Evaluation of the meningitis surveillance system in Luanda Province, Angola, March 2017
Dilunvuidi Dievie N’dongala Pode1,&, João Esteves Pires2, Felix Balbina Ventura2, Regina Muquila António3, Olufemi Olamide Ajumobi4
1Angola National School of Public Health, Agostinho Neto University, Angola, 2National School of Public Health of Angola, Ministry of Health, Angola, 3Luanda Provincial Department of health, Angola, 4African Field Epidemiology Network Nigeria Country Office, Abuja, Nigeria
&Corresponding author
Dilunvuidi Dievie N’dongala Pode, Angola Field Epidemiology and Laboratory Training Programme, Angola. dilupode@gmail.com
Introduction:
Meningitis due to Neisseria meningitidis is a priority public health disease given its high epidemic potential and associated mortality. Angola is not one of the countries in the African meningitis belt and frequent outbreaks are uncommon. This might affect the preparedness and capacity of the surveillance system to promptly detect and effectively respond, should a meningitis outbreak occur. From 2014 to 2015, there was an increase in the number of meningitis cases identified in Angola, partly due to heightened disease surveillance. We evaluated the meningitis surveillance system to establish if the surveillance system was meeting its set objectives and made recommendations for improvement
Methods:
A cross-sectional study was conducted among health workers in Luanda province in March 2017. Using a pretest structured questionaire, we obtained information on the participants demographic characteristics, work experience, training and their knowledge about the meningitis surveillance system. Participants’ knowledge was graded poor (<50%), reasonable (50 – 69%), good (70 – 90%) and excellent (> 90%). We assessed the key system attributes using the updated CDC guidelines for evaluating public health surveillance systems.
Results:
Of the 52 operators interviewed, 51.9% were (27/52) nurses, 61.5% (32/52) had >5years work experience and 85.6% (45/52) had not been trained in public health surveillance in the last 5 years. Doctors and nurses had knowledge score of <20%, disease specific focal points and the program coordinator scored 85.7% and 100% respectively. Overall scores for the system’s attributes were as follows; simplicity-(33.3%), data quality-69.2 % and timeliness 33.3%. There was no evidence to suggest that data from the surveillance system was analysed at the source.
Conclusion:
Knowledge of surveillance system among doctors and nurses was very poor. Overall, the system was complex, with poor data quality, not timely and of low utility. We recommend periodic training of health workers, simplifying operation of the system, compliance with reporting timelines and regular data analysis and use for action at the source
Introduction

Bacterial meningitis is a public health priority given its high epidemic potential, and profound impact on public health [1–3]. Bacterial meningitis has multiple aetiologies, however, meningococcal meningitis caused by Neisseria meningitides assumes a particular importance for public health. Meningitis caused by Neisseria species has a high fatality rate of ≥50% if left untreated or when adequate treatment is delayed. The disease can cause severe brain damage with residual sequelae in more than 10% of the cases [4–9]. Among the 12 known serotypes of Neisseria meningitides, six serotypes (A, B, C, W, X and Y) have caused disease outbreaks [5,6,10,11].
The main objectives of the meningitis surveillance system are prompt detection and confirmation of outbreaks, monitoring trends of specific meningococcal strains and the determination of the impact of preventive strategies, including vaccination campaigns [
5,
12]. The largest disease burden of bacterial meningitis is confined to the meningitis belt in sub-Saharan Africa, where large outbreaks occur frequently [
13–15]., Angola is not one of the countries in the meningitis belt. Frequent outbreaks are uncommon in Angola and this might affect the preparedness and capacity of the surveillance system to promptly detect and evoke an effective public health response in the event of an outbreak.
From 2014 to 2015, there was an increase in the number of meningitis cases reported at the national level, partly due to improved disease surveillance efforts in the country. In 2014, Luanda Province accounted for 64.7% (360/556) of meningitis cases and 63.8% (67/105) of the meningitis related deaths reported in Angola [
16]. In 2015, 707 cases and 78 deaths due to meningitis were reported nationally. Of these, Luanda-the Angola capital city had the highest incidence rate of 8.5 / 100,000 inhabitants and mortality rate of 1.2 / 100,000 [
17]. Based on increase in the incidence of meningitis cases the Luanda Provincial Health Department proposed an evaluation of the meningitis surveillance system. In March 2017, we evaluated the meninigitis surveillance system to establish whether the system was robust enough for its intended purpose, determine any weaknesses there in, devise strategies and implement actions to improve the performance of the surveillance system.
Methods


Study design: We conducted a cross-sectional study among the staff of the surveillance division of Luanda Provincial Health Department and three health facilities (HF) in Luanda province in March 2017 to evaluate the meningitis surveillance system attributes. The evaluation was based on the US Centers for Disease Control 2001 updated guidelines for evaluating public health surveillance systems. The selected health facilities included Américo Boavida Hospital, David Bernardino Paediatric Hospital and Cajueiros do Cazenga General Hospital.
Study Population: The study population comprised of the employees working at the aforementioned health facilities, namely: doctors, nurses, focal points, statisticians and surveillance coordinators. All employees who were available at work on the day of the visit were eligible for inclusion in the survey. Employees who did not consent to participate were excluded from the study.
Sampling technique: We obtained the list of health facilities existent in the province obtained from Luanda Provincial Health Department. The health facilities were stratified sample by level of operation, i.e., national (tertiary) and provincial (secondary) levels, we included, randomly selected two national hospitals and also included the only provincial hospital that had the laboratory capacity to diagnose of meningitis. The provincial hospitals without the capacity for microbiology tests were excluded from the study. Study participants responsible for meningitis case management in selected health facilities (hospitals) were included purposively.
Data collection: The primary data were obtained by interview, using a semi-structured questionnaire administered to health workers responsible for the operation of the system. We obtained secondary data from the health information system database and technical reports using a pre-tested and standardised data collection tool.
Definition of variables
a) Socio-demographic variables comprised: age, sex, academic level.
b) Professional variables comprised: role in system, years of work experience and training.
c) Level of knowledge was ascertained based on scores assigned to parameters about the system, namely: concept of the meningitis epidemiological surveillance, objectives of the meningitis epidemiological surveillance, case definition of meningitis, the need to notify a meningitis case and notification deadlines defined by national level. Participants provide answers to a total of five questions scored mark (
Annex 1) and each correct answer would score 20%. Knowledge scores of <50%, 50 – 69%, 70 – 90%, > 90% were considered poor, reasonable, good and excellent respectively.
d) Attributes:
Simplicity - refers to both its structure and ease of operation. The following parameters were checked: domain of case definition and objectives of the surveillance system by health workers, types of data required to establish the diagnosis, number of notification levels and data sources, and need for trained team.
Data quality - reflects the completeness and validity of the data recorded in the public health surveillance system. The following parameters were checked: completeness, correctness and match information. Each parameter was scored. Data quality scores of <70%, 70 – 79%, 80 – 89%, 90-100% were considered poor, reasonable, good and excellent, respectively [
18].
Timeliness - reflects the expected time frame of reporting between the different stages in a public health surveillance system. We verified the compliance with the deadlines established for sending weekly and monthly reports at different levels.
Usefulness - refers to ability of public health surveillance system in contributing to the prevention and control of adverse health-related events, including an improved understanding of the public health implications of such events. We verified the fulfilment of its objectives through the existence of analysis reports of the data collected, documents with guidelines to the reporting units, evidence of implementation of measures after completion of data analysis.
Data processing and analysis
The data obtained were processed and analysed using Epi-Info software version 7.2.0.1. Results were presented in tables and charts.
Ethical considerations
The ethical approval of the study was obtained from the Luanda Provincial Health Department and from the Health facilities directorates. Informed verbal consent was obtained from the participants. Participants were informed they could opt out of the study at any time. Confidentiality of information given by participants was maintained throughout the study.
Results


Notification flows and deadlines for the Angolan meningitis surveillance system
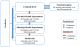
The health unit notifies the municipal health department weekly and monthly on information on meningitis cases. Similarly, municipal health department notifies the provincial health department and finally from the provincial level follows a notification to the national level. The national hospitals notify the central level directly. The feedback follows the same pathway at all levels (
Figure 1).
Socio-demographics and professional characteristics: Overall, 52 operators of the system were interviewed, with a mean age of 39.0 ± 4.7years. Of these 51.9% (27/52) were females, 51.9% (27/52) nurses, 55.8% (29/52) completed secondary education, 61.5% (32/52) operated the system for more than 5 years, 85.6% (45/52) did not have any type of training in the last 5 years (
Table 1).
Level of knowledge: All respondents knew the case definition of meningitis. Overall, 9.6% (5/52) knew the concept of the meningitis epidemiological surveillance; 11.5% (6/52) the objectives of the meningitis epidemiological surveillance, 15.4% (8/52) knew the necessity of notifying a meningitis case and the notification deadlines defined by national level (
Table 2). Doctors (13) and nurses (27) had the lowest average scores of 20% of correct answers, compared to the disease specific focal points (7) and the program coordinator (1) who had an average scores of 85.7% and 100% respectively (
Figure 2).
Simplicity: While evaluating simplicity attribute of the system, we found the following: 4 (7.7%) out of the 52 interviewees were aware of the objectives of the surveillance system; both the clinical and laboratory data were necessary to establish the diagnosis. There were several sources of data (9 sources) but there was no standardised notification form in the health facilities involved in the study. There were expert teams trained in the management of cases and samples.
Data quality: Overall, 61.5% (16/26) of the analysed forms were fully completed, in 100% of the cases such forms were correctly filled-in. =When analysing the different data sources there was only a 46.1% (12/26) concordance across all the different sources.
Timeliness: In the evaluation of the attribute timeliness, 63.4% (33/52) of provincial health department reported weekly and 2.1% (1/48) out of the 48 monthly reports analysed, were delivered within the stipulated timeframe defined at the national level.
Overall, the final score for these attributes, simplicity, data quality and timeliness were 33.3%, 69.2 % and 34.0 %, respectively (
Table 3).
Usefulness: We found reports of meningitis cases in the various data sources analysed in both levels of the health system included in the study (provincial and national) without any evidence regarding the analysis of data collected, guidelines to reporting units and implementation of measures according to the conclusions of secondary data analysis.
Discussion


Overall, the meningitis surveillance system in Luanda system was complex, not timely and the data quality was poor. In addition, the level of knowledge of the users of the system was low, although they all knew the case definition, with the doctors and nurses having the lowest level of knowledge. In the meningitis surveillance system, ideally staff should be involved from the point of identification of a suspected case to the institution of disease prevention and control measures [19]. The professional training of staff involved in the epidemiological surveillance system is the key to the achievement of the set objectives. The fact that doctors and nurses focus their activity in the clinical management of cases may be responsible for their poor knowledge of surveillance system. A similar study conducted in Ghana in 2017 by Kaburi et al. revealed a good overall knowledge among respondents due to the clear understanding of the purpose and objectives of the system, unlike the findings of our study [20].
We found the system to be complex because most of the interviewees did not have a clear understanding about the objectives of the system, there was a need for both clinical and laboratory data to establish the diagnosis, there were many data sources, and the system relies on specialist teams trained in case management and collection of samples. In a similar study in Brazil, Figueira
et al. 2014, also found the meningitis surveillance system to be complex, due to the characteristics of the event itself requiring several criteria for case diagnosis, which required continuous training of the staff to maintain the quality of the surveillance system [
8]. In Nigeria, Bajoga
et al., found a complex system due to the specialised training needed to collect samples [
21]. However, in Ghana Kaburi
et al. found the meningitis surveillance system to be simple due to the clarity of case definition and the ease of capturing cases [
20]. In Marocco, Essayagh
et al. found a system to be simple regarding structure [
22].
Overall, the data quality in our study was poor due to the incomplete filling of the blank spaces existing in the surveillance forms and non-matching of information from different sources. Ideally the surveillance system should have good data quality that accurately reflects the event under surveillance and allows the available resources to be used efficiently and effectively in monitoring public health priority events. Contrary to our study, in Ghana, Kaburi
et al. and Figueira
et al. in Brazil concluded that the systems in their own settings, had a good data quality due to its completeness and concordance of the information across all data sources [
18,
20]. Quality of data is influenced by the clarity of surveillance forms, the quality of training and supervision of persons who complete surveillance forms, and the attention to detail exercised in data management [
19].
Our results revealed a non-compliance with the weekly and monthly deadlines established by the central level. Lack of knowledge of the need for notification and the established deadlines, may be the basis for this finding. In line with our results, Kaburi
et al. also found the system not to be timely in meeting the deadlines for report submission at the different stages of data flow [
20].
We found a system with low utility since there was no evidence to justify the fulfilment of its objectives, namely reports of the analysis of data collected, guidelines to reporting units and implementation of measures emanating from data analysis. Figueira
et al. found a useful system due to the publications related to the meningitis surveillance in the São Paulo Epidemiological Bulletin [
18]. Apanga and Awoonor-Williams found a surveillance system very useful as data from the system has informed policy and decision making that has led to the formulation of policies on meningitis control and prevention [
23]. Countries like Angola with fragile or poor-quality surveillance systems will have a greater difficulty in detecting early and/or responding promptly and in a timely manner to adverse public health events, such as meningitis outbreaks.
Though the Luanda surveillance system was designed to rapidly detect and confirm meningitis, use the data for planning, assess and status of epidemic, effectiveness of control measures, yearly changes in
Neisseria meningitides serogroups and ascertain antimicrobial susceptibility; the system did not meet these objectives [
1].
The study has a few limitations. We were unable to evaluate the positive predictive value of the system due to insufficient data. Sensitivity for laboratory diagnosis was not assessed because laboratory data was not available to conduct such evaluation. Stability, flexibility and acceptability were not evaluated.
Conclusion


Overall, the meningitis surveillance system was considered to be complex, with poor data quality, not timely and with low utility. Particularly alarming, was the poor knowledge among doctors and nurses which hinders the quality of the surveillance system from its starting point. We recommend Luanda Provincial Health Department and the Health Facilities Directorates should ensure periodic training of health workers, harmonisation and standardisation of data sources, improvement in immediate reporting using electronic platform, daily processing of data to facilitate compliance with reporting deadlines at central level, analysis of processed data and provision of feedback to the respective reporting units.
Availability of data and materials
Data is available at Agostinho Neto University, Angola National School of Public Health and the Luanda Provincial Department of health.
Competing interests


The authors declare that they have no competing interests. The findings and conclusions in this report are those of the authors and do not necessarily represent the official position of the Provincial Health Department.
Funding
This study was funded by Angola National School of Public Health through a Cooperative Agreement with CDC/PEPFAR and personal funds.
Authors´ contributions


DDNP and RMA planned the study. DDNP and JEP designed the study. DDNP was responsible for data collection, entry and analysis, and wrote the manuscript. JEP, BVF and OOA revised subsequent drafts of the manuscript. All authors read and approved the final manuscript.
Acknowledgments


The health facilities directorates, namely, Hospital Paediatric David Benardino, Hospital Américo Boavida, Hospital Geral dos Cajueiros de Luanda and the Provincial Health Department provided local support for study implementation. The authors would like to thank these institutions and all health workers interviewed for the purpose of this evaluation.
Tables and figures


Table 1: Socio-demographics and professional characteristics of the health workers interviewed on meningitis surveillance system, Luanda, March 2017 (N=52)
Table 2: Knowledge of the health workers on meningitis surveillance system, Luanda, March 2017 (N = 52)
Table 3: Attributes of Meningitis Surveillance System, Luanda, March 2017
Figure 1: Weekly and monthly notification flows and deadlines
Figure 2: Distribution of level of knowledge of the health workers interviewed, Luanda, March 2017
Annex


Annex 1: Level of knowledge
References


- Ministério da saúde. Manual de vigilância epidemiológica integrada de doenças e resposta. 2013. Angola. Ministério da saúde.
- Martin C. J. Maiden. The impact of protein-conjugate polysaccharide vaccines: an endgame for meningitis? Philos Trans R Soc Lond B Biol Sci. August 2013;368(1623):20120147. https://doi.org/10.1098/rstb.2010147. PubMed | Google Scholar
- Batista RS, Gomes AP, Dutra Gazineo JL, Balbino Miguel PS, Santana LA, Oliveira L, et al. Meningococcal disease, a clinical and epidemiological review. Asian Pacific Journal of Tropical Medicine. November 2017;10(11):1019-1029. https://doi.org/10.1016/j.apjtm.2017.10.004. Google Scholar
- Ministério da saúde. Guia de vigilancia epidemiológica. 7a edição. Brasilia - DF. 2009. Brasil. Ministério da saúde.
- World Health Organization. Meningitis meningocócica. World Health Organization. 2018; Accessed 25 July 2018.
- Jafri RZ, Ali A, Messonnier NE, Tevi-Benissan C, Durrheim D, Eskola J, et al. Global epidemiology of invasive meningococcal disease. Popul Health Metr. September 2013;11:17.https://doi.org/10.1186/1478-7954-11-17. Google Scholar
- World Health Organization. Meningitis meningocócica. World Health Organization. 2018; Accessed 25 July 2018.
- Centers for Disease Control and prevention. Meningococcal Disease. CDC. 2018; Accessed 19 Sepember 201.
- Stephen I.Pelton. The Global Evolution of Meningococcal Epidemiology Following the Introduction of Meningococcal Vaccines. Journal of Adolescent Health. August 2016;59(2, Supplement):S3-11. https://doi.org/10.1016/j.jadohealth.2016.04.012. Google Scholar
- Judith E. Mueller. Conjugate vaccine introduction in the African meningitis belt: meeting surveillance objectives. Tropical Medicine & International Health. November 2012;18(1):58-64. https://doi.org/1111/tmi.12009. Google Scholar
- Borrow R, Caugant A. D, Ceyhan M, Christensen H, Dinleyici E. C, Findlow J. et al. Meningococcal disease in the Middle East and Africa: Findings and updates from the Global Meningococcal Initiative. Journal of infection. July 2017;75(1):1-11https://doi.org/10.1016/j.jinf.2017.04.007. Google Scholar
- World Health Organization. Epidemic meningitis surveillance in the African meningitis belt Deciding on the most appropriate approach. 2014. Geneva. WHO.
- Kamal Elbssir, Tarig babiker, Ahmed Abu-Rayyan, Hamid Nourain. Assessment of epidemiological meningitis surveillance system in Khartoum locality, 2015. European journal of pharmaceutical and medical research. 2017;3(11):704-710. Google Scholar
- Thomson MC, Molesworth AM, Djingarey MH, Yameogo KR, Belanger F, Cuevas LE. Potential of environmental models to predict meningitis epidemics in Africa. Tropical Medicine & International Health. June 2006;11(6):781-788.https://doi.org/10.1111/j.1365-3156.2006.01630.x. Google Scholar
- Agier L, Martiny N, Thiongane O, Mueller JE, Paireau J, Watkins ER, et al. Towards understanding the epidemiology of Neisseria meningitidis in the African meningitis belt: a multi-disciplinary overview. International Journal of Infectious Diseases. January 2017;54:103-112. https://doi.org/10.1016/j.ijid.2016.10.032. Google Scholar
- Centro nacional de processamento de dados epidemilogicos-C.P.D.E. Boletim epidemiológico 2014. 2014. Angola. Direcção Nacional de Saúde Pública-Ministério da saúde.
- Centro nacional de processamento de dados epidemilogicos-C.P.D.E. Boletim epidemilógico 2015. 2015. Angola. Direcção Nacional de Saúde Publica-Ministério da saúde.
- Gerrita de Cassia N. FigueiraI, Telma R.M.P. Carvalhanas, Maria Inês Gonçalves Okai, Ana Lúcia Frugys Yu, Bernadete de Lourdes Liphaus. Avaliação do sistema de vigilância das meningites no município de São Paulo, com ênfase para doença meningocócica. BEPA Boletim Epidemiológico Paulista (Online). January 2012;9(97):05-25. Google Scholar
- Centers for Disease Control and prevention. Updated Guidelines for Evaluating Public Health Surveillance Systems. CDC. 2001; Accessed 25 July 2018.
- Basil Benduri Kaburi, Chrysantus Kubio, Ernest Kenu, Kofi Mensah Nyarko, Jacob Yakubu Mahama, Samuel Oko Sackey, Edwin Andrew Afari. Evaluation of the enhanced meningitis surveillance system, Yendi municipality, northern Ghana, 2010-2015. BMC Infectious Diseases. April 2017;17(306). https://doi.org/10.1186/s12879-017-2410-0. PubMed | Google Scholar
- Bajoga UA, Abubakar A, Shamang A, Olufemi A, Dalhat M, Balarabe H, et al. Evaluation of Kaduna State meningitis surveillance system: 2014 - 2015. Pan African Medical Journal. February 2018;2(8)96. https://doi.org/10.11604/pamj.cp.2018.8.96.697. PubMed | Google Scholar
- Essayagh T, Khattabi A, Essayagh S, Khouchoua M. Evaluation of the Meningitis Surveillance System in Meknes, Morocco. Iproceedings. 2018;4(1):e10614. https://doi.org/10.2196/10614. Google Scholar
- Paschal Awingura Apanga, John Koku Awoonor-Williams. An Evaluation of Meningitis Surveillance in Northern Ghana. International Journal of Tropical Disease & Health. 2016;12(2):1-10. https://doi.org/10.9734/IJTDH/2016/22489. Google Scholar