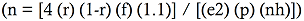Prevalence of non-fatal injuries and associated factors in Mbarara Municipality, Western Uganda, December 2016-June 2017
Rebecca Nuwematsiko1,&, Angela Nakanwagi Kisakye1,2, David Musoke1, Delia Bandoh3, Lillian Bulage4, Olufemi Olamide Ajumobi5,6, Frederick Oporia1, Fiston Muneza1, Nino Paichadze7, George Pariyo8, Abdulgafoor Bachani8, Olive Kobusingye1, Kenneth Mugwanya1, John Ssempebwa1
1Makerere University School of Public Health, College of Health Sciences, Kampala, Uganda, 2African Field Epidemiology Network, Kampala Uganda, 3Ghana Field Epidemiology and Laboratory Training program, Accra, Ghana, 4Public Health Fellowship Program/African Field Epidemiology Network, Kampala, Uganda, 5Nigeria Field Epidemiology and Laboratory Training Program, Abuja, Nigeria, 6African Field Epidemiology Network Nigeria Country Office, Abuja, Nigeria, 7Milken Institute School of Public Health, George Washington University, Washington, DC, USA, 8Johns Hopkins International Injury Research Unit, Department of International Health, Johns Hopkins University Bloomberg School of Public Health, Baltimore MD, USA
&Corresponding author
Rebecca Nuwematsiko, Makerere University School of Public Health, College of Health Sciences, New Mulago Hill Hospital Complex, P.O Box 7072, Kampala, Uganda,
Email: beckyrich123@gmail.com
Background:
Injuries are a significant public health problem but poorly quantified especially in low and middle-income countries. In Uganda, the burden of injuries is poorly quantified with most of the data reported being facility and mortality based. Many non-fatal injuries, therefore, remain unreported in communities. We conducted a household survey in Mbarara Municipality to identify and describe all non-fatal injury events and the associated factors.
Methods:
We conducted a cross-sectional study of non-fatal injuries among 966 household members in Mbarara Municipality, from May to June 2017. The most recent non-fatal injury (within a six-month recall period; December 2016 to June 2017) resulting in loss of at least one day of usual daily operating activity was considered. We conducted a descriptive statistical analysis to estimate the counts and frequencies of non-fatal injuries. We identified factors associated with non-fatal injuries using a modified Poisson regression model.
Results:
The prevalence of non-fatal injuries was 18.2% (176/966) with 92% (162/176) of the non-fatal injuries being unintentional. Falls 27.3% (48/176) were the most common cause of injury followed by road traffic injuries (RTI), 26.7% (47/176), burns 16.5% (29/176) and the least being poisoning 2.8% (5/176). Occupation as casual laborer (Adjusted PR=2.1, 95% CI: 1.2 - 3.7), urban residency (Adjusted PR=1.5, 95% CI: 1.1 - 1.9) and being a non-native of the study area (Adjusted PR=1.7, 95% CI: 1.3 - 2.3) were independently associated with non-fatal injuries.
Conclusion:
Almost one out of five people had suffered a non-fatal injury in the past six months in Mbarara Municipality. Majority of the non-fatal injuries were unintentional, caused by falls and RTIs, and were amongst casual labourers and urban residents. These findings reveal a gap in injury prevention in Uganda that needs to be addressed to improve the quality of life.
Introduction

Injuries and the resulting disabilities are a significant but poorly quantified public health problem, especially in low- and middle-income countries [1]. An injury is a bodily lesion at the organic level, resulting from acute exposure to physical agents such as mechanical energy, heat, electricity, chemicals, and ionising radiation interacting with the body in amounts or at rates that exceed the threshold of human tolerance [2]. Injuries often result from road traffic crashes, falls, burns, poisoning, animal bites, cuts and violence [3].
Globally, 4.8 million deaths occur each year from injuries with 973 million more people sustaining non-fatal injuries [
1]. In 2015, injuries contributed to 10% of all disability adjusted life years (DALYs) lost in Africa, with road traffic injuries (RTIs) contributing the greatest burden [
4]. In Uganda, injuries are the 10th leading cause of DALYs with RTIs, burns, falls, drowning, and inter-personal violence being the most prevalent [
4]. In 201
5, injuries in Mbarara District contributed to 1% of the total injury burden in the country [
5].
A study at Mbarara Regional Referral Hospital showed that, on average, three patients presented with an injury in a day [
6]. However, most injury reports are facility-based, from hospitals and police records [
7]. Facility-based reports do not capture injury events that are not reported and are limited in providing information on factors associated with non-fatal injuries [
8]. Also, most of the reporting is mortality based, yet fatal injuries are only a small fraction of the total burden. Many non-fatal injuries therefore remain unreported in the communities thus underestimating the injury burden [
7,
9].
Studies show that non-fatal injuries have economic, social and psychological consequences and sometimes lead to disability [
1,
7,
10,
11]. The consequences of non-fatal injuries greatly impact an individual’s life, family and society as a whole.
Most previous studies on injuries have focused on particular causes of injuries such as road traffic crashes (RTCs), burns, drowning but not on all other causes [
6,
12]. Focus on particular causes of injuries leads to increased attention to those specific types of injuries whose data is available while other types of injuries continue to increase unnoticed. Reducing the burden of non-fatal injuries requires implementing interventions informed by epidemiological data on all types of injuries [
13]. We therefore conducted a household survey in Mbarara Municipality to identify and describe all non-fatal injury events that occurred from December 2016 to June 2017 and the associated factors.
Methods


Study site
We conducted the study in Mbarara Municipality, Mbarara District. Mbarara District is located in southwestern Uganda about 290 kilometres from Kampala. (
Figure 1). Mbarara Municipality has a population of 195,013 people with six divisions, 22 wards and 170 villages as per the National Population and Housing Census 2014 [
14]. Mbarara District is one of the fastest growing districts in Uganda. In 2017, Mbarara was ranked the 1
stdistrict in the country with high numbers of death by mob action and the 2
ndwith high numbers of homicide cases [
15].
Study design and population
We conducted a cross-sectional study of non-fatal injuries in Mbarara Municipality between May and June 2017. It was a household survey employing quantitative methods of data collection. We included household members of all ages who had lived in Mbarara municipality for at least three months before the study period.
Sample size estimation
We arrived at the sample size of 212 households with 966 household members using the World Health Organisation (WHO) formula for calculating households in a community survey
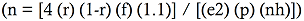
where n = number of households, 4 = the factor to achieve 95% level of confidence, r = estimated prevalence of injuries in the community, 55.6% [
12], f = design effect, 2 [
16] , 1.1 = 10% non-response rate, e = margin error to be tolerated, p = the proportion of the total population that the smallest subgroup comprises, 1 (whole population), nh = average household size,4 [
14].
Sampling procedure
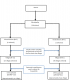
Our study was based on the sampling of households, and we used a multi-stage sampling technique from the division to the household level (
Figure 2). We divided the six divisions of Mbarara Municipality into two strata - urban and rural, based on the population density and characteristics as per the National Population and Housing Census 2014 [
14]. One division was randomly selected from each stratum. In each division, simple random sampling proportionate to size was used to select villages to participate in the study (Panel 1). Ten villages were conservatively added in the urban division to cater for the differences in injury patterns between urban and suburban areas as described by Kobusingye et al. [
7]. In each sampled village, systematic sampling was used to identify the number of households visited (Panel 1).
In each village, the complete list of all households was obtained from the local village chairperson and the ‘nth’ interval was determined, n
thbeing the total number of households in the village/sample size of households needed in that village. To select a starting point, we stood at the centre of the village as identified by the help of the village chairperson. At that point, we rolled a pen to determine the direction of the start point, which was the direction facing the ballpoint of the pen. After listing and numbering the households in the chosen direction, we randomly selected the starting household using a table of numbers. Subsequent households were selected with every ‘nth’ house in that direction. In case we reached the other boundary of the village before completing the sample required, we took another direction after rolling the pen again.
At the household level, we interviewed only one person (most senior female representative of the household head) who gave information about all household members. In the absence of the female representative, we interviewed the spouse or the eldest person (≥ 18 years of age) who was present. When present, the female representative of the household head was the most preferred respondent because they are deemed more knowledgeable about events on their other household members. Sampled households with no occupants present at the time of the visit were revisited one more time, and if on the second time no one was present, the next household was considered as a replacement.
Study Variables
We collected self-reported information on demographics, non-fatal injury occurrence, injury event characteristics and cause of non-fatal injury. We used a structured questionnaire adapted from WHO Guidelines for conducting community surveys on injuries to obtain data on the study variables [
4]. Interviews were carried out in the local language with a translated questionnaire. We defined non-fatal injury as any physical harm due to road traffic crashes, burns, cuts/stabs, blunt injury, poison, near-drowning, animal bites, falls, gunshots and other causes that did not lead to death but instead resulted in losing one or more days of usual daily operating activity. The most recent non-fatal injury (within a 6 month recall period; December 2016 to June 2017) which occurred in Mbarara Municipality resulting in loss of at least one day of usual daily operating activity was the non-fatal injury considered. We used a recall period of 6 months to reduce the possibility of recall bias. A household member was regarded as a usual resident of the household who lived and shared meals in the same dwelling. Cause of non-fatal injury was classified based on ‘external cause of injury’ such as road traffic crash, fall, burns, poisoning and others as per the International Classification of Diseases (ICD) -11 [
17].
We assessed socioeconomic status by evaluating 11 household assets of the family. That is: television, radio, mobile phone, bicycle, motorcycle, motor vehicle, a piece of land, large farm animals like cattle, goats and sheep, small farm animals like poultry, manufactured beds and house wall made of brick [
18]. This method has been used in the Uganda Demographic and Health survey to determine the wealth index of the population [
18]. A study in Uganda on the prevalence of diabetes and pre-diabetes among persons aged 35 to 60 years in Eastern Uganda also used a similar approach [
19].
Data analysis
We entered data in Epi Info Version 7 and later exported to Stata 14 (StataCorp, College Station, TX) for cleaning and analysis. We summarised participant demographics, injury occurrence and injury event characteristics using frequencies and proportions. We used Principle Component Analysis (PCA) to analyse for socioeconomic status and outcomes coded into four parts of lowest quartile, second quartile, middle quartile and fourth quartile.
Each household item was weighted, and a total score for each household generated in Stata 14 (StataCorp, College Station, TX). Participants’ total scores were then grouped into quartiles. Items that were more unequally distributed between households were given more weight [
20]. Also, variables with low standard deviations carried a low weight; for example, an asset which all households owned or which no households owned exhibited no variation between households; hence was zero weighted [
21]. Households were then categorized into quartiles comprising lowest quartile, second quartile, third quartile and fourth quartile.
We conducted bivariate analysis to generate unadjusted prevalence ratios and chi-squared values. We conducted multivariable analysis to identify potential factors independently associated with non-fatal injuries while controlling for potential confounding. Independent variables that were statistically significant at the bivariate analysis at p<0.2 and those known from the literature to be associated with injuries were considered for modelling in the multivariable analysis as recommended by In Lee [
22]. Given the high prevalence of the outcome from our study (non-fatal injury prevalence, 18.2%), we used modified Poisson regression model via generalized linear models to estimate unadjusted and adjusted prevalence ratios (PRs) and corresponding 95% Confidence Intervals of factors associated with non-fatal injury prevalence [
8]. Modified Poisson regression was preferred over logistic regression because when the proportion of the outcome is >10%, odds ratios give biased estimates of prevalence ratios [
9,
10].
Ethical approval
This study was approved by the Higher Degrees Research and Ethics Committee of Makerere University, School of Public Health. We obtained permission to conduct the study from Mbarara Municipal Council offices. We also obtained written informed consent from the study participants. The data obtained was also treated with strict confidentiality: stored in password-protected computers only accessed by the research supervisor and the Principal Investigator. We referred participants who complained of persistent pain and injuries to the nearest health facility for medical attention.
Results


Socio-demographic characteristics
Overall, we included 966 individuals from 212 households. The median age of participants was 20 years (Q1=0.3; Q3=68), 24.8% (240/966) were aged 16-25 years, and 53.5% (517/966) were females. Almost half, 48.9% (472/966) of the participants were in the middle wealth quartile, and 71.5% (691/966) had attained either or both primary or secondary education (
Table 1).
Prevalence of non-fatal injuries
The prevalence of all non-fatal injuries was 18.2% (176/966) of which 92% (162/176) were unintentional non-fatal injuries. Participants aged ≥35 years had the highest prevalence of non-fatal injuries at 22.7% (40/176). Non-fatal injuries were common among males at 54.6% (96/176), and the urban division registered the highest number of non-fatal injuries at 60.2% (106/176) see
Table 2.
Causes of non-fatal injuries
The reported highest cause of non-fatal injuries was falls 27.3% (48/176) followed by RTIs 26.7% (47/176) and burns 16.5% (29/176). Poisoning 2.8% (5/176) constituted the lowest (
Figure 3). Burns were the common cause of non-fatal injuries at 32.3% (10/31) among participants aged 0-5 years. Falls 47.2% (17/36) and cuts 19.4% (7/36) were highest among participants aged 6-15 years and RTIs highest among those aged over 35 years at 45% (18/40).
Injury event characteristics
A small proportion 5.1% (9/176) of the injured people had consumed alcohol before the injury event. More than half 53.2% (25/47) of the RTIs victims were travelling on motorcycles at the time of injury, 53.2% (25/47) were speeding and 80% (20/25) of the motorcycle riders had never used a helmet while riding. Half of the fall victims 52.1% (25/48) fell while walking, and hot liquids were the leading cause of burns at 72.4% (21/29). For violence 7.9% (14/176), strangers were the common perpetrators of violence at 42.8% (6/14) followed by intimate partners at 28.6% (4/14). An equal proportion, 40% (2/5) were poisoned by a cleaning agent and poisonous plant (
Table 3).
Factors associated with non-fatal injuries
At bivariate analysis, non-fatal injury was associated with being male (unadjusted PR = 1.4, 95% CI: 1.1 - 1.8), a casual labourer (unadjusted PR = 2.0, 95% CI: 1.1 - 3.6), staying in an urban division (unadjusted PR = 1.6, 95% CI: 1.2 - 2.1), and being a non-native (unadjusted PR = 0.3, 95% CI: 0.2 - 0.3). After adjusting for confounders, factors that remained statistically significant regarding association with non-fatal injury were occupation as casual laborer (adjusted PR=2.1, 95% CI: 1.2 - 3.7), urban residency, Kakoba division (adjusted PR=1.5, 95% CI: 1.1 - 1.9), and being a non-native (adjusted PR=1.7, 95% CI: 1.3 - 2.3) see
Table 3 (Suite).
Discussion


In this community survey in Mbarara Municipality to identify and describe all non-fatal injury events that occurred from December 2016 to June 2017 and the associated factors, we found a non-fatal injury prevalence of 18.2%, 92% of them being unintentional. This prevalence was higher in comparison to the prevalence of 1.3% reported in a study conducted at Iganga-Mayuge Health and Demographic Surveillance Site (IM-HDSS), Uganda [23]. The higher prevalence in Mbarara Municipality could be related to its location, more urbanized, thus more exposed to many risk factors for injuries. A study carried out in multiple countries in sub-Saharan Africa also reported a lower prevalence of 6.6% [15]. The high prevalence of reported non-fatal injury in our study was expected as injury prevention in Uganda is not proactive. Measures such as sensitisation on prevention of injuries, preparedness of firefighting equipment, checking for drunk driving, speed limit, use of helmets are taken in the wake of increased injury burden and are poorly enforced [26]. A high prevalence of non-fatal injuries implies a reduced quality of life of people and consequently reducing their life expectancy and affecting the country’s economic development.
Overall, falls were the leading cause of non-fatal injury in our study, and most of them occurred when walking. Among adults, falls were majorly due to slips when walking and in children most falls occurred during play. The high prevalence of falls may be due to unsafe neighbourhoods and poor parental supervision for children during play. Similarly, falls as the major causes of injury have been reported in rural community studies from Sudan, India and Abu Dhabi [
8,
24,
27,
28]. Falls were common among all age groups which reveals the need for interventions across the entire lifespan and not just for the children and elderly which had been the focus of interventions hitherto [
29]. Falls have short and long-term effects that significantly impact one´s social and economic life most especially when they result in disability [
30].
Motorcycles were the most significant contributor to RTIs perhaps because they are increasingly being used as a major means of transportation in Uganda yet they remain unregulated in most towns [
31]. Studies from other districts within Uganda, namely Gulu in Northern Uganda and at Mulago referral hospital in Kampala, show similar results of motorcycles’ contributing to RTIs [
32–34]. Despite the overwhelming evidence that speeding increases the risk of a crash, most motorists often drive over the speed limit in Mbarara Municipality [
34]. More so, a big proportion (80%) of motorcycle users had never used a helmet. Our finding is contrary to a study in Uganda which showed otherwise with more than 80% of motorcyclists having used a helmet at the time of the crash [
35]. This may be due to the difference in enforcement of helmet use at the time the two studies were carried out. Bishai
et al. (2008) found traffic enforcement to be a cost-effective intervention in reducing road traffic crashes [
36] suggesting the need for vigilance in traffic law enforcement and rider sensitisation.
We found that non-natives were more likely to report injury compared to the natives. Majority of the non-natives come to Mbarara District as casual labourers and are thus more likely to be exposed to harsh working conditions and risky behaviour to earn a living. Similar, findings have been reported in other studies in Abu Dhabi and Kenya where non-natives were found to be more injured than the natives [
28,
37]. Casual labourers were also more prone to injuries possibly because of the unsafe working conditions at their places of work. The unsafe conditions casual labourers are exposed to at work are as a result of the weak enforcement of the occupational health and safety law in Uganda [
38,
39]. Similar studies in Uganda, Ethiopia and Iran revealed similar findings with a high number of casual labourers being injured [
12,
40,
41]. Increased injury prevalence among casual labourers may result in low productivity and loss of earnings.
To our knowledge, this was the first community survey on non-fatal injuries in Mbarara District focusing on all causes of injuries. The study, however, had some limitations such as recall bias since it involved remembering events in the past 6 months and was based on self-reporting. During the interviews, respondents were allowed sufficient time to adequately recall the events of the past to minimise the recall bias. Additionally, interviewing only one person on injury-related information for all members of the household may have resulted in information bias. However, this potential bias was mitigated by verifying responses with the family members who were available at the time of the interview. The study assessed non-fatal injuries for six months hence we were unable to show the extent of variation by season. However, the available information from this study is beneficial, as only RTIs tend to be seasonal.
Conclusion


The prevalence of injuries was high in Mbarara Municipality, the majority of them being unintentional and caused by falls and RTIs. These findings reveal a gap in injury prevention in Uganda that needs to be addressed to improve the quality of life and reduce the number of avoidable hospital visits that continue to burden the health system. Home improvement campaigns promoting safer homes should be implemented encouraging promotion of levelled grounds and supervision of children during play. Casual labourers and people in self-employment were more injured in our study calling for inspection of workplaces for safety measures and the strengthening of enforcement of occupational health and safety laws.
Consent for publication
We sought consent to publish our study from the Fogarty International Center of the U.S. National Institutes of Health (Chronic Consequences of Trauma, Injuries, Disability Across the Lifespan: Uganda) and Makerere University School of Public Health.
Availability of data and materials
Data and materials can be made available by the corresponding author based on reasonable request.
Competing interests


The authors declare no competing interests.
Funding
This study was supported by grant # D43TW0092884 from the Fogarty International Center of the U.S. National Institutes of Health (Chronic Consequences of Trauma, Injuries, Disability Across the Lifespan: Uganda).
Authors´ contributions


RN conceived the idea and designed the study; led data analysis and interpretation; developed the first draft of the manuscript and revised based on the co-authors comments and suggestions. ANK, DM, DB, LB, OA contributed to data interpretation, revised the manuscript critically for important intellectual content; ensured the requirements of submission of the manuscript are met. FO, FM contributed towards analysis and interpretation of the data to agree with results and conclusion; revised the manuscript and editing. NP, GP, AB, OK made contribution towards content review for expert opinion from study design and manuscript writing. KM, JS supervised the study from designing to writing of the manuscript. All authors read and agreed to the final version of the manuscript for publication.
Acknowledgments


We are grateful to the study participants for sharing their information with us, and to the study team for their role in data collection. We thank Mbarara Municipality administration for allowing us to conduct the study in the district. We are indebted to the Africa Field Epidemiology Network (AFENET) secretariat which facilitated a writing workshop that led to the progress of this manuscript writing.
Tables and figures


Table 1: Socio-demographic characteristics of community members of Mbarara Municipality, December 2016 - May 2017
Table 2: Distribution of non-fatal injuries among community members of Mbarara municipality, December 2016 - May 2017
Table 3: Injury event characteristics of participants
Table 3 (suite): Injury event characteristics of participants
Figure 1: The map of Uganda showing the location of Mbarara District (42)
Figure 2: Sampling procedure for the community study on non-fatal injuries and factors associated in Mbarara Municipality from May to June 2017
Figure 3: Causes of non-fatal injuries among community members of Mbarara Municipality, December 2016 - May 2017
Annex


Annex 1: Panel 1: Sampling Strategy for Villages and Households
References


- Haagsma JA, Graetz N, Bolliger I, Naghavi M, Higashi H, Mullany EC, et al. The global burden of injury: incidence, mortality, disability-adjusted life years and time trends from the Global Burden of Disease study 2013. Inj Prev. 2016 Feb;22(1):3–18. PubMed | Google Scholar
- Baker SP, Baker SP, editors. The Injury fact book. 2nd ed. New York: Oxford University Press; 199 344 p. PubMed | Google Scholar
- WHO.Injuries [Internet]. WHO. [cited 2018 Jul 25].
- WHO.Disease burden and mortality estimates [Internet]. WHO. [cited 2018 Jul 25].
- MoH. Uganda Health Management Information System database. 201.
- G. Ruhinda, P. Kyamanywa, D. Kitya, F. Bajunirwe. Abdominal injury at Mbarara Regional Referral Hospital, Uganda. East and Central African Journal of Surgery. 2008 Sep;13(2):29–3. PubMed | Google Scholar
- Kobusingye O. Injury patterns in rural and urban Uganda. Injury Prevention. 2001 Mar 1;7(1):46–50.https://doi.org/10.1136/ip.7.1.46 PubMed | Google Scholar
- Kalaiselvan G, Dongre AR, T M. Epidemiology of injury in rural Pondicherry, India. Journal of Injury and Violence Research. 2011 Jun 1;3(2):61–6. https://doi.org/10.5249/jivr.v3i2.74 PubMed | Google Scholar
- Gyedu A, Nakua EK, Otupiri E, Mock C, Donkor P, Ebel B. Incidence, characteristics and risk factors for household and neighbourhood injury among young children in semiurban Ghana: a population-based household survey. Inj Prev. 2015 Apr;21(e1):e71-7.https://doi.org/10.1136/injuryprev-2013-040950 PubMed | Google Scholar
- Gosselin RA. The Increasing Burden of Injuries in Developing Countries: Direct and Indirect Consequences. Techniques in Orthopaedics. 2009 Dec;24(4):230–2.https://doi.org/10.1097/BTO.0b013e3181bfd56c
- Zonfrillo MR, Durbin DR, Winston FK, Zhao H, Stineman MG. Physical Disability After Injury-Related Inpatient Rehabilitation in Children. PEDIATRICS. 2013 Jan 1;131(1):e206–13.https://doi.org/10.1542/peds.2012-1418 PubMed | Google Scholar
- Bashah DT, Dachew BA, Tiruneh BT. Prevalence of injury and associated factors among patients visiting the Emergency Departments of Amhara Regional State Referral Hospitals, Ethiopia: a cross-sectional study. BMC Emerg Med. 2015 Aug 25;15:20.https://doi.org/10.1186/s12873-015-0044-3 PubMed | Google Scholar
- Cinnamon J, Schuurman N. Injury surveillance in low-resource settings using Geospatial and Social Web technologies. International Journal of Health Geographics. 2010 May 24;9(1):25. https://doi.org/10.1186/1476-072X-9-25 PubMed | Google Scholar
- Uganda Bureau of Statistics.The National Population and Housing Census 2014 – Main Report [Internet]. Kampala, Uganda; 2016 [cited 2019 Jul 25] p. 105.
- Uganda Police. Annual Crime Report - 2017 [Internet]. 2018 [cited 2018 Sep 10].
- Gosavi SV, Deshmukh PR. Epidemiology of injuries in rural Wardha, central India. Med J Armed Forces India. 2014 Oct;70(4):380–2. https://doi.org/10.1016/j.mjafi.2014.02.003 PubMed | Google Scholar
- WHO. International Classification of Diseases, 11th Revision (ICD-11) [Internet].[cited 2018 Aug 25].
- UBOS.Uganda Demographic and Health Survey 2016: Key Indicators Report. [Internet]. UBOS, and Rockville, Maryland, USA: UBOS and ICF.; 2017 [cited 2018 Aug 25].
- Mayega RW, Guwatudde D, Makumbi F, Nakwagala FN, Peterson S, Tomson G, et al. Diabetes and Pre-Diabetes among Persons Aged 35 to 60 Years in Eastern Uganda: Prevalence and Associated Factors. PLOS ONE. 2013 Aug 14;8(8):e72554.https://doi.org/10.1371/journal.pone.0072554 PubMed | Google Scholar
- McKenzie DJ. Measuring inequality with asset indicators. Journal of Population Economics. 2005 Jun;18:229–60. https://doi.org/10.1007/s00148-005-0224-7 Google Scholar
- Vyas S, Kumaranayake L. Constructing socio-economic status indices: how to use principal components analysis. Health Policy Plan. 2006 Nov;21(6):459–68.https://doi.org/10.1093/heapol/czl029 PubMed | Google Scholar
- Lee KI, Koval JJ. Determination of the best significance level in forward stepwise logistic regression. Communications in Statistics - Simulation and Computation. 1997 Jan 1;26(2):559–75. https://doi.org/10.1080/03610919708813397 Google Scholar
- Jafri AF.Injuries and Socioeconomic Status in Iganga and Mayuge, Uganda: Inequities, Consequences and Impacts [Internet] [Thesis]. Johns Hopkins University; 2016 [cited 2018 Jul 30].
- Tayeb SE, Abdalla S, Mørkve O, Heuch I, Van den Bergh G. Injuries in Khartoum state, the Sudan: a household survey of incidence and risk factors. International Journal of Injury Control and Safety Promotion. 2014 Apr 3;21(2):144–53.https://doi.org/10.1080/17457300.2013.792283 Google Scholar
- Diamond MB, Dalal S, Adebamowo C, Guwatudde D, Laurence C, Ajayi IO, et al. Prevalence and risk factor for injury in sub-Saharan Africa: a multicountry study. Inj Prev. 2018 Aug;24(4):272–8.https://doi.org/10.1136/injuryprev-2016-042254 PubMed | Google Scholar
- Kobusingye OC, Guwatudde D, Owor G, Lett RR. Citywide trauma experience in Kampala, Uganda: a call for intervention. Inj Prev. 2002 Jun;8(2):133–6.https://doi.org/10.1136/ip.8.2.133 PubMed | Google Scholar
- Swarnkar M, Singh PK, Dwivedi S. Pattern Of Trauma In Central India: An Epidemiological Study With Special Reference To Mode Of Injury. The Internet Journal of Epidemiology [Internet]. 2009 Dec 31 [cited 2018 Jul 30];9(1).https://doi.org/10.5580/6a3
- Rahman MH, Allen KA, Hyder AA, Health Authority of Abu Dhabi. Descriptive epidemiology of injury cases: findings from a pilot injury surveillance system in Abu Dhabi. Int J Inj Contr Saf Promot. 2016;23(2):214–23.https://doi.org/10.1080/17457300.2014.908225 PubMed | Google Scholar
- Rehmani R, LeBlanc JC. Home visits reduce the number of hazards for childhood home injuries in Karachi, Pakistan: a randomized controlled trial. Int J Emerg Med. 2010 Dec 7;3(4):333–9.https://doi.org/10.1007/s12245-010-0238-0 PubMed | Google Scholar
- Chippendale T, Gentile PA, James MK. Characteristics and consequences of falls among older adult trauma patients: Considerations for injury prevention programs. Australian Occupational Therapy Journal. 2017 Oct 1;64(5):350–7.https://doi.org/10.1111/1440-1630.12380 PubMed | Google Scholar
- Tumwesigye NM, Atuyambe LM, Kobusingye OK. Factors Associated with Injuries among Commercial Motorcyclists: Evidence from a Matched Case Control Study in Kampala City, Uganda. PLOS ONE. 2016 Feb 26;11(2):e0148511. https://doi.org/10.1371/journal.pone.0148511 PubMed | Google Scholar
- Kitara DL. Boda Boda Injuries in Gulu Regional Hospital, Northern Uganda. East and Central African Journal of Surgery. 2011 Jan 1;16(2):97–101. PubMed | Google Scholar
- Galukande M, Jombwe J, Fualal J, Gakwaya A. Boda-boda injuries a health problem and a burden of disease in Uganda: A tertiary hospital survey. East and Central African Journal of Surgery. 2009 Jan 1;14(2):33–7. PubMed | Google Scholar
- Balikuddembe JK, Ardalan A, Khorasani-Zavareh D, Nejati A, Munanura KS. Road traffic incidents in Uganda: a systematic review of a five-year trend. J Inj Violence Res. 2017 Jan;9(1):17–25. https://doi.org/10.5249/jivr.v9i1.796 PubMed | Google Scholar
- Richard Sebaggala , Fred Matovu , Dan Ayebale, Vincent Kisenyi , Mesharck Katusiimeh. The Cost of Motorcycle Accidents in Uganda [Internet]. 2014 [cited 2019 Jul 26].
- Bishai D, Asiimwe B, Abbas S, Hyder AA, Bazeyo W. Cost-effectiveness of traffic enforcement: case study from Uganda. Inj Prev. 2008 Aug;14(4):223–7.https://doi.org/10.1136/ip.2008.018341 PubMed | Google Scholar
- Ziraba AK, Kyobutungi C, Zulu EM. Fatal injuries in the slums of Nairobi and their risk factors: results from a matched case-control study. J Urban Health. 2011 Jun;88 Suppl 2:S256-265.https://doi.org/10.1007/s11524-011-9580-7 PubMed | Google Scholar
- Kiconco A, Ruhinda N, Kyobutungi V, Watya S, Bazeyo W. Determinants of Occupational Injuries among Building Construction Workers in Kampala City, Uganda. Annals of Global Health. 2017 Jan;83(1):86.https://doi.org/10.1016/j.aogh.2017.03.189 PubMed | Google Scholar
- Irumba R. Spatial analysis of construction accidents in Kampala, Uganda. Safety Science. 2014;64:109–20. https://doi.org/10.1016/j.ssci.2013.11.024
- Hsia RY, Ozgediz D, Mutto M, Jayaraman S, Kyamanywa P, Kobusingye OC. Epidemiology of injuries presenting to the national hospital in Kampala, Uganda: implications for research and policy. International Journal of Emergency Medicine. 2010 Sep;3(3):165–72.https://doi.org/10.1007/s12245-010-0200-1 PubMed | Google Scholar
- Saadat S, Mafi M, Sharif-Alhoseini M. Population based estimates of non-fatal injuries in the capital of Iran. BMC Public Health. 2011 Jul 31;11(1):608. https://doi.org/10.1186/1471-2458-11-608 PubMed | Google Scholar
- getamap.net. Mbarara District (Mbararadistrict) Map, Weather and Photos - Uganda: first-order administrative division - Lat:-0.416667 and Long:30.75 [Internet]. [cited 2018 Oct 16].