sci Med. 2010 Oct; 71(8):1428-35.https://doi.org/10.1016/j.socscimed.2010.07.025. PubMed | Google Scholar
- PEPFAR. Democratic Republic of the Congo country operational plan (COP) 2019 strategic direction summary. PEPFAR. 2019. Accessed Mar 2021.
- Ministère de la Sante République Démocratique du Congo. Plan Stratégique Sectoriel Sante de la Lutte Contre le VIH/SIDA 2018-2021. République Démocratique du Congo. 2018. Accessed Mar 2021.
- Herbst CH, Soucat A, Tulenko K. HIV/AIDS and human resources for health. This Changing HIV/AIDS Landscape. Washington DC: The World Bank; 2009. 327p. Google Scholar
- Chopra M, Munro S, Lavis JN, Vist G, Bennett S. Effects of policy options for human resources for health: an analysis of systematic reviews. Lancet. 2008 Feb 23; 371(9613):668-74.https://doi.org/10.1016/s0140-6736(08)60305-0. Google Scholar
- Deussom RH, Rottach E, Prabawanti C, Rahmat E, Rachmawati T, Sirajulmunir N. Health Workforce Assessment in Jakarta for Effective HIV Policy Implementation: Challenges and Opportunities toward Epidemic Control. Jurnal Ekonomi Kesehatan Indonesia. 2019; 3(2).http://dx.doi.org/10.7454/eki.v3i2.2790. Google Scholar
- Brentlinger PE, Assan A, Mudender F, Ghee AE, Torres JV, Martínez PM, Bacon O, Bastos R, Manuel R, Li LR, McKinney C. Task shifting in Mozambique: cross-sectional evaluation of non-physician clinicians' performance in HIV/AIDS care. Hum Resour Health. 2010 Oct 12; 8(1):23.https://doi.org/10.1186/1478-4491-8-23. PubMed | Google Scholar
- Manzi F, Schellenberg JA, Hutton G, Wyss K, Mbuya C, Shirima K, Mshinda H, Tanner M, Schellenberg D. Human resources for health care delivery in Tanzania: a multifaceted problem. Hum Resour Health. 2012 Feb 22; 10(1):3.https://doi.org/10.1186/1478-4491-10-3. PubMed | Google Scholar
- Ministry of Health Zambia, Ministry of Health. Zambia population-based HIV impact assessment (ZAMPHIA) 2016: Final report. Ministry of Health Zambia, Ministry of Health. 2019. Accessed Mar 2021.
- Michaels-Strasser S, Smith J, Khanyola J, Sutton R, Price T, El Sadr WM. Strengthening the Quality and Quantity of the Nursing and Midwifery Workforce: Report on Eight Years of the NEPI Project. Ann Glob Health. 2018 Apr 30; 84(1):31.http://doi.org/10.29024/aogh.6. PubMed | Google Scholar
- Dräger S, Gedik G, Dal Poz MR. Health workforce issues and the Global Fund to fight AIDS, Tuberculosis and Malaria: an analytical review. Hum Resour Health. 2006 Aug 24; 4(1):23.https://doi.org/10.1186/1478-4491-4-23. PubMed | Google Scholar
- Dieleman M, Shaw DM, Zwanikken P. Improving the implementation of health workforce policies through governance: a review of case studies. Hum Resour Health. 2011 Apr 12; 9(1):10.https://doi.org/10.1186/1478-4491-9-10. PubMed | Google Scholar
- World Health Organization. The world health report 2006: Working together for health. 2006. Accessed Mar 2021. Google Scholar
- PEPFAR. PEPFAR 3.0, Human Resources for Health Technical Working Group. PEPFAR rapid site-level health workforce assessment tool, version 1.2. PEPFAR. 2017. Accessed Mar 2020.
- PEPFAR. Monitoring, evaluation, and reporting (MER 2.0) indicator reference guide. PEPFAR. 2017. Accessed Mar 2020.
- Gormley W, McCaffery J, Quain EE. Moving forward on human resources for health: next steps for scaling up toward universal access to HIV/AIDS prevention, treatment, and care. J Acquir Immune Defic Syndr. 2011 Aug; 57:S113-5.http://dx.doi.org/10.1097/QAI.0b013e31821e9320. Google Scholar
- Dovlo D. Using mid-level cadres as substitutes for internationally mobile health professionals in Africa. A desk review. Hum Resour Health. 2004 Jun 18; 2(1):7. https://doi.org/10.1186/1478-4491-2-7. PubMed | Google Scholar
- Mathauer I, Imhoff I. Health worker motivation in Africa: the role of non-financial incentives and human resource management tools. Hum Resour Health. 2006 Aug 29; 4(1):24.https://doi.org/10.1186/1478-4491-4-24. PubMed | Google Scholar
- Bajunirwe F, Twesigye L, Zhang M, Kerry VB, Bangsberg DR. Influence of the US President´s Emergency Plan for AIDS Relief (PEPfAR) on career choices and emigration of health-profession graduates from a Ugandan medical school: a cross-sectional study. BMJ Open. 2013 May 31; 3(5):e002875.https://doi.org/10.1136/bmjopen-2013-002875. Google Scholar
- Callaghan M, Ford N, Schneider H. A systematic review of task-shifting for HIV treatment and care in Africa. Hum Resour Health. 2010 Mar 31; 8(1):8.https://doi.org/10.1186/1478-4491-8-8 . Google Scholar
- Lagarde M, Blaauw D. A review of the application and contribution of discrete choice experiments to inform human resources policy interventions. Hum Resour Health. 2009 Jul 24; 7(1):62.https://doi.org/10.1186/1478-4491-7-62. PubMed | Google Scholar
- Porter LE, Bouey PD, Curtis S, Hochgesang M, Idele P, Jefferson B, Lemma W, Myrick R, Nuwagaba-Biribonwoha H, Prybylski D, Souteyrand Y. Beyond indicators: advances in global HIV monitoring and evaluation during the PEPFAR era. J Acquir Immune Defic Syndr. 2012 Aug 15; 60:S120-6.https://doi.org/10.1097/qai.0b013e31825cf345. Google Scholar
- Wyss K. An approach to classifying human resources constraints to attaining health-related Millennium Development Goals. Hum Resour Health. 2004 Jul 6; 2(1):11.https://doi.org/10.1186/1478-4491-2-11. PubMed | Google Scholar
- Anand S, Bärnighausen T. Human resources and health outcomes: cross-country econometric study. Lancet. 2004 Oct 30-Nov 5;364(9445):1603-9.https://doi.org/10.1016/s0140-6736(04)17313-3. Google Scholar
- Sturke R, Harmston C, Simonds RJ, Mofenson LM, Siberry GK, Watts DH, McIntyre J, Anand N, Guay L, Castor D, Brouwers P. A multi-disciplinary approach to implementation science: the NIH-PEPFAR PMTCT implementation science alliance. J Acquir Immune Defic Syndr. 2014 Nov 1;67:S163-7.https://doi.org/10.1097/qai.0000000000000323. Google Scholar
- Biradavolu M, Deshpande A, Guida M, Kearns M, Trasi R, Wilhelmsen S. Fostering PEPFAR sustainability through leadership, management, and governance. USAID. 2017. Accessed Mar 2021. Google Scholar