Factors associated with Partners Elicitation during HIV Index client´s testing in Dar es Salaam Region, Tanzania
Catherine Gale Gitige1,2,3,&, Gideon Paul Kwesigabo1, Onna Duuma Panga4, Florence George Samizi2, Ahmed Mohamed Abade2, Peter Masunga Mbelele3,5, Rogath Saika Kishimba2
1Muhimbili University of Health and Allied Sciences-Dar es Salaam, Tanzania, 2Tanzania Field Epidemiology and Laboratory Training Program-Dar es Salaam, Tanzania, 3Kibon´goto Infectious Diseases Hospital-Kilimanjaro, Tanzania, 4Regional Health Management Team, Geita 315, Tanzania, 5Nelson Mandela African Institution of Science and Technology, Arusha, Tanzania
&Corresponding author
Catherine Gale Gitige, Kibong´oto Infectious Diseases Hospital (KIDH), Box 12, Mae Street, Lomakaa Road, Kilimanjaro, Tanzania. cathygitige@gmail.com
Introduction:
Identifying people exposed to HIV is critical towards achieving the UNAIDS 90-90-90 goals for HIV epidemic control. The first 90 in Tanzania is at 53% and yet factors for partner's elicitation to HIV care providers are poorly understood. The objective of this study was to determine predictors of partner's elicitation among index HIV positive clients.
Methods:
We conducted a cross-sectional study from January to March 2019 among HIV positive clients diagnosed within the previous 12 months within HIV care and treatment centers in Dar-es Salaam. A structured questionnaire was used to collect the indexes' partner such as including name, type and status of relationship, and location. Participants were asked to choose the preferred approach to notify partners.
Using modified Poisson regression estimate prevalence ratios predictors were determined for variables at p< to 0.05.
Results:
A total of 438 HIV index clients, mean age 37yrs ±11 SD were identified. Of these, 243 (55.5%) provided partners information to HIV Testing and Care (HTC) provider. Predictors for partner elicitation were awareness of notification methods aPR 3.80, 95%CI 2.11-7.01; having privacy at initial HTC visit aPR 3.20 95%CI 1.30-7.40; awareness of partner's HIV status aPR 1.16, 95%CI 1.03-1.30 and having no fear of rejection by partner aPR1.52, 95%CI 1.23-1.88. However, being a female HIV index client was significantly associated with decreased likelihood of partner's elicitation aPR 0.87, 95% CI 0.80-0.95.
Conclusion:
There is a low elicitation rate of exposed partners by index clients. Awareness of notification approaches, confidentiality, having no fear of rejection by partner, and privacy during HTC services contribute to high partner elicitation. Promotion of community awareness on partner's notification approaches and HIV transmission dynamics, and provision of additional support networks for women improve elicitation outcomes are recommended.
Introduction

Human immunodeficiency virus (HIV) and its related acquired immunodeficiency syndrome (AIDS) is still a disease of public health importance. In 2018 for example, 37.9 million people were living with HIV and 1.7 million were newly infected worldwide. A total of 770 000 died from the disease in the same year, withsub-Sahara Africa (SSA) countries carrying over 60% of the burden [1,2]. Despite the fact that HIV/AIDS is incurable, anti-retroviral Therapy (ART) medicines that restore impaired immunity and improve people´s quality of life are available [3]. Unfortunately, efforts to meet the 2020 targets set by the Joint United Nations Programme on HIV/AIDS (UNAIDS) in 2015 that 90% of people should know their HIV status, 90% of them should be kept on ART and 90% of those on ART should achieve HIV viral suppression are clearly off-track [2]. For instance, since 2015, only 79% of people living with HIV knew their status, 62% were on ART and 53% of those on ART had achieved viral suppression globally [2]. In Tanzania the first 90% which is a gateway to treatment stands at 57% well below the UNAIDS target. If efforts are not made to improve the first 90 target, a significant number of individuals will not know their status, and consequently will not be linked to care. This implies that, not only will morbidity and mortality due to HIV/AIDS prevail in Tanzania but also, transmission of HIV in the community will continue unabated.
Modelling studies have cautiously documented that achieving the global 90-90-90 targets by 2020 in sub-Saharan Africa was realistic. However, this is possible if each country can identify and address the specific gaps needing attention along the cascade of care, right from HIV diagnosis, linkage to care and treatment, adequate retention and adherence to care [
4] . The UNAIDS global report shows that over half of new HIV infection commonly occurs among key population and their sexual partners. In African countries, the number of lifetime sexual partners and previous marriage are independent predictors of HIV prevalence [
5,
6]. Delayed diagnosis/case detection, is a core challenge in HIV prevention and care leading to continual transmission of HIV in the community [
7]. One of the approaches recommended by the UNAIDS for increasing HIV case detection is to conduct contact investigation of HIV index people, and link them to HIV testing services [
8]. In HIV endemic settings, mutual disclosure of index persons who test for HIV has been recommended [
9]. Despite this recommendation, Eastern and Southern Africa still account for 45% of the world´s new HIV infections and 53% of people living with HIV globally [
10]. In Tanzania, only 78% of people living with HIV know their HIV status [
10]. Elicitation is a technique used by health care providers to allow HIV positive index clients to agree voluntarily to provide information of their sexual and drug injecting partner(s), so that they can be identified, notified, tested and linked together with their sexual partner into care and treatment [
11]. By doing so, the chain of HIV transmission is interrupted through early referral and treatment initiation [
12]. Partner disclosure has the potential to increase case detection and consequently achieve the target for the first 90 of the UNAIDS goal by 2020 [
10,
13]. The prevalence of partner disclosure varies, for instance in Scotland, 86% of index clients provide their partner´s information to an HIV care provider while in Zimbabwe the figure is 95% [
14,
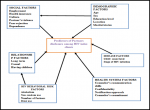
15]. Predictors of index HIV positive persons to disclose their partner personal details include factors such as the number of sexual partners, their lifestyle and voluntary acceptance for contact tracing for their partners by the health service providers. However, these factors are not well studied in resource limited countries like Tanzania. In conducting this study, the analysis of factors influencing naming of exposed partners by the index clients used the following conceptual framework
Figure 1.
This study therefore was conducted with the following objectives: (1) to determine the proportion of HIV index clients who disclose their partners´ information to HIV service providers in Dar es Salaam, (2) to determine the notification approaches preferred, (3) to determine predictors for partner disclosure among index clients and (4) to ascertain barriers to partner naming and locating among HIV index clients in Dar es Salaam.
Methods


Study design and population
This was hospital-based cross sectional study among HIV positive clients who were diagnosed within the previous 12 months. Criteria for inclusion were: HIV index clients who were aged 18 years and above and currently had a sexual or drug injecting partner(s). Exclusion criteria included individuals with language or communication barriers, very sick or hospitalized patients and pregnant women since they had a separate partner notification programme.
Study setting
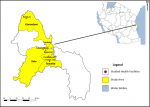
The study was conducted in Dar es Salaam, the largest multicultural city and economic capital of Tanzania. It is located in a quiet bay off the Indian Ocean coast, with a population of over 3 million according to the official 2012 population census. Its residents are mainly business persons whose main economic activities include trade and of recent manufacturing in small scale industries. The city consists of five Municipal councils namely Kinondoni in the north, Ilala in the centre, Ubungo and Temeke in the south and Kigamboni in the east across the Kurasini creek. In 2017, the HIV prevalence in Dar es Salaam was 4.7% (compared to the national average of 5.0%) The city also has the highest prevalence of homosexual and commercial sex work activities in the country. The study was conducted in three municipal councils with high volume of HIV index client´s enrolment in a year. These were Kinondoni, Ilala and Temeke with populations of 1,775,049, 1,220,611 and 1,368,881 respectively as per national population census 2012.
Figure 2.
Sampling
Three municipal councils with high enrollment of HIV index clients were selected from Dar es Salaam region. Two sites from each municipal council were randomly selected from the list through lottery methods. The number of respondents per site were obtained through probability proportional to size (PPS) sampling, in such a way that sites with high volumes of clients, yielded a higher number of clients to participate in the study. At each site, participants were selected using the systematic sampling approach.
Sample size estimates and data collection
The sample size was determined using the Kish-Leslie formula with assumption that index clients would list an average of one sexual partner, and that 50% of index clients would elicit their partners information to an HIV care provider as previously determined [
13]. With a 5% level of precision, standard critical value of 1.96 with 95% confidence interval and after adjusting for non-response rate of 10%, a minimum sample size of 427 participants were calculated.
A tool to assess the index client naming of partners was developed to collect the index and partner´s information among those who consented. In addition to the questionnaire, a data abstraction form for collecting data from the Care and Treatment Centers (CTC) databases was also developed. The data collection tools were pre-tested to ascertain their validity and reliability and in addition, the tools acceptance by the target respondents was also assessed prior to data collection. After obtaining the necessary permissions to conduct the study in the respective CTCs, and after administering the informed consent procedure, exit interviews were conducted individually for each respondent in a confidential way from January to March 2019. For each systematically selected consenting participant satisfying the inclusion and exclusion criteria, information from the face to face interview was complimented by that from the CTC database after abstraction.
Data Management and Analysis
Interviews were conducted by trained Interviewers by filling in the pretested questionnaire. The questionnaires were checked for completeness before conclusion of the interviews and were later cross checked by the field editor to ensure they are properly filled. Partners´ information such as, including name, type and status of relationship, and location was collected. Index clients were asked to choose between self- notification (index client notifies partner alone); assisted notification (index client notifies partner in the presence of a HIV care worker); or health care worker (HCW) alone (health care worker notifies possibility of HIV exposure to partners without revealing the identity of the index client). Data was entered in computers using Epi info version 7.2.2.6 by CDC Atlanta, Georgia (US) with the necessary range, consistency, logical and skip patterns. The data was cleaned and analyzed using both Epi Info 7.2.2.6 and Stata 13 by College Station, Tx:StataCorpLLC. All participants without sexual or drug injecting partners were excluded from the analysis. Confidence Intervals around proportions were calculated using Fleiss Quadratic approximation formula and are reported at 95% level. Following descriptive analysis, generalized linear model with modified Poisson regression was used to estimate prevalence ratio and negative multinomial regression for prevalence ratio. The variables were further subjected to Poisson regression model with negative binomial link robust. The variables with p≤0.05 were regarded as predictors of partner´s disclosure. Social, behavioral and health system factors were analyzed and summarized in Tables 2 and 3. Factors for HIV risk behavior were categorized based on patient´s self-reported sexual orientation as well as their sexual or drug use activities in the previous 12 months.
Ethical Considerations
Ethical clearance with reference.No.DA.287/398/01A/ was obtained from the Muhimbili University of Health and Allied Sciences Research and Publications Ethical Committee. Research permits were obtained from the respective municipal councils and health care facility authorities. The patient data from medical register/CTC databases and charts were accessed after permission from the Hospital Administration and informed consent from the study participants. Confidentiality was secured during the data collection, thus name and addresses of the patient were not recorded in the data collection form or questionnaire and data was kept in safe location. Written informed consent was obtained from willing respondents prior data collection. Interviews were conducted strictly in a private place. Individuals not willing to participate after informed consent were excluded and this did not affect in any way the services they were getting at the CTC.
Results


A total of 482 individuals diagnosed with HIV within the previous 12 months and meeting the recruitment criteria were recruited into the study. Of these, 44 (9%) reported no sexual or drug injecting partners and these were excluded from the analysis. Of the 438 participants included in the analysis, their mean age was 37yrs with a standard deviation of ±11 years, there was a female preponderance at 270 (62%). Of 438 HIV index clients only 243 (55%) participants agreed to give their partners information to HIV counselor, majority of HIV index clients 173 (71%) preferred the passive partner´s notification approach and of these 108 (63%), agreed to share their partner´s information. The index clients were likely to be married, have primary or no education and slightly over half, 248 (57%) were unemployed. Of the female´s indexes, 67 (24%) reported having children aged less than 15 years. Of the index clients interviewed, majority 317 (72%) reported no use of condoms regardless of types of partnership they engaged in. One third 167 (38%) of participants had reported using alcohol in past 12 months. Few engaged in homosexual relationship (MSM) and intravenous drug use in their lifetime 19 (4%) and 33 (8%) respectively, Table 1 and Figure 3 for details. The proportion of partner´s elicitation was at 243 (55.5%). Those who disclosed their partners and yet couldn´t locate their partner´s residential place were 128 (29%).
As indicated above, a total of 243 indexes agreed to provide information to the health care provider about their contacts, the information provided included the partner´s name and address. A total of 570 persons were listed by the index clients which is almost double their number. The HIV status of the listed partners was not determined in this study, this is self reported from interviewed indexes.
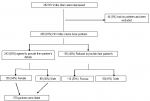
Figure 4 provides the details of the recruitment process and the numbers at each level.
Factors associated with partner elicitation
A number of factors were investigated as to their association with the likelihood of indexes eliciting their partners. Prevalence ratio estimates of partner´s elicitation among HIV index clients indicated that females were 13% less likely to name partners compared to males, (aPR 0.87, 95%CI 0.80-0.95). Single, widowed, divorced, and separated indexes were (borderline) likely to elicit their partners (aPR 1.12,95%CI 0.99-1.27) at p-value 0.056. Those who were aware of their partner´s HIV status (aPR1.16, 95%CI 1.03-1.30), p-value 0.01 and those who did not fear rejection by partner (aPR1.52, 95%CI 1.23-1.88), p-value 0.001 were more likely to elicit partners compared to those who were not aware of their partner´s HIV status or were afraid of rejection by partners
Table 2.
Index clients currently living with their partner(s) (aPR3.65,95% CI 1.50-6.52), at P < 0.001 were more likely to name partners. The index clients who are aware of notification methods were 3.80 times more cooperating in elicitation of partners to the HIV counsellor compared to those unaware of methods of notification aPR 3.8, 95%CI 2.11-7.01). The index clients who are counseled jointly with their partners during initial HIV diagnosis (aPR 1.02 95%CI 0.94-1.11), p-value 0.053 and those who reported HTS services being provided with privacy (aPR 3.20, 95% CI1.30-7.40) were more likely to elicit partners compared to those who did not report as such
Table 3.
Discussion


In this study we have found out that 55.5% of index clients with HIV name their partners. The named partners were double the number of index clients, suggesting that index testing is a favorable strategy for identifying HIV-exposed persons and having them tested particularly in countries with a high prevalence of HIV infection [16]. The identified factors associated with naming partners include: single, widowed, divorced or separated; awareness of partner status, no fear of rejection, currently living with partner, privacy and confidentiality in services and awareness of notification methods. Naming by index partners is generally low as also found in Kenya. This could have been influenced by passive referral notification approaches whereby, the majority of clients opt for passive notification approaches. However, studies in sub-Saharan Africa have found active partner notification to be more effective than passive referral in finding and testing partners for HIV infection [17].
Generally our study sample was predominantly female and married index clients. These findings were in agreement with the study done by Henley et al in Cameroon [
18] who also found out that females and married index clients constituted more than 70% and 53% respectively, implying that women were more likely to be tested for their HIV status than males.
Overall findings showed elicitation of partners were more promising in male compared to female index clients. This is contrary to a study done on gender roles that could have contributed to these findings in sub Saharan Africa [
18]. In our study, more than half of the studied participants agreed to name and provide their partner´s information. The finding is above elicitation rates reported by Song B, et al [
19], but is similar to findings from the WHO report [
8]. These differences could be attributed to the differences in culture and beliefs of the studied populations.
Indexes who are counseled in joint sessions with their partners during the first HIV test were more likely to provide their partners information compared to those counseled individually. This is in agreement with the study [
20] which reported that ongoing counseling that involves partner participatory initiatives right from the beginning increases the likelihood of the HIV index clients to name and locate their partners.
Our study found out that indexes who were single, widowed or divorced were more likely to disclose the names of their partners (although they could not pinpoint their location) to the HIV counselor compared to married or cohabiting persons. This may be due to fear of separation among the married and cohabiting individuals. On the other hand, single indexes may have casual or temporary partners similar to findings from Uganda were it was reported that casual partners are more likely to be named compared to permanent partners [
7]. Similarly, a study done by Myers et al., in Mozambique also revealed that casual partners disclosed their partners´ information than regular partners. This can be explained by trust since causal partners are difficult to trace due to uncertainty [
21].
Types of notification approaches were catalysts to successful index disclosure. In this study, 71% percent of those who agreed to name their partners had opted for the passive notification approach. This is different from findings reported by Wamuti et al., in which provider assisted notification was more preferred by index clients [
22]. This difference may be due to health care providers´ preferences of notification approaches and or unawareness of notification approaches among index clients. On the other hand, our results are in agreement with the study done by Brown et al., [
23] were the studied participants preferred the passive approach to notify their partners for HTC services.
Awareness of notification methods was an independent predictor of partner´s elicitation compared to those unaware of notification methods. More than half of the index clients had opted for the passive method of notification which, matched with the the study in Malawi [
23] that passive notification was the most preferred method by the indexes. This could be attributed to variable HIV counselor communication skills that in some instances could determine which method may be used.
The partner´s disclosure is the strategy towards active case finding among exposed individuals leading to an increased yield of HIV positive individuals who can be linked to care and treatment. In this study it was found out that index partners who are living together with their partners/spouses were less likely to disclose their partner´s compared to those in casual relationships. This could possibly be due to fear of the unknown whereby the index client is not sure of the partner´s reaction when he/she is approached for inclusion into care and treatment following being named by the partner.
The index clients reported having privacy during HIV care as one of the factors associated with an increased likelihood of naming and providing information about the exposed partner compared to lack of privacy. This is in line with the study done that trusting the counselor and having privacy were factors anticipated for successful contacts naming and tracing among HIV partners [
17,
24].
This cross-sectional study provided baseline findings to partner´s elicitation and the notification approaches preferred. The findings need to be evaluated for effectiveness in different settings.
Study limitation
Recall bias for some key variables was minimized by using secondary data from the CTC database. Interviewer bias was minimized by training of the research assistants and ensuring that they adhere to the agreed study protocol, including following the agreed sampling strategies to minimize selection bias.
Much as the predictors of partner´s elicitation were found, temporal relationships could not be established due to the study design that assesses exposure and outcome at the same point in time.
Conclusion


Elicitation of exposed partners by index clients is still low at 55.5%. Awareness of notification approaches, confidentiality and privacy during HTC services contribute to high partner´s elicitation including provision of partner´s information. Other factors associated with an increased likelihood of naming partners included: being single, widowed, divorced or separated, awareness of partner status, lack of fear of rejection and currently living with a partner. Female gender, being married or in a cohabiting type of relationship were associated significantly with low partner´s elicitation.
Recommendations
We recommend promotion of community awareness on partner's notification approaches and HIV transmission dynamics would to improve the level of elicitation. Provision of additional support networks to women could improve elicitation outcomes.
What is known about this topic
- Gender has contribution to HIV partner's notifications services
- High education was associated with failure of elicitation
- Temporary sexual partners are more listed compared to permanent partners
What this study adds
- Long term exposure to HIV counselling will positively influence elicitation
- The clients who are not aware of notification approaches may not cooperate during elicitation of partners hence assisted partner's notification can improve elicitation by index clients
- Partners who are living together are more likely to accept HIV partner's notifications services
Competing interests


The authors declare no competing interests.
Authors' contributions


CG conceived the idea, designed the study, acquired, analyzed data, interpreted the results, as well as drafted the manuscript. AA contributed to idea conception, and also thoroughly reviewed the manuscript and provided the feedback. GK designed and supervised the Study, thoroughly reviewed the manuscript and provided the feedback. PMM, RK OP, FS, interpreted the result, and thoroughly reviewed the manuscript and provided the feedback. All authors read, approved the final manuscript and agreed to be accountable for all aspect of the work.
Acknowledgements


Special appreciation to Tanzania Field Epidemiology and Laboratory Training Program for financial and technical support to conduct this study, Dar es Salaam Regional administration for permission to conduct study, Fellow cohort residents for their constructive ideas.
Tables and figures


Table 1: Socio demographic and behavioral risk characteristics of index case, Dar es salaam Tanzania 2019
Table 2: Independent social predictors of partner´s elicitation among HIV index clients in Dar es Salaam, 2019
Table 3: Behavioral and Health System Predictors of partner´s elicitation among HIV index client in Dar es Salaam, 2019 Multiple Poisson Regression´
Figure 1: Conceptual framework of factors influencing disclosure/naming of HIV index partners
Figure 2: Map showing Dar es Salaam region and the health care facilities from where the study sample was drawn
Figure 3: Demographic Characteristics of the studied population.
Figure 4: Recruitment flow of study participants
References


- Laura Dwyer-Lindgren, Michael A. Cork, Amber Sligar, Krista M. Steuben, Kate F. Wilson, Naomi R. Provost, Benjamin K. Mayala, John D. VanderHeide, Michael L. Collison, Jason B. Hall, Molly H. Biehl, Austin Carter, Tahvi Frank, Dirk Douwes-Schultz, Roy Burstein, Daniel C. Casey, Aniruddha Deshpande, Lucas Earl, Charbel El Bcheraoui, Tamer H. Farag, Nathaniel J. Henry, Damaris Kinyoki, Laurie B. Marczak, Molly R. Nixon, Aaron Osgood-Zimmerman, David Pigott, Robert C. Reiner Jr, Jennifer M. Ross, Lauren E. Schaeffer, David L. Smith, Nicole Davis Weaver, Kirsten E. Wiens, Jeffrey W. Eaton, Jessica E. Justman, Alex Opio, Benn Sartorius, Frank Tanser, Njeri Wabiri, Peter Piot, Christopher J. L. Murray & Simon I. Hay. Mapping HIV prevalence in sub-Saharan Africa between 2000 and 2017. Nature . 2019; 570(7760):189-93.https://doi.org/10.1038/s41586-019-1200-9 . PubMed | Google Scholar
- UNAIDS. Global HIV & AIDS statistics � Fact sheet 2019. UNAIDS. 2019. Accessed July 2021.
- Lu D-Y, Wu H-Y, Yarla NS, Xu B, Ding J, Lu T-R. HAART in HIV/AIDS Treatments: Future Trends. Infect Disord - Drug Targets. 2017; 18(1):15-22.https://doi.org/10.2174/1871526517666170505122800 . Google Scholar
- Estill J, Marsh K, Autenrieth C, Ford N. How to achieve the global 90-90-90 target by 2020 in sub-Saharan Africa? A mathematical modelling study. Trop Med Int Heal. 2018; 23(11):1223-30.https://doi.org/10.1111/tmi.13145 . Google Scholar
- Mtenga SM, Pfeiffer C, Merten S, Mamdani M, Exavery A, Haafkens J, Tanner M, Geubbels E. Prevalence and social drivers of HIV among married and cohabitating heterosexual adults in south-eastern Tanzania: Analysis of adult health community cohort data. Glob Health Action. 2015; 8(1).https://doi.org/10.3402/gha.v8.28941 . PubMed | Google Scholar
- Fagbamigbe AF, Adebayo SB, Idemudia E. Marital status and HIV prevalence among women in Nigeria: Ingredients for evidence-based programming. Int J Infect Dis. 2016; 48:57-63.https://doi.org/10.1016/j.ijid.20105.002 . Google Scholar
- Nichols BE, Götz HM, Van Gorp ECM, Verbon A, Rokx C, Boucher CAB, Van De Vijver DAMC. Partner notification for reduction of HIV-1 transmission and related costs among men who have sex with men: A mathematical modeling study. PLoS One. 2015;10(11):1-15.https://doi.org/10.1371/journal.pone.0142576 . PubMed | Google Scholar
- WHO. Guidelines on HIV self-testing and partner notification: supplement to consolidated guidelines on HIV testing services. Geneva, WHO. 2016 December. PubMed | Google Scholar
- Kababu M, Sakwa E, Karuga R, Ikahu A, Njeri I, Kyongo J, Khamali C, Mukoma W. Use of a counsellor supported disclosure model to improve the uptake of couple HIV testing and counselling in Kenya: A quasi-experimental study. BMC Public Health. 2018;18(1):1-10.https://doi.org/10.1186/s12889-018-5495-5 . PubMed | Google Scholar
- Government of Tanzania under the Ministry of Health, Community Development, Gender, Elderly and Children (MoHCDGEC) and the Ministry of Health (MoH) Zanzibar. Tanzania HIV Impact Survey (THIS 2016-17). MOH, Tanzania. 2017. Accessed July 2021.
- Buhikire K, Voss J, Kigozi J, Nyakato P, Ankunda N, Kalebbo B, Musiitwa M, Muganzi A, Sewankambo NK, Nakanjako D. Reaching the First 90 in Uganda: Predictors of Success in Contacting and Testing the Named Sexual Partners of HIV+ Index Clients in Kiboga District. AIDS Behav. 2018; 22:2458-2467. https://doi.org/10.1007/s10461-018-2137-y. Google Scholar
- Hogben M, McNally T, McPheeters M, Hutchinson AB. The Effectiveness of HIV Partner Counseling and Referral Services in Increasing Identification of HIV-Positive Individuals. A Systematic Review. Am J Prev Med. 2007; 33(Suppl 2):89-100.https://doi.org/10.1016/j.amepre.2007.04.015 . Google Scholar
- Kahabuka C, Plotkin M, Christensen A, Brown C, Njozi M, Kisendi R, Maokola W, Mlanga E, Lemwayi R, Curran K, Wong V. Addressing the First 90: A Highly Effective Partner Notification Approach Reaches Previously Undiagnosed Sexual Partners in Tanzania. AIDS Behav. 2017; 21(8):2551-60.https://doi.org/10.1007/s10461-017-1750-5 . PubMed | Google Scholar
- Noreen Mir, Anne Scoular, Karen Lee, Avril Taylor, Sheila M Bird, Sharon Hutchinson, Anne-Marie Worm, David Goldberg. Partner notification in HIV-1 infection: A population based evaluation of process and outcomes in Scotland. Sex Transm Infect. 2001; 77(3):187-9.https://doi.org/10.1136/sti.77.3.187 . PubMed | Google Scholar
- Mahachi N, Muchedzi A, Tafuma TA, Mawora P, Kariuki L, Semo B, Bateganya MH, Nyagura T, Ncube G, Merrigan MB, Chabikuli ON. Sustained high HIV case-finding through index testing and partner notification services?: experiences from three provinces in Zimbabwe. 2019; 22(Suppl 3): e25321. https://doi.org/10.1002/jia2.25321. PubMed | Google Scholar
- Arielle Lasry, Amy Medley, Stephanie Behel, Mohammed I Mujawar, Meagan Cain, Shane T Diekman, Jacqueline Rurangirwa, Eduardo Valverde, Robert Nelson, Simon Agolory, Achamyeleh Alebachew, Andrew F Auld, Shirish Balachandra, Sudhir Bunga, Thato Chidarikire, Vinh Q Dao, Jacob Dee, L E Nicole Doumatey, Edington Dzinotyiweyi, Eric J Dziuban, K Alexandre Ekra, William B Fuller, Amy Herman-Roloff, Nely B Honwana, Nompumelelo Khanyile, Evelyn J Kim, S Francois Kitenge, Romel S Lacson, Peter Loeto, Samuel S Malamba, André H Mbayiha, Alemayehu Mekonnen, Mirtie G Meselu, Leigh Ann Miller, Goabaone P Mogomotsi, Mary K Mugambi, Lloyd Mulenga, Jane W Mwangi, Jonathan Mwangi, Amassanh A Nicoué, Mtemwa K Nyangulu, Ismelda C Pietersen, Puleng Ramphalla, Chanie Temesgen, Alfredo E Vergara, Stanley Wei. Scaling up testing for human immunodeficiency virus infection among contacts of index patients —20 countries, 2016-2018. Morb Mortal Wkly Rep. 2019; 68(21):474-7.https://doi.org/10.15585/mmwr.mm6821a2 . PubMed | Google Scholar
- Goyette M, Wamuti BM, Owuor M, Bukusi D, Maingi PM, Otieno FA, Cherutich P, Ng´ang´a A, Farquhar C. Understanding Barriers to Scaling Up HIV-Assisted Partner Services in Kenya. AIDS Patient Care STDS. 2016; 30(11):506-11.https://doi.org/10.1089/apc.2016.0151 . Google Scholar
- Henley C, Forgwei G, Welty T, Golden M, Adimora A, Shields R, Muffih PT. Scale-Up and Case-Finding Effectiveness of an HIV Partner Services Program in Cameroon: An Innovative HIV Prevention Intervention for Developing Countries. Sex Transm Dis. 2013 Dec; 40(12):909-914.https://doi.org/10.1097/OLQ.0000000000000032 . PubMed | Google Scholar
- Song B, Begley EB, Lesondak L, Voorhees K, Esquivel M, Merrick RL, Carrel J, Sebesta D, Vergeront J, Shrestha D, Oraka E, Walker A, Heffelfinger JD. Partner Referral by HIV-Infected Persons to Partner Counseling and Referral Services (PCRS) - Results from a Demonstration Project. Open AIDS J. 2012; 6:8-15. https://doi.org/10.2174/1874613601206010008. PubMed | Google Scholar
- Isaac K, Fred N. Factors influencing disclosure of HIV status in Mityana district of Uganda. Afri Heal Sc. 2009; 9(1):26-33. PubMed | Google Scholar
- Myers RS, Feldacker C, Cesár F, Paredes Z, Augusto G, Muluana C, Citao S, Mboa-Ferrao C, Karajeanes E, Golden MR. Acceptability and Effectiveness of Assisted Human Immunodeficiency Virus Partner Services in Mozambique: Results from a Pilot Program in a Public, Urban Clinic. Sex Transm Dis. 2016; 43(11):690-5. https://doi.org/10.1097/OLQ.0000000000000529. Google Scholar
- Wamuti BM, Welty T, Nambu W, Chimoun FT, Shields R, Golden MR, Farquhar C, Muffih PT. Low risk of social harms in an HIV assisted partner services programme in Cameroon. 2019; 22(Suppl 3):e25308.https://doi.org/10.1002/jia2.25308 . PubMed | Google Scholar
- Brown LB, Miller WC, Kamanga G, Kaufman JS, Pettifor A, Dominik RC, Nyirenda N, Mmodzi P, Mapanje C, Martinson F, Cohen MS, Hoffman IF. Predicting partner hiv testing and counseling following a partner notification intervention. AIDS Behav. 2012; 16(5):1148-55.https://doi.org/10.1007/s10461-011-0094-9 . PubMed | Google Scholar
- Hall HI, Holtgrave DR, Maulsby C. HIV transmission rates from persons living with HIV who are aware and unaware of their infection. 2012; 26(7):893-896.https://doi.org/10.1097/QAD.0b013e328351f73f . Google Scholar