Uptake of HIV testing and its associated factors among long-distance truck drivers in Zambia, 2015
Lwito Salifya Mutale1,2,3,&, Mumbi Chola3, Gershom Chongwe3, Webster Kasongo4, David Kasanga Mwakazanga4, Maurice Owiny5, Olufemi Olamide Ajumobi6,7, Choolwe Nkwemu Jacobs3
1Field Epidemiology Training Program, Zambia, 2Ministry of Health, Zambia, 3Department of Epidemiology and Biostatistics, School of Public Health, University of Zambia, Zambia, 4Tropical Diseases Research Center, Zambia, 5African Field Epidemiology Network, Nairobi, Kenya, 6African Field Epidemiology Network Nigerian Country Office, Abuja, Nigeria, 7Nigeria Field Epidemiology and Laboratory Training Programme, Abuja, Nigeria
&Corresponding author
Lwito Salifya Mutale, University of Zambia, Lusaka, Zambia. lwitosalifyanji@gmail.com
Introduction:
Globally, long distance truckers have been reported to have an important role in the spread of sexually transmitted infections (STIs) including Human Immunodeficiency Virus (HIV). Evidence on the uptake of HIV testing among this key population is not well established. We analysed the 2015 Behavioral Surveillance Survey (BSS) data to determine the uptake of HIV testing and assess factors associated with HIV testing among Long Distance Truck Drivers (LDTDs) in Zambia.
Methods:
We analysed secondary data from the 2015 BSS. The BSS was carried out in five of the 10 Corridors of Hope (COH) III project sites (Kazungula, Solwezi, KapiriMposhi, Chipata and Chirundu) among male LDTDs. The Zambian Corridors of Hope HIV and AIDS Prevention Initiative project was formed to address rising rates of HIV and other sexually transmitted infections. The BSS study included LDTDs from truck depots, border sites, Zambia Revenue Authority offices and those parked along the road side. Association between independent variables and history of HIV testing was determined by bivariate logistic analysis. Multivariable logistic regression was done to control for confounders.
Results:
Overall, 1,386 male LDTDs were included in the study, with mean age of 38 years. Over 75% reported being currently married and living with a spouse while 82% reported having only one wife. Uptake for ever having tested for HIV among LDTDs was 83%. Having a relative or friend who was infected or who had succumbed to HIV/AIDS (adjusted OR: 0.61, 95%CI: 0.40 – 0.92) and having two or more wives (adjusted OR: 0.4, 95%CI: 0.2 – 0.6) were independent inhibitory factors for uptake of HIV testing.
Conclusion:
Knowledge of someone infected or died of HIV and having at least two wives were drivers for HIV testing. These findings suggest the need to implement focused Behavioral Change interventions and messages to increase uptake of HIV testing among LDTDs.
Introduction

Long Distance Truck Drivers (LDTDs) have been identified as a group vulnerable to HIV and sexually transmitted infection (STI), making them one of the key populations for STI and HIV controls efforts worldwide [1,2]. Compared with non-mobile male populations in Africa and Asia, LDTDs have a relatively and persistently high HIV prevalence [1,3–5]. This observed pattern could be attributed to the truckers spending extended stays away from home leaving their stable partners behind and inclining them towards risky sexual activity such as sex with commercial sex workers who are strategically focused along the major highway routes [6–8].
HIV testing is one of the critical policy responses to the HIV/AIDS epidemic, principally as a primary prevention strategy and as an entry point to other HIV/AIDS-related services [
9]. While undergoing HIV testing services, individuals learn about their serostatus and become knowledgeable about ways to avoid risky behaviours [
10,
11].
In order to upscale the prevention of HIV transmission and improve Antiretroviral Treatment (ART) client outcomes, Zambia adopted the Joint United Nations Programme on HIV/AIDS (UNAIDS) Fast Track Strategy for HIV AIDS epidemic control in 2030. The UNAIDS Fast Track Strategy aims at ensuring that 95% of all people with HIV are diagnosed, 95% of HIV diagnosed persons receive ART, and 95% of those on ART have achieve and maintain viral suppression by the year 2030 [
12].
Available studies suggest that HIV testing uptake among Long Distance Truck Drivers (LDTDs) remains low. A study done in 2012 by the North Star Alliance, an organisation that runs 35 roadside wellness clinics that provide services to truck drivers on major transit routes in Africa (Kenya, Netherlands, Tanzania, Uganda, South Africa) reported that about 21% of the visits of LDTDs to these clinics resulted in HIV testing despite the fact that testing is offered at every visit [
13]. A survey in South Africa found that 38.2% of the LDTDs had ever been tested for HIV while this was 47.4% in another study in Togo [
14,
15].
A deeper understanding of the factors associated with HIV testing among male LDTDs is essential to reducing HIV transmission in Zambia. However, this is hampered by the lack of evidence on the factors associated with HIV testing among male LDTDs in Zambia. We analysed secondary data from the LDTDs to determine the uptake of HIV testing among male LDTDs in Zambia and asses HIV testing associated factors to inform strategies aimed at HIV/AIDS epidemic control by 2030.
Methods


Study design
We conducted a cross sectional analysis of secondary data from the 2015 Behavioral Surveillance Survey (BSS), whose aim was to evaluate the impact of the Corridors of Hope (COH) project implemented by Family Health International 360 (FHI 360). FHI 360 has implemented the COH and BSS Projects in Zambia targeting female sex workers and their main male clients the LDTD) with behaviour change information and biomedical interventions since 2000. The BSS 2015 was a cross-sectional survey which provided nationally representative data.
The 2015 Behavioral Surveillance Survey
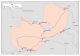
Study sites: Zambia’s major highways run alongside the two major rail routes. Thus, from Livingstone on the southern border with Zimbabwe to Kasumbalesa that borders with Democratic Republic of Congo in northwest of Zambia, and from the inland town of Kapiri Mposhi which is at the junction of the two major railway routes to Nakonde which is the northern border of Zambia with Tanzania. The major trucking border towns are Chirundu, Livingstone, Kazungula, Nakonde and Kasumbalesa and the major internal trucking towns include Lusaka, Ndola, and Kapiri Mposhi. Of the trucking border towns mentioned, the BSS was carried out in five of the 10 COH III project sites in Kazungula, Solwezi, Kapiri Mposhi, Chipata and Chirundu districts, in Zambia (
Figure 1).
Sampling and recruitment
In the BSS, the calculated sample size was 1400 LDTDs [
16]. To get a representative sample of LDTDs, the BSS used places where LDTDs parked, mapped and grouped them into clusters as primary sampling units (PSUs). These sites were along and or near the border sites, truck hubs, Revenue Authority collection points, weigh bridges and rest houses. The total numbers and average number of LDTDs passing through a point over a day and over a week were assessed prior to the study to develop a sampling frame. 20% to 30% clusters were selected depending on the total number of clusters in the sampling frame. Once the clusters were selected, total sample size was proportionately allocated across all the selected clusters. Then size estimation and mapping information gathered were then used to determine the appropriate number of LDTDs to be recruited from each site. Then all eligible respondents were selected for an interview at the selected cluster [
16].
Data collection
In the BSS, data was collected using a pre-tested standardised structured questionnaire. Qualitative data was collected through face-to-face interviews. Any male driver or co-driver aged ≥18years, with a driving license and who had crossed atleast once a year on either one or more country borders, was included during the survey. Exclusion criteria were any male driver aged <18 years at the time of the survey or any truck driver who was aged ≥18years but had previously participated in a similar survey [
16].
Data processing and analysis
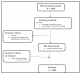
We reviewed data collected from the BSS survey. From the 1406 LDTDs interviewed, we cleaned the data excluding all whose age was <18years and included 1386 LDTDs at analysis stage (
Figure 2). We used HIV testing (drivers who had ever tested and drivers who had never tested) as our outcome variable and we examined explanatory variables such as social - demographics (age, educational level, marital status), length of stay at the site or border, knowledge on HIV and condoms use, number of female sexual partners, ever experienced sexually transmitted diseases, and male circumcision.
Data analysis were performed using STATA software, version 13.0 SE (Stata Corporation, College Station, TX, USA). We described categorical variables using frequencies and percentages and used means and standard deviations to describe continuous variables. We used QQ plots and normal distribution curves to tests for normality for age distribution (continuous variable) of LDTDs. The association between independent variables and the history of HIV testing was determined by bivariate logistic analysis. We carried out stratified analysis to control for confounding and assess for effect modification on age to assess whether HIV testing was different in the two age groups. Variables that had p-values ≤ 0.1 were entered into a model for multiple logistic regression analysis to control for confounding. We removed variables with p-value > 0.05 one at a time until only significant variables were left in the model. We assessed associations between the outcome and independent variables and presented the results using Odds Ratios (OR) at 95% confidence Intervals (CI).
Ethical Clearance
We used ethical clearance obtained for the BSS study from Tropical Diseases Research Centre (TDRC) to obtain a waiver for the analysis of data on HIV testing uptake among male LDTD in Zambia. We obtained permission to use the BSS data from TDRC. The previous interviews which gave rise to BSS data were conducted in secluded private places, with privacy and confidentiality ensured. All data were de-identified to ensure confidentiality and the database was stored in a password- protected computer.
Results


Demographic characteristics of LDTDs
This analysis included 1,386 LDTDs with a mean age of 38 years (Standard Deviation =± 0.2 years). The majority of the drivers were <39 years old and accounted for 53.3% (739/1386) of the participants. While 84.3% (1169/1386) had secondary or higher education, 79.7% (1104/1328) were married and lived with their spouses, and 82.3% (1140/1363) had only one wife. A total of 538 (39%) of participants were circumcised. The main reasons for undertaking circumcision among LDTDs varied, with the majority being circumcised because of traditional and religious beliefs 42% (224/538), followed by 32% (171/538) who were circumcised for health and hygiene purposes. The uptake of HIV testing was 83% (1153/1386) and 81% (568/700) among the overall sampled population and amidst Zambians respectively (
Table 1).
Bivariate analysis of factors associated with HIV uptake among LDTDs
LDTDs who had at least two wives were less likely to have ever tested for HIV compared to their counterparts who had one wife (OR: 0.4, 95%CI: 0.2 – 0.6). Among the 38.8% (538/1372) LDTDs who were circumcised, those whose reason for circumcision was health and hygiene were more likely to be tested for HIV compared to their counterparts whose reason was tradition or religion (OR: 2.4, 95%CI: 1.3 – 4.5). LDTDs whose reason for circumcision was to prevent genital infections were more likely to be tested for HIV compared to their counterparts whose reason was tradition or religion (OR: 2.9, 95%CI: 1.3 – 6.3) (
Table 2).
Age modified the effects of both marital union and having two or more wives being tested for HIV. Among those LDTDs who were aged <40 years, having at least two wives was significantly associated with not having had an HIV test (OR: 0.21, 95% CI: = 0.1 – 0.5). LDTDs who were married and aged <40 years old were 1.9 times more likely to have ever tested for HIV than those who were not married. However, among those LDTDs who were aged ≥40 years and being married, were significantly associated with having ever tested for HIV (OR = 0.3, 95% CI = 0.01 – 2.2) (
Table 3).
Multivariate analysis of factors associated with HIV uptake among LDTDs
The variables that remained statistically significant after multivariable logistic regression included; having two or more wives (adjusted OR 0.45, 95%CI: 0.23 – 0.86) and having a relative or friend who was infected or died of HIV (adjusted OR 0.61, 95%CI: 0.40 – 0.92) (
Table 4).
Discussion


This analysis provides information on uptake of HIV testing (defined as having ever tested for HIV) and associated factors among male long-distance truck drivers in Zambia. Our analysis found that 81% of the Zambian LDTDs had ever tested for HIV. This high testing rate can be attributed to the many interventions that the government of Zambia has put in place, of which the Corridors of Hope HIV/AIDS Prevention Initiative (COH III) could be one of them. The COH III aims to reduce the spread of HIV in high prevalence border and transportation corridor to provide comprehensive HIV and AIDS prevention services. Although our analysis found that those who had ever tested for HIV among LDTDs in Zambia was high, the proportion did not meet the national target of 95% [12]. The HIV testing among LDTDs in our data analysis is higher in comparison with what has been found in earlier studies. A study done in South Africa found that only 38.2% had ever been tested for HIV [14]. Another study done in Togo in 2012, shows that only 47.4% had ever tested for HIV [15].
Interestingly in our analysis, we found that LDTDs with two or more wives were at a reduced likelihood of having an HIV test done compared with truckers who had only one wife. This may be because having multiple sexual partners makes one unsure of their health situation since faithfulness in the relationships is not guaranteed, hence the unwillingness to go for an HIV test for fear of a positive result. Further analysis showed that the association between HIV testing and the number of wives was modified by age: LDTDs who are in polygamous union and are ≥40years, their likelihood of taking an HIV test was very low. Within marital union, intervention should be targeted at encouraging ≥40years LDTDs with at least two or more wives for uptake of HIV testing.
Our study shows that the association between HIV testing and marital status was modified by age. Married LDTDs <40years (irrespective of whether they have one or more wives) are likely to be tested. This finding, strengthens initial findings and intervention should be targeted at single LDTDs especially <40 years old for uptake of HIV testing because they might have a low HIV risk perception. The finding could be because younger single LDTDs were unable to judge risk appropriately and had strong beliefs in their invulnerability to acquiring HIV. Hence reason why at crude analysis there is an association between being single reduced the chance for HIV testing.
Our analysis showed that LDTDs who reported having a relative or having known any friend who was infected or had died of HIV had a reduced chance of taking an HIV test. This finding shows that knowing someone being sick or dying of HIV reduced the likelihood of one taking an HIV test; this could be attributed to one having a fear of testing because of having prior knowledge of the seriousness of the disease. However, due to paucity of studies done on this particular group, we are unable to compare with finding from other studies.
Our analysis, at bivariate analysis found that knowing the benefits of circumcision like enhancing health and hygiene and prevention of genital infections increased the chances of having an HIV test among LDTDs. This finding could mean that creating awareness and highlighting the important benefits of circumcision services among LDTDs would lead to further increase in the uptake of the HIV service in general. Our findings were consistent with those of previous studies [
17–20]. These studies highlight the importance of counselling occurring alongside male medical circumcision which encourages the uptake of HIV services. However, this finding was not significant in multivariable analysis.
Our analysis of available data had some limitations in that, it was looking at ever tested and not tested in the past year. Another limitation was that the BSS data used was unable to collect certain information on some variables mentioned in literature such as tribe, stigma, income and health system barriers. Self-reported information could have led to bias. The low consumption of alcohol could be attributed to self-reporting by the respondents, which would result in an increased chance of underreporting in the study causing the true odds ratios to be higher than what is. However, we believe that the limitations did not adversely affect the final outcome of the study as the findings are useful for HIV programming activities for LDTD such as addressing barriers towards HIV testing among LDTD.
Our analysis shows that being married, having a reason for circumcision being health and hygiene, having a reason for circumcision to prevent genital infections were positively associated while having more than two wives and having a relative or friend who was infected or died of HIV were negatively associated with HIV testing uptake.
Conclusion


Our analysis found high HIV testing rate among LDTDs in Zambia, not far from the national testing target for the country. We found inhibitory factors for HIV testing among LDTDs such as having two or more wives and having a relative or friend who was infected or died of HIV.
We, therefore, recommend implementation of focused behavioural change education and messages to increase knowledge on the importance of HIV testing. This would lead to reduced self-stigma or fear of trial because of knowing someone who was infected or died of HIV. Lastly because of the new testing option that have become available after the BSS study of 2015, we recommend that emphasis be made on education about new testing options (such as use of self-testing kits)
Public Health Action
We presented the results of our study at an HIV stakeholder forum, during the Zambia´s 8th Health Research and 12th Annual HIV Technical Conference.
Declarations
The findings and conclusions in this paper are those of the authors
Ethics
All study activities were approved by the TDRC Ethics Review Committee (FWA 00003729). During the actual survey, confidentiality of information given to participants was assured and maintained throughout the analysis.
Competing interests


The authors declare that they have no competing interests.
Authors’ contributions


LSM, MC, CJ, GC and WK designed the study. LSM performed data analysis and writing of the manuscript. MC, CJ, GC, DM, MO and OA guided the analysis and interpretation of data, and critically revised the manuscript. All authors read and approved the final manuscript.
Availability of data and materials
The datasets used and/or analysed during the current analysis are available from the corresponding author on reasonable request
Acknowledgements


We would like to express gratitude to TDRC for affording us the BSS, without which this paper would not have been possible. Staff of the Zambia Field Epidemiology Training Program deserve appreciation for support given during the whole process of working on this study.
Tables and figures


Table 1: Social-demographic characteristics of long distance truck drivers, Zambia 2015
Table 2: Factors associated with HIV testing among truck drivers, in Zambia - Bivariate analysis (N= 1386)
Table 3: Association between HIV testing, number of wives and marital status, stratified by Age group among LDTDs in Zambia
Table 4: Factors associated with HIV testing among male long distance truck drivers - Multivariable analysis
Figure 1: Map of Zambia showing the five 5 BSS Study sites
Figure 2: Flow Chart Showing Number of LDTDs from Data Collection to Analysis Stage
References


- Gibney L, Saquib N, Metzger J. Behavioral risk factors for STD/HIV transmission in Bangladesh's trucking industry. Social Science and Medicine. 2003;56(7):1411-24. https://doi.org/10.1016/S0277-9536(02)00138-7 Google Scholar
- Atilola G.O, Akpa OM, Komolafe I.O.O. HIV/AIDS and the long-distance truck drivers in south-west Nigeria: a cross-sectional survey on the knowledge, attitude, risk behaviour and beliefs of truckers. J Infect Public Health. 2010;3(4):166-78. https://doi.org/10.1016/j.jiph.2010.08.002 Google Scholar
- Dude A, Oruganti G, Kumar V, Mayer KH, Yeldandi V, Schneider JA. HIV Infection, Genital Symptoms and Sexual Risk Behavior among Indian Truck Drivers from a Large Transportation Company in South India. J Glob Infect Dis. 2009;1(1):21-8. https://doi.org/10.4103/0974-777X.52977 PubMed | Google Scholar
- Pandey A, Benara SK, Roy N, Sahu D, Thomas M, Joshi DK, et al. Risk behaviour, sexually transmitted infections and HIV among long-distance truck drivers: a cross-sectional survey along national highways in India. AIDS. 2008;22:S81-S90. https://doi.org/10.1097/01.aids.0000343766.00573.15 Google Scholar
- Rakwar J, Lavreys L, Thompson ML, Jackson D, Bwayo J, Hassanali S, et al. Cofactors for the acquisition of HIV-1 among heterosexual men: prospective cohort study of trucking company workers in Kenya. AIDS. 1999;13(5):607-14https://doi.org/10.1097/00002030-199904010-00010 Google Scholar
- Essuon AD, Simmons DS, Stephens TT, Richter D, Lindley LL, Braithwaite RL. Transient Populations: Linking HIV, Migrant Workers, and South African Male Inmates. Journal of Health Care for the Poor and Underserved. 2009;20(2):40-52. https://doi.org/10.1353/hpu.0.0157 Google Scholar
- García PJ, Fazio B, Bayer AM, Lizarraga AG, Chiappe M, La Rosa S, et al. Sexual health knowledge and practices and STI/HIV prevalence among long-distance truck drivers in Peru. SAGE Open Medicine. 2017;5:205031211774630. https://doi.org/10.1177/2050312117746308 PubMed | Google Scholar
- Sawal N, Hans GDR, Verma G. Sexual practices, myths and misconceptions among long distance truck drivers in North India. QJM. 2016;109(7):467-72. https://doi.org/10.1093/qjmed/hcv205 Google Scholar
- Denison JAD, McCauley AP, Dunnett-Dagg WA, Lungu N, Sweat MD. The HIV testing experiences of adolescents in Ndola, Zambia: do families and friends matter? AIDS Care. 2008;20(1):101-5.https://doi.org/10.1080/09540120701427498 Google Scholar
- World Health Organization. Increasing Access to HIV Testing and Counselling: Knowing your HIV status – the first step to accessing care and preventing further infection.WHO. 2003. Accessed November 2018.
- Federal Ministry of Health, Nigeria. National HIV/AIDS and Reproductive Health Survey, 2007 (NARHS Plus). Federal Ministry of Health Nigeria. 2008. Accessed November 2018.
- Elizabeth Glaser. UNAIDS Issues New Fast-Track Strategy to End AIDS by 2030. Elizabeth Glaser Pediatric AIDS Foundation. 2014. Accessed November 2018.
- The North Star Alliance. Annual Overview, 2012. The North Star Alliance. 2012. Accessed November 2018.
- Delany-Moretlwe S, Bello B, Kinross P, Oliff M, Chersich M, Kleinschmidt I, et al. HIV prevalence and risk in long-distance truck drivers in South Africa: a national cross-sectional survey. Int J STD AIDS. 2014;25(6):428-38. https://doi.org/10.1177/0956462413512803 Google Scholar
- Yaya I, Landoh DE, Saka B, Vignikin K, Aboubakari A-S, N'dri KM, et al. Consistent Condom Use during Casual Sex among Long-Truck Drivers in Togo. PLOS ONE. 2016;11(4):e0153264. https://doi.org/10.1371/journal.pone.0153264 PubMed | Google Scholar
- FHI360 (Family Health International), Tropical Diseases Research Centre (TDRC). Integrated Biological and Behavioural Surveillance Survey (IBBSS) among Female Sex Workers and Behavioural Surveillance Survey (BSS) among Male Long Distance Truck Drivers in Five Corridors of Hope Project District Sites in Zambia. FHI360 and USAID. 2015. Accessed November 2018.
- Grund JM, Hennink MM. A qualitative study of sexual behavior change and risk compensation following adult male circumcision in urban Swaziland. AIDS Care. 2012;24(2):245-51. https://doi.org/10.1080/09540121.2011.596516 Google Scholar
- L'Engle K, Lanham M, Loolpapit M, Oguma I. Understanding partial protection and HIV risk and behavior following voluntary medical male circumcision rollout in Kenya. Health Educ Res. 2014;29(1):122-30. https://doi.org/10.1093/her/cyt103 PubMed | Google Scholar
- Fiellin DA, O'Connor PG, Wang Y, Radford MJ, Krumholz HM. Quality of Care for Acute Myocardial Infarction in Elderly Patients with Alcohol-Related Diagnoses. Alcoholism: Clinical and Experimental Research. 2006;30(1):70-5. https://doi.org/10.1111/j.1530-0277.2006.00001.x Google Scholar
- Clark RE, Weir S, Ouellette RA, Zhang J, Baxter JD. Beyond Health Plans: Behavioral Health Disorders and Quality of Diabetes and Asthma Care for Medicaid Beneficiaries. Medical Care. 2009;47(5):545-52.https://doi.org/10.1097/MLR.0b013e318190db45 Google Scholar